The high prevalence of substance abuse in patients with schizophrenia has sometimes been interpreted as a means of self-medicating negative symptoms, anhedonia, depression, or neuroleptic side effects
(1). However, although preclinical
(2) and genetic studies
(3) have given some theoretical consistence to this theory, clinical studies have lead to discrepant conclusions. One hypothesis is that in nonschizophrenic patients, high levels of impulsivity
(4) and sensation seeking
(5) are associated with substance abuse, but this has been little studied in patients with schizophrenia. In limited samples, novelty seeking
(6) or disinhibition
(7) has been related to substance abuse. Our objective was to compare the occurrence of impulsivity, sensation seeking, and anhedonia in a group of patients with schizophrenia with and without lifetime substance abuse or dependence per DSM-III-R criteria.
Method
The study included 100 consecutively hospitalized inpatients (N=76) or outpatients (N=24) with diagnoses of schizophrenia (N=91) or schizoaffective disorder (N=9) according to DSM-III-R. The study was approved by the local ethics committee, and all subjects provided their informed consent. The psychoactive substance use disorders section of the Composite International Diagnostic Interview
(8) was used to make computerized DSM-III-R diagnoses of abuse of or dependence on alcohol, cannabis, amphetamines, sedatives, opioids, cocaine, hallucinogens, phencyclidine, inhalants, and other substances. Patients were assessed with the Positive and Negative Syndrome Scale for schizophrenic symptoms
(9), the Barratt Impulsivity Scale (a 34-item self-report)
(10), the Zuckerman Sensation Seeking Scale (form V) (a 40-item self-report)
(11), and the Chapman Physical Anhedonia Scale (a 61-item self-report)
(12).
Subjects with lifetime abuse or dependence (substance-abusing patients) were compared to subjects without abuse or dependence. Quantitative variables were studied by using analyses of covariance (ANCOVAs) adjusted on the basis of age and gender since these variables could be confounding factors. Since there was a statistical interaction between gender for Positive and Negative Syndrome Scale scores, we used these scores as covariates together with sex and group in a comparison of scores on the Barratt Impulsivity Scale and the Zuckerman Sensation Seeking Scale. Subjects without lifetime substance abuse were further compared to subjects with past abuse or dependence, defined by the disappearance of DSM-III-R criteria for abuse or dependence at least six months before assessment. All tests were two-tailed, with an alpha set at 0.05.
Results
Forty-one subjects had lifetime abuse or dependence for one (N=24) or more (N=17) substances, mainly alcohol (N=27) and cannabis (N=27). Cocaine dependence occurred in only one subject. Only eight subjects met the criteria for abuse. Thirty-three substance-abusing patients were male (80.5%) compared to 35 (59.3%) in the group without lifetime substance abuse or dependence (χ
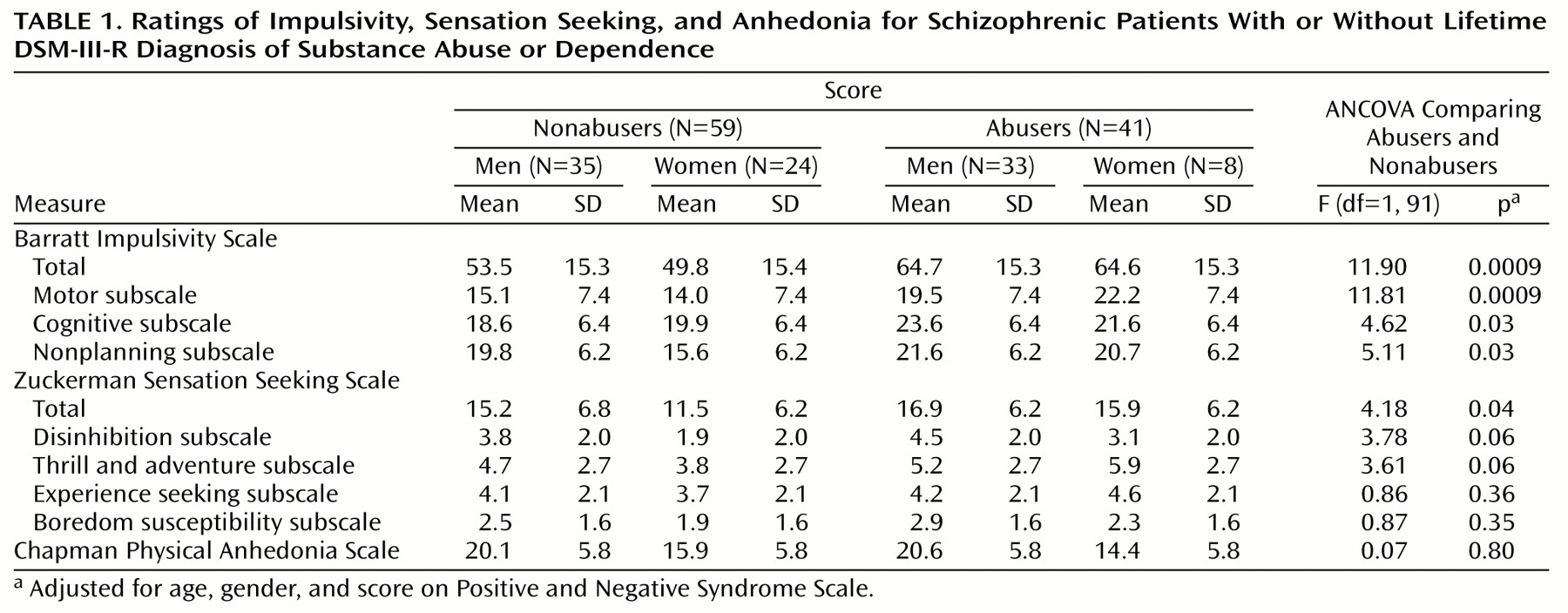
2=4.98, df=1, p=0.03), and the substance abusers were significantly younger (mean=31.3 years, SD=7.1, versus mean=37.1, SD=12.3) (ANCOVA, F=7.20, df=1, 96, p=0.009). No significant difference between the two groups was found for other demographic or clinical variables, including age of first psychiatric treatment, number of hospitalizations, and scores on the Positive and Negative Syndrome Scale and the Chapman Physical Anhedonia Scale. In the group with substance abuse, Barratt Impulsivity Scale and Sensation Seeking Scale scores were significantly higher than in the group without substance abuse (
Table 1).
In the past abuse or dependence subgroup (N=15), Barratt Impulsivity Scale scores were higher (men: N=10, mean=69.7, SD=11.5; women: N=5, mean=59.8, SD=9.9) than in the group without abuse or dependence (men: N=35, mean=53.5, SD=15.3; women: N=24, mean=49.8, SD=15.4) (ANCOVA, F=8.14, df=1, 66, p=0.006). Zuckerman Sensation Seeking Scale scores were also found to be higher in the subgroup with past abuse or dependence, but the difference did not reach statistical significance (ANCOVA, F=2.80, df=1, 66, p=0.09).
Discussion
Our results do not support the self-medication hypothesis of substance abuse in schizophrenia
(1). Indeed, substance-abusing patients were not significantly different from those without substance abuse with regard to physical anhedonia or scores on the Positive and Negative Syndrome Scale negative subscale or scores for anxiety or depression. The self-medication hypothesis has especially been suggested for cocaine abuse, which is less widespread in Europe than in North America for reasons of availability. Our results indicate that schizophrenic patients with a lifetime comorbidity of substance abuse or dependence are more impulsive and seek more intense sensations than schizophrenic patients without abuse or dependence. The persistence of higher scores on the Barratt Impulsivity Scale in the subgroup with past abuse or dependence suggests that impulsivity is not induced by alcohol or drugs, although no definitive conclusion can be reached. Our findings are consistent with those of Blanchard et al.
(7) and with those obtained by our group in an independent study (unpublished report by Gut-Fayand et al.): substance abuse in schizophrenic patients, as in nonschizophrenic patients, is related to personality components.
Several limitations to this study can be raised. First, the representativity of our study group can be challenged, although the exhaustive recruitment process limited the selection bias. Second, as in any retrospective study, the prevalence of lifetime substance abuse may have been underestimated, but urinary toxicology tests would not have been able to improve the detection of former substance abuse. A prospective longitudinal follow-up study of a cohort of adolescents, examining the occurrence of substance abuse and/or schizophrenia, would be more reliable but hardly feasible.
Conclusions
We suggest that impulsivity and sensation seeking are more clinically relevant than anhedonia as risk factors for substance abuse in schizophrenia. The nature of the link between the susceptibility to substance abuse and schizophrenia (common susceptibility or the addition of risk factors) remains to be identified.