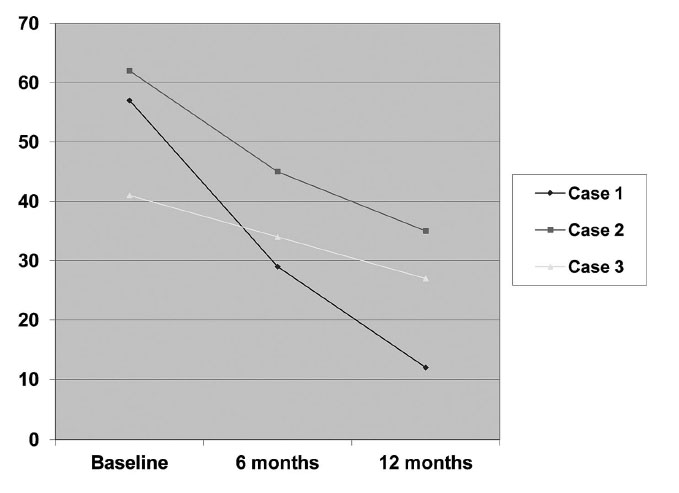
Results
Case 1
Ms. A. was a 33-year-old Caucasian female with a history of chronic major depression, severe dissociation, and narcissistic and borderline personality disorders. She started DDP with a psychiatric resident trainee after several years of recurrent psychiatric admissions for depression, suicidal attempts, and self-mutilation. She would whip herself with chains and used torture devices with religious/medieval themes. She had twice required cardiac resuscitation after overdoses.
Ms. A. also described multiple dissociative symptoms that occurred on a frequent basis. These included flashbacks of traumatic experiences, psychogenic amnesia of important events, derealization, depersonalization, and lapses in time. In addition, the patient described having three separate alters, each having a different name, age, and characteristics. On admission her DES score was 57.
Ms. A. stated her childhood was saddened by her father leaving home when she was about 3 years old; she spent most of her childhood awaiting his return. She vividly recalls feeling alone and spending hours in a rocking in a chair staring at a wall.
Her mother remarried a man who sexually abused Ms. A.’s younger brother and older sister and physically abused Ms. A. When the children revealed the abuse to their mother, she sought counseling at their church, which recommended therapy and that he remain in the home. Ms. A. felt betrayed by her mother for allowing the terror in the home to continue. Ms. A. could not recall feeling loved by her mother, who was a nurse and busy portraying herself a caring individual for others.
Ms. A. did well in school despite having chronic dissociative symptoms, she described as “spacing out” and feeling detached from the world. She enjoyed writing, and she pursued her interest in literature.
Ms. A. became pregnant during her senior year of high school, married, and had a second child. She had difficulties recalling most of her married life, but remembered her husband as being demanding and unloving. Eventually, her husband left her for her best friend.
Initially Ms. A. took on raising the two children on her own, but she was unable to work or even to talk on the telephone due to anxiety. Because of her prolonged periods of dissociation, she was unable to provide adequate and safe care for her children; Child Protective Services eventually removed them from her custody. They went to live with their father in another state. Ms. A. lost contact with her children because they refused to communicate with her.
Ms. A. engaged well in treatment with DDP, attending weekly sessions and developing a therapeutic alliance over the first few months. Much of her early treatment focused on her relationship with her mother, with whom she was living. The predominant theme was, “Do I have a right to be angry?”
She was angry at her mother for her behaviors and attitudes; her mother sympathized with Ms. A.’s ex-husband, insisted that Ms. A. use bed sheets and clothing stained with blood from Ms. A.’s prior cutting episodes, and discouraged her from attending psychotherapy.
At 6 months of therapy, Ms. A. had developed a strongly positive and somewhat dependent transference with the therapist, and she was much better at identifying and articulating feelings of anger, guilt, and shame. She also felt much less need to punish herself, and self-mutilating episodes became less frequent and less severe. Her DES score had decreased from 57 at baseline to 29 at 6 months. However, during therapist vacations, feelings of abandonment would surface in Ms. A., and these sometimes resulted in an exacerbation of self-mutilation and/or severe depression needing hospitalization.
During the final 6 months of therapy, Ms. A. focused a great deal on the preset planned termination of treatment. Vacations and the pending termination were reminders of the limitations of the therapist as an all-caring idealized object. On the one hand, Ms. A. felt as if she had a more integrated self, and she was beginning to expand her functional capacity through the formation of friendships and returning to school part-time. On the other hand, she felt abandoned by the therapist, and this was accompanied with exacerbations of depression, as Ms. A. redirected the anger towards her therapist onto herself. Ms. A. expressed worries about the future and she devalued treatment and the therapist’s role. The therapist struggled to remain empathic with Ms. A.’s worries (without giving false reassurance) and to tolerate the devaluation without becoming defensive.
By the end of treatment, Ms. A. appeared to have a more balanced view of her treatment and of herself. She could express anger with less internal hatred. Depression and suicide ideation markedly improved and 12-month DES score was 12. At termination, she gave the therapist a drawing of a Celtic knot to symbolize the integration of her disconnected self. She was transferred to the care of another therapist; the exact nature of her treatment and course is unknown. However, a chance encounter with the DDP therapist 5 years later revealed that Ms. A. was generally doing well and participating in part-time college coursework.
Case 2
Ms. B. was a married Caucasian female in her 30s with a long history of severe psychopathology. She delineated five alters, each with a separate name, gender, and age. She was unable to control unexpectedly switching between alters. Ms. B. also described frequent disruptive and embarrassing time lapses. On two occasions, these lapses occurred while she was in the changing room of a Department store: she would become aware of her surroundings after the store had closed and locked its doors.
In addition to dissociative symptoms, the client met criteria for multiple Axis I and II disorders, including BPD, Bipolar I, alcohol and drug dependence, post traumatic stress disorder, obsessive compulsive disorder, and anorexia nervosa, bingeing/purging type. She had a history of six psychiatric hospitalizations beginning in her early twenties; she was treated for suicide attempts, manic episodes, and/or psychosis.
Over the course of her illness, Ms. B. had tried multiple classes of psychotropic medications none successes in treatment, but she has some improvement with mood stabilizers and antipsychotic medications. She had been treated for 5 years in twice-weekly supportive psychotherapy, which had involved a progressively pathological and regressive client-therapist relationship, including cuddling and playing with blocks on the floor. As the client regressed, she also became intrusively demanding of her therapist’s time, which eventually led to the therapist terminating treatment and subsequent deterioration in the client’s condition.
Ms. B. began to see demons in her house, and develop paranoid delusions necessitating psychiatric hospitalization. Following hospitalization, the client was referred for a trial of DDP. At that time, her DES score was 62. Initial sessions focused on establishing clear parameters of treatment, boundary limitations within the client-therapist relationship, and psycho-education regarding the importance of avoiding boundary violations. The client repeatedly brought up interactions with her prior therapist, including her feeling abandoned by the therapist. She was able to work through conflicts regarding agency, i.e. if she or her therapist was to blame for various incidents. As the client gradually worked through her issues she had with her prior therapist, the focus shifted to her marital relationship. Her husband was extremely physically and emotionally abusive. He had prostituted her to his friends and acquaintances. Episodes of physical abuse would be followed by increased psychiatric symptoms, including dissociation. The DDP therapist helped the client identify, label, and acknowledge her emotions in interactions with her husband, and to work through her conflict of agency in that relationship, i.e. whether or not she provoked him to attack her. As Ms. B. worked this through, she decided to terminate the relationship with her husband. She temporarily lived with her parents and eventually lived independently. There was a mourning process involving de-idealization of her husband and of her parents, who pressured her to return to her husband.
Her symptoms of Axis I disorders steadily improved during the course of treatment, despite diminishing dosages of antipsychotic and mood stabilizer medications. Her symptoms of dissociation also improved and her DES score decreased to 45 by 6 months of treatment and to 35 by 12 months. Ms. B. described time lapses as less frequent and of shorter duration, and she began to sense an increased ability to control them. Shifts in personality style became less frequent and pronounced, and Ms. B. no longer described herself as having independent personalities, but rather described “parts of herself” that emerged at different times. She also described herself as “waking up” and feeling “more whole.”
As termination approached, the last phase of weekly treatment was difficult and involved working through feelings of abandonment. After 18 months of weekly sessions, monthly maintenance treatment, which was primarily supportive in nature, was initiated. Despite discontinuing all medications against advice 6 months after termination of weekly DDP, Ms. B. displayed gradual improvement in symptoms at 8-year post-treatment, however, she continued monthly supportive psychotherapy sessions.
During the follow-up period, Ms. B. decided to pursue a professional degree while on social security disability, which supported her efforts through Vocational and Educational Services for Individuals with Disabilities. She successfully completed her courses, came off disability, and has worked full time for the last 3 years of her follow-up period in a responsible professional position.
Case 3
Ms. C. was a divorced African American woman in her 30s, having a history of alcohol and cocaine dependence. She had moved to the area to “get clean” and leave negative influences. She heard about the study for co-occurring BPD and alcohol use disorders (
Gregory et al., 2008), and subsequently enrolled and was randomized to DDP.
Ms. C. described lifelong difficulties with sudden shifts in mood and personality combined with impulsive behaviors, including misuse of alcohol, cocaine, and cannabis. Significant dissociative symptoms included frequent episodes of derealization, feelings of spaciness, fugue episodes, and three distinct personalities, each with a specific name. One of her alters was called “Sunlight.” Sunlight had been the primary alter in Ms. C.’s life for the past few years. Sunlight enjoyed dominating and manipulating men as a drug dealer and prostitute. Unlike Ms. C., Sunlight felt no emotional pain and saw no need for treatment.
Ms. C. was diagnosed with cocaine, alcohol and cannabis dependence, DID, and BPD at evaluation. An 18-month course of DDP therapy was planned. Her initial DES score was 41. Throughout treatment, the therapist addressed the client by her legal name, and reframed the different personalities as different being parts of Ms. C. that were poorly integrated. The focus in early treatment was an exploration of a series of tumultuous relationships with boyfriends. These men had histories of imprisonment and tended to be manipulative or threatening. Her relational pattern was initially to idealize the men. This was followed by disappointment, anger, and fear. She would then engage in manipulating or controlling them. In therapy, the client was able to identify, label, and acknowledge conflicting feelings towards them and to describe a core conflict between her desire to be taken care of by a strong man versus her desire to be independent and in control.
By 6 months in treatment, dissociative episodes were much improved; DES score was 34. Ms. C. was maintaining abstinence and she was able to avoid harmful relationships with men. She began to develop female friendships for the first time in her life and to pursue educational courses leading up to a professional degree.
By 9 months, Ms. C. began to take responsibility for her life but was felt overwhelmed by responsibilities. She became less committed to treatment and recovery, and she began to have increased cravings for substances along with drug dreams. She would speak glowingly about times in the past when she felt in control and without emotional pain in the role of Sunlight. Much of the remaining 6 months of treatment involved bringing Ms. C.’s ambivalence about recovery to consciousness and helping her to mourn the loss of grandiose fantasies. Ms. C. also had to mourn the loss of the therapy relationship. She left treatment 3 months before the scheduled termination so that she “wouldn’t have to say goodbye.” As part of the BPD and alcohol use disorder study, Ms. C. met with the research assistant for follow-up 30 months after enrollment (
Gregory et al., 2010). She remained abstinent during the follow-up period despite lack of further treatment, finished her course work for a professional degree, and had been working fulltime during the last 12 months of the follow-up period.