Recurrent Foreign Body Ingestions Following Rapid Methadone Taper: Neurological Aspects of Self-Injury and Opioid Therapy
The following case details the treatment of a patient with opioid use disorder and borderline personality traits hospitalized for recurrent foreign body ingestion after rapid taper of methadone. Methadone is a leading treatment for opioid-addicted patients, reducing relapse and other substance use, and shown to have anti-manic and anti-psychotic effects (1). The medical literature equivocates about methadone-taper versus long-term therapy, and the risks cessation can present to patients with psychiatric comorbidities (2, 3). Although usefulness of naltrexone and anti-psychotic therapy for curbing self-mutilation has been demonstrated, the relationship between self-harm and methadone is largely unstudied, despite high concordance between parasuicidality and opioid abuse (4–6). The present case highlights the neurological relationship between methadone and parasuicidal behavior in patients with borderline traits and illustrates the risks of inadequate methadone therapy in patients with these psychiatric comorbidities.
We present a case with discussion surrounding the relationship between self-harm and opioid pathways in patients with borderline personality disorder. Informed consent was obtained from the case patient, and our institutional review board opined that this report is exempt from institutional review board inspection.
Case
“Mr. A” is a homeless, 39-year-old Caucasian man, who presented to the emergency department of an urban academic medical center after he swallowed a 6-inch knife (see Figure 1). He endorsed a history of opioid use disorder, depression, psychotic episodes, and childhood sexual abuse but denied suicidality. He described episodes of cutting and self-electrocution with an electric fence in his teens, calling these behaviors a means of emotional release. He reported trying foreign body ingestion once as a manipulative behavior 13 years before, learning it from fellow inmates while incarcerated on drug charges. His vitals and physical examination were benign, without signs of opioid withdrawal. Urinary toxicology showed marijuana, cocaine, and opioids. Mini-Mental State Examination and Montreal Cognitive Assessment scores were normal (29 and 30, respectively). Mental status examination demonstrated a well-dressed male, cooperative to interview, with appropriate eye contact and normal speech. He described his mood as depressed and angry, with congruent affect. The patient's thought content showed no suicidal or homicidal ideation, with linear, goal-oriented process. No perceptual distortions were elicited.
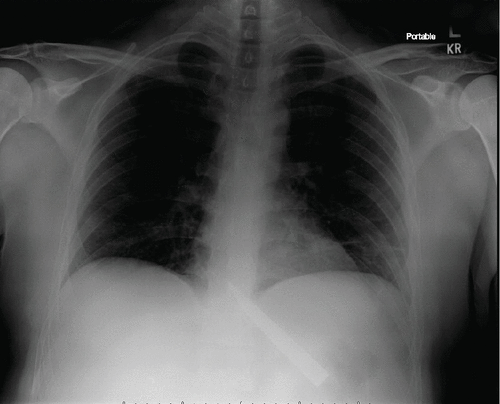
FIGURE 1. Emergency Room X-Ray of Patient Who Swallowed a 6-Inch Knifea
a The image is a portable chest X-ray of the patient, showing a 6-inch linear opacity overlying the spinal column and gastric bubble. (Courtesy of the SUNY Downstate Department of Radiology.)
Collateral from prior treatment programs revealed a 3-year period of stability at daily doses of methadone (190 mg–210 mg), sertraline (100 mg), and quetiapine (200 mg). Since he had inpatient-restricted Medicaid, his outpatient methadone treatment had not been paid. Subsequently, he had an administrative discharge from a methadone maintenance treatment program (MMTP) and a 6-week taper to 0 mg. After several weeks without treatment, he presented to our hospital for foreign body ingestion.
After endoscopic removal of the knife, he was started on sertraline (100 mg), quetiapine (200 mg), and methadone. The daily methadone dose was gradually increased, and we planned to refer him to an MMTP. Despite 2-to-1 observation, the patient locked himself in his bathroom and ingested three screws and a broken light bulb, since his physician only prescribed a 35-mg dose of methadone, whereas the consultant psychiatrist had recommended 40 mg (dosage confirmed by chart review). The objects perforated his gastric wall, requiring immediate laparotomy and repair. Even with this injury, when his demands for medication were not heeded or he feared that he might be discharged without referral to an MMTP, he would again ingest, with items ranging from screws and cabinet knobs to a pencil.
We hypothesized that Mr. A's recurrent foreign body ingestion was the result of exacerbation of his borderline personality traits secondary to the cessation of his opioid-agonist therapy. Once his methadone was titrated to 100 mg daily, episodes of foreign body ingestion ceased. He was discharged with appropriate Medicaid and referred to an MMTP.
Discussion
The above patient's initial foreign body ingestion was a pathologic manipulative response to ensure access to methadone, but it generalized to situations in which he felt frustrated, such as confrontations with nurses, surgical teams, and even housekeeping. A differential diagnosis for foreign body ingestion includes malingering, psychosis, and self-harm in patients with cluster B personality traits (7). Although Mr. A's aggression, drug history, and criminality suggested antisocial personality, his affective instability, idealization, and devaluation of medical staff and impulsive self-harm (in excess of what was necessary to remain hospitalized) indicated significant borderline personality traits.
Case reports have described cessation of self-mutilation of borderline patients using naltrexone and atypical antipsychotics, but to our knowledge the efficacy of methadone for this purpose has not been demonstrated (4, 5). Opioid addiction, manipulative parasuicidality, and psychiatric symptoms share neurological underpinnings. Self-injury can lead to release of endogenous opioids, creating an antinocioceptive state via altered µ-opioid receptor activity (8). Oyefeso et al. found 49% prevalence of alexithymia and self-harm (most commonly cutting) in a cohort of 80 opioid-addiction treatment patients, pointing toward a commonality between drug use and self-injurious methods for endogenous opioid release (6). A 2010 neuroimaging study of 18 sober, female borderline personality disorder patients showed increased µ-opioid receptors in the prefrontal cortex, nucleus accumbens, and amygdala (suggesting a resting opioid deficit), with paradoxically elevated endogenous opioid system activation during times of induced stress (9). Though the exclusion of male subjects and those with comorbid substance abuse disorders (within 3 months of positron emission tomography scan) limits this study's generalizability, it corroborates the model of opioid-deficiency in borderline personality disorder and suggests a mechanism for these patients' exaggerated stress response.
The neurological models previously illustrated beg the question of whether methadone could stabilize the opioid receptors of our borderline personality disorder patient. From his own reporting, as well as collateral information obtained from multiple sites (hospitals, outpatient treatment centers, police records, family members), it was clear that Mr. A was stable when receiving high doses of methadone. By restarting the high-dose methadone therapy, he returned to his non-impulsive, non-self-injurious baseline. Frankenberg et al. demonstrated opioid prescription rates in borderline personality disorder populations to be double that of patients with other axis II diagnoses. Though limited by size in the comparison group (borderline personality disorder patients: N=264 vs. axis II patients: N=63), this study suggests a neurological convergence of physical and psychical pain unique to the borderline personality disorder pathology that is assuaged by opioid therapy (10). These studies all offer possible explanations for Mr. A's period of psychiatric stability and substantiate the idea that he could return to baseline by resuming high-dose methadone.
A neurological commonality between parasuicidality and opioid use is tempered by the fact that by increasing Mr. A's methadone in response to his foreign body ingestion, we positively reinforced a maladaptive behavior. Nevertheless, this case makes clear the consequences of inappropriate methadone maintenance treatment cessation and the benefits of high-dose methadone maintenance treatment. Case studies of prisoners show elevated risk of re-incarceration and resumption of opioid use by patients previously on methadone maintenance treatment (1). Although withdrawal can be mitigated with as little as 20 mg of methadone, high-dose treatment (>80 mg) has been shown to more greatly reduce incidence of relapse and other drug use (8, 10) Methadone tapering is most successful in patients with stable housing, finances, and psychiatric well-being, conditions that Mr. A clearly did not meet (3). With the help of a multi-faceted team of social workers, physicians, and nursing staff, Mr. A was able to acquire temporary housing and was discharged to an MMTP, where it was agreed another taper would not be attempted.
Conclusions
Rapid taper of high-dose methadone therapy led a man with borderline personality traits to engage in repeated foreign body ingestion until his treatment was reinstated. This case illustrates the danger of behavioral destabilization if opioid agonist maintenance therapy is abruptly discontinued in such patients.
Key Points/Clinical Pearls
Opioid agonist maintenance can be an essential treatment for people receiving it, and too rapid taper risks psychiatric behavioral decompensation.
In addition to reducing opioid abuse and other drug use, methadone may curb impulsive and self-injurious behavior in patients with borderline personality traits.
Although withdrawal can be mitigated with as little as 20 mg of methadone, high-dose treatment (>80 mg) has been shown to more greatly reduce incidence of relapse and other drug use.
1. : Methadone dose at the time of release from prison significantly influences retention in treatment: implications from a pilot study of HIV-infected prisoners transitioning to the community in Malaysia. Drug Alcohol Depend 2013; 132(1–2):378–82 Crossref, Google Scholar
2. : Phases of treatment: a practical approach to methadone maintenance treatment. Int J Addict 1994; 29(2):135–160 Crossref, Google Scholar
3. : Slow tapering from methadone maintenance in a program encouraging indefinite maintenance. J Subst Abuse Treat 2006; 30(2):159–163 Crossref, Google Scholar
4. : Cessation of self-mutilation in a patient with borderline personality disorder treated with naltrexone. J Clin Psychiatry 1997; 58(1):32–33 Crossref, Google Scholar
5. : Remission of self-mutilation in a patient with borderline personality during risperidone therapy. J Nerv Ment Dis 1997; 185(5):348–349 Crossref, Google Scholar
6. : Self-injurious behaviour, traumatic life events and alexithymia among treatment-seeking opiate addicts: prevalence, pattern and correlates. Drug Alcohol Depend 2008; 98(3):227–234 Crossref, Google Scholar
7. : Foreign-body ingestion in patients with personality disorders. Psychosom 2007; 48(2):162–166 Crossref, Google Scholar
8. : Dynorphin promotes abnormal pain and spinal opioid antinociceptive tolerance. J Neurosci 2000; 20(18):7074–7079 Crossref, Google Scholar
9. : Dysregulation of regional endogenous opioid function in borderline personality disorder. Am J Psychiatry 2010; 167(8):925–933 Link, Google Scholar
10. : The use of prescription opioid medication by patients with borderline personality disorder and axis II comparison subjects: a 10-year follow-up study. J Clin Psychiatry 2014; 75(4):357–361 Crossref, Google Scholar



