Minority ethnicity or race plays an important role not only in attitudes toward seeking professional mental health services but also in the likelihood of obtaining access to mental health care. Social and cultural differences in both seeking and obtaining mental health services have been well documented
(1–
4). Recent studies
(3) have shown, for example, that African Americans report more positive attitudes toward seeking mental health services than do Caucasians. Nevertheless, Asian and Hispanic Americans are more likely to use outpatient mental health services than African Americans
(4). These differences point to the need for a detailed examination of the pathways followed by patients from the community into and through the mental health treatment system and back into the community. It has been known for a long time that, in addition to sociodemographic and clinical variables, variables related to these pathways, such as source of referral and type of treatment service used most recently, are important predictors of the use of mental health services
(5–
8).
Little is known, however, about whether patients who schedule appointments ahead of time (“scheduled patients”) differ significantly from patients who walk in and seek treatment without scheduling appointments (“walk-ins”). This issue is particularly important when the outpatient system is designed to serve low-income groups because of their greater vulnerability to many mental disorders, especially those requiring immediate attention
(9).
The objective of this research was to determine whether among low-income individuals from minority groups, scheduled patients differ from walk-ins in terms of sociodemographic, clinical, and pathway variables.
Method
The subjects (N=382) were all admitted to a university-affiliated outpatient psychiatric clinic serving a low-income, inner-city population. All were indigent, were enrolled in Medicaid, and had no other source of payment for their treatment. This clinic was the only place where they received outpatient psychiatric treatment during the 2-year study period. There were 164 men in the group (43%). Blacks formed 51% of the group, Hispanics 25%, and whites 24%. The percentages of men in each group were as follows: blacks, 42%; Hispanics, 38%; and whites, 51%. The mean age was 33.5 years (SD=13.4).
After a comprehensive initial evaluation, a psychiatrist made the psychiatric diagnosis according to DSM-III-R criteria. Patients with primary diagnoses of alcoholism or substance abuse were not admitted to this clinic; they were referred elsewhere.
The charts of all of the subjects were reviewed for sociodemographic characteristics (age, gender, race/ethnicity, and marital status), clinical variables (diagnosis and type of presenting complaint), and pathway variables (source of referral and most recent setting visited for mental health services). Two researchers (H.B. and J.M.D.) independently classified each presenting complaint into one of four types: mental state, physical functioning, social relationships, and social performance. The first two areas of disturbance were considered medical complaints (i.e., symptoms); the last two were considered social complaints (i.e., problems of living). For example, hearing voices and seeing things were regarded as medical complaints in the area of mental state, inability to fall or stay asleep and loss of appetite were considered complaints in the area of physical functioning, conflicts with spouse and peers were considered complaints in the area of social relationships, and criminal charges and difficulty with job interviews were regarded as complaints in the area of social performance. Agreement between the two raters on the classification of each specific complaint into one of these areas was achieved in one or two attempts
(10).
Bivariate analyses (chi-square tests and t tests) were done to determine the statistical significance of the relationships between each study variable and the mode of entry into outpatient psychiatric treatment.
Results
Almost two-thirds of the patients (63%, N=241) were walk-ins. The mean ages for the two groups were identical: 33.7 years (SD=12.4) for the scheduled patients and 33.7 years (SD=14) for the walk-ins.
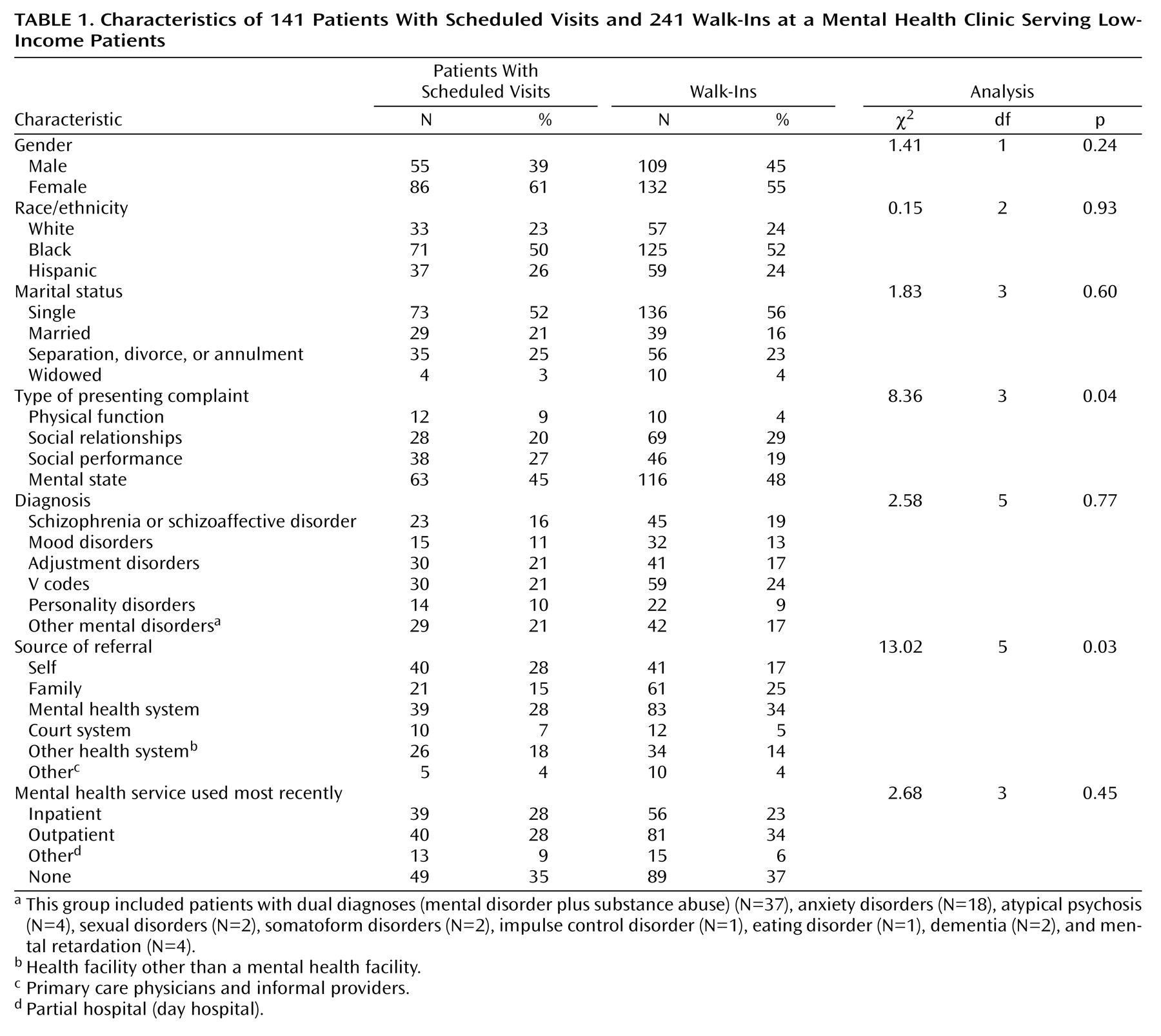
Table 1 shows the distribution of the subjects in the two groups for each variable studied in this research. Type of presenting complaint and source of referral were the only variables that were statistically significantly associated with the mode of entry (p<0.05). Complaints related to physical function and to mental state tended to occur with similar frequencies in the two groups. Walk-ins were more likely to express complaints related to social relationships, whereas scheduled patients were more likely to express disturbance in social performance. The mental health system was the most important referral source for the walk-ins, and it tied with self-referral among the scheduled patients. Family members were the second most frequent source of motivation among the walk-ins. The direction and the statistical significance of the associations did not change when the 37 subjects with comorbid mental health problems and substance abuse were excluded from the analysis.
Discussion
In this study, scheduled patients and walk-ins had more in common with each other than might be expected. Several variables were examined, but only two variables, type of presenting complaint and source of referral, were associated with the mode of entry with statistical significance. Perhaps walk-ins typically postpone asking for help until their families urge them to do so in view of a serious disruption in social relationships. Scheduled patients are probably more motivated to seek treatment to begin with and therefore more likely to initiate their appointments, particularly if they are obligated to do so because of pressures from the legal system. The clinic in which this study was conducted did not admit patients with a primary diagnosis of alcoholism or substance abuse. Because only 37 subjects received dual diagnoses of mental disorder and substance abuse, it was impossible to examine the pathways of this group of patients in detail. Research indicates, however, that source of referral is an important variable in predicting the engagement of dual-diagnosis patients in outpatient treatment
(11).
Three models of entry into psychiatric care have been proposed. In the first, called the “choice” model, while the impact of the social context is recognized, the individual is viewed as a rational decision maker choosing to do what he or she wants to do
(12–
14). In the “coercion” model, the individual is viewed as being pushed into care by friends, relatives, co-workers, or the legal system, thus implying active resistance to treatment
(15,
16). In the third, called the “network episode” model, the mode of entry is interpreted as a sociodynamic process, in which the individual neither actively chooses nor resists entry into treatment but passively follows the decisions made by agents from the individual’s social network as a way of “muddling through” the system
(17). In this study, how the subjects got into the mental health system was not examined, and therefore it is impossible to determine what percentage of this group actually “muddled through” the system. More research is needed to identify the sociodynamic processes that lead some patients to schedule appointments while others simply walk in for treatment.
The fact that a large majority of the patients were walk-ins suggests that the option of coming without scheduling an appointment should be made available in treatment settings similar to the one studied in this research. Cost-effectiveness studies should be done to determine whether the additional cost of staff time involved in the walk-in mode of entry is offset by the higher rates of admission to outpatient treatment. The findings of this study suggest that linkages with the community and outreach to families are critical for the success of this type of mental health program. Families need support and encouragement in their role as facilitators of mental health treatment. Considerable thought should be given to practical obstacles that prevent or discourage patients from coming to treatment, such as availability of transportation or services for child care. Mechanisms for overcoming these barriers should be an integral part of all comprehensive outpatient mental health programs designed to serve low-income and minority groups.