Despite advances in pharmacotherapy, rates of attempted and completed suicide remain inordinately high among persons with bipolar disorder (
1). Much of this elevated risk of suicidality appears to be driven by depression (
2,
3) and mixed mania (
4)—clinical states for which existing treatments are often suboptimal. Standard antidepressants are often presumed to reduce suicide risk, with comparable efficacy among patients with either bipolar disorder or unipolar disorder (
5). However, in the absence of controlled trials, the utility of long-term antidepressants for bipolar disorder remains subject to debate. Further investigations are needed to help clarify the relationships between pharmacotherapy and suicidality among patients with bipolar disorder.
The extent to which clinicians prescribe medications for bipolar disorder according to practice guideline recommendations or evidence-based algorithms is controversial (
6–
9). Suicidality as a target symptom represents one clinical variable of growing importance in prescribing decisions. Understandably, a considerable literature has emerged regarding the antisuicidal properties associated with some psychotropic drugs (
10). Perhaps most notably, a six- to eight-fold reduction in the risk of suicide attempt or completion has been attributed to lithium therapy (
11). Ahrens and Muller-Oerlinhausen (
12) found this association to be independent of lithium’s prophylactic benefit for affective episodes; however, these investigators did not control for antidepressant exposure. Angst and colleagues (
1) found a protective effect for antidepressants and the combination of antidepressants or neuroleptics and lithium but not of lithium alone.
It is inherently difficult to study suicide prospectively, given the low ratio of events to patient years, and even more difficult to conduct studies in randomized comparator trials. To provide a description of community-based pharmacotherapy treatments relative to suicidal ideation, in this article we report cross-sectional rates of suicidal ideation and use of psychotropic medications in a large, well-characterized group of patients with bipolar disorder upon their entry into a multisite outpatient study. The study examined the prevalence of prescriptions for mood stabilizers, second-generation antipsychotics, and antidepressants and the clinical features of patients who received these different classes of medications.
Results
The mean ± SD age of the study participants was 40.6 ± 2.7 years. Of the 1,000 patients, 588 (59 percent) were women, 919 (92 percent) were Caucasian, 39 (4 percent) were African American, 11 (1 percent) were Asian American, 74 (.8 percent) were Native American, and 25 (2.5 percent) were of other ethnic origins. Participants were classified as having bipolar disorder type I (710 participants, or 71 percent), bipolar disorder type II (239 participants, or 24 percent), bipolar disorder not otherwise specified (41 participants, or 4 percent), schizoaffective bipolar disorder (seven participants, or .7 percent), or “bipolar other” (cyclothymic disorder) (three participants, or .3 percent).
At the time of study entry, 605 (61 percent) of 998 participants were euthymic, 58 (6 percent) were manic or hypomanic, 87 (9 percent) were mixed or cycling, and 248 (25 percent) were depressed; two patients did not provide complete data on syndromal status and suicidal ideation. Among this group, 211 (21 percent) exhibited signs of suicidal ideation on the ADE. Suicidal ideation was significantly more common among persons who were experiencing depressed (49 percent) or mixed (47 percent) episodes than among those who were manic or hypomanic (9 percent) or who were euthymic (7 percent) (χ2 = 224.198, df = 3, p < .001).
Pharmacotherapy at study intake
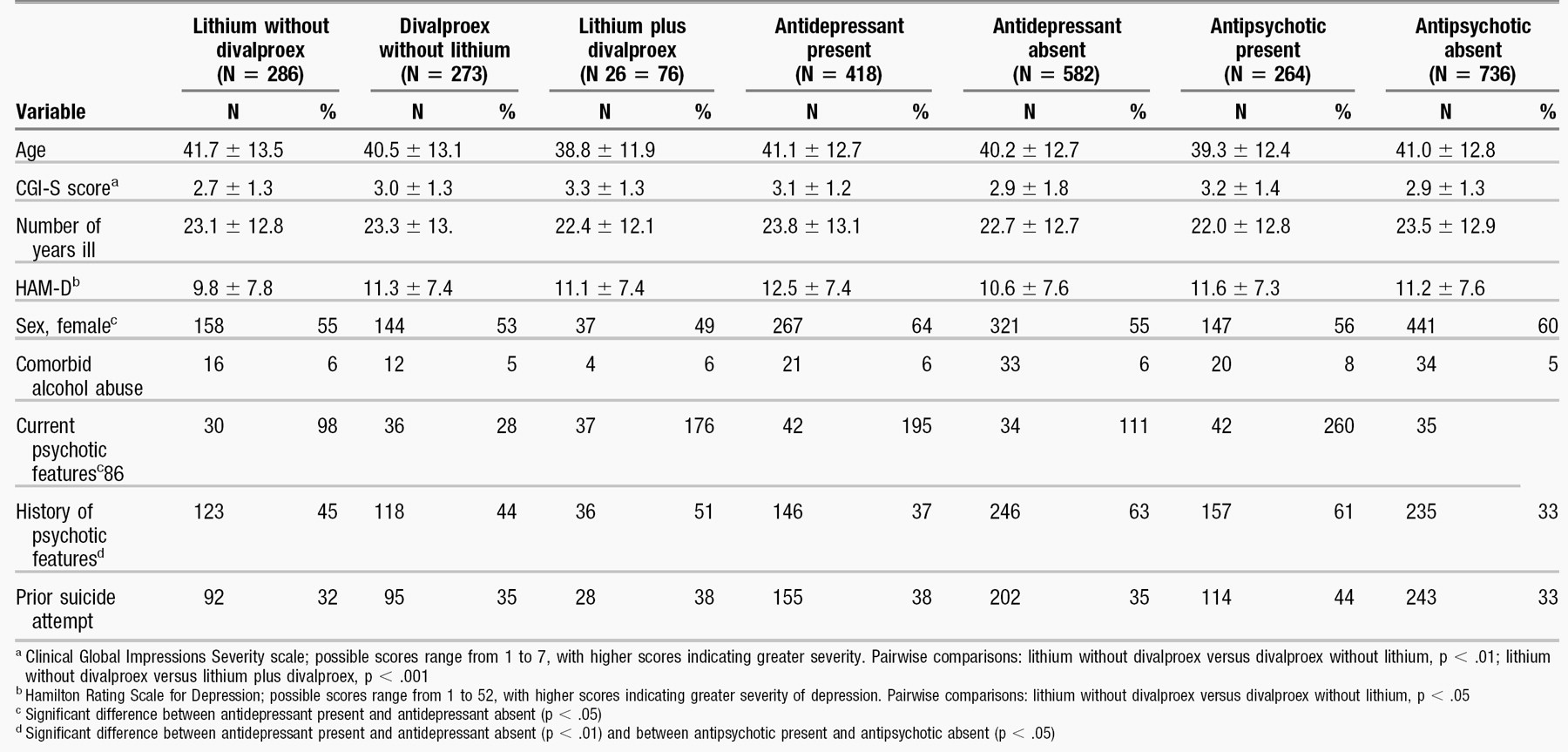
Most participants (849, or 85 percent) were taking psychotropic medications at the time of study entry. Clinical characteristics of participants across medication groups are summarized in Table 1.
A total of 362 participants (36 percent) were taking lithium (overall mean ± SD dosage, 944.8 ± 383.2 mg/day), and 349 (35 percent) were taking divalproex (overall mean ± SD dosage, 1,181.9 ± 578.4 mg/day). A total of 270 persons (27 percent) were taking antipsychotics; nearly all were taking second-generation agents (264 persons). About two-thirds of the participants who were taking a secondgeneration antipsychotic were also taking lithium or divalproex (174 of 264, or 66 percent). Specific agents included olanzapine (135 participants; mean ± SD dosage, 10.7 ± 10.5 mg/day), risperidone (73 participants; 3.9 ± 14.9 mg/day), quetiapine (47 participants; 150.0 ± 134.6 mg/day), ziprasidone (two participants; 90.0 ± 99.0 mg/day), and clozapine (seven participants; 197.0 ± 157.7 mg/day).
A total of 418 participants (42 percent) were taking an antidepressant (346, or 83 percent, were taking one antidepressant, and 72, or 17 percent, were taking at least two antidepressants) at study entry. Specific antidepressants or subclasses included bupropion (143 participants), selective serotonin re-uptake inhibitors (239 participants), venlafaxine (61 participants), mirtazapine (17 participants), nefazodone (29 participants), and monoamine oxidase inhibitors (six participants).
Suicidal ideation and treatment at study entry
Rates of suicidal ideation were similar between participants who were taking any lithium and those who were not (80 of 361 participants, or 22 percent, and 131 of 638 participants, or 26 percent, respectively) and were similar between those who were and those who were not taking any divalproex (71 of 349 participants, or 20 percent, and 140 of 650 participants, or 22 percent, respectively). Mean ± SD lithium dosages did not differ significantly between patients with suicidal ideation (909.5 ± 408.4 mg/day) and those without (954.7 ± 376.5 mg/day), and there were no differences between those who were suicidal and those who were not in mean ± SD divalproex dosages (1,209.7 ± 741.9 compared with 1,174.8 ± 530.0 mg/day, respectively).
The mean ± SD number of medications being prescribed for patients with suicidal ideation—including multiple antidepressants, second-generation antipsychotics, and psychotropics in addition to lithium or divalproex—was significantly higher than for patients without suicidal ideation (1.64 ± .96 and 1.41 ± .96, respectively; Kruskal-Wallis χ2 = 11.64, df = 1, p = .001). Multinomial regression adjusted for the effects of baseline HAM-D and GAF scores on the relationship between suicidal ideation and the number of medication groups (lithium, divalproex, second-generation antipsychotics, or antidepressants). Compared with persons who did not have suicidal ideation, those with suicidal ideation were more likely to be taking medications from two of these groups (p = .004) or three of these groups (p = .040) but not from all four groups.
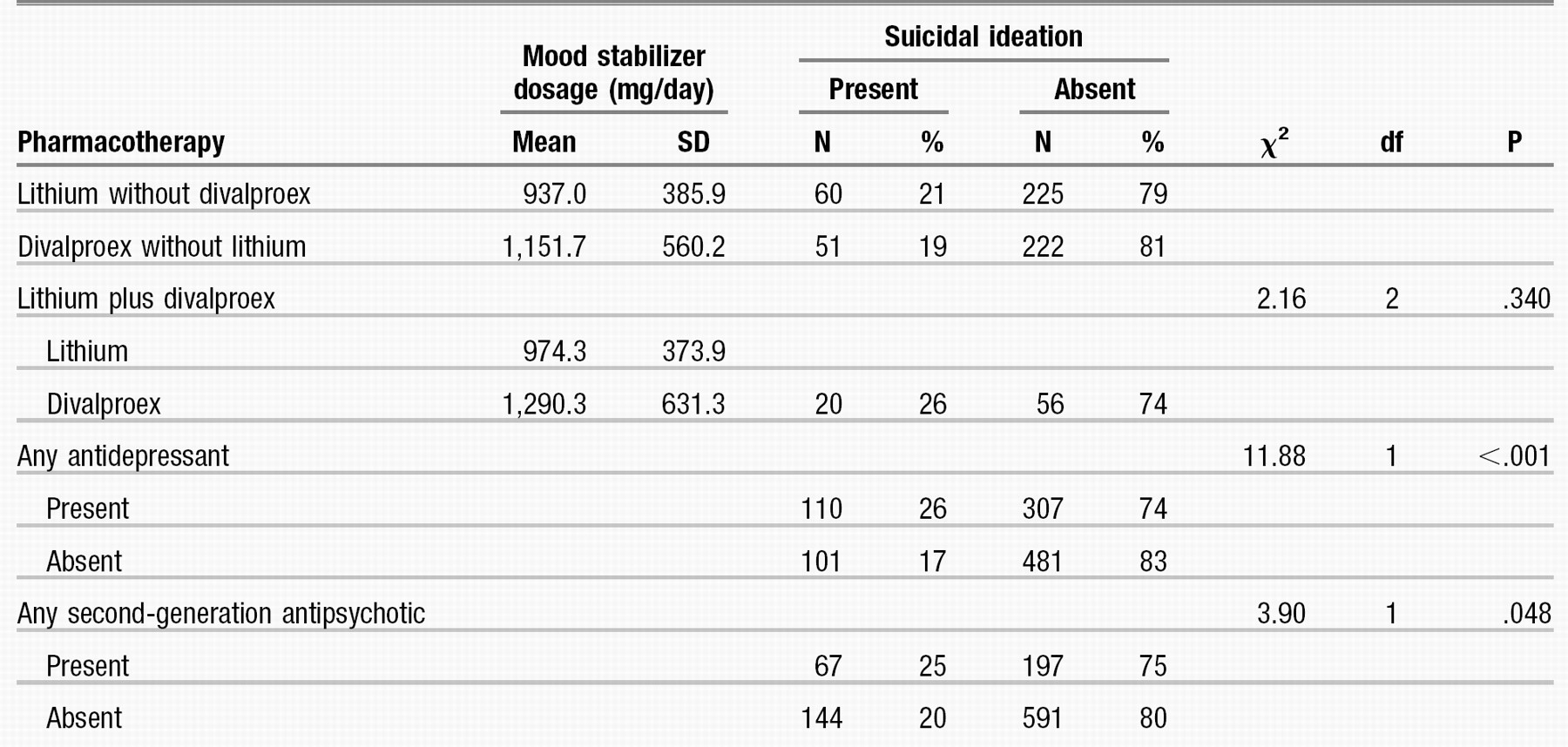
Table 2 summarizes the proportions of study participants with and without suicidal ideation by medication groups. No significant differences in suicidal ideation were found across mood stabilizer combinations. Suicidal patients were more likely than nonsuicidal patients to have been taking an antidepressant (p < .001) or an antipsychotic (p < .05).
A logistic regression model was used to examine the strength of association between medication groups and patient characteristics (those that showed variation across medication groups) and the presence or absence of suicidal ideation (the dependent variable). Variables from Table 1 for which p was less than .10 were chosen for entry into the regression model.
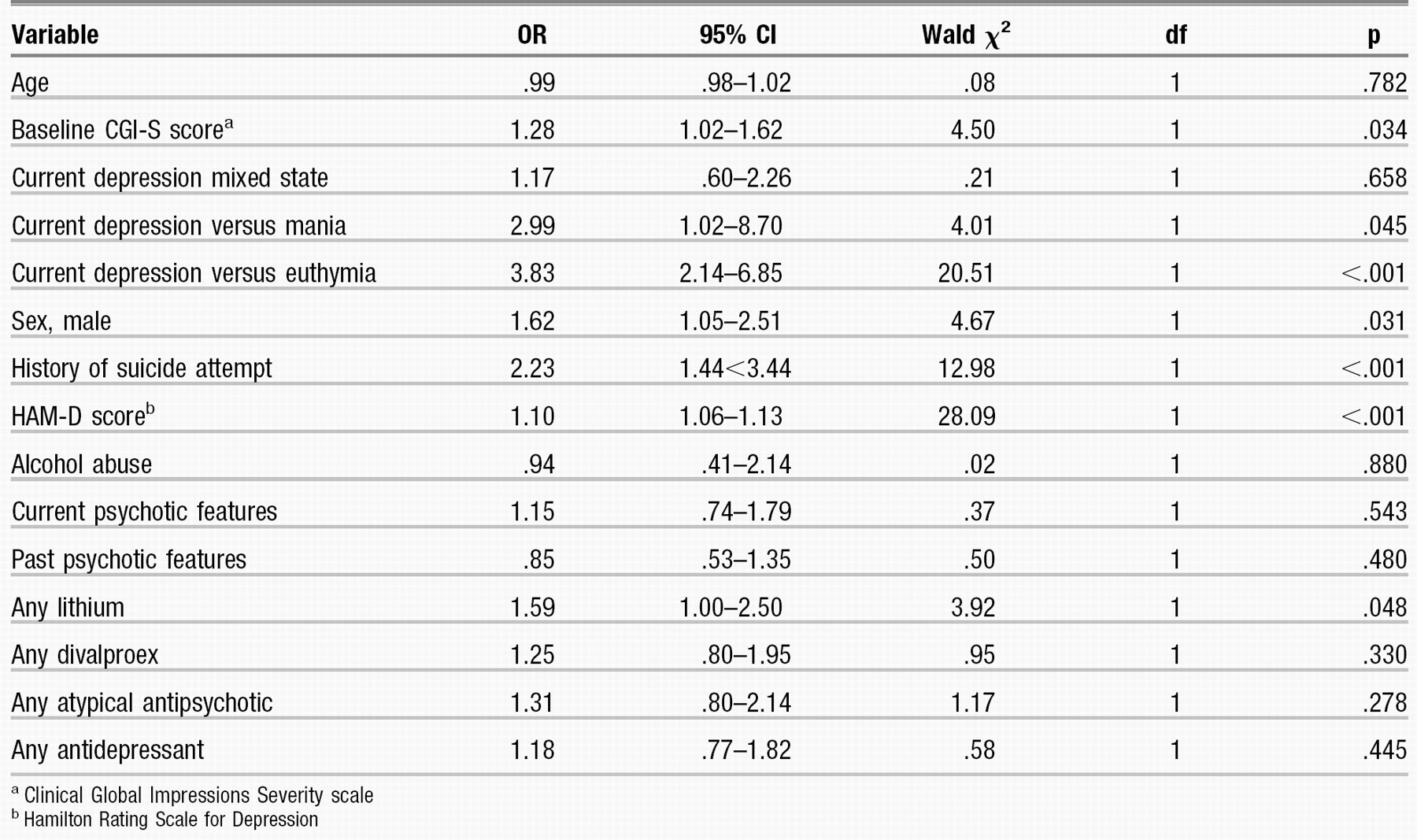
As shown in Table 3, significant associations were evident between the presence of suicidal ideation and global severity of illness, current depressive episode, severity of current depression, a history of suicide attempts, and male gender (p < .05 for all). Use of lithium was significantly associated with suicidal ideation after these factors were controlled for, whereas no significant associations emerged between suicidal ideation and the use of divalproex, second-generation antipsychotics, or antidepressants.
Separate analyses were conducted to examine possible interactions between current HAM-D scores and lithium use relative to current suicidal ideation. In this model, HAM-D was highly associated with suicidal ideation (Wald χ2 = 65.94, df = 1, p < .001), and lithium use was not, and there was no significant interaction. There also was no significant interaction between lithium use and a history of suicide attempts in predicting current suicidal ideation; a past suicide attempt in itself was significantly associated with current suicidal ideation (Wald χ2 = 18.70, df = 1, p < .001), but lithium use was not.
Discussion
In this large cohort of patients with bipolar disorder who were evaluated at the time of entry into a specialized research-based treatment program, about one-fifth had suicidal ideation contemporaneous with taking lithium, divalproex, or a combination of the two. Atypical antipsychotics and antidepressants were both more likely to be taken by suicidal patients with bipolar disorder overall, although these distinctions were not maintained after baseline severity of illness characteristics and suicide attempt histories were controlled for.
Limitations of this study include the cross-sectional (rather than longitudinal) design, as well as the lack of control for treatment assignment, duration of treatment, and medication adherence. Although we report findings on practice patterns, causal inferences about treatment use and suicidality cannot be drawn.
Univariate analyses indicated that patients who were suicidal at study entry were more often receiving antidepressants or second-generation antipsychotics than patients without suicidal ideation. However, after suicidal patients’ higher levels of illness severity, depression, and past suicide attempts were accounted for, practitioners were actually somewhat more likely than expected to prescribe lithium.
Our findings suggest that, after use of other medications and baseline severity indices were controlled for (such as severity of illness and history of suicide attempts), psychiatrists may be more likely to prescribe lithium for suicidal patients with bipolar disorder. It is possible that community practitioners will initially favor using antidepressants and second-generation antipsychotics for depressed patients with bipolar disorder who have suicidal features and reserve lithium for when greater signs of illness severity are present. However, the lack of an observed interaction between lithium use and current depressive severity or past suicide attempts relative to current suicidal ideation suggests that other factors mediate decisions about when to prescribe lithium for outpatients with bipolar disorder who have suicidal features. One could speculate that such factors might involve the degree to which practitioners may be apprehensive about the potential for lithium overdose, a preference for first using other medications with less narrow therapeutic indices or less intensive monitoring, and possibly an assumption that antidepressants are preferable to mood stabilizers among depressed and suicidal patients with bipolar disorder.
Although reports of the potential antisuicidal benefits of lithium are extensive, the data in this area derive mainly from uncontrolled studies that did not account for factors such as concomitant use of other medications (for example, antidepressants), rates and reasons for attrition, and clinicians’ prescribing biases (for example, concerns about lethality in overdose) (
10). As in the study we report here, Coryell and associates (
26) found that lithium therapy was more common among persons who attempted or completed suicide than among those who did not attempt suicide. In addition, Angst and colleagues (
1) found during a 34- to 38-year follow-up period that significantly fewer suicide completions occurred among patients with mood disorders who took lithium plus antidepressants, but no such reduction was evident among those who took lithium alone.
Only two prospective long-term randomized trials have specifically assessed suicide risk with lithium compared with an active comparator: Thies-Flechtner and colleagues (
27), over a 2.5-year study of 378 patients with bipolar disorder, unipolar disorder, or schizoaffective disorder, found significantly more suicide attempts or completions with carbamazepine (nine patients) than with lithium (zero patients). Prien and colleagues (
28), over a two-year period in which they studied 205 patients with bipolar disorder, observed no suicide completions with lithium or imipramine, compared with two completions in a placebo group. A recent meta-analysis of controlled trials of lithium use among patients with mood disorders showed a significant reduction in suicide deaths and deliberate self-harm (
29), although the possibility exists that the optimal antisuicide effects of lithium become attenuated under conditions of ordinary clinical practice.
The observed cross-sectional association between lithium use and higher rates of suicidal ideation raises a number of further points of clinical and theoretical importance. Although one could hypothesize from our findings that lithium might induce suicidal ideation among patients with bipolar disorder, a causal link cannot be tested or substantiated on the basis of our cross-sectional design. Moreover, such an explanation would be unlikely and would be inconsistent with previous evidence (
10). On the basis of current crosssectional observations, other, more plausible hypotheses warrant future prospective examination.
First, lithium use could lead to a dissociation between suicidal ideation and suicidal behaviors. That is, lithium could diminish the likelihood of acts related to suicidality—for example, via modulatory effects on impulsivity or aggression—even if it fails to diminish suicidal thoughts. This hypothesis is consistent with findings that suicide attempts and completions are more closely associated with impulsivity than premeditation (
30) and that lithium reduces impulsivity and aggression (
31). No previous studies have addressed the potential impact of lithium or other psychotropic agents on suicidal thoughts as opposed to suicidal acts.
Second, it is possible that lithium could reduce suicidality through its effects on depression among patients with bipolar disorder (
2). In the study we report here, a majority of persons who had suicidal features were seeking treatment for a current depressed or mixed episode—that is, patients for whom current medications had, by definition, not provided optimal thymoleptic benefits. The potential antisuicidal properties of lithium relative to other compounds with demonstrated antidepressant effects—such as standard antidepressants or lamotrigine—deserves investigation (
10).
A third consideration involves uncertainty about when clinicians may have chosen to prescribe lithium, or other medications, relative to longitudinal changes in psychopathology. Although data on the duration of lithium treatment and adherence to adequate dosing were not available, such factors play a critical role in assessments of the efficacy of lithium (
32) and attempts to discern changes in suicide risk over time. Such considerations become highlighted by previous observations that most patients with bipolar disorder discontinue lithium within three months of starting it (
33) and that suicidal behaviors may increase above baseline rates in the year after discontinuation of lithium (
2). Recent findings also indicate that the use of a maximally supportive formal treatment program may be an essential ingredient to optimize the antisuicidal benefits of lithium (
34).
Our data raise the possibility that practitioners may reserve lithium use for more severely ill, high-risk patients. Because the prophylactic value of lithium appears better when lithium is introduced early rather than late in the lifetime course of illness, it is possible that its antisuicidal benefit also may attenuate if it is not introduced early in treatment. Longitudinal studies are needed to examine this hypothesis.
Suicidal behavior is a heterogeneous and multi-determinate phenomenon. Numerous factors mediate or moderate the relationship between thymoleptic drug therapies and suicide risk. Such factors may include elements specific to treatment itself (for example, medication adherence, duration of treatment, adequacy of therapy, and pharmacokinetic synergies) as well as illness-related characteristics (for example, comorbid illnesses). Subsequent longitudinal study of drug therapies, mediating variables, and suicidal thoughts or behaviors may help to shed greater light on the prevention of suicide among patients with bipolar disorder.