The serotonergic system, which is thought to mediate various physiological and psychological conditions related to certain disease states, including obsessive-compulsive disorders, anety disorders, eating disorders, depression, and schizophrenia, has been the subject of much research in both psychopharmacology and psychiatric genetics. The serotonin syndrome, a severe drug side effect caused by enhanced activity of the serotonergic system, is characterized by symptoms of restlessness, hyperthermia, diaphoresis, myoclonus, hyperreflexia, tremor, and lack of coordination. Insel et al.
(13) first described the serotonin syndrome in a patient with obsessive-compulsive disorder who used clomipramine after discontinuing treatment with clorgyline. Advances in molecular biology have revealed at least 15 subtypes of serotonin receptors in rodents and humans. The 5-HT
1A receptor is thought to mediate symptoms of serotonin syndrome based on psychopharmacological experiments using rodents
(14). The 5-HT
2A receptor has a relatively high affinity for various neuroleptics, including clozapine.
In view of the physiological role of the serotonergic system and similarities in the clinical manifestations of the serotonin syndrome and the neuroleptic malignant syndrome, the serotonergic system may be involved in the pathophysiology of neuroleptic malignant syndrome. Some investigators have speculated that a dopamine/serotonin imbalance is responsible for the occurrence of these drug-induced syndromes
(10,
15). We designed our experiments to screen well-defined amino acid substitutions in the 5-HT
1A and 5-HT
2A receptors in patients who had previously suffered from neuroleptic malignant syndrome because we hypothesized that some structural change in the receptor might confer sensitivity to psychotropic drugs and cause these drug side effects. The 659G/T polymorphism of the 5-HT
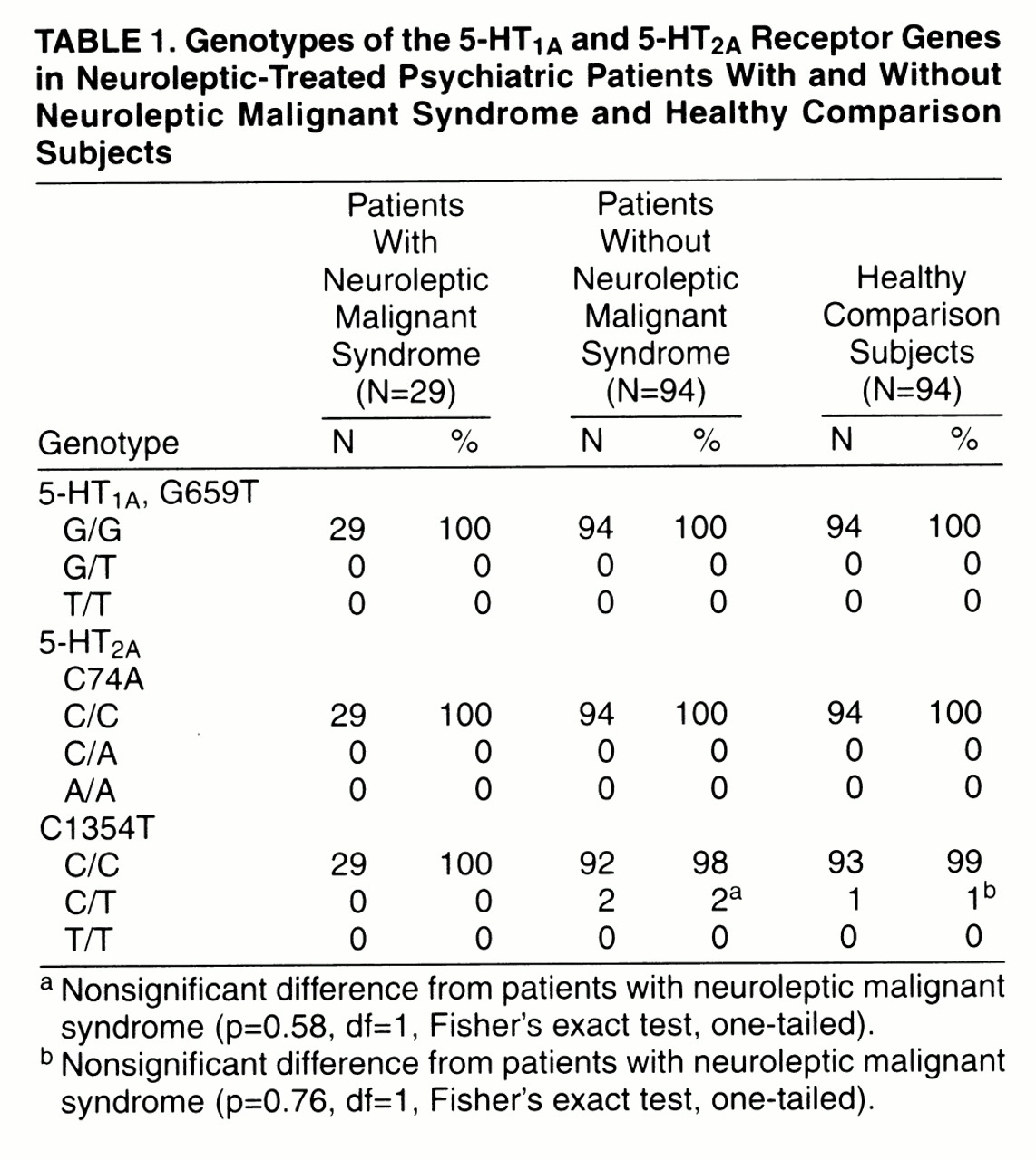
1A receptor gene, which is thought to be a very rare polymorphism in the North American population
(11), was not observed in any of the Japanese subjects in our study. The frequencies of the 74C/A and 1354C/T polymorphisms in the 5-HT
2A receptor gene were lower than those observed in a German study
(12), and none of our neuroleptic malignant syndrome patients possessed these alleles (no reference was available on 5-HT genotype frequencies in Asian populations). Consequently, there is no evidence of susceptibility to neuroleptic malignant syndrome in terms of three polymorphisms we examined in this small study group. However, we cannot rule out the existence of mutations in serotonin receptor genes that affect drug response, and further studies might be needed. The interindividual variation in psychopharmacological responses, including side effects, could be affected by genetic predisposition, and we think that the study of genetic associations is still a potent tool for investigating the development of neuroleptic malignant syndrome.
Large genetic studies are needed to investigate the mechanism of neuroleptic malignant syndrome. The goal of these genetic studies should be to predict the response to psychotropic drugs in individuals in order to permit safe and effective drug therapy.