Schizophrenia is accompanied by impairments in several domains of cognitive functioning (
1,
2,
3,
4,
5). Cognitive dysfunction has been found to be related to employment status and performance at work (
2,
6,
7,
8,
9,
10). Furthermore, disability in social functioning has been found to be related to work functioning (
9,
11).
Data on work functioning and cognition in schizophrenia has emerged mostly from developed countries. Work is an activity that is under considerable influence from environmental factors, including availability of employment and alternate sources of income. Reports on work functioning of patients with schizophrenia from developing counties have differed from such reports about patients from developed countries. Studies from India have shown that the annual rate of employment in a cohort of 90 patients with first-episode schizophrenia ranged between 63 and 73 percent during the first ten years of follow up (
12). In another study from India, among 43 male patients with schizophrenia who had never been treated, 35 percent were employed at the time that their schizophrenia was detected (
13); that percentage increased to 51 percent after one year of treatment with antipsychotics (
14). These rates of employment were distinctly higher than those found in a similar population in a developed country (
9,
15,
16). This discrepancy was attributed to differences in the social and economic environment, such as the lack of disability benefits compelling patients to work and contribute to the family's income (
12). It is possible that these social factors prevalent in India could modify the known association between cognition and work dysfunction observed in populations of a developed society.
We aimed to study the employment status and performance at work of patients with schizophrenia and to examine their relationship to performance on tests of cognitive function as well as clinical and demographic variables and measures of social functioning. This was a cross-sectional study of urban patients who attended a rehabilitation center in southern India.
Results
Study population
Employment before onset of illness or thereafter was not expected for 12 participants because they were full-time housewives or students. The data from the remaining 88 participants are presented here. The general demographic and clinical characteristics and work status of this population are presented in
Table 1.
Variables associated with employment status
Fifty-nine participants (67 percent) were employed. The ratio of men to women was similar among participants who were employed and those who were not (38 men, or 64 percent, and 21 women, or 36 percent, in the employed group, compared with 18 men, or 62 percent, and 11 women, or 37 percent, in the unemployed group). The proportion of persons who were married was comparable in the two groups (20 participants, or 34 percent, in the employed group, compared with five participants, or 17 percent, in the unemployed group). Employment before onset of illness was also comparable in the two groups (33 participants, or 56 percent, in the employed group, compared with 15 participants, or 52 percent, in the unemployed group). The groups did not differ significantly in the medication that they received (32 participants, or 54 percent, in the employed group received second-generation antipsychotics, compared with 21 participants, or 72 percent, in the unemployed group).
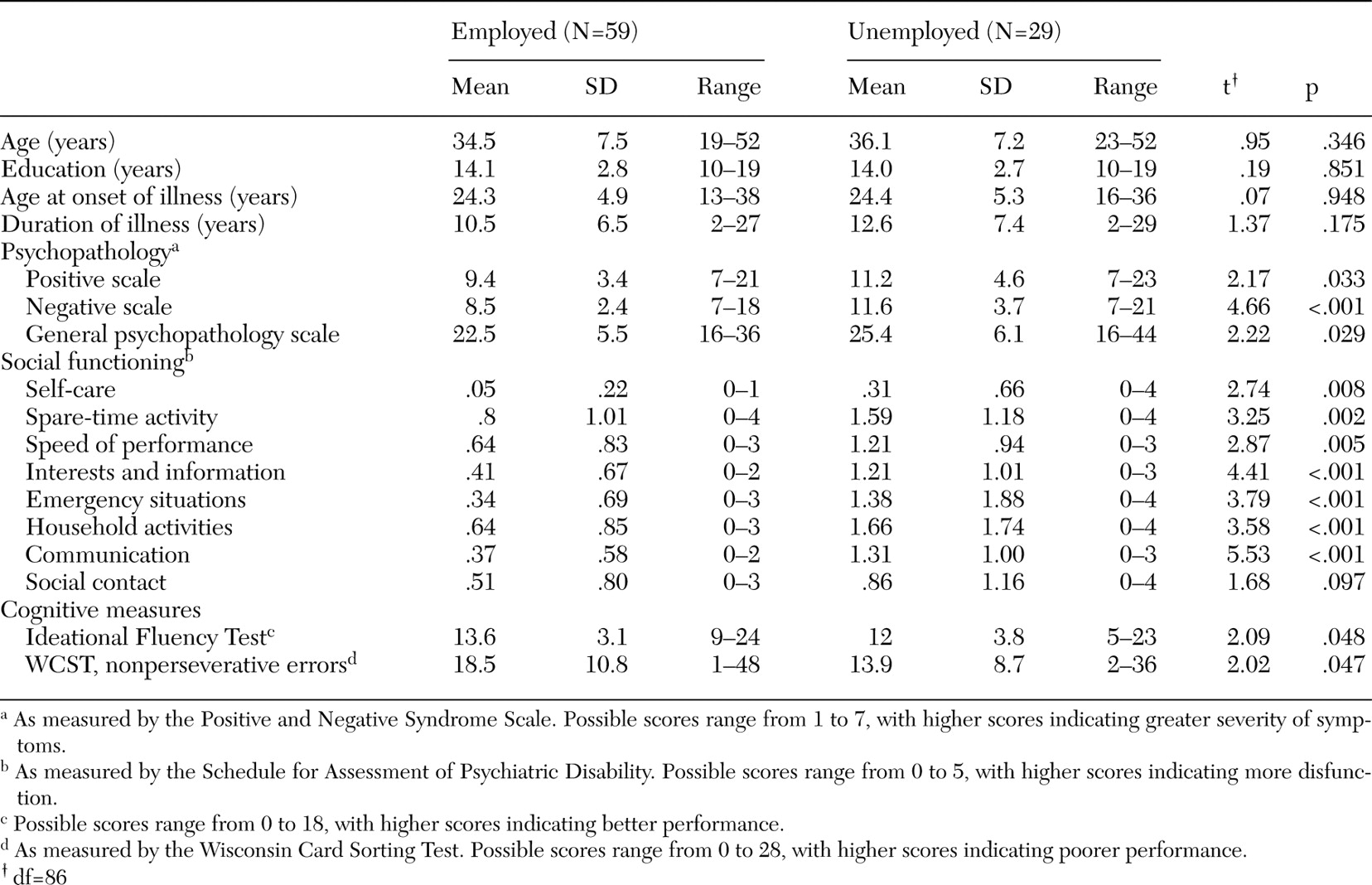
The comparison of the two groups on other variables is presented in
Table 2. Persons who were employed differed significantly from those who were not on the scores of all three subscales of PANSS and all measures of social functioning. They differed on two cognitive measures: ideational fluency and the number of nonperseverative errors on the Wisconsin Card Sorting Test. Scores on both of these two parameters were associated with employment status with an effect size (as an expression of strength of the association) of .45. The differences between the two groups on other neurocognitive measures were not significant. Two measures of attention (time taken on the visual scanning test and the forward digit span test) and some measures of memory (number of sets correctly responded to on the letter-number span test, delayed recall on the visual memory and learning test, and immediate and delayed recall on the visual reproduction and the visual paired-association tests) had a small effect size of .20 (
27). All other cognitive variables had effect sizes of less than .20.
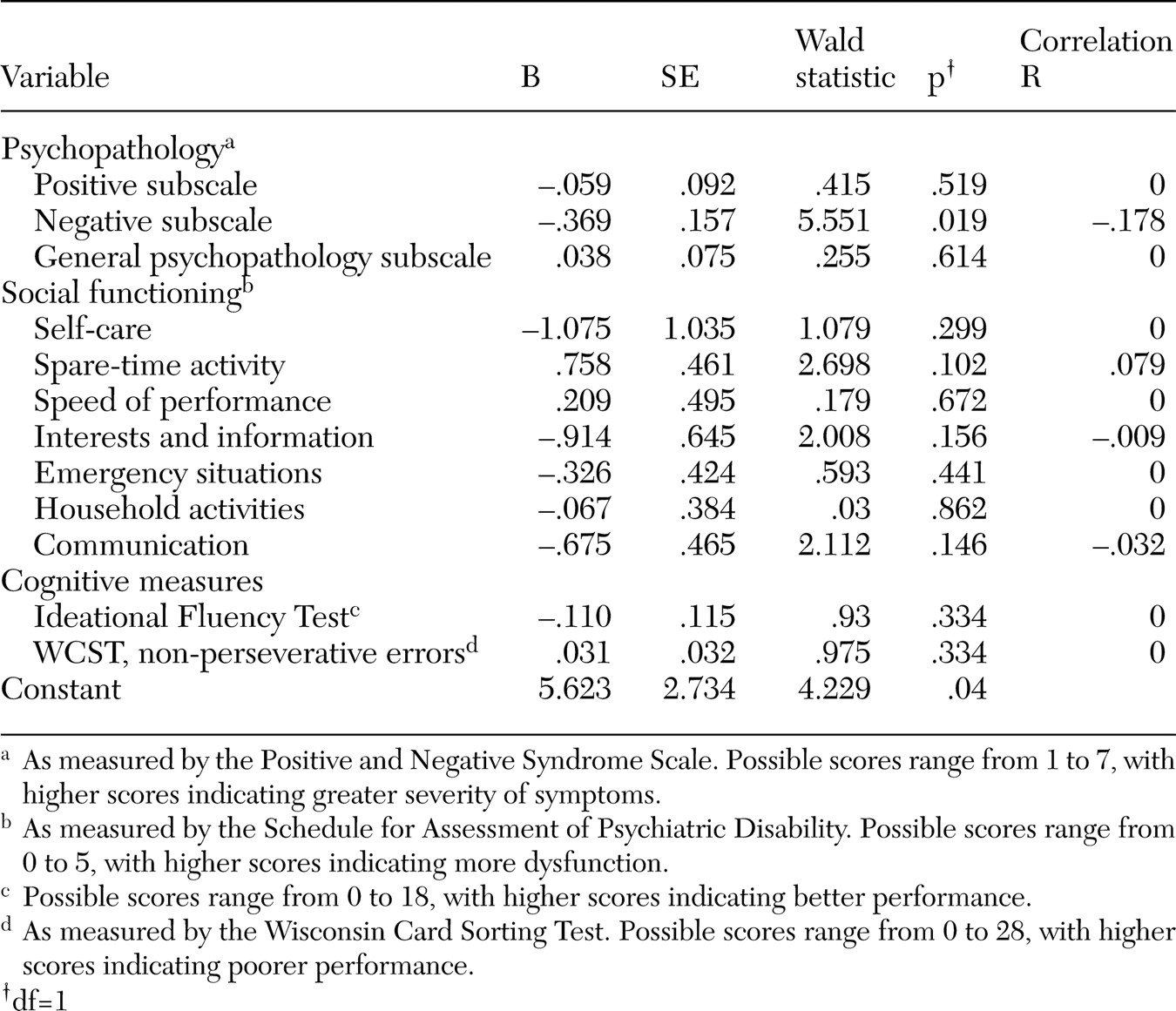
As shown in
Table 3, when logistic regression analysis was performed, the PANSS negative subscale was the only predictor of employment status among variables that were significant on univariate analysis. Abstract thinking, an item on the negative subscale, could be considered a cognitive function. When this item was entered into the analysis separately, the rest of the negative subscale was still the only significant factor (beta coefficient=-.334, SE=.162, Wald statistic=4.227, df=1, p=.040).
Variables associated with disability in work performance
Men and women did not differ in their mean±SD scores of disability in work performance (4.4±3.4 for men and 4.1±3.7 for women). Married patients had mean scores that were similar to those of single patients (3.4±2.9 for married patients and 4.7±3.5 for single patients). The degree of disability did not correlate significantly with age or years of education. Patients with a moderate or significant degree of poor performance had a history of poor work performance before illness more often than those with current good performance (five of eight participants with a history of poor work performance, or 63 percent, compared with five of 25 participants with a history of good work performance, or 20 percent; Fisher's exact two-tailed p=.036).
Disability in work performance correlated with mean scores on PANSS's positive subscale (r=.240, p=.024), negative subscale (r=.444, p<.001), and general psychopathology subscale (r=.277, p=.009) but not with age at onset or duration of illness. Patients who were given a prescription for a second-generation antipsychotic had greater disability in work functioning than patients who were given a prescription for a first-generation antipsychotic (a mean score of 4.9±3.5 compared with a mean score of 3.4±3.2; t=2.04, df=86, p=.044).
A significant positive correlation was seen between disability in work performance with the following domains of social functioning: self-care (r=.310, p=.003), spare-time activity (r=.394, p<.001), speed of performance (r=.369, p<.001), interests and information (r=.473, p<.001), emergency situations (r=.404, p<.001), household activities (r=.388, p<.001), and communication (r=.511, p<.001). The work disability did not correlate with measure of social contacts.
The degree of disability in current work performance correlated with scores on the visual learning and memory test, delayed recall (r=-.326, p=.05) and on the visual reproduction test, immediate recall (r=-.354, p=.01). No significant correlation was found between work disability and scores on other cognitive tests.
Among variables that were significant at univariate analysis, only two measures of social functioning—communication (β=.363, t=3.448, p=.001) and interests and information (β=.282, t=2.686, p=.009)—were predictive of work performance on the regression analysis. The two accounted for nearly 32 percent of the variation in disability (R2=.319; F=19.893, df=2, 85, p<.001).
Discussion
The study showed that negative symptoms and social functioning, but not cognitive deficits, were related to employment and disability in performance at work. The lack of a strong relationship between cognitive deficit and work functioning was in contrast to the available evidence. In univariate analysis, some of the cognitive tasks were related to employment status and work functioning. However, these factors were not significant when multivariate analysis was performed. The number of participants was small considering the number of variables entered into the regression analyses; this restriction placed a limitation on the extent to which the negative findings of the regression analysis can be firmly supported. Two other factors need to be considered in interpreting the observations. First, the study group, living in a large metropolitan city, had potentially a better opportunity to enter the workforce than a nonurban population. Second, the study center was a specialized center for schizophrenia rehabilitation. Selection of participants from this source could have included patients who had undergone successful intervention in terms of work rehabilitation. These two factors could have helped the participants to be employed and perform better despite the cognitive impairment.
In the regression analysis, the negative symptom score was the only variable that predicted current employment status. Isolation of a putative cognitive item from the negative subscale did not alter this relationship. The relationship between negative symptoms and poor work outcomes has been well established in other studies (
28,
29,
30). Studies have identified negative symptoms (
29) or cognitive deficits (
6) or both as contributing to poor work outcomes (
8,
30).
As has been shown in other studies, (
9,
11,
12), we found that disability in social functioning in schizophrenia was related to work functioning. Social competence may help in securing and maintaining jobs (
11). Measures of social functioning in two domains—the communication domain and the interests and information domain—strongly predicted work performance in this study. The communication domain measured the patient's communicative ability, which would be essential to get a job and maintain a good level of functioning on the job. The interests and information domain measured the individual's general level of motivation and drive to engage in social activity, which would also come into play in the work situation. Social functioning may reflect a core motivational characteristic that is often impaired among persons with schizophrenia. Patients who were motivated by social contact and leisure activities were more interested in work (
9).
A note on the work environment of the study population will give a better perspective. In our study all but eight participants were working in mainstream competitive environment: four patients were working in family establishments and were not paid and four were working in sheltered employment. Participants had various jobs—such as a data entry clerk, proofreader, and security guard, which involve monotonous work—as well as jobs in health care, teaching, and marketing, which involve multitasking and require a significant level of work and social skills. Some participants worked in 9-to-5 jobs, and others (for example, manual workers and professionals) worked longer hours. Patients who were employed in regular jobs in the organized sector more freely used their sick-leave benefits. People performing below par in productivity-linked jobs in the unorganized sector did not always lose their jobs, but they received payment according to the work output. Some patients' families employed them in family establishments. These patients did not earn a wage but were productively employed. People were generally supportive of the patients at work. The education, past abilities, and social and economic background was given some credence, and this support often helped patients get and maintain jobs and provided a milieu for better performance. Some patients were able to keep their employment because their colleagues did not make an issue of their social and behavioral oddities and often supported them on assigned duties.
The large number of patients who faced full responsibility with little or no support at work could lead to questions about whether many of the patients had adequate cognitive functioning. Compared with a matched control population, the study population performed poorly on all the neuropsychological tests with medium to large effect size (data not shown). Hence the lack of a significant relationship between cognition and work functioning was not due to better cognitive ability of the population.
The number of years of formal education among our patients was notable; many patients (52 participants, or 62 percent) had completed 15 years. The high level of education of this urban population could have favored their chances of getting a job in the employment market. Although education did not emerge as a contributor to employment in this study, we believe it was a factor to reckon with. Completion of many years of academic training was also indicative of premorbid intellectual functioning and use of a high level of information processing skills in the past. The patients probably did well in work because of this inherent capability that helped them overcome any cognitive deficit of the psychosis. A parallel can be drawn with clinical manifestation of cognitive decline in neurodegenerative disorders. Years of education influenced the relationship between neuropathological changes in Alzheimer's disease and cognitive function (
31). Mental stimulation occurring with many years of education delayed clinical expression of cognitive deficits in such diseases by maintaining global cognitive efficiency through enhancement of certain cognitive processes (
32).
Economic pressure may be one other reason that many patients were employed despite cognitive impairments. Most families provided accommodation and care, but this was a heavy burden if the patient was not contributing financially. This burden was significant in the absence of financial support from the state to the mentally disabled, support that can be found in developed countries. This economic pressure, along with the motivational push from the family, may have motivated patients to seek a job and perform adequately despite cognitive dysfunction.