This article reviews the literature on criminal recidivism among adults with schizophrenia or other psychotic disorders as well as the current literature in the field of criminology. On the basis of this review and synthesis, a conceptual framework for understanding and preventing criminal recidivism is proposed and necessary elements of intervention are identified and discussed.
Scope of the problem
Psychotic symptoms are reported by 15% and 24% of all prison and jail inmates, respectively, according to the latest U.S. Department of Justice survey (
5 ). Although these findings are based on self-report, findings about the prevalence of schizophrenia and other psychotic disorders from more rigorous studies are also concerning. Using data from the Epidemiologic Catchment Area program, Robins and Regier (
6 ) found that 6.7% of prisoners had experienced symptoms of schizophrenia at some point in their lives. A Correctional Service of Canada study using the Diagnostic Interview Schedule and the American Psychiatric Association's (APA's)
DSM-III-R criteria found a 7.7% prevalence of psychotic disorders in a sample of 9,801 inmates (
7 ). Also, a large study comparing the weighted prevalence of psychotic disorders between the national household survey and prisons in Great Britain found a tenfold higher prevalence of psychotic disorders among prisoners (
8 ). These findings are consistent with reports that individuals with psychotic disorders are arrested more frequently and have higher rates of criminal conviction for both nonviolent and violent offenses, compared with the public (
9,
10 ).
Most persons with schizophrenia are arrested for minor crimes, such as disturbing the peace and public intoxication (
11 ), but some commit violent acts, including assault and murder (
12,
13,
14 ). Although these events are rare, their serious and tragic nature highlights the need for effective treatment strategies (
15 ). Patients with schizophrenia and other psychotic disorders are unlikely to receive adequate treatment within correctional facilities. According to the U.S. Department of Justice only about half of all inmates with mental illness receive treatment, with most receiving no treatment other than medications while in custody (
16 ).
Current treatment strategies for adults with psychotic disorders
Treatment strategies for schizophrenia and related disorders have recently been evaluated in two major reviews, the Schizophrenia Patient Outcomes Research Team (PORT) (
17 ) project and the APA's Practice Guideline for Treatment of Patients With Schizophrenia (
18 ). However, these reports provide little guidance about management of patients with a history of repeated arrest and incarceration. Reviewing current treatments, the PORT recommends, "Assertive community treatment programs should be targeted to individuals at high risk for repeated hospitalizations or who have been difficult to retain in active treatment with more traditional types of services." Although the PORT cites evidence that this approach is effective at reducing hospital use, it has not been shown to reduce rates of arrest and incarceration (
19,
20 ).
The APA's Practice Guideline for Treatment of Patients With Schizophrenia reviews the literature on mandatory outpatient treatment, an intervention strategy present in 42 states (
15,
18 ). Mandatory outpatient treatment, also called outpatient commitment, involves the use of potential legal consequences in order to compel patients to accept outpatient treatment (
21 ). Although not discussed by either the PORT or the APA practice guideline, legal consequences are also used in jail diversion. Jail diversion encompasses a wide range of interventions that are positioned within the criminal justice system, including mental health courts, specialized police teams, and pretrial service agencies (
22,
23 ). Jail diversion differs from mandatory outpatient treatment in that patients who receive the latter have typically not committed a recent crime, whereas those involved in jail diversion have been arrested or incarcerated.
For purposes of this article, the use of potential legal consequences to promote adherence to outpatient treatment will be called "legal leverage," regardless of whether the requisite legal authority originates from a judge, a probation or police officer, or another criminal justice source. Published reviews indicate that the use of legal leverage is effective at improving outpatient treatment adherence (
24,
25,
26,
27 ), although findings regarding its effectiveness at reducing rates of arrest and incarceration have been mixed (
21,
28,
29,
30,
31,
32 ). Examining these inconsistencies, reviews of mandatory outpatient treatment by Swartz and Swanson (
33 ) and by Hiday (
21 ) and reviews of jail diversion by Steadman and colleagues (
34 ) strongly suggest that the effectiveness of legal leverage is dependent upon its use in conjunction with intensive treatment. However, a recent review of mental health courts found no standards or guidelines regarding clinical services (
35 ). Similarly, a national survey of specialty probation programs found "staggering diversity" among agencies, including substantial variability in how they interfaced with treatment providers (
29 ). Also, a national survey of jail diversion programs indicated that few had specific procedures to follow up with diverted detainees or to ensure that initial linkages to treatment were maintained (
24 ). Although the APA practice guideline recommends combining mandatory outpatient treatment with "intensive individualized outpatient services," the question of how to define and deliver such services is not addressed.
In sum, our current approach to preventing criminal recidivism involves the widespread use of legal authority to promote treatment adherence in the absence of guidelines about treatment. What constitutes effective treatment for reducing arrest and incarceration among adults with psychotic disorders? Surprisingly, discussions of crime prevention within the mental health literature have largely ignored the considerable body of research on the subject within the field of criminology. A search for English-language articles in the Medline database from 1966 to 2006 with the combined keywords "schizophrenia," "crime," and "prevention" yielded only 23 articles. Less than half cited criminology journals, and none discussed how contemporary crime prevention principles could be applied to preventing criminal recidivism in schizophrenia.
Understanding criminal recidivism
In order to develop effective prevention strategies, it is necessary to understand why adults with psychotic disorders enter the criminal justice system. Although the mental health literature typically cites deinstitutionalization and our fragmented health care system as primary causes (
36,
37,
38 ), this rationale is not sufficient to explain why some patients enter the criminal justice system whereas others do not. A predominant approach to understanding and preventing arrest and incarceration in the general population includes the principles of risk, needs, and responsivity (
39,
40,
41 ). This framework states that individuals with criminal recidivism have many needs, but only certain needs are associated with criminal behavior and therefore should be the target of prevention strategies. On the basis of an extensive body of research, eight primary risk factors have been established that are strongly predictive of future criminal behavior (
41 ). These risk factors have been incorporated into standardized assessment tools that have demonstrated high levels of reliability and validity in predicting criminal recidivism (
42 ).
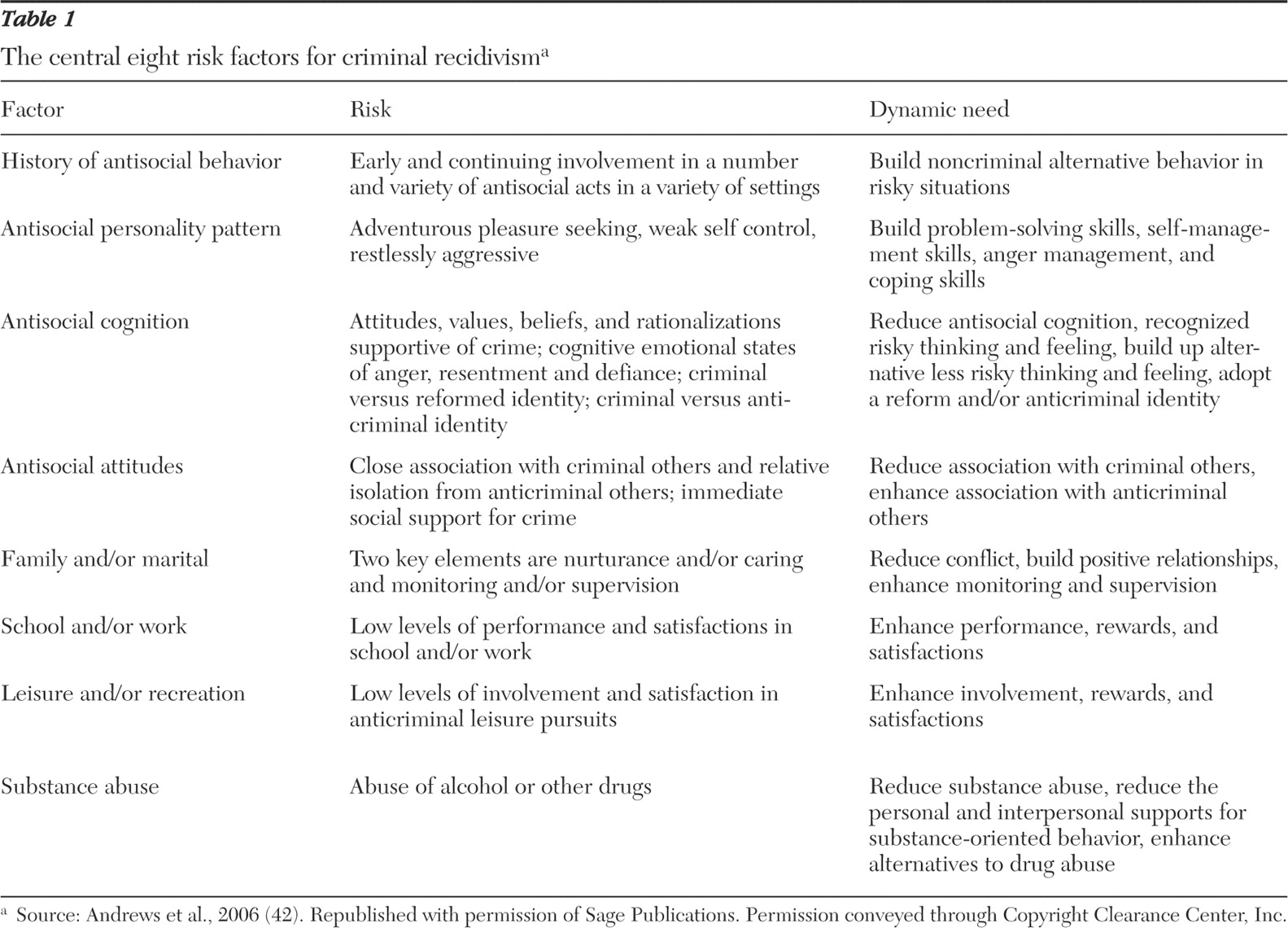
Table 1 shows the eight primary risk factors with their associated risks and needs.
Most studies of criminal recidivism have found little or no relationship between mental illness and the risk of criminal behavior (
43 ). As noted by Andrews and colleagues (
42 ) in their recent literature review, "the predictive validity of mental disorders most likely reflects antisocial cognition, antisocial personality pattern, and substance abuse." Adults with schizophrenia and other psychotic disorders have an increased prevalence of these established risk factors. According to the Epidemiologic Catchment Area study, nearly half of persons with psychotic disorders have co-occurring substance use disorders (
44 ). Also, the prevalence of antisocial personality disorder is significantly higher among adults with schizophrenia than in the general population (
45 ). In addition, many such individuals live in poverty and experience an associated lack of education, problems with employment, and absence of prosocial attachments (
46 ). Adults with psychotic disorders also have high rates of homelessness, a risk factor that has been associated with criminal behavior among individuals with and those without psychotic disorders (
47,
48,
49 ). The strength of homelessness as a recidivism risk factor relative to established risk factors has not been determined. However, research on the social-environmental context of violence suggests that access to appropriate housing is an essential need among adults with psychotic disorders (
50,
51 ).
Despite the high prevalence of established risk factors, the presence of psychosis itself may be an additional risk factor for criminal recidivism. As observed by Bonta and colleagues (
43 ) the episodic nature of psychotic symptoms may obscure their relationship with recidivism. Such a relationship could be affected by remission of acute psychosis as well as by diversion of some patients into the mental health system. Although lack of an association between psychosis and crime was reported by the landmark MacArthur Violence Risk Assessment Study, the study did not account for the role of social withdrawal and diminished social networks (
52 ).
Since publication of the MacArthur study, several studies have been published that address the methodological limitations of previous studies (
51,
53,
54,
55 ). These new studies provide compelling evidence that active psychosis is an additional risk factor for violence, independent of substance use disorders or antisocial personality features. Most notably, Swanson and colleagues (
51 ) examined the relationship between psychotic symptoms and violence by using data from 1,410 patients with schizophrenia in the rigorous Clinical Antipsychotic Trials of Intervention Effectiveness (CATIE) study by the National Institute of Mental Health. The CATIE study provides a unique opportunity to examine this association because it features a large sample of patients, a highly specific measure of violent behavior, and comprehensive clinical assessments. By using the Positive and Negative Syndrome Scale, Swanson and colleagues found that psychotic symptoms were strongly associated with increased risk of both minor and serious violence. However, violence risk was increased by positive symptoms only when negative symptoms were low, suggesting that certain levels of energy, initiative, and social contact are necessary to carry out violent acts.
Conceptual framework
The key to preventing criminal recidivism among adults with psychotic disorders is to engage them in interventions that target risk factors for recidivism. Engagement refers to the level of involvement in treatment interventions, and it encompasses both active participation in treatment as well as basic adherence to treatment (
56 ). Adherence can be defined as "the extent to which a person's behavior coincides with medical or health advice" (
57 ). Unfortunately, patients with psychotic disorders often refuse to accept treatment despite being advised to do so (
58 ). Most recently, the 74% medication discontinuation rate observed in the CATIE study provides strong evidence of the need to develop strategies to improve adherence (
59 ).
Patients are nonadherent with necessary treatment and support services for many reasons. Although the principles of risk, needs, and responsivity do not directly address treatment nonadherence, they highlight the importance of matching individuals who are at risk of arrest and incarceration with appropriate intervention strategies (
41 ). According to the responsivity principle, an individual's likelihood of benefiting from a particular intervention is determined by internal and external responsivity factors. Internal responsivity factors are individual characteristics, including learning style, verbal intelligence, and interpersonal sensitivity. Beyond determining whether an individual is capable of responding to a given treatment approach, however, individual characteristics can affect whether an individual adheres to treatment. Studies of patients with schizophrenia have established several individual characteristics that are associated with nonadherence. These include psychotic symptoms, depression, substance abuse, attitudes toward medications, low social functioning, young age, male gender, recovery style, residential instability, and family influences (
58,
60,
61,
62,
63,
64 ).
External responsivity factors are characteristics of treatment interventions or programs, such as whether a program provides outreach. Medication side effects and lack of efficacy are also known to impact adherence in schizophrenia (
59,
65 ). In addition, clinicians' interpersonal skills are likely to strongly affect adherence. In a recent study of medication adherence among patients with schizophrenia, quality of the relationship with clinicians was found to be an important determinant of patients' attitudes toward treatment and adherence to medications (
66 ). Beyond clinician and program characteristics, patients may likewise fail to adhere to treatment because of geographical, financial, cultural, and language barriers.
On the basis of the risk, needs, and responsivity framework, the clinical features of adults with psychotic disorders, and the characteristics of existing service delivery systems, the following three principles are proposed regarding treatment adherence and nonadherence.
The first principle is that nonadherence is the result of a mismatch between individuals and systems of care. Rather than viewing nonadherence as a patient characteristic or label, it is conceptualized as the result of interactions between individual risk variables and service-system risk variables. Individual risk variables for nonadherence include those cited above, such as attitudes toward medications, in addition to established recidivism risk factors, such as substance abuse and lack of family caring and supervision. Service-system risk variables include an absence of necessary treatment and support services, inaccessibility of existing services because of the barriers noted above, and clinical variables, such as clinician skill level and medication side effects. Although nonadherence may still occur among low-risk patients receiving optimal services, it is more likely to occur in the presence of multiple individual and service-system risk variables.
The second principle is that nonadherence mediates the relationship between modifiable risk variables and criminal recidivism. Some established risk factors for criminal recidivism are not modifiable, such as criminal history. However, others can be modified by interventions that target the needs listed on
Table 1 . Because risk factors for crime can be modified by appropriate treatment interventions, treatment nonadherence represents a common denominator in criminal recidivism. Treatment nonadherence is commonly found among both patients with schizophrenia and those with chemical dependency. It is strongly associated with homelessness, is frequently reported among offenders with mental illness, and is associated with violence and increased rates of arrest and incarceration (
60,
67,
68 ). The predictive strength of nonadherence relative to established risk factors for criminal recidivism has yet to be determined. However, the fact that most central risk factors for crime are potentially treatable argues that treatment nonadherence is a critical target for crime prevention strategies.
The third principle is that adherence to standard psychiatric treatment will prevent criminal recidivism to the extent that recidivism is driven by psychiatric treatment issues. Although psychiatric treatment interventions for psychosis, co-occurring substance abuse, and homelessness can prevent criminal recidivism, these interventions are not sufficient for all patients because they do not directly address other recidivism risk factors (
69 ). For instance, although some evidence suggests that intensive outpatient mental health services can lower recidivism rates among patients with schizophrenia and psychopathy, optimal prevention probably requires interventions that specifically target problematic personality traits (
70 ). This principle may be especially true for individuals with antisocial behaviors that predate the onset of schizophrenia (
71,
72 ).
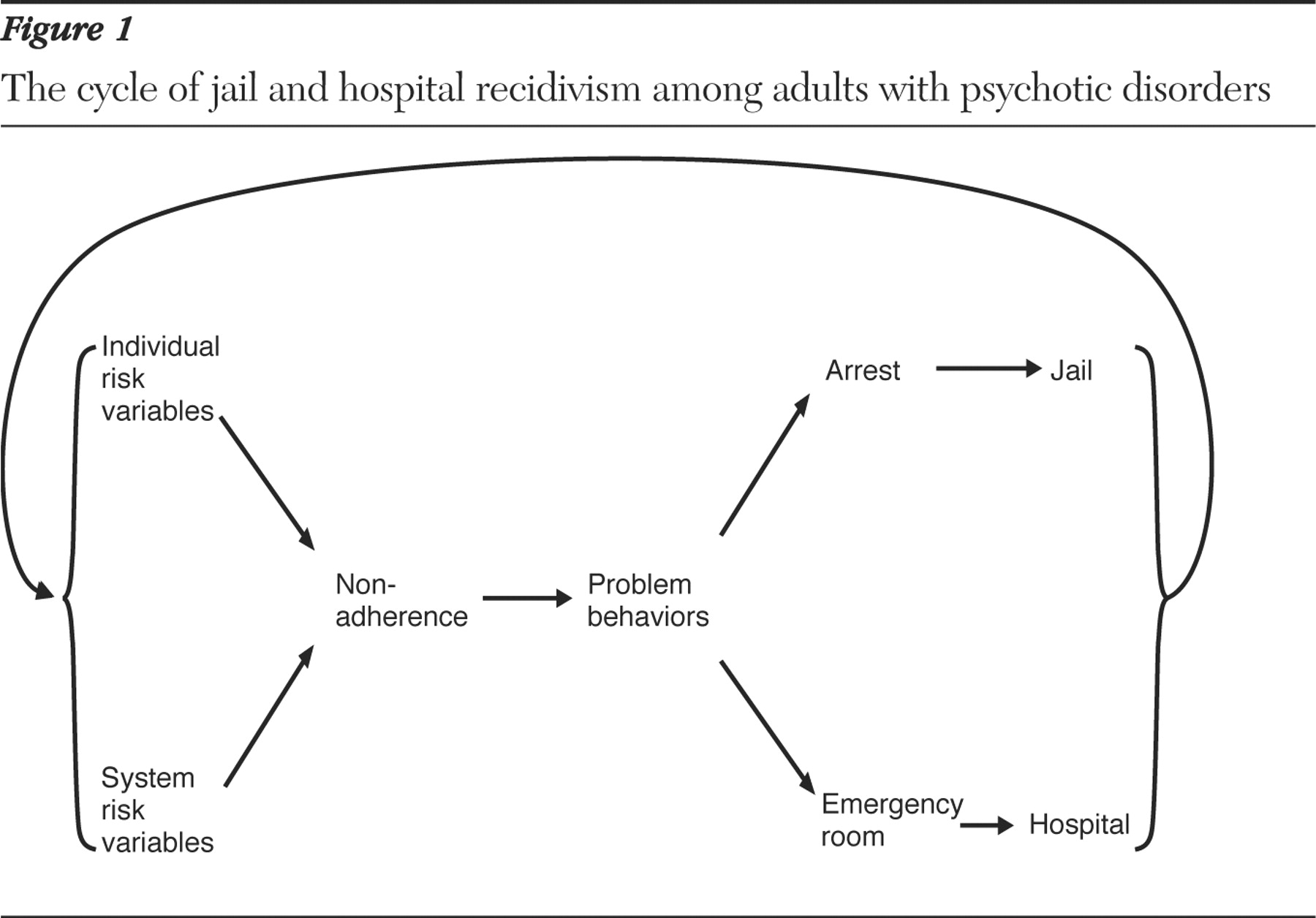
The relationship between risk variables, nonadherence, and recidivism are shown in a simplified schematic diagram (
Figure 1 ). The diagram is consistent with evidence that patients with a criminal history are at increased risk of both repeated incarceration and hospitalization (
73 ). As illustrated in
Figure 1, the likelihood of treatment nonadherence increases as the number of individual and service-system risk variables increases. Without appropriate treatment and support services, high-risk adults with psychotic disorders are more likely to exhibit problematic behaviors, such as loitering, trespassing, public intoxication, agitation, and verbal or physical assaultiveness. Such behaviors commonly go unreported. However, they can also result in emergency room intervention or arrest, depending upon who intervenes and how the intervention is conducted.
If a patient is taken to an emergency room, the decision of whether to hospitalize is largely based on whether the patient is determined to be dangerous to self or others. If hospitalized, patients are typically treated for five to seven days with sedating psychotropic medications and discharged with a follow-up appointment at the local community mental health center. In the absence of appropriate intervention after discharge, patients with multiple risk factors are likely to stop their medications, resume their use of illegal drugs and alcohol, and return to living on the streets. Such patients are at risk of continuing the cycle of problematic behaviors, arrest or emergency room intervention, and persisting nonadherence.
If a patient is arrested instead of taken to an emergency room, several issues will determine whether that individual will become incarcerated. Lack of appropriate treatment and support services can contribute to this outcome by decreasing the resources necessary for successful jail diversion. Other variables, such as the crime committed, laws of the local jurisdiction, and skill of the lawyers involved, can affect outcomes independently of individual risk variables or the presence of treatment services. In the absence of adequate follow-up services upon release from custody, patients are likewise at increased risk of continuing the cycle of nonadherence and recidivism.
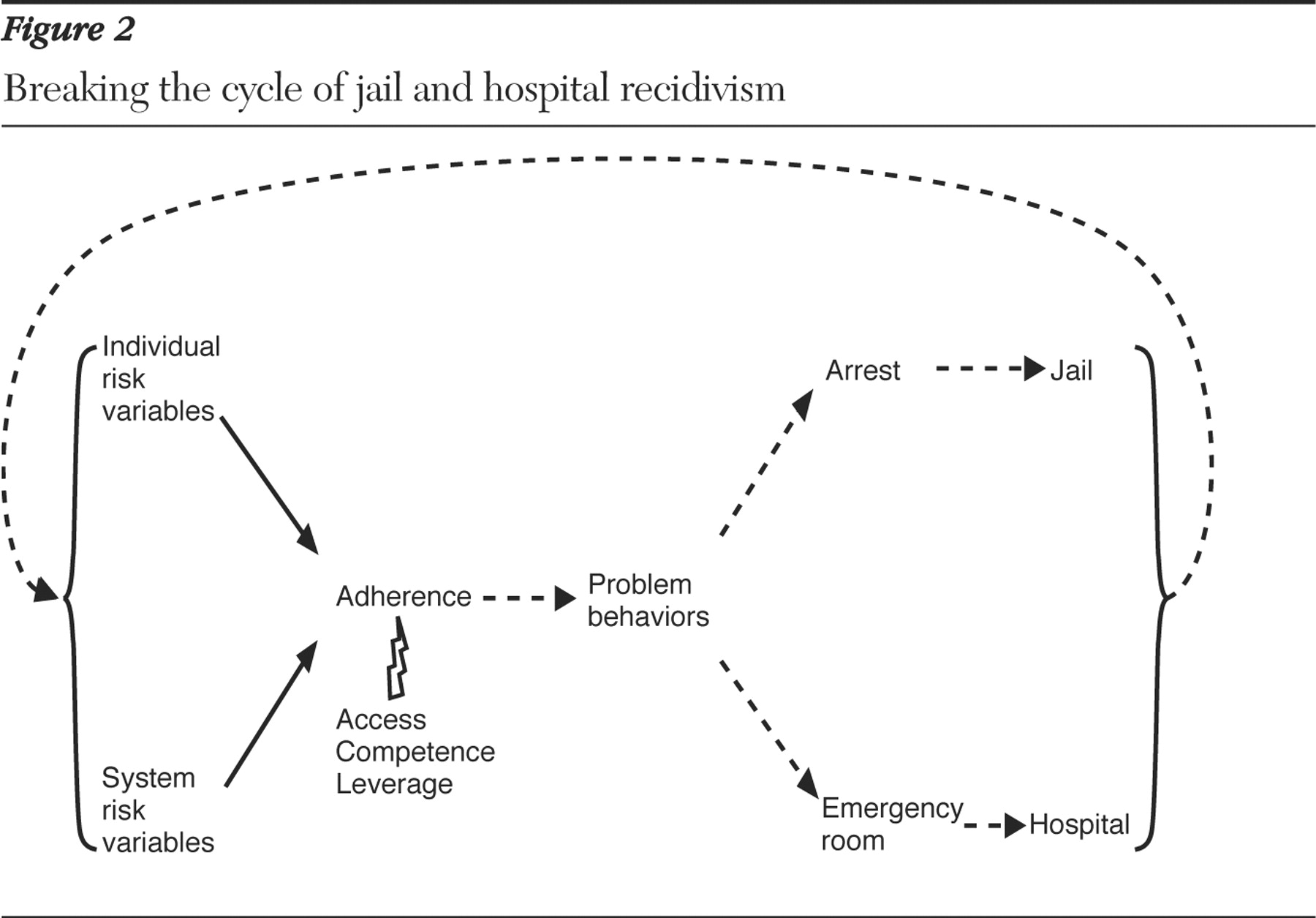
Promoting long-term improvement
Although legal leverage combined with accessible, competent treatment can interrupt the cycle of recidivism, lasting behavioral change is unlikely to occur unless patients become active participants in their own care. A potentially useful model for promoting treatment engagement among adults with psychotic disorders is the self-determination theory of behavior change. According to self-determination theory, treatment motivation may be either controlled or autonomous (
90,
91 ). Autonomous motivation for taking medication, for instance, means that patients freely choose to take medication because they believe it is personally important to their well-being (
92 ). Studies of conditions that are associated with treatment adherence problems, such as alcoholism (
93 ), opioid dependence (
94 ), nicotine dependence (
95 ), and obesity (
96 ), have confirmed that long-term behavioral change is associated with autonomous motivation. In studies of adults with psychotic disorders, legal leverage is associated with improved adherence (
24,
25,
26,
27,
9 7) but less so when it is associated with perceived coercion (
98,
99 ). For example, in Elbogen and colleagues' (
25 ) recent study of outpatient commitment and adherence, nonadherent participants perceived legal leverage as significantly more coercive compared with those who were adherent. According to self-determination theory, potentially coercive interventions, such as legal leverage, are more likely to promote autonomous motivation if conducted in a manner in which patients receive empathy, options, and a clear rationale about the decisions made (
92 ).
These qualities are similar to those that promote "procedural justice" within mental health court settings. Procedural justice, or perceived fairness of the court process by the patient, has been associated with low levels of perceived coercion despite the use of legal leverage (
100,
101 ). Similar findings have been reported with the process of involuntary hospitalization (
87 ). Thus legal leverage will be most effective at promoting active treatment engagement if applied not only in combination with accessible, competent care but also in a manner that supports patient autonomy to the extent allowable by each patient's circumstances.
Acknowledgments and disclosures
The author thanks the following colleagues for their suggestions and support during the development of this article: Steven Belenko, Ph.D., Eric D. Caine, M.D., Catherine Cerulli, J.D., Ph.D., Yeates Conwell, M.D., John F. Crilly, Ph.D., Paul Duberstein, Ph.D., Steven Erickson, J.D., Ph.D., Edward Latessa, Ph.D., Kim T. Mueser, Ph.D., Robert L. Weisman, D.O., and Geoffrey C. Williams, M.D., Ph.D. This article is dedicated in memory of Joseph W. Lamberti, M.D.
The author reports no competing interests.