Some postmortem studies have reported reduced density of serotonin receptors in patients with schizophrenia than in nonschizophrenic comparison subjects, but others have failed to find any significant differences between subjects with and without schizophrenia
(1). Extrapolation of postmortem data is limited because of possible changes in receptor characteristics secondary to death, postmortem delay, and tissue preparation. Furthermore, most autopsy studies use brain tissues from older patients, who have had a long course of illness and in some cases long treatment periods. All of these factors may contribute to observed differences between subjects with and without schizophrenia in serotonin receptor density. In addition, decreases in serotonin receptor density with aging have been reported in both postmortem
(2) and positron emission tomography (PET)
(3) studies. The observed decreases in schizophrenic patients in postmortem studies may reflect an increased rate of loss of serotonin receptors or a decreased number of receptors throughout the course of illness.
Two in vivo studies of serotonin 2A (5-HT
2A) binding potential using a region of interest analysis
(3,
4) have reported no significant difference between subjects with and without schizophrenia. In the absence of well-defined anatomical or functional regions of interest, a voxel-based image analysis is potentially more sensitive than a region of interest approach. In this study, we used a voxel-based image analysis to determine whether there were specific regions in which patients with schizophrenia have reduced 5-HT
2A receptor density compared with healthy subjects.
Method
This study was approved by the research ethics review board at the University of British Columbia. All subjects signed written consent forms before participating in this study. Six patients with schizophrenia (five men and one woman) and seven healthy aged-matched adults (four men and three women) between the age 18 and 28 were recruited into the study. The mean age of the patients with schizophrenia was 21.5 years (range=18–27), and the mean age of the comparison subjects was 22.5 (range=19–28). All patients had a DSM-IV diagnosis of schizophrenia. Symptom severity was assessed by using the Scale for the Assessment of Negative Symptoms (SANS) and the Scale for the Assessment of Positive Symptoms (SAPS). For the patients, the mean sum of global scores was 10.0 for the SANS and 8.2 for the SAPS. The mean duration of psychotic illness before treatment was 15.4 months (SD=22.8, range=0.5–60.0). All patients had never been given neuroleptic medications.
The normal comparison group was recruited by advertisement posters placed in the community. They were screened by using the Structured Clinical Interview for DSM-IV—Non-Patient Edition.
None of the subjects had a history of alcohol or substance abuse disorder, and none had been exposed to antipsychotic or antidepressant medications. The use of benzodiazepines before the initiation of neuroleptic treatment was permissible for the patients with schizophrenia.
Images of 5-HT
2A receptor binding were obtained with an ECAT 953B PET camera using [
18F]setoperone, prepared according to a procedure described elsewhere
(5). Data were collected in 31 contiguous axial slices covering an axial field of view of 10.8 cm. Subjects were administered 7.5 millicuries of tracer by intravenous injection over a period of 1 minute. Scanning began immediately after tracer injection. Images were collected over a period of 110 minutes in 15 frames. Structural magnetic resonance images (MRIs) were acquired by using a GE three-dimensional spoiled gradient recall acquisition sequence. The PET images were coregistered to the MRIs using statistical parametric mapping software (SPM 96) (Wellcome Department of Cognitive Neurology, London).
Time-activity curves for each subject showed that the cortical-to-cerebellar ratio reached pseudoequilibrium by the 14th and 15th frames (70–110 minutes). Therefore, the data from these two frames were averaged together for subsequent analysis. The cerebellar activity was determined as the mean of six cerebellar regions drawn on the coregistered MRIs. This mean cerebellar value was used as an index of nonspecific binding. It has been shown that under pseudoequilibrium conditions the ratio of cortical activity to cerebellar activity is linearly proportional to B
max/K
d (6). A binding potential image was created by dividing each voxel by the mean cerebellar activity.
A nondirected search of differences between groups was performed by using SPM 96. Previous reports of an age-dependent decrease in 5-HT2A receptor density was confirmed in our study. Therefore, age was entered as a covariate in the analysis.
Results
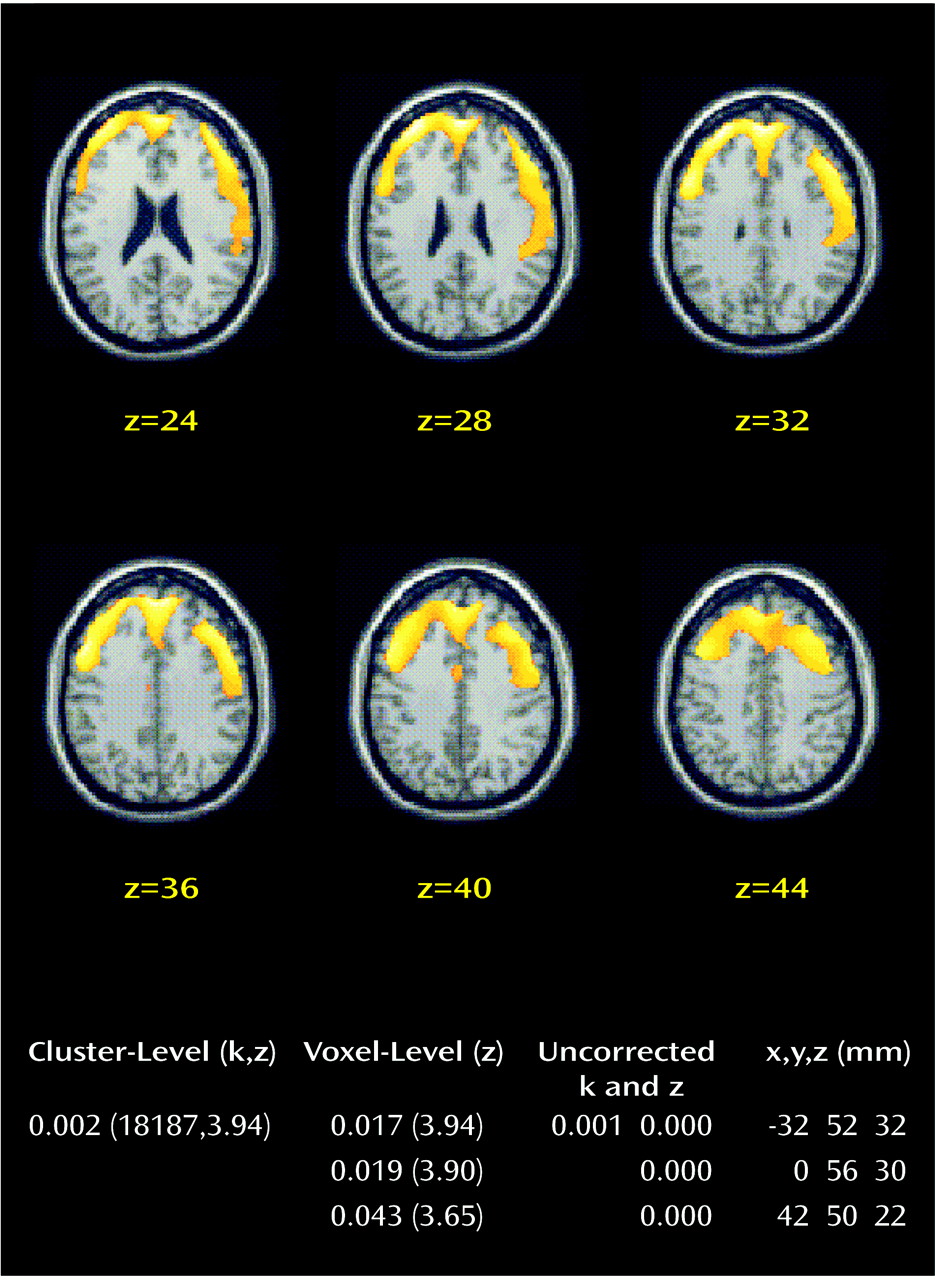
There was a significant decrease in serotonin receptor binding with age in both groups. The average decrease for the two groups combined, with the mean global value defined as the mean gray matter binding potential index for the five middle slices, was 4% per year. There were no significant differences in the age-adjusted binding potential index between men and women in the healthy comparison group. There was a significant decrease in the serotonin binding potential index in patients with schizophrenia compared with the nonpatient group in the frontal cortex. The decrease was most significant in the left lateral frontal cortex (Talairach coordinates: x=–32, y=52, and z=32 mm from the anterior commissure) (z=3.94, N=13, p<0.001; p=0.02 corrected for multiple comparisons). This voxel was part of a larger cluster encompassing both left and right prefrontal cortex (p=0.002, k=18,187, z=3.94, N=13) (
Figure 1). The age-adjusted binding potential index was 16.3% lower in the patients with schizophrenia (mean=3.25, SD=0.77) than in the healthy comparison group (mean=3.82, SD=0.37).
Discussion
To our knowledge, this study is the first positive report of significant decreases in 5-HT
2A binding potential in young neuroleptic-naive patients compared with healthy subjects. There have been two previous reports on combined neuroleptic-naive and neuroleptic-free patients with schizophrenia
(3,
4), both of which found no significant difference. Both studies used a region of interest analysis. Our finding of a 16.3% difference in [
18F]setoperone binding in the identified cluster is higher than the difference of 8%–11% reported by Lewis et al.
(3) in regions that were specified according to somewhat arbitrary criteria. In the cortex, where there are few consistent anatomical landmarks, it is difficult to define regions of interest that coincide exactly with functionally homogeneous cerebral areas. Unless the cerebral change of interest is homogeneous throughout a wide area, regions that are defined on the basis of relatively arbitrary criteria are unlikely to coincide precisely with the area in which the effect of interest occurs. Under such circumstances a voxel-based image analysis is potentially more sensitive than a region of interest approach, despite the need to perform a more stringent correction for multiple comparisons.
Our results show that the decreases in serotonin receptors previously reported at autopsy in older patients with schizophrenia are present during earlier phases of the illness and before exposure to neuroleptics. Our study does not have a sufficient number of patients to address whether there is also a difference in the rate of loss of serotonin receptors in patients with schizophrenia compared with normal subjects.