Characteristics
Most data came from quantitative studies published before 1991 (
1,
2,
3,
4,
5,
6,
7,
8,
9 ) that, except for two studies (
1,
7 ), did not provide control groups. In these studies, most of the difficult patients were between 26 and 32 years of age, whereas control patients were either of the same age (
1 ) or somewhat older (
7 ). More than control patients, difficult patients were unemployed and poorly educated. In most studies, difficult patients were predominantly men (between 60 and 68 percent). Diagnoses of psychotic and personality disorders were the most common. Prevalence of the former varied (19 to 44 percent), and prevalence of the latter was consistently high (32 to 46 percent) across all studies. Mood disorders (8 to 24 percent) and other disorders (4 to 16 percent) were less frequently found. Data on comorbidity of
DSM axis I and II disorders were absent across all studies.
Together, the studies refer to four dimensions of difficult behaviors: withdrawn and hard to reach, demanding and claiming, attention seeking and manipulating, and aggressive and dangerous. The first category is found mostly among patients with psychotic disorders, the second and third mostly among those with personality disorders, and the fourth appears with both diagnostic groups. Estimates of relative or absolute frequency of difficult patients were available from only one study, in which 6 percent of all 445 inpatients in a psychiatric hospital were considered difficult by at least two members of an inpatient nursing team (
7 ).
Difficult patients appear in both inpatient (
2,
3,
4,
5,
6,
7,
8 ) and outpatient (
1,
9 ) settings, yet no data were found on the prevalence of difficult patients in these subgroups, except for the study previously mentioned. One study (
9 ) found a high correlation between difficult patients, the number of hospital admissions, and inpatient days, which indicated a higher prevalence of difficult patients among inpatients. All studies considered psychiatric treatment centers at general psychiatric hospitals and outpatient clinics.
Most difficult patients are offered a pragmatic, eclectic form of psychiatric treatment. Because of their easy accessibility, both financially and physically, general mental health centers tend to attract a greater number of difficult patients, especially when emergency care is delivered (
1 ). Neill (
1 ) also found significant differences regarding a treatment plan and a primary caregiver. All control patients had both, whereas the difficult patients had neither. Difficult patients' files were updated less thoroughly, and communication between professionals of different treatment programs about these patients was minimal (
1 ).
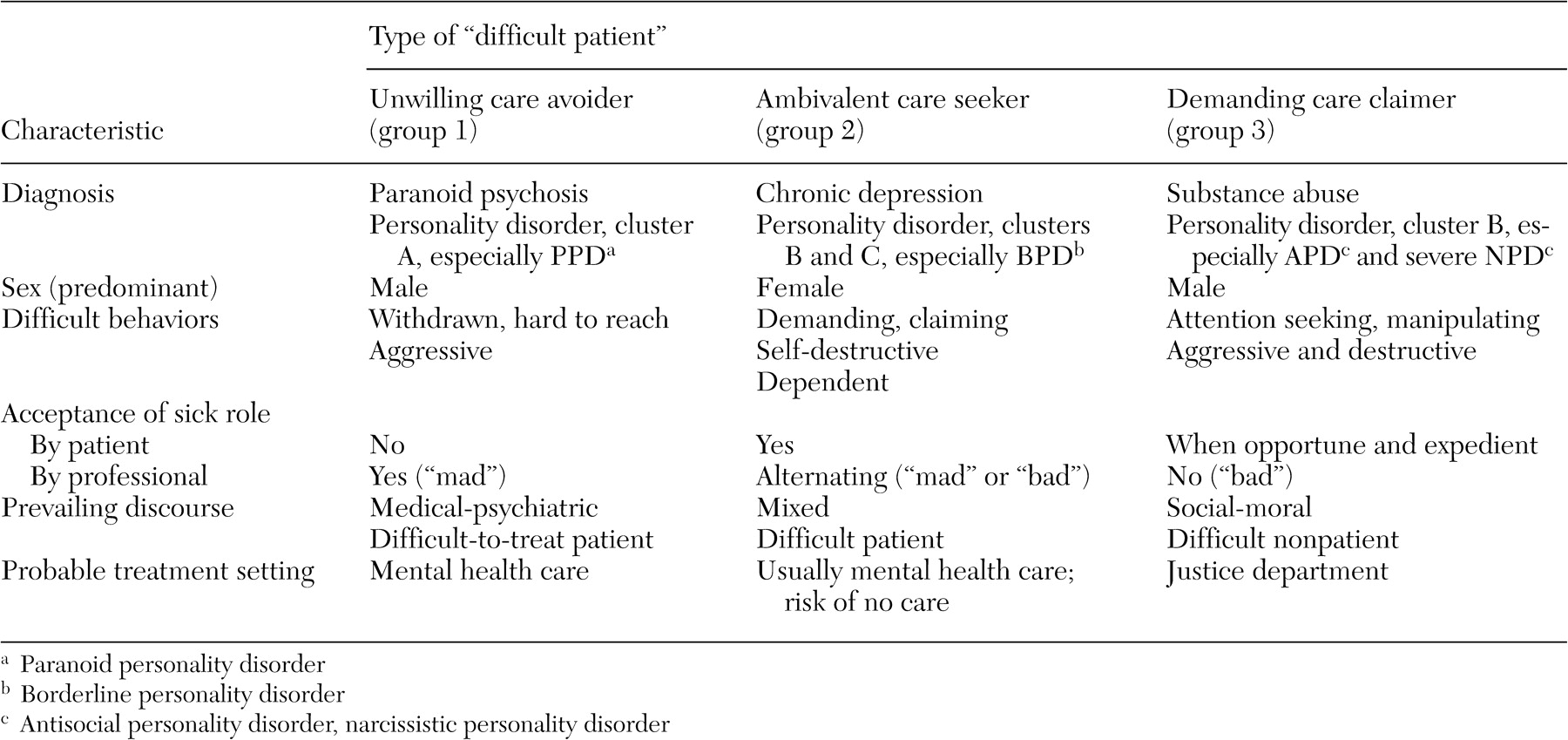
From the data reviewed, we hypothesize three subgroups of difficult patients, as presented in
Table 1 . In this scheme the first group of difficult patients, care avoiders, consists of severely psychotic patients who do not consider themselves ill and who view mental health care as interference. The second group, care seekers, consists of patients who have chronic mental illness yet have difficulty maintaining a steady relationship with caregivers. The third group, care claimers, consists of patients who do not need long-term care but need some short-term benefit that mental health care offers, such as housing, medication, or a declaration of incompetence.
Theoretical explanations
Individual factors . Four major theoretical explanations were frequently identified in the articles reviewed: chronicity, dependency, character pathology, and lack of reflective capabilities.
The first, chronicity, considers the course of the difficult patient's psychiatric disorder, which almost always is chronic and renders the patient dependent on mental health institutions (
10,
11,
12,
13 ). Chronic patients experience problems that are difficult to resolve by the psychiatric system, which leads to labeling these patients as problematic and difficult. Although chronicity of a mental disorder is a patient's personal matter, chronicity is also considered problematic for mental health professionals: "the sufferer who frustrates a keen therapist by failing to improve is always in danger of meeting primitive behavior disguised as treatment" (
14 ). Apart from being one explanation for patients' difficulty, chronicity induces specific responses by the psychiatric treatment system and is covered in more detail later.
Dependency on care is a second reason for perceived patient difficulty. Severe, unmet dependency needs lead the patient to project a lack of stable self and basic trust onto the caregiver (
1,
15,
16,
17,
18 ). The caregiver then experiences the patient as demanding and claiming, which makes the interpersonal contact difficult. Underlying the difficult behaviors of so-called hateful patients there seems to be a strong need for dependency (
16 ). These patients, who exhibit clinging, denying, entitled, or self-destructive behaviors, all have problems in tolerating a normal dependency (
18 ). In qualitative interviews with nurses, a clear difference was found between "good" and "difficult" dependent patients (
19 ). Good patients were described as reasonable and thankful; difficult patients were described as unreasonable, selfish, and not able to appreciate the value of given care. Power struggles arose easily with the latter category (
20 ). The relationship with the mental health professional becomes so important for many difficult patients that terminating it seems impossible, both for patient and professional (
21 ).
A third, psychodynamic view is that difficult patients have character pathology. Specifically, paranoid, borderline, narcissistic, and antisocial (
22,
23 ) personality disorders would make for difficult patients. Psychiatrists mentioned the diagnosis borderline personality disorder up to four times more often than any other diagnosis when asked about characteristics of difficult patients. Less frequent were paranoid, antisocial, sociopathic, obsessive, and narcissistic disorders (
24 ). According to several authors (
10,
18,
25 ), almost all difficult patients have a so-called borderline personality organization, which would explain why so many difficult patients have a highly ambivalent relationship with mental health care. People with this kind of personality organization perceive reality accurately yet feel overwhelmed by it, resulting in intense feelings of suffering and a need to seek help. In combination with so-called primitive defenses, such as splitting, idealizing, and projective identification, this lack of a clear self is considered a major source of the often confusing and negative interactions with professionals (
18,
26,
27,
28 ).
The fourth explanation for patients' being difficult is related to their perceived lack of reflective capacities. Reflection lies at the core of most psychotherapies; therefore, an incapability to reflect will easily turn the patient into a not-so-suitable (difficult) patient. People who are not securely attached in their younger days especially seem to lack these reflective or "mentalizing" capacities (
29 ). This insecure attachment may have many causes, one of which is trauma (
30 ), and easily creates problems in interpersonal relations, including those with caregivers (
28,
31 ).
Interpersonal factors. Some authors emphasized that it is not the patient but the therapeutic relationship that is difficult, thus taking the blame off the patient and situating problems in an interpersonal context. Traditional concepts of transference and countertransference are often used in this context, yet in a broader sense than in classic psychoanalytic theory. Countertransference in this context refers to the emotional struggles that emerge while working with difficult patients (
6 ). Transference is defined as the unconscious feelings the patient has toward the therapist, based on earlier experiences in the patient's life (with therapists in general or with this particular therapist). Countertransference is, likewise, defined as the unconscious feelings the therapist has toward the patient, either based on the patient's present behavior or on the therapist's earlier professional and personal experiences. Examples of professionals' countertransference feelings toward difficult patients are anger, guilt, helplessness, powerlessness, dislike, and disappointment (
3,
4,
14,
16,
32,
33,
34,
35,
36,
37 ).
Transference and countertransference issues between professionals and difficult patients are sometimes described in vivid detail (
14,
16,
32,
33 ). Although the concept of transference and countertransference is interpersonal, some authors maintained that the patient is responsible for evoking strong countertransference reactions (
38 ). Some critics have indicated that early psychoanalysts who were unable to maintain a transference relation used the transference concept to blame the patient for therapy failure (
39,
40 ). Others assumed that the difficult patient exists only because of a lack of professionalism among caregivers. In other words, if all caregivers were properly psychoanalyzed, these interpersonal problems would not occur (
41 ). Moreover, the transference relation is not a static one-way interaction but an intersubjective undertaking. In this view, two worlds need to meet, which is possible only if the therapist is able to put his or her own subjective views into perspective (
42 ). A strong working alliance can be reached only by mutual understanding and giving meaning to difficult behaviors displayed by the patient and to the nature of the therapeutic relationship (
43 ).
Countertransference in a multidisciplinary treatment setting has a different character, often strongly influenced by the so-called phenomenon of splitting. The difficult patient is considered a specialist in behaving differently with various team members, resulting in mutual disagreement (
14,
32 ). At the same time, the literature indicates that multidisciplinary teamwork with difficult patients is highly necessary, yet complex. Such teamwork leads to less trouble and fewer mistakes, because countertransference issues can be shared (
44 ). Feelings that emerge in countertransference may lead to distinctive reactions—extra care on the one hand, active neglect on the other—and different professionals may experience distinctive feelings of countertransference (
2,
4,
8,
34 ). For example, physicians are challenged when medication fails, when patients manipulate, or when treatment is difficult (
8 ). Nurses experience annoyance and anger when their caring attitude and competence are questioned (
8,
45 ). Both doctors and nurses get irritated when patients challenge their authority (
1,
46 ). Distinctions also have been noted between nurses' experiences on different types of psychiatric wards. Difficult behaviors were less easily interpreted as deliberate on wards with a psychodynamic orientation than on wards with a psychopharmacological orientation (
47 ). Perceived difficulty differed between on-floor staff and off-floor staff. The former group experienced patients' difficulty more intensely because on-floor staff has closer physical and emotional interaction with them (
48 ).
We found no studies that solely focused on the role of the professional. Yet some authors pointed out that some personality traits may increase the risk of difficult relationships with patients: a strong wish to cure, a great need to care, trouble with accepting defeat, and a confrontational and blaming attitude (
14,
33,
49,
50 ). Research on therapist variables that may account for good and bad treatment is still in its infancy (
50 ). Given the previously discussed concept of "blaming the patient," such variables appear to be closely linked to patients' being called difficult.
Systemic and sociological factors. We next review the social environment as the major explanation for difficult patients. In general, authors who supported this view assumed that different forms of social judgment are responsible for patients being called difficult, including prejudice, labeling, and exclusion.
Prejudice takes place largely within the individual, although it often is influenced by societal beliefs. Psychiatric literature, especially, covers the negative effects of certain diagnoses on professionals' attitudes. In this review, these negative attitudes were found among psychiatrists working with patients with personality disorders (
51 ) and among psychiatric nurses treating patients with borderline personality disorder (
52 ). In these studies, professionals were asked to rate the difficulty of certain behaviors, dependent on the patient's diagnosis. Patients who were diagnosed as having borderline personality disorder were judged more negatively than were patients with other diagnoses—schizophrenia, for example—although their difficult behaviors, such as expressing emotional pain or not complying with the ward routine, were equal. This difference seems to imply that certain difficult diagnoses evoke negative reactions from professionals, independent of the patient's actual behavior. However, only a few articles on this matter were identified with the search terms used.
Labeling differs from prejudice in that it implies a form of action rather than a mere attitude. In group-therapeutic practice this phenomenon is specifically documented (
53 ). It is not the diagnosis but deviancy from the particular group culture that leads to patients' being called difficult. This scapegoating may induce counter-therapeutic reactions by therapists (
54 ), which refer to actions and reactions that reinforce the characterization of an individual as the difficult patient in a group. Intersubjective theory, in which patients' and professionals' beliefs and actions are considered as equally subjective input into the therapy process, highlights the risk of negative labeling of particular patients. This theory contrasts with some psychoanalytic views in which individual behaviors tied to specific diagnostic terms, such as borderline and narcissistic disorders, are held responsible for patients' difficulty in groups (
55,
56 ).
The phenomenon of labeling is especially present in nursing literature. Behavior that deviates from what may be expected in a specific context, such as a hospital ward, risks being labeled as difficult, sometimes resulting in withdrawal of necessary care (
57 ). The difficult-patient label is easily and rapidly communicated among nurses and may lead to care of less quantity or quality (
58 ). Some authors claimed that difficult patients are socially constructed in a complex web of social influences, including power, status, the management of uncertainty, and negotiation (
59 ). Also the term stigma, first introduced by sociologist Erving Goffman as a superlative form of labeling, is used in this context (
60 ). Nurses tend to label patients as bad when they do not express gratitude for the help they receive (
61,
62 ), yet patients who do not improve but try hard are regarded positively (
46 ). Feelings of incompetency and powerlessness among professionals may lead to labeling patients as difficult, consequently leading to power struggles over control and autonomy (
45,
46,
63 ).
A step beyond labeling is the exclusion of patients from mental health care. Creating barriers to specific forms of treatment or care legitimizes the denial of care. Critics have gone go so far as to state that mental health providers deny the very existence of severe and disabling diseases, such as schizophrenia, by constantly being too optimistic about patients' opportunities to conduct their lives outside psychiatric hospitals (
64 ). As a result, responsibility for difficult patients is fended off, and patients may be passed on to another institution. Patients who do not fit into the system, because their problems differ from those of the mainstream, run a high risk of being labeled as difficult. This situation also occurs with patients who have alternative, nonmedical explanations or solutions for their health problems, such as maintaining a healthy lifestyle instead of using medication (
20 ). Chronic patients run a high risk of encountering this problem, because their complex and long-term needs often do not fit into the psychiatric care system (
11,
12,
13 ). According to this view, many difficult interactions are explained by the interpersonal stances of professionals and patients and by the mental health care system's tendency to consider atypical demands as difficult.
From an organizational perspective, the ongoing replacement of inpatient care by outpatient care is considered as possibly harmful for the difficult patient (
65 ). When the psychiatric hospital ceases to be a safe haven that offers long-term stay and therapy, the pressures on both patient and professional in outpatient care increase. This situation may have negative consequences for the working alliance and the patient's health situation, especially when busy community mental health centers can devote little time to difficult, long-term therapies (
65 ). Recent studies have stressed that the psychiatric hospital increasingly becomes a last resort for very specialized care or treatment of more disturbed difficult patients (
48,
66 ).
One study (
67 ) showed that patients whose treatment borders on different health care terrains—specialized medical care or addiction treatment—run a greater risk of being considered difficult. Iatrogenic damage may be the result of the diffusion of responsibility among different health care professionals. Comparable matching problems are likely to occur when a patient shows or threatens criminal behavior. Subsequent exclusion from the mental health system may have a detrimental effect on the patient. In general, professionals appear to be reluctant to set limits and tend to diffuse responsibility with patients who violate or do not know the "rules of the game" in the mental health system (
1 ).
Interventions
Many interventions suggested in the literature are rather standard and could therefore be characterized as common practice. Examples include respecting the patient, careful listening, validating feelings and behaviors, and being nonjudgmental (
68,
69 ). Yet difficult patients, as described in previous sections, seem to be very attentive to professionals' attitudes and behaviors. Therefore, these common practices are more important with this population than with patients who are not difficult. Apart from these standard interventions, some specific interventions are listed next, as well as interventions that consider the professional instead of the patient. Unfortunately, none of these interventions have been evaluated for effectiveness in empirical studies.
First, as stated earlier, a supportive and understanding attitude is suggested. A so-called holding environment, in which the patient may feel safe to experience different feelings and experiment with different behavior, is encouraged. To maintain the safety of this holding environment, setting limits for the patient is suggested. Other structuring interventions include assigning the patient the responsibility for his or her own safety, framing a clear treatment structure and contract, and maintaining one professional as a case manager for both patient and other professionals (
1,
23,
70 ). Interpretation of transference and countertransference issues as they arise is necessary and effective and may serve to ameliorate the doctor-patient relationship (
71 ). Others have recommended that modes of treatment or attitudes be modified according to different types of difficult patients, with different strategies for dealing with denying, dependent, and demanding patients (
17 ). Also mentioned are the need for a nonauthoritative attitude and power sharing (
45 ), forgiveness as a counterpart of a judgmental attitude (
72 ), and consciousness of the patient's situation and situational factors (
73 ).
Some more specific therapeutic techniques include slowly decreasing the amount of care (
74 ), modifying dialectical behavior therapy (
75,
76 ), creating a very strict and clear treatment contract in behavioral terms (
77 ), using strategic and paradoxical interventions (
78 ), and establishing a specialized aftercare program for former inpatients considered to be difficult (
79 ).
Additional interventions that professionals may use consist of two major categories: individual supervision and interdisciplinary team consultation. Through supervision, the attitude of the supervised professional may improve and treatment quality may increase. On the other hand, a parallel process may occur: the supervisor may consider the supervisee as a difficult person because none of the suggested interventions seem to work (
18,
43,
80 ). Other options on a personal level include collaborating and consulting instead of working alone and maintaining balance in both private and personal life (
49 ). Multidisciplinary meetings are suggested as a way to form a collective vision. In such meetings, staff feelings are channeled into more professional modes, and development of consistent treatment plans is endorsed (
48,
81 ). Sessions that value the views of different professions and lack the need of forming immediate solutions offer the best insight in team troubles and processes (
6 ). Outside consultation by a third-party professional is a useful variant that may help immersed treatment teams to gain a fresh perspective (
82,
83 ). Last, reading literature on patient care is suggested to help students and trainees to gain perspective on the difficult patient's vantage point (
84,
85 ).
In summary, the professional should maintain a validating attitude and strict boundaries within a clear treatment structure. Consciousness of the patient's background and one's own limitations helps the professional to see different perspectives, and consultation and supervision may strongly reinforce the importance of different perspectives.