Approximately 21 percent of women experience a mood disorder and 30 percent an anxiety disorder at some point in their lives (
1). Although historically it was believed that pregnant women were at lower risk of mood and anxiety disorders (
2,
3), recent studies do not support this belief. Rather, between 10 and 27 percent of women experience depressive symptoms during pregnancy (
2,
4,
5,
6,
7,
8,
9,
10,
11,
12,
13,
14), including 2 to 11 percent who experience major depressive disorder (
2,
15,
16,
17). It remains to be determined whether rates of anxiety syndromes differ between gravid and nongravid women.
Nevertheless, less attention has been devoted to the detection and treatment of mood and anxiety disorders among obstetric-gynecologic patients (
19,
20,
21,
22,
23). In a recent study of 3,000 obstetric and gynecology patients, 20 percent of the patients met criteria for a psychiatric diagnosis, but among 77 percent of the patients a disorder was not recognized by their health care provider (
22). The only study to prospectively investigate rates of identification of psychiatric illness and referral for depression, anxiety, and substance abuse among pregnant patients (
24) found that half of patients who screened positive for a psychiatric diagnosis in an independent screening did not receive a diagnosis from their physicians and that three-quarters were not treated. No study of pregnant women has presented detection rates specific to type of psychiatric illness; nor has any study examined detection and referral for posttraumatic stress disorder (PTSD).
The main aim of the study reported here was to extend previous findings by systematically evaluating rates of detection and treatment of minor and major depressive disorder, panic disorder, and PTSD among women receiving prenatal care at publicly supported clinics.
Methods
Sample and data collection
Women were eligible to participate in the study if they were pregnant, spoke English or Spanish, and were receiving prenatal care from either of the two federally funded hospital-based obstetric clinics or two affiliated community health center obstetric programs in the New Haven, Connecticut, area. A majority of the providers (25 providers, or 58 percent) administering prenatal care at the clinics were obstetrician-gynecologists. Seven providers (16 percent) were obstetric-gynecologic residents. Other providers included certified nurse midwives (ten providers, or 23 percent) and one physician assistant (2 percent). Four providers (9 percent) were bilingual in English and Spanish.
Pregnant women were approached during their usual prenatal appointment during a six-month period from November 2001 through April 2002 on selected clinic days that changed weekly, depending on patient flow. Prenatal care providers were told that a study of moods during pregnancy was being conducted at their clinic but were not specifically told that the study involved screening for depression, PTSD, or panic disorder. Institutional review board approval was obtained from Yale University and from each participating site's institutional review board. The women were asked to provide written informed consent after the study was fully explained.
The women were screened in a private section of the waiting room, an examination room, or a private office in the clinic and received a package of diapers on completion of the interview. Screening occurred only once, at any point in the pregnancy; this approach yielded cross-sectional rates of illness. Participants included 387 pregnant women, or 98 percent of those approached. Women were on average 23.8±11.2 weeks pregnant when evaluated (range, 6.7 to 41.1 weeks). Eighty women (23 percent) were seen during the first trimester, 144 (34 percent) during the second trimester, and 163 (43 percent) during the third trimester. If suicidal ideation was identified at any point during the screening process, the patient's health care provider was notified.
Measures
Trained research assistants (social workers with educational qualifications ranging from B.A. to M.S.W.) administered a structured questionnaire before each patient saw her health care provider. The questionnaire collected information about psychiatric history (whether the participant had previously received a diagnosis of depression, anxiety, PTSD, or any other mental disorder), the patient's awareness of the clinician's diagnosis, the time at which a diagnosis was made (more than a year ago, during the current pregnancy, or during the previous year but not during current pregnancy), and whether the participant had received mental health treatment. All questionnaires were administered in an interview format. A total of 107 screenings (28 percent) were conducted in Spanish.
All patients were administered the Primary Care Evaluation of Mental Disorders (PRIME-MD) Brief Patient Health Questionnaire (BPHQ) (
25,
26), which recorded diagnoses of major depressive disorder, minor depressive disorder, or panic disorder. This questionnaire was augmented with the PTSD module from the MINI International Neuropsychiatric Interview (MINI) (
27). The BPHQ and the MINI have been independently validated (
22,
26,
27). The BPHQ has been used in obstetric-gynecologic settings and correlates highly with the Structured Clinical Interview for DSM-III-R (SCID). The overall reliability between the BPHQ and the SCID for major depressive disorder was 92 percent, for minor depression was 89 percent, and for panic disorder was 96 percent (
26). Both the BPHQ and the MINI have been validated in Spanish (
22,
28).
A diagnosis of major depressive disorder was assigned to women who met a minimum of five of the DSM-IV criteria, including either depressed mood or anhedonia, for more than half the days in a two-week interval. A diagnosis of minor depression was made for women who endorsed two to four symptoms of depression, including depressed mood or anhedonia, for more than half the days in a minimum period of two weeks. A diagnosis of panic disorder was given to women who responded "yes" to the following four items: they experienced a panic attack, the attack "came out of the blue," the attack resulted in a change of behavior, and the attack was associated with somatic symptoms. A diagnosis of PTSD was made for traumatized women who responded "yes" to reexperiencing a traumatic event and at least four PTSD symptoms—irritability, avoidance, amnesia, detachment, dissociation, foreshortened future, difficulty concentrating, and easily startled—for "several days" or more. A time frame of one month was applied for panic disorder and PTSD.
Study participants were questioned again after their prenatal visit and were asked whether they had discussed depression, panic, posttraumatic stress disorder, or any other mental disorder with their health care provider. In addition, they were asked whether they had been referred for treatment.
A medical record review using a standardized form of the patient's prenatal chart and entire medical record both from the prenatal care site and from the hospital at which the patient delivered was also performed to identify clinicians' documentation of psychiatric illness, treatment for a psychiatric illness, number of prenatal care visits attended, presence of domestic violence (previous or current), pregnancy history, major medical illnesses, and other medical problems during the current pregnancy.
Data for women who screened positive on the BPHQ for minor or major depression, PTSD, or panic disorder (N=99) were combined to assess the women as a group for current and previous health care use. If the patient's medical record documented symptoms, even when no treatment was indicated, the patient was considered to have a mental condition.
Statistical analysis
The frequencies of depressive disorder, panic disorder, and PTSD were calculated. Differences in the prevalence of mood disorders between racial or ethnic groups were examined by using chi square tests calculated by using SAS (
29). There were too few women with anxiety disorders to explore differences in rates between racial or ethnic groups.
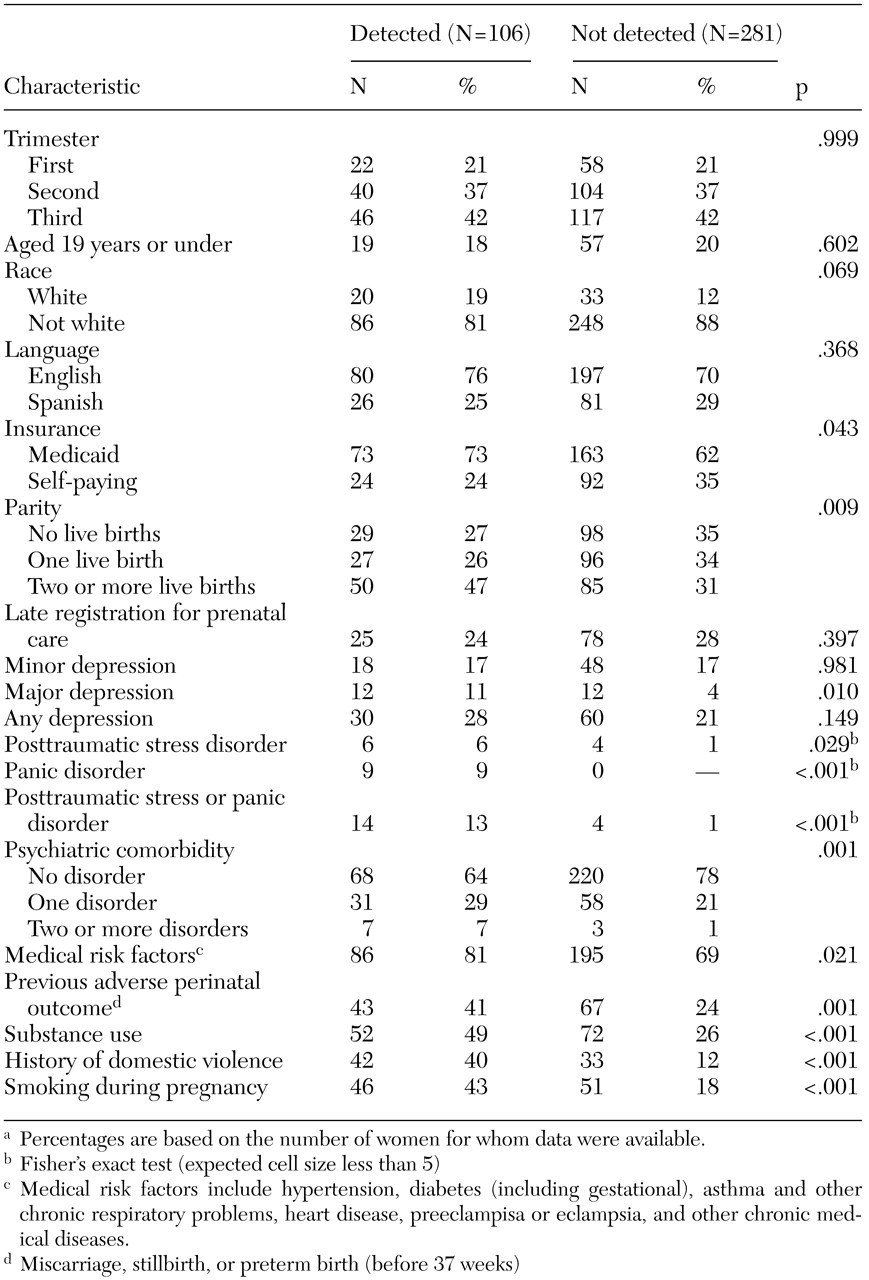
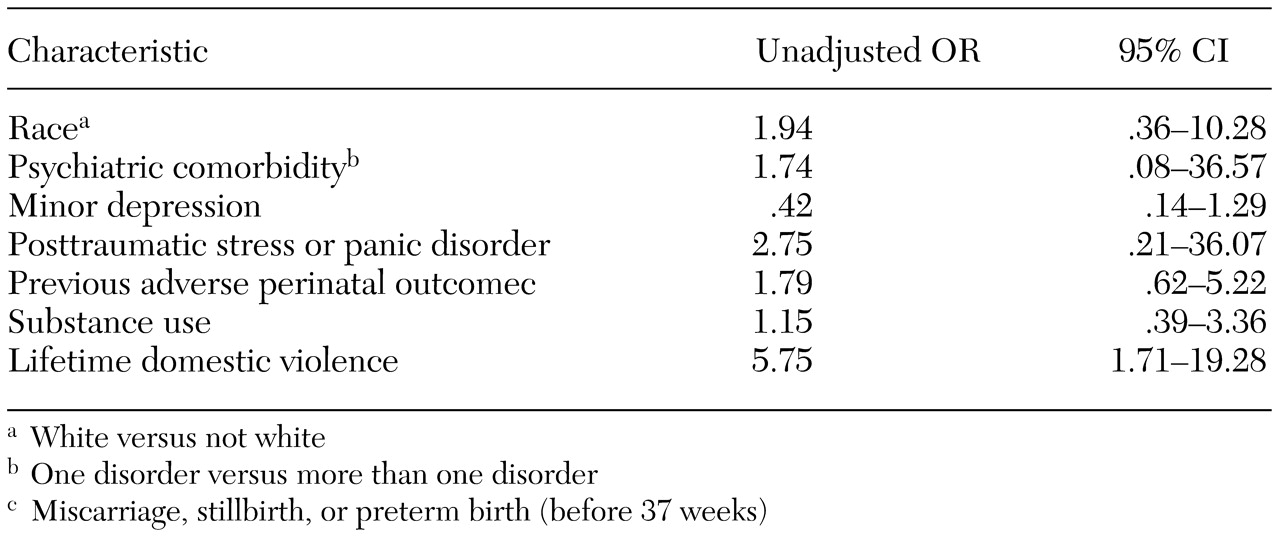
Bivariate associations between illness identification and other maternal demographic and medical risk variables, including psychiatric disorders, were computed for the cohort of 387 women by using the chi square statistic or, for expected cell sizes of less than 5, Fisher's exact test. Logistic regression (proc logistic) was used to determine which variables increased the likelihood of case identification by any health care provider among the 99 women who screened positive for a disorder. Independent variables entered into the model included those that were significant at a .1 level on bivariate testing. The final model included covariates significant at .05 or variables that were effect modifiers. For all nine women with panic disorder, the disorder was detected before or at the time of screening, bivariate odds ratios were not computed. Therefore, the combined independent variable of PTSD or panic disorder was entered into the model.
Discussion
Our findings show that mood and anxiety disorders are highly prevalent and constitute significant morbidity among low-income pregnant patients treated in publicly funded clinics. The rates of major depressive disorder (6 percent) and panic disorder (2 percent) found in this study are within the range of estimates reported elsewhere for low-income populations (
7,
17,
18,
24). To our knowledge, this is the first study to explore the likelihood that PTSD will be identified and treated in a pregnant population. The rate of PTSD we report (3 percent) was within the range reported in other epidemiologic studies. For example, the one-month prevalence of PTSD among women included in the National Comorbidity Survey was 2.8 percent.
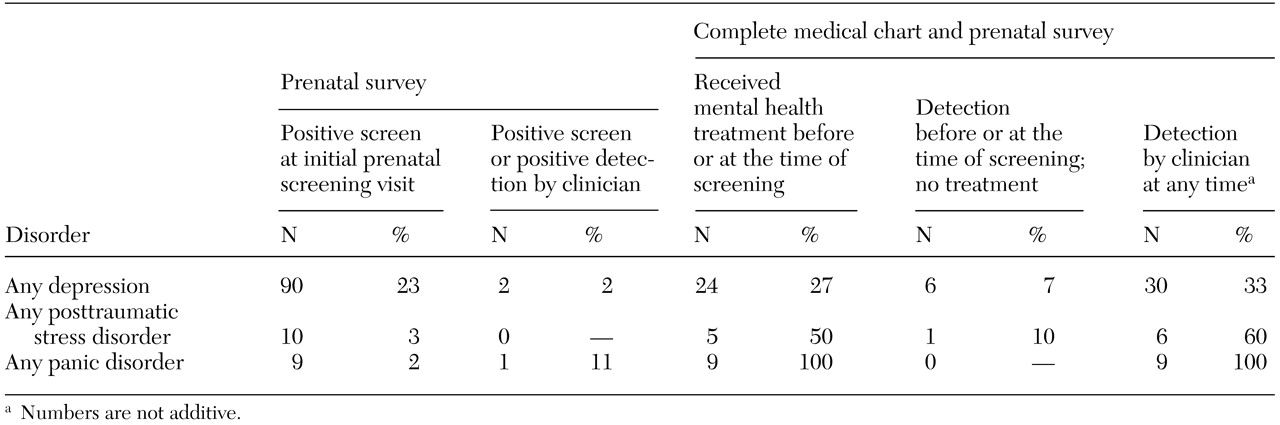
In our cohort, all but a minority of symptomatic depressed women remained undiagnosed and untreated, despite the fact that women were seen an average of six times in as many months by a health care professional. This finding is even more sobering when one considers that 18 percent of women with undetected depression had suicidal ideation that was experienced at least several times a week. Only 2 percent of the women with a depressive disorder, none of the women with PTSD, and 11 percent of the women with panic disorder received a diagnosis from a health care professional at their prenatal visit.
When we evaluated rates of any detection of psychiatric illness, operationalized as patient report or documentation in the medical chart of any symptoms or treatment, only 26 percent of psychiatrically ill patients were recognized as having a mood or anxiety disorder. On the other hand, it is notable that all nine women who screened positive for panic disorder reported receiving mental health treatment before or at the time of screening. Rates of anxiety disorder detection in primary care settings are typically quite low (
22). Therefore, it is unusual to find that the nine cases of panic disorder were detected in an obstetric setting. One reason may be that panic disorder typically presents in the form of physical symptoms, such as breathing difficulties or tightness in the chest, that can mimic catastrophic illnesses such as heart attacks or pulmonary emboli. It may be that prenatal health care providers are more watchful of serious general medical conditions that affect the mother or the fetus and thus thoroughly evaluate somatic symptoms like shortness of breath and chest pain.
Women were more likely to have their depressive or anxiety disorder identified by a health care provider if they reported previous or current domestic violence. Although this finding needs to be confirmed in a larger sample, it suggests that women with severe forms of psychosocial stress are more likely to receive a diagnosis. Kelly and associates (
24) found a similar result in that concurrent pregnancy risk factors, such as not living with a partner, involvement of child protective services, and history of abortion, increased the likelihood of chart-documented mental health evaluation or treatment. Furthermore, detection could also be higher among women who have been the victims of domestic violence, because they are more likely to seek medical attention (
30).
Although detection rates for depression in obstetric-gynecologic practices are moderate (15 percent to 30 percent) (
19,
20,
21,
22,
23) and are somewhat lower than those for other primary care providers (35 percent to 56 percent) (
31,
32,
33,
34), the recognition of depressive and anxiety disorders among pregnant patients (27 percent) was less than that found in other reproductive health settings (
22,
24,
32). One of the few studies to examine detection and treatment of depression, substance abuse, and panic disorder among pregnant women (N=186) noted that only 18 percent of those who had a diagnosis were identified by clinicians and that only 37 percent of those identified had any symptom recorded in the patient chart (
24). Our results are in line with these findings, although we did find higher detection rates specifically for panic disorder and PTSD. Our study differed from the one mentioned above in that we used patients' self-reported diagnoses in addition to diagnostic information from medical record reviews to determine whether clinicians identified a patient as psychiatrically ill.
The low detection and referral rates for depression among pregnant patients may be a result of a number of factors. Clinicians may be reluctant to ask questions, and patients may avoid reporting problems that arise from depression or anxiety. Symptoms of depression during pregnancy may not raise clinicians' or patients' concerns given that several of these experiences—for example, disturbances in appetite, sleep, and energy levels—are normative for many pregnant women (
15,
35).
Other possible contributions include time constraints, insurance and referral limitations, and provider education and training. Large survey studies have shown that a majority of obstetric-gynecologic residents neither received training about clinical depression during their residency (80 percent) nor completed a continuing medical education course on the treatment of clinical depression among women (60 percent) (
23,
36). Approximately 50 percent of obstetrician-gynecologists cite incomplete knowledge of diagnostic criteria as a barrier to identification of depression (
23). The expectation that obstetric and gynecologic practitioners will diagnose and treat common mental health disorders is of recent origin, and many providers may not think that it should be part of their clinical responsibilities (
36).
In addition, as in other studies of primary care, nonpsychiatric providers may be less familiar with psychiatric diagnostic codes or may fear that patients will be stigmatized if they are given a chart-recorded diagnosis (
37,
38). In our cohort and in many obstetric settings, a large proportion of women see certified nurse midwives. It is not clear that the training of midwives adequately addresses the identification and management of mood and anxiety disorders (
39,
40).
There are important considerations in interpreting the results of this study. The study was not designed as a prevalence study, and it is not known whether our rates are similar to those in other community settings. Nevertheless, illness rates are consistent among studies that screened for depression in obstetric settings (
41). However, one might hypothesize that because depressed women initiate prenatal care later than women who are not depressed (
24,
42), studies may underestimate the illness rates and treatment need.
Our method for assessing rates of identification should also be considered. We deemed a patient as having a "detected" disorder if she reported detection or if there was documentation in the medical chart. Therefore, the results of this study are subject to reporting bias. It is possible that providers made a diagnosis and referred the patient but that the patient did not accurately report the diagnosis and referral and the clinician did not document them in the chart. In addition, because the BPHQ relies on patient self-report, definitive psychiatric diagnosis must be verified by a clinician to determine how well the patient understood the questionnaire and other relevant clinical information. Although the BPHQ performs well in validity studies (
22,
26) with
DSM-IV, it is possible that it overestimated or underestimated the rate of depression and panic disorder in this study.
Finally, an additional limitation of the study is that we did not determine the duration of a depressive episode. Thus women could have been nondepressed at five of the average six visits. We believe that this is unlikely given that the mean and median duration of major depressive disorder has been found to be about ten weeks (
43). The high rate for endorsement of suicidal symptoms in our cohort indicates substantial morbidity and severity rather than mild and transient episodes of illness.