Primary familial brain calcification is characterized by the presence of symmetrical and bilateral brain calcifications, mainly on the basal ganglia but also on other brain structures, such as the thalamus, cerebellum, and cerebral white matter.
1 Over the years, a variety of names have been associated with this disease, and the commonly used eponym, “Fahr’s disease,” has slowly been substituted by other terms, following a tendency seen in medicine as a whole.
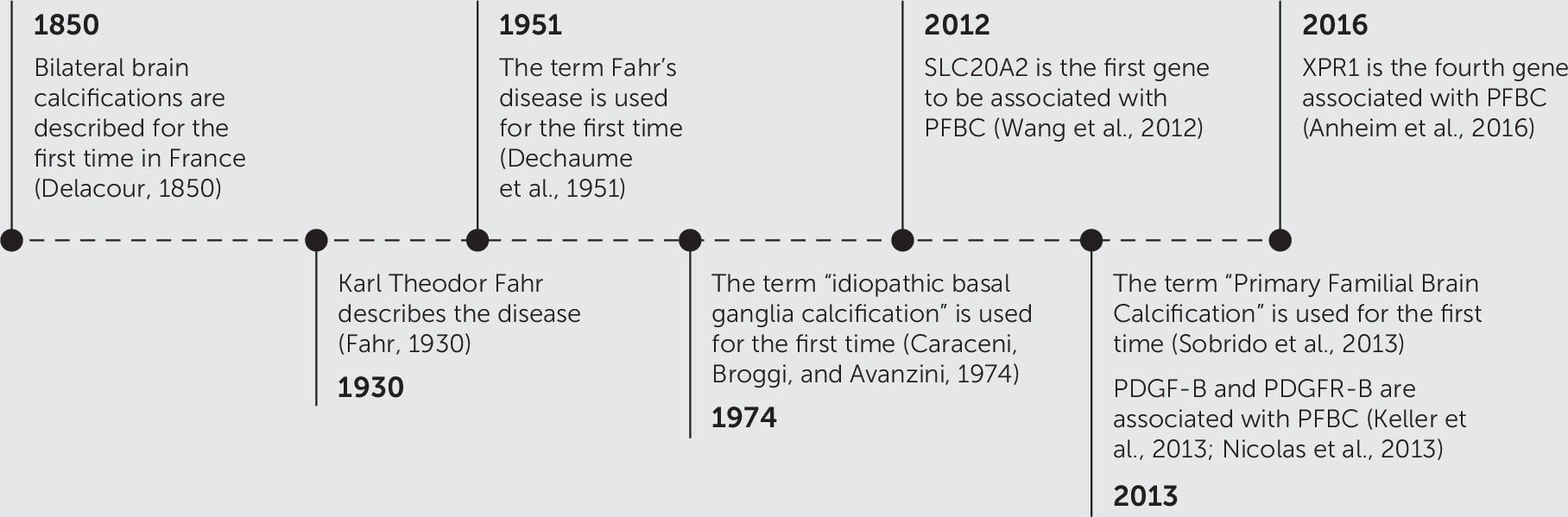
2,3Although Fahr’s disease was first described in 1850 in France, its name refers to Karl Theodor Fahr, the German physician who described the disorder 80 years later.
4,5 (
Figure 1) The eponym was used for the first time in 1951,
6 and variations of it are seen, ranging from possessive to nonpossessive forms, as well as from syndrome to disease. This results in four different variations of the original eponym: Fahr’s disease, Fahr disease, Fahr’s syndrome, and Fahr syndrome. Furthermore, since 1952 a large selection of terms has been used in the literature when referring to this disorder, and more recently there has been a tendency to move toward biologically based names.
3,7The diminished use of eponyms is not exclusive to Fahr’s disease. Although common in the past, it has fallen in popularity among researchers and physicians around the world for several reasons. The main reason is that in recent years the scientific community has mostly agreed that disease names should focus primarily on conveying the underlying cause of the disease, not on the physician who first described it.
3 Some disadvantageous aspects related to the use of eponyms include the possibility of several names being attributed to a single disorder, which can generate confusion, as well as the use of a single eponym to describe different disorders.
2 In addition, some eponyms are being avoided due to the connection between the physicians honored and unethical practices.
8 On the other hand, it can be argued that the use of eponyms makes referring to a disease easier—especially for patients—saves physicians time, and prevents misunderstanding.
9,10 Some well-known examples of commonly used eponyms include Alzheimer’s, Parkinson’s, and Huntington’s disease, and there is no indication that these terms will be discontinued any time soon. Regardless, the use of the correct term when referring to a disease is important not only to ensure that no confusion is generated between health care providers and researchers but also in order to represent the disease in its entirety.
11With regard to Fahr’s disease, the names used from 1951 until now include, but are not limited to, the four Fahr eponyms, idiopathic basal ganglia calcification,
12 and primary familial brain calcification,
13 resulting in a total of more than 35 different names.
14 The terms mentioned above are the most commonly used, and there appears to be no exact criteria to distinguish them or to define when one is used over the others. Use of the correct nomenclature is especially important for this disease, because the term used has the capacity to identify whether the patient’s calcifications developed primarily, when they can be attributed to genetics, or whether they developed secondarily in response to traumatic, metabolic, or infectious stimuli.
1Taking this into consideration, here we aimed to compare the use of different terms used when referring to primary familial brain calcification throughout the years and, possibly, to identify a tendency from the research community to abolish or adopt a specific term.
Methods
In January 2018, we searched PubMed for Fahr eponyms (Fahr’s disease and syndrome, possessive and nonpossessive forms), as well as for the terms “primary familial brain calcification” and “idiopathic basal ganglia calcification.” To ensure that the data analyzed reflect the scientific production of an entire year, studies dated to 2018 were not included in the analysis. Papers in all languages available on the platform were included, while abstracts of work presented at conferences, symposiums, and similar events were not included. Graphs were plotted by using Microsoft Excel.
Results
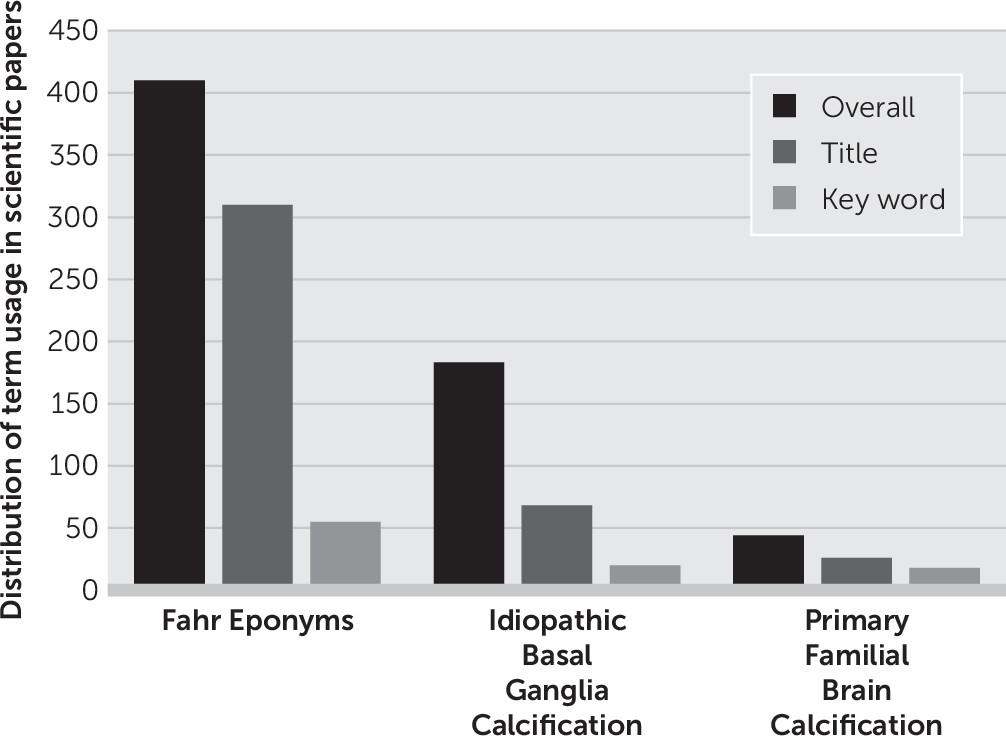
Overall, our results showed that Fahr eponyms and the term idiopathic basal ganglia calcification have been used more than the term primary familial brain calcification (
Figure 2). This was expected, because the term primary familial brain calcification was introduced in 2013,
13 while Fahr eponyms were first used in 1951
6 and idiopathic basal ganglia calcification in 1974,
12 as shown in the timeline displayed in
Figure 1.
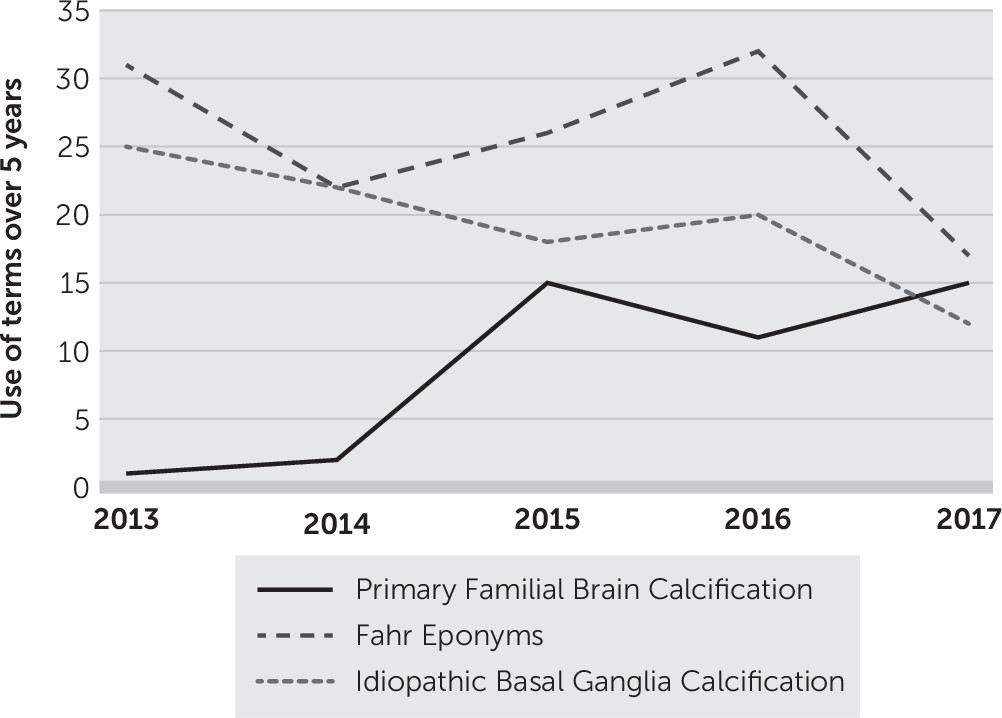
Since the introduction of the term primary familial brain calcification in 2013, use of the term in scientific papers has increased, indicating the acceptance of the term by researchers and physicians. This is simultaneous to decline in the use of Fahr eponyms. However, to date, these eponyms are used more than any of the alternative terms (
Figure 3). Moreover, until 2017, the term idiopathic basal ganglia calcification was used more than the term primary familial brain calcification and has been used in studies in which mutations are identified, although this contradicts use of the term “idiopathic.” Nevertheless, a decline in the use of the term idiopathic basal ganglia calcification can be observed, which is a positive sign and indicates that more thought is being put into choosing the correct terminology (
Figure 3).
Conclusions
It is our position that there is no foreseeable end to the discussion regarding which term—primary familial brain calcification or idiopathic basal ganglia calcification—is the most appropriate. Considering that there is currently no exact definition for either term, it is easy to understand why they are used interchangeably. Until a neurology or psychiatry institution formally approves one or more terms, the speculation will continue, and each specialty group will use the term they judge best. We preferentially use the term primary familial brain calcification, because we believe it to be the most appropriate to designate brain calcifications of genetic origin that occur in the absence of any metabolic, infectious, or traumatic stress. Regardless, it is important to conduct a critical analysis, especially regarding the use of terms such as “idiopathic,” “primary,” and “familial,” to ensure that the disease is not misconstrued on the basis of the name alone.
Additionally, we would like to propose a variation of the term primary familial brain calcification, since it currently excludes cases of de novo mutations. We believe that a term such as “primary bilateral brain calcification” can be used for both inherited and sporadic cases, which in turn facilitates differentiation between primary and secondary cases as a whole. Moreover, the term highlights the disease’s main finding (calcification in both cerebral hemispheres) and does not erroneously indicate that the lesions are restricted to a specific group of structures, as does idiopathic basal ganglia calcification. The proposed term can encompass the variations—“familial primary bilateral brain calcification,” “sporadic primary bilateral brain calcification,” and “idiopathic primary bilateral brain calcification ”—when it is necessary to further define whether a genetic mutation has been found. Although the first two terms would refer to familial and de novo cases, respectively, the latter should only be used in cases in which all appropriate genetic screening has been performed and no pathologic variants are detected.
Thus, we believe that primary bilateral brain calcification and its subcategories are good alternatives to the current denominations of primary familial brain calcification. Taken together, these terms represent the disease as a whole while clearly differentiating patients with known mutations from those whose genetic base for the disease is unidentified. Only in time will it be possible to determine whether the scientific community elects these terms as the most suitable, whether older terms such as primary familial brain calcification remain in use, or whether new options are proposed. Either way, it is important to focus on choosing clear and straightforward terms that will facilitate communication and improve understanding in the field.