Evidence indicates that people with severe mental illnesses from minority racial and ethnic groups experience service disparities compared with whites with severe mental illnesses (
1,
2 ). Blacks utilize fewer psychiatric outpatient and case management services and more acute psychiatric services than whites (
3,
4,
5 ). Although studied less extensively, Latinos also appear to utilize fewer nonacute psychiatric services than whites (
5 ). Little empirical research exists, however, regarding service disparities among adults with severe mental illnesses who are also homeless. Most studies of service utilization in diverse homeless populations have not focused on racial and ethnic disparities or have been conducted in nonnaturalistic conditions (
6,
7,
8 ). Furthermore, no study has reported on the experience of Latinos.
To determine whether there are service disparities for black and Latino homeless adults with severe mental illnesses compared with their white counterparts, we reanalyzed data generated by the federally funded Access to Community Care and Effective Services and Support (ACCESS) study. Although ACCESS was conducted over a decade ago, the insights learned from our disparities-focused analyses remain relevant because access to health and social services has not improved in any substantial way for this underserved population. At a minimum, the information thus generated may be regarded as a baseline profile of service disparities in this population.
Methods
We assessed service disparities by comparing utilization of three services among racial and ethnic groups that were similar with respect to variables associated with service utilization. We used propensity scores to adjust for need-related differences between the groups. Because ACCESS used state as a design variable, we estimated differences in service utilization within nine states and subsequently combined state-specific estimates.
Data sources and study population
In this study we used data generated by the ACCESS program, a quasi-experimental study conducted between 1994 and 1998. The background, methods, and findings of the ACCESS study have been presented in detail elsewhere (
11,
12,
13 ). Briefly, ACCESS recruited 7,055 adults with severe mental illnesses who lacked a fixed, regular, and adequate nighttime residence; people were recruited from the streets, shelters, soup kitchens, and health organizations. Active involvement in mental health treatment was an exclusion criterion. Participants were assessed at baseline and during the course of a year-long intensive case management intervention delivered at 18 sites located in nine states. Our study focused on baseline data for black, Latino, and non-Latino white ACCESS participants.
Outcome variables
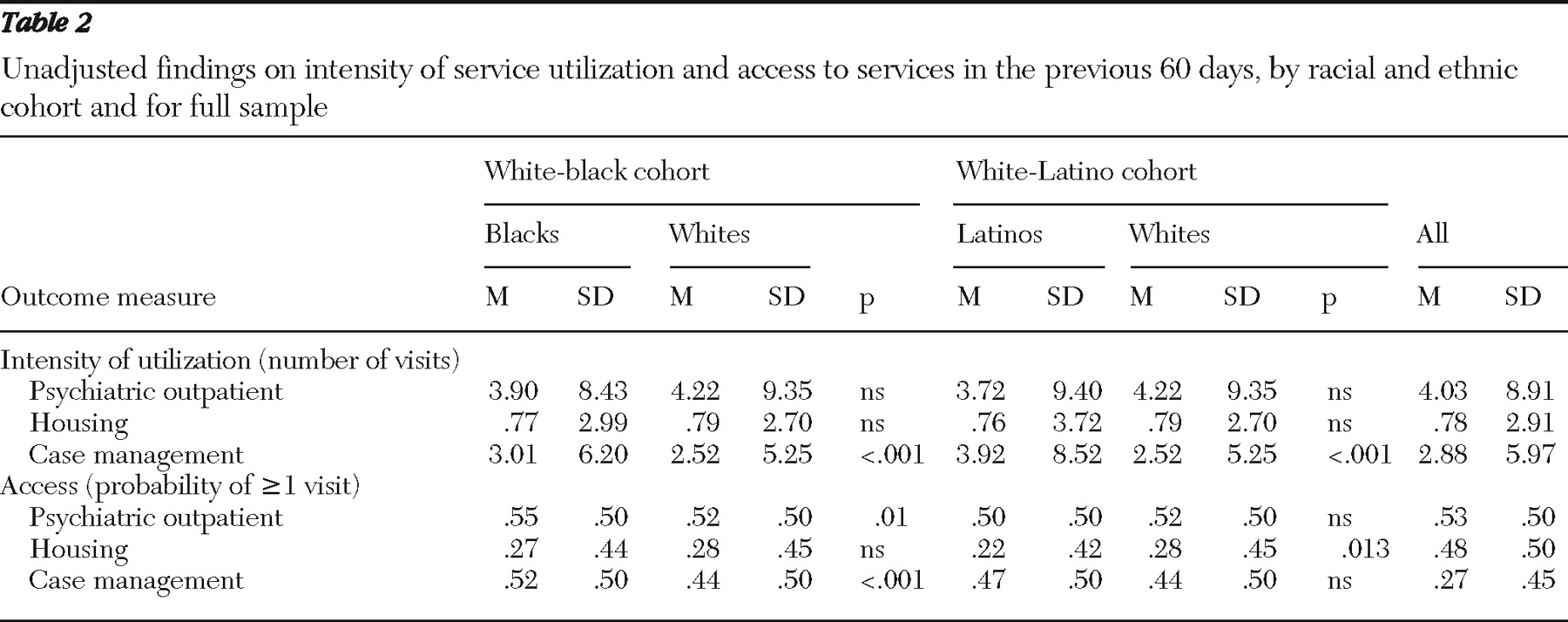
Outcome variables were measures of self-reported utilization of psychiatric outpatient, housing, and case management services derived from participants' responses to yes-no items used to characterize service utilization (for example, "Did you meet with someone who helped you find or keep housing?"). If the answer was yes, participants were asked how often in the past 60 days they had met with the respective provider. Utilization in the 60-day period preceding study enrollment was captured through measures of intensity of utilization (mean number of visits) and measures of access (the probability of any utilization, constituting at least one visit).
Although ACCESS also collected information on use of psychiatric inpatient, substance use disorder, medical-dental, and vocational services, we focused on the above-mentioned three services because of their critical importance for this population. It is self-evident that a population saddled with severe mental illness and homelessness has a fundamental need for psychiatric outpatient and housing services. Our decision to focus on case management services stems from evidence that these services can improve care coordination, a critical feature of health care for populations of this level of complexity (
14 ), and may narrow preexisting disparities (
15 ).
Explanatory variables
The main explanatory variable was self-reported race-ethnicity, which we used to construct one cohort comprising white and black participants and another comprising white and Latino participants.
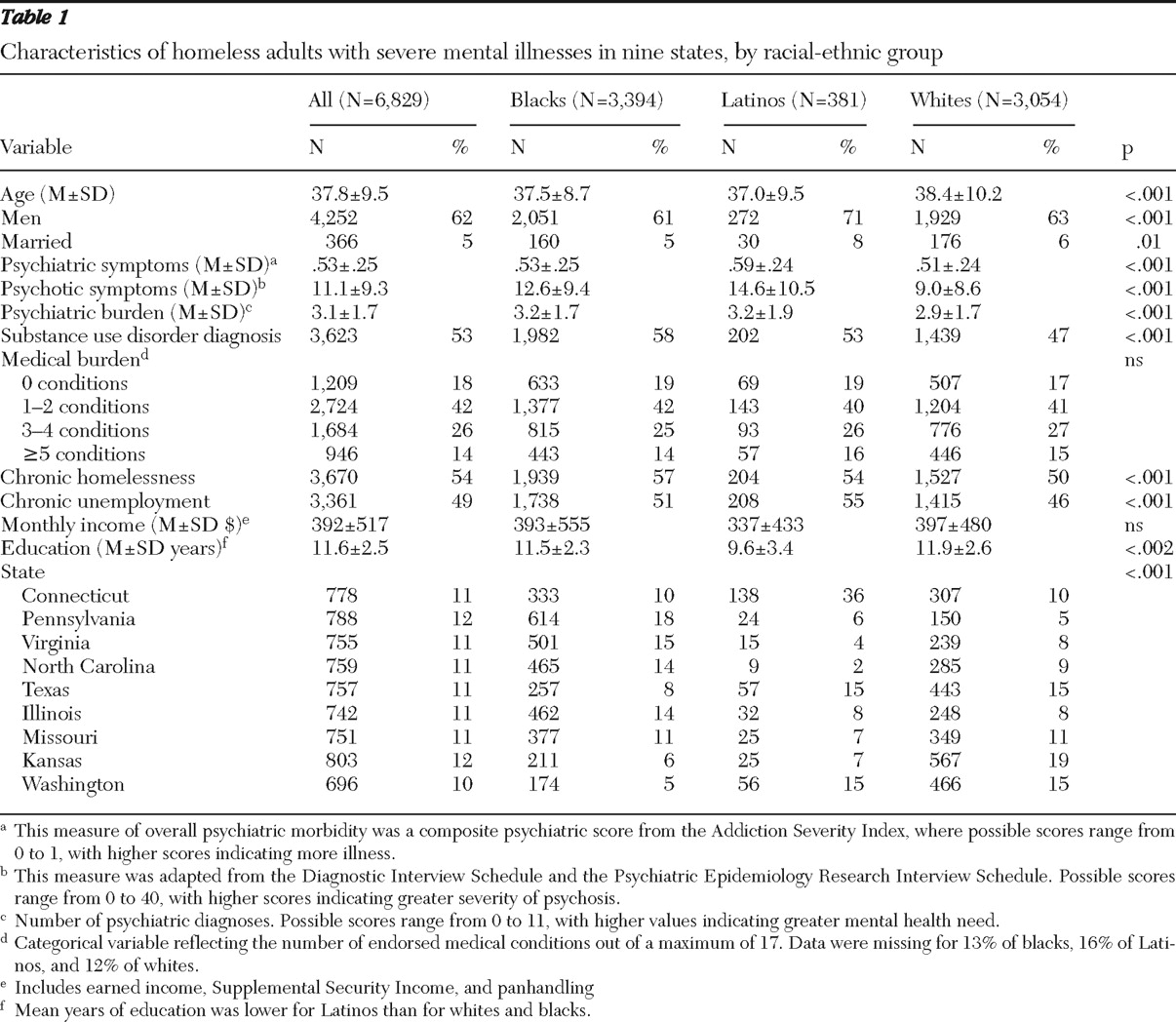
In addition, our multivariate model included several variables associated with need for health or social services: age (continuous), sex, marital status (dichotomous, yes or no), three measures of psychiatric need (psychiatric symptoms, psychotic symptoms, and psychiatric burden), substance use disorder diagnosis, medical burden, chronic unemployment, and chronic homelessness.
The measure of psychiatric symptoms was the composite psychiatric score from the Addiction Severity Index (ASI) (
16 ); values could range between 0 and 1. The measure of psychotic symptoms was a scale adapted from the Diagnostic Interview Schedule (
17 ) and the Psychiatric Epidemiology Research Interview Schedule (
18 ); values could range between 0 and 40. Psychiatric burden was a count of all clinician-formulated psychiatric diagnoses; values could range between 0 and 11. For these three variables, higher values indicate greater mental health need. Substance use disorder diagnosis was a dichotomous yes-no variable also based on clinician-formulated diagnoses.
Medical burden was a four-level categorical variable that grouped self-reported general medical conditions into zero, one to two, three to four, or five to 17 conditions.
Chronic homelessness was a dichotomous variable that indicated whether participants had one or more years of lifetime homelessness and had not lived in a residence of their own in the previous 60 days. Chronic unemployment was a dichotomous variable that indicated whether participants' typical employment pattern in the previous year was characterized by subemployment or unemployment (
19 ).
Additional variables of interest not included in our primary analyses were two indicators of socioeconomic status: income and education. Education was a continuous variable reflecting years of schooling. Income was a continuous variable that measured the total amount of money received on a monthly basis in the previous year from several sources, including earned income, Supplemental Security Income, and panhandling.
Statistical analyses
We compared the racial-ethnic groups with chi square tests (for categorical variables) and analysis of variance and the Bonferroni-Dunn test (for continuous variables).
Rates of missing data were negligible for race-ethnicity, service utilization, and most variables in our multivariate model. Exceptions were age and medical burden, for which rates of missing data varied by race-ethnicity. Medical burden had the highest rates of missing data, which ranged from 12% to 16% per group.
Data were analyzed with SAS, version 9.1 (
20 ). We imputed missing data with PROC MI with MCMC and subsequently created five multiply imputed data sets. We used complete-data methods to analyze each data set separately and combined parameter estimates across imputed data sets using standard rules (
21 ).
Adjusted analyses
Although race-ethnicity is not a modifiable variable, we used propensity scores to adjust for differences in need-related variables between the racial-ethnic groups because we wanted to ensure that the racial-ethnic groups were as comparable as possible (
22 ). We estimated models separately for comparisons between blacks and whites and then again for comparisons between Latinos and whites. We modeled the log-odds of being black (or Latino) as a function of the need-related variables included in our multivariate model. We then obtained an estimated logit of being black (or Latino) and compared probabilities between participants who were black or Latino and those who were white. Overlap in the distributions of estimated logits suggests that the racial-ethnic groups were comparable on the basis of observed confounding variables.
Using the empirical deciles of the estimated logits, we created ten strata for the white-black cohort. Similarly, using empirical tertiles of the estimated logits, we created three strata for the smaller white-Latino cohort. Next, we evaluated the comparability of the groups by assessing the extent to which they overlapped on each variable. Acceptable comparability was defined before the analysis as standardized differences between the groups of 10% or smaller (
23 ). Attempts were made to improve comparability by including quadratic terms and interactions in the model.
Estimating disparities
Because state was a key design aspect of the ACCESS study, we adjusted for state effects by stratifying differences by state and then combining them. Specifically, for each state and for each outcome variable and propensity score stratum, we calculated group-specific means and standard deviations for number of visits. Next, for each cohort we calculated stratum-level mean differences and standard errors in number of visits between the groups, which we subsequently combined across strata to generate state-level weighted mean±SE differences. In a final step, we combined state-level differences across states into an overall weighted mean±SE difference. [Further details are provided in the technical appendix, which is available as an online supplement to this article at
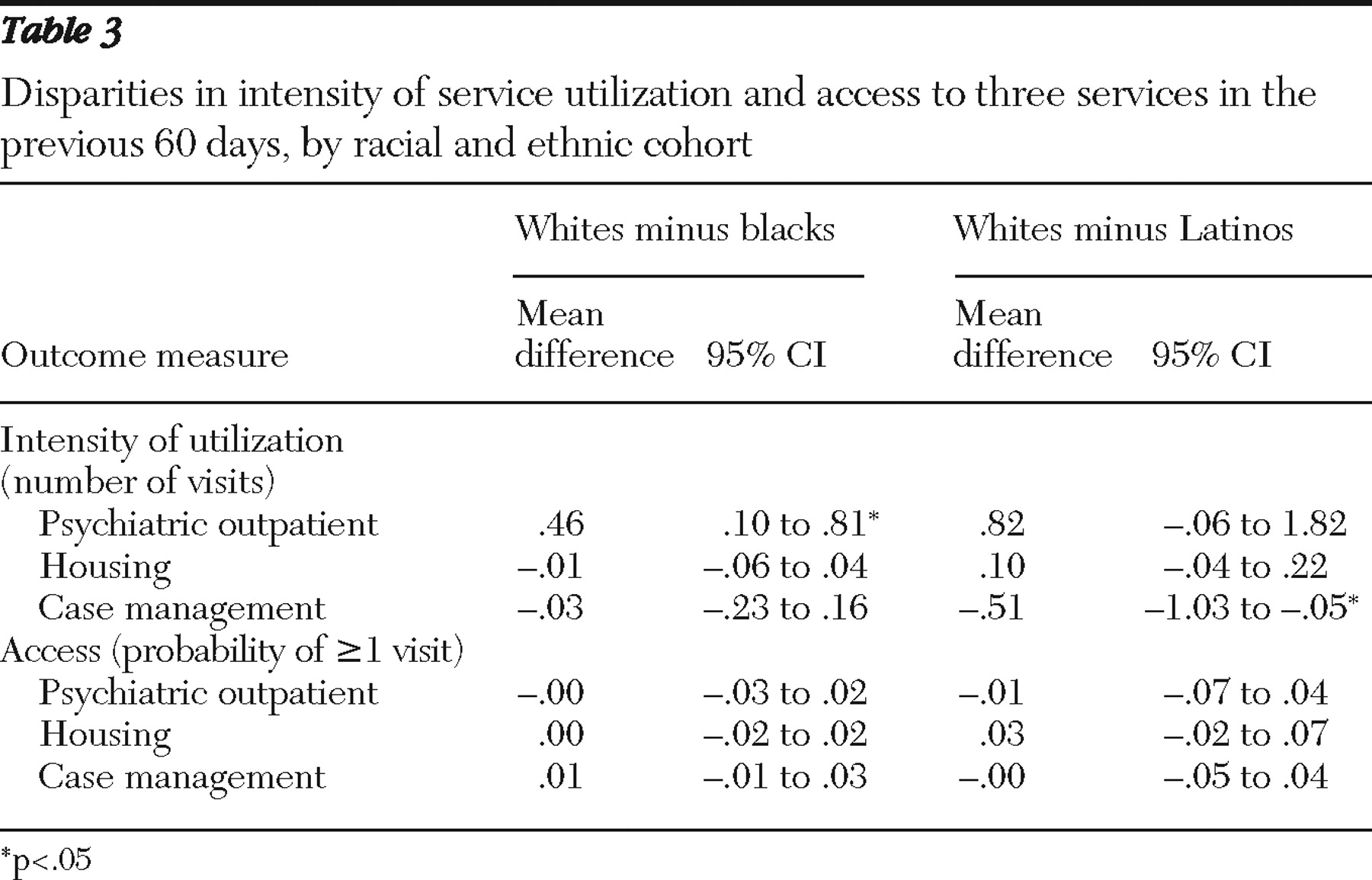
ps.psychiatryonline.org .] For each combining step, we used the inverse of the variance of the difference as the weight. We used a two-tailed z test to evaluate the significance of the differences; positive values indicated a racial-ethnic disparity, whereas negative values indicated higher intensity of utilization by blacks or Latinos. We repeated these steps using the mean probability of at least one visit as the outcome measure, thus comparing groups on their access to services.
We conducted additional analyses to evaluate the role of socioeconomic status in the observed disparities. Log-odds of being black or Latino versus white were modeled as a function of the expanded set of variables, and analyses proceeded as above.
We used a critical value of .05 to evaluate statistical significance of the p values, and we report our disparities results along with 95% confidence intervals (CIs); we did not control for multiple testing.
Because we used previously collected data that had no personal identifiers, our study was granted exempt status by the University of Pittsburgh Institutional Review Board.
Discussion
Our results indicate that black homeless adults with severe mental illnesses experienced a disparity in intensity of utilization of psychiatric outpatient services. The evidence was that black consumers had a lower mean number of psychiatric outpatient visits than white consumers on state-stratified disparities analyses of self-reported service utilization data collected at baseline by the ACCESS study. Although the difference of .5 visits is modest in absolute terms, it is substantial compared with the unadjusted mean of four visits for the previous 60 days. We did not find disparities in intensity of utilization by Latino consumers. To the contrary, our only significant finding for white-Latino comparisons was Latinos' higher utilization of case management services. Here too, although the difference of .5 visits appears modest in absolute terms, it was significant given that the unadjusted mean number of case management visits for the previous 60 days ranged between 2.5 and 3.9 for the three groups. We did not find access disparities for white-black or white-Latino comparisons.
Consistent with evidence generated by previous research (
8,
24 ), we found that our sample had low intensity of utilization of services of critical importance to their well-being. This finding may have been influenced by the ACCESS study exclusion of individuals receiving mental health care at study enrollment. However, the notoriously tenuous connections of homeless adults with severe mental illnesses to the health care system (
6,
7,
25 ) make it unlikely that our utilization figures represent a substantial underestimate. Low levels of insurance coverage, social marginalization, and distrust of the system are among the many barriers to care that this vulnerable population faces (
13 ).
Our finding of variable service utilization across states mirrors findings from other areas of health care (
26 ). Possible contributors include state differences in availability of resources for the homeless population and the characteristics of the social welfare apparatus, including ease of access to public insurance programs.
Ours is the first study of homeless adults with severe mental illnesses to have assessed disparities separately for blacks and Latinos. A previous study that compared services used by Latinos and whites was based on an incomplete ACCESS data set that focused on utilization during the course of the study and not before it (
27 ).
Our finding of a disparity in intensity of utilization of psychiatric outpatient services for blacks is not consistent with available evidence. A study of a homeless population of veterans with severe mental illnesses, a substance abuse problem, or both and who were receiving care from the Veterans Health Administration (VHA) found that blacks and whites had comparable service utilization (
28 ). Further, a cost-effectiveness study based on data from a randomized trial of assertive community treatment versus usual care for homeless people with severe mental illnesses found that blacks and whites in the usual care arm of the trial had comparable utilization of outpatient mental health services (
29,
30 ). However, neither study aimed to systematically evaluate racial-ethnic disparities in use of services. Further, whereas the VHA study may have obscured potential disparities by adjusting for socioeconomic status, the cost-effectiveness study did not adjust for potential differences in need between the groups.
Possible contributors to our disparity finding include individual characteristics, such as socioeconomic status (
31 ), and characteristics of the service system and the policy environment (
1,
2,
10,
32 ).
That our disparity finding dissipated when we controlled for education suggests that blacks' lower education level compared with whites played an important role in this disparity. We were unable to evaluate the role of insurance in this finding because our data set lacked insurance information. However, it is unlikely that insurance differences played a major role because we did not find access disparities. Although our state-stratified analyses controlled for state-specific policies that may contribute to disparities, we may not have fully accounted for geographic variations in access and quality of critical services for this population. For example, because we did not control for study site, if the racial-ethnic groups gravitated to different geographic areas served by providers of varying quality (
33,
34 ) or cultural and linguistic competency (
35 ), such differences may have influenced our results.
Racial-ethnic differences in service utilization may also result from stigma and negative attitudes toward treatment (
36 ). However, we were unable to assess the role played by these factors in our findings.
That we did not find white-black disparities in intensity of utilization of housing or case management services may point to a smaller effect of education on utilization of these services relative to psychiatric outpatient services or to a smaller quality gap across providers of nonmedical services relative to psychiatric providers.
Our finding that Latinos with severe mental illnesses who are homeless had higher intensity of case management utilization than whites is a new contribution to the research literature, which, even for the larger population of those with severe mental illnesses, is sparse in evidence with regard to this ethnic group. Two previous studies that assessed differences in case management utilization between mentally ill whites and Latinos differed from ours not only in that their samples contained largely nonhomeless people but also in that they adjusted for socioeconomic status. Whereas one study found that Latino adults with schizophrenia had lower access to these services (
5 ), the second study found comparable access for Latino and white children and adults with schizophrenia and other mental illnesses (
3 ).
Socioeconomic differences between whites and Latinos may have contributed to this unexpected finding, given that the difference disappeared when we controlled for education. Although we do not have an explanation for either finding, it is possible that Latinos' greater use of case management services may have been driven by a targeted use of such services to assist people whose educational deficits encumber their ability to navigate the welfare system. It is unlikely that insurance differences or the presence of Spanish-only speakers explain our finding because both dynamics would likely act in the opposite direction (
5,
37 ).
Little is known about whether the magnitude and direction of disparities found are sensitive to the type of outcome measure used—that is, access versus intensity of utilization. Two studies evaluated mental health disparities with measures of access and measures of quality constructed with data on intensity of utilization. Whereas one study found racial disparities regardless of the measure used (
31 ), the disparities found in the second study were measure sensitive (
38 ).
This study had several limitations. First, despite adjustment for propensity score, we were unable to achieve optimal comparability between whites and Latinos. This imbalance means, however, that our Latino group had greater severity of psychotic symptoms than whites, a fact that may underlie the higher intensity of case management utilization among Latinos (
5 ). Second, because people receiving mental health care at study enrollment were excluded, our findings may not be representative of the typical experience of homeless adults with severe mental illnesses. However, because of the tenuous treatment connections of this population (
6,
7,
25 ), psychiatric outpatient and case management utilization may not have been substantially higher in the absence of this exclusion criterion. Furthermore, despite this exclusion criterion, utilization of these two services was larger than zero for many participants, which indicates that a substantial fraction of people had been in treatment in the previous 60 days but had dropped out before enrolling in the study. Third, although concerns may be raised about our outcomes on self-reported utilization, adults with severe mental illnesses can provide reliable utilization data (
39 ). Last, we were not able to assess the effect of language preference because of the relatively small Latino group in our sample.