Posttraumatic stress disorder (PTSD) is a chronic, disabling disorder (
1) for which efficacious treatments are available (
2,
3). Yet few studies have examined the use of mental health services by persons with PTSD.
Studies of mental health service use after trauma exposure have yielded inconsistent results. A few studies have focused only on exposure to trauma without assessing PTSD. For example, persons who have been sexually assaulted appear to be more likely to seek mental health care than those who have not, regardless of gender or ethnicity (
4). In contrast, after experiencing personal victimization, adolescents were less likely to use mental health services than adolescents who had not been victimized when background characteristics were controlled (
5). Moving beyond simple trauma exposure studies, one study showed that crime victims who were experiencing depressive symptoms and those who were the victims of violent crimes were more likely to seek care (
6). However, that study did not assess PTSD symptoms.
Comparisons of persons with PTSD and those without PTSD have shown greater use of mental health services among those with PTSD in samples of psychiatric outpatients (
7) and veterans (
8) as well as greater use of substance abuse inpatient services among substance users (
9). Yet studies based on community or traumatized samples show that persons with PTSD tend not to seek care for mental health problems (
10,
11) and that rates of service use are low relative to need (
12).
Predictors of mental health care after trauma include having previous contacts with the mental health system (
5), having had previous mental health problems (
13), and having more severe PTSD (
10). Few studies have examined multiple predictors, and only one has applied a conceptual framework in examining service use. A recent study applied the behavioral model of health service use (
14) to treatment seeking among 2,713 persons with PTSD who presented for National Anxiety Disorders Screening Day (
15). The researchers found that need factors (interference of anxiety symptoms with daily life and diagnosis of panic disorder), predisposing demographic factors (age and marital status), and social structure factors (race or ethnicity) all influenced the use of services for PTSD. Older, white, divorced or separated, unemployed, and disabled persons were the most likely to seek care. When demographic factors were controlled, persons who had anxiety that interfered with daily activities or who had panic disorder were most likely to seek care (
15). However, the study had limitations, including its use of a nontraditional method for establishing PTSD diagnosis, its cross-sectional design, and its use of a self-selected sample of participants, a majority of whom had sought services in the past (75 percent).
In the prospective study reported here, we examined the natural pattern of use of mental health services in the year after hospitalization for an injury caused by community violence. We assessed the need for services in the sample; the rates of use and types of mental health services used in the year before and after the injury; factors that predicted which individuals sought care; and perceived barriers to use of care. In accordance with the behavioral model of health service use (
14), we expected both predisposing and need variables to influence the use of mental health services. Specifically, we expected that the persons with the greatest need and those with previous experience with treatment would be more likely to seek care.
Methods
Study participants and procedures
Data were collected as part of a larger prospective study focusing on the mental health consequences of exposure to community violence that resulted in significant physical injury (
16,
17). Participants were recruited after admission to a large level 1 trauma facility in Southern California for treatment of physical injuries stemming from community violence. The study procedures were approved by local institutional review boards, and informed consent was obtained from participants.
Between October 1998 and June 2000, we attempted to screen for eligibility all consecutively hospitalized persons aged 18 to 35 years who were admitted for treatment wounds stemming from community violence. To be eligible for the study, participants had to have sustained an injury inflicted by a person other than a family member or a former sexual partner and had to be able to communicate fluently in English or Spanish. Participants completed a short interview to screen for eligibility only after they were judged to be medically capable of being interviewed through discussions with medical staff.
Using computer logs, we identified 1,237 individuals who were potentially eligible for the study and screened 653 of them. The primary reason for not screening a potential participant was discharge from the hospital before an approach could be made, although five patients did refuse to participate in the screening interview. Among those who were screened, 423 (65 percent) met the eligibility criteria. Of these, 413 (98 percent) completed a baseline interview. Of the 413 individuals who were originally interviewed, 248 (59 percent) completed both three-month and 12-month follow-up interviews. The vast majority of participants were men (93 percent). Because there were too few women in the sample to enable us to properly investigate the predictors of service use among women, we included only the 231 male participants in our analysis.
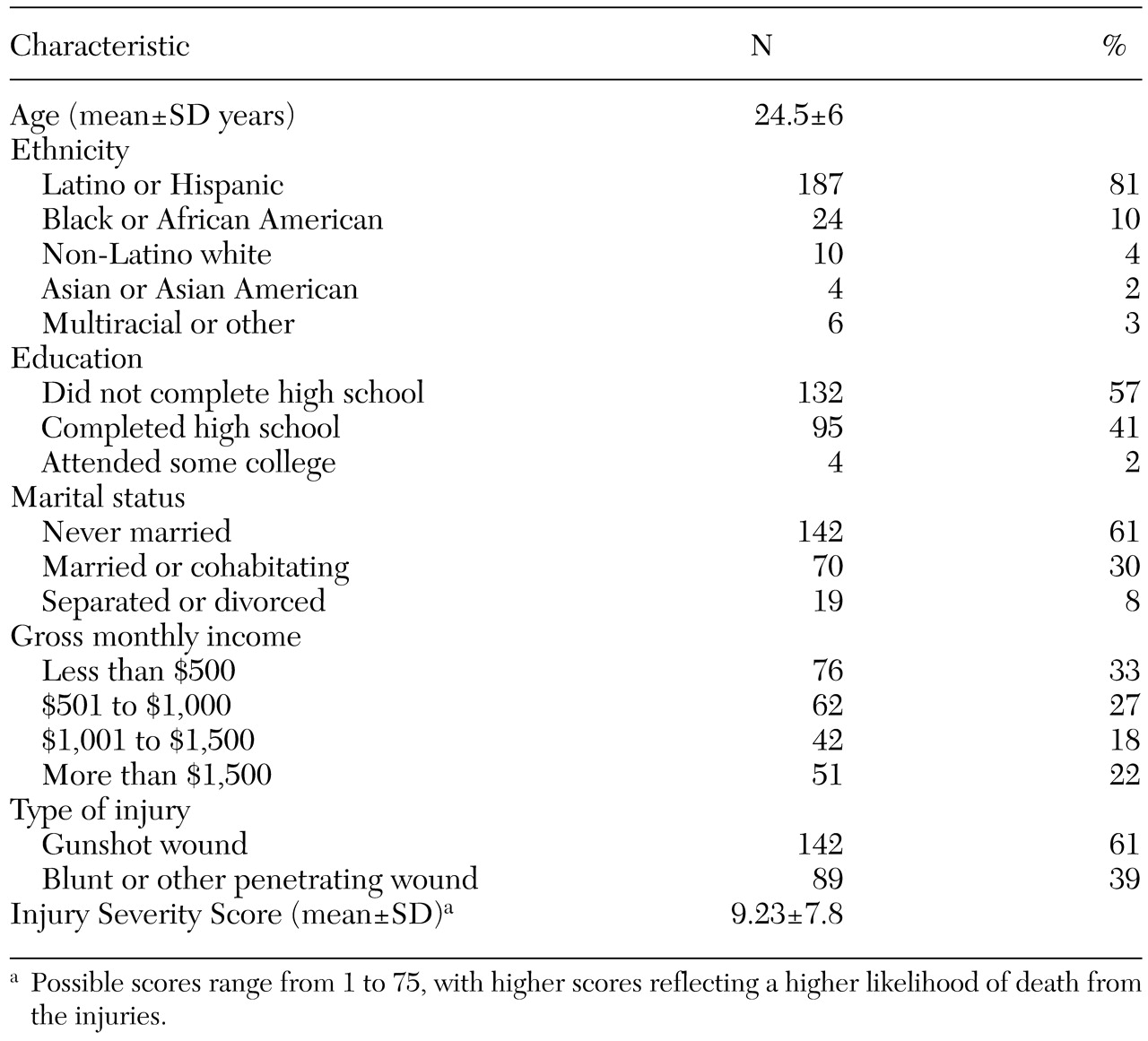
Participants completed assessments within several days of hospital admission (mean±SD=7.3±8.8 days, median=4, mode=1) and again three and 12 months later. The attrition pattern was not significantly related to the baseline measures used. The resulting sample comprised mostly Latino and impoverished men who had sustained mild to moderate injuries, predominantly resulting from gunshot wounds, as can be seen from
Table 1.
Measures
The survey was an orally administered, fully structured self-report questionnaire read by highly trained lay research assistants. A Spanish version of the survey was developed through a process of translation into Spanish, back-translation into English, reconciliation of discrepancies, and pilot testing. Monolingual Spanish speakers completed the Spanish version, which was read by fluent Spanish speakers.
PTSD symptoms and status. The severity of PTSD symptoms was assessed at each interview by summing the 17-item PTSD Checklist (PCL), Civilian Version (
18). Respondents answered the questions with reference to a specific assault, for the period since the attack, and, in the case of the follow-up interviews, for the past seven days (
18). The PCL has solid psychometric properties, construct validity, and good concordance with diagnoses established through semistructured clinical interviews (
19,
20,
21). We scored the PCL to indicate the presence or absence of a possible diagnosis of PTSD by counting the number of symptoms that received an endorsement of at least "moderately" and assessing whether each participant had endorsed symptoms consistent with a diagnosis—for example, one reexperiencing, two arousal, and three avoidance symptoms (
18).
Use of mental health services. We assessed use of services for mental health problems at each interview by asking about particular types of services that were obtained. We assessed lifetime use of mental health services at baseline, including overnight stays in a hospital or treatment program, visits to a physician or a mental health specialist, and prescription of any medication. At each follow-up interview, we asked about these same types of services for the interval since the last interview. Because rates of service use were low, we summed service use during these two intervals to create a 12-month follow-up mental health service use variable that covered the entire year after the injury. Service use included any of the mental health contacts defined above.
Perceptions of problems and service use. At the 12-month interview, we used several items to assess the way in which respondents understood their problems and their service use. First, we assessed their perception of any problems related to the attack. We asked, "Do you believe that you have had emotional or adjustment problems—including problems with drinking or drug use—because of the attack?" This item used a 5-point response scale: definitely yes, probably yes, not sure, probably no, and definitely no.
Second, we assessed the perception of lack of care with one item: "Since the attack, was there ever a time when you didn't get as much mental health care for emotional or personal problems related to the attack as you needed? Please include any problems because of the attack with alcohol or drugs."
Finally, we assessed barriers to care among participants who indicated a lack of care in the previous 12 months. Respondents checked off the main reasons they didn't get as much help as they needed from a list of 12 possible barriers.
Injury severity. We used hospital computer records of Injury Severity Scores (
22) to assess severity. The Injury Severity Score system incorporates information about the site and extent of injuries into a single score ranging from 1 to 75, with higher scores reflecting a higher likelihood of death from the injuries.
Neuroticism. Dispositional neuroticism was assessed with five items drawn from the 12-item neuroticism scale of the Five-Factor Inventory (NEO-FFI) (
23). The subset of items was selected because of considerations about respondent burden and was averaged to form a scale that had an internal consistency reliability estimate of .79.
Analysis
We used descriptive statistics to address the questions about rates of need for services and service use (frequencies and cross-tabulations). To examine predictors of mental health service use, we began with separate bivariate logistic regressions and examined odds of service use in relation to each predictor. We then entered all these predictors into a multivariate logistic regression and used stepwise deletion of predictors (removing those with p values greater than .1) to examine independent effects of these predictors. We then replicated this model in the symptomatic subsample. Because this was a preliminary study, we did not correct for type 1 error. Analyses were performed with SPSS 11.0 for Windows.
Results
Need for services
Although participants could not meet criteria for a diagnosis of PTSD at the baseline assessment because their symptoms had not lasted for at least one month, 60 (26 percent) of the 231 participants had possible PTSD without this duration requirement. At the three-month assessment, 63 (27 percent) had possible PTSD, and 42 (18 percent) had possible PTSD at 12 months. For simplicity, throughout this article we describe individuals as being objectively "in need" if they had possible PTSD at either follow-up assessment (34 percent of the sample).
We assessed subjective need by asking participants at the 12-month assessment whether they perceived a problem related to their injury. A total of 38 participants (16 percent) endorsed this item (25, or 11 percent, said "probably yes," and 13, or 6 percent, said "definitely yes"), whereas 22 participants (10 percent) were not sure, and 171 (74 percent) did not perceive a problem.
Possible PTSD and perception of a problem at follow-up were not perfectly matched. Agreement across the two measures was only 67 percent (58 percent without a problem and 9 percent with a problem). Importantly, 25 percent of the sample had possible PTSD but did not perceive that they had a problem.
Use of mental health services
A total of 34 participants (15 percent) reported any lifetime use of mental health services before their injuries. A minority of patients sought mental health care in the year after their injury, with only 34 (15 percent) reporting use of services during that period. A majority of these services were outpatient—a visit to either a physician or a specialist (29 participants, or 13 percent) or use of medication (25 participants, or 11 percent)—rather than hospitalization (six participants, or 3 percent). To eliminate the potential confounding effect of previous treatment and examine new service use only, we also assessed service use among participants with no treatment history (N=197). Here rates of service use were slightly lower: 24 participants (12 percent) received services—19 (10 percent) visited a physician or a specialist as an outpatient, 16 (8 percent) received medications, and three (1.5 percent) were hospitalized.
Predictors of service use
We examined the hypothesis that persons in need of mental health services would seek services at a higher rate in the year after their injury than those without need, and we found support for the hypothesis. Specifically, 19 (24 percent) of the 79 participants with possible PTSD at follow-up reported use of services, whereas only 15 (10 percent) of the 152 without possible PTSD reported service use (χ2=8.33, df=1, p<.01). Similarly, the rate of service use was greater among those who perceived a problem than among those who did not; 13 (34 percent) of the 38 participants who perceived a problem reported greater use of mental health services, compared with 21 (11 percent) of the 193 participants who did not (χ2=13.77, df=1, p<.001).
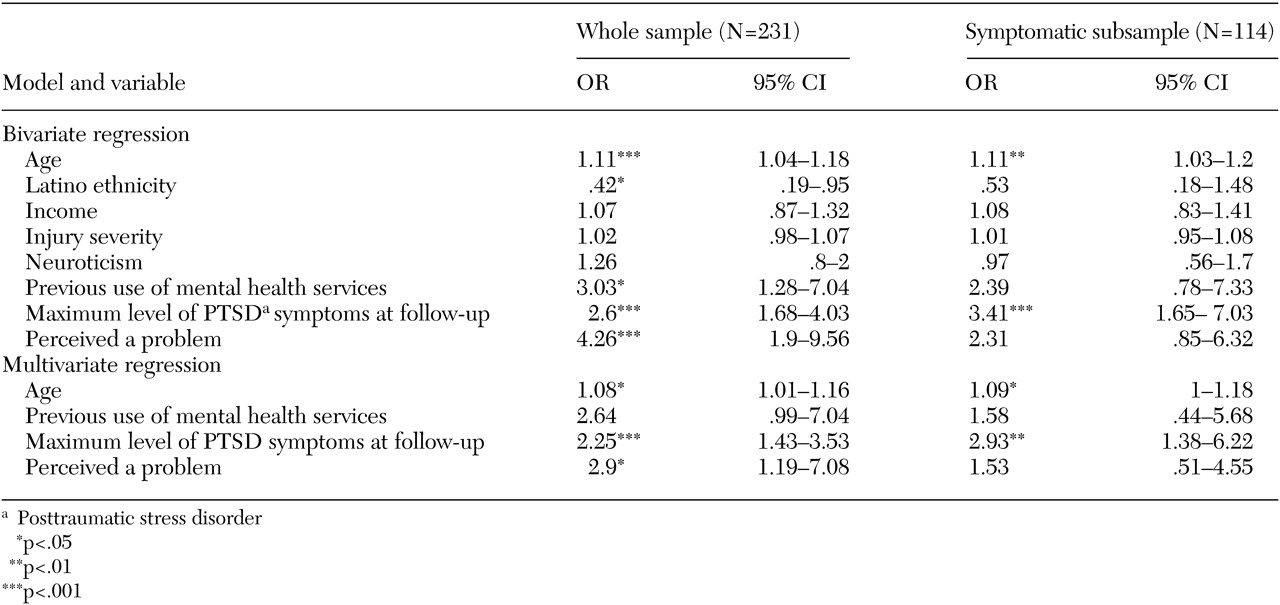
In a series of bivariate logistic regressions predicting postinjury service use, we examined age, ethnicity (Latino versus non-Latino), income, severity of injury, neuroticism, previous use of mental health services, maximum level of PTSD symptoms at follow-up, and perception of a mental health problem related to the attack. We used the dimensional symptom severity measure of PTSD rather than the possible PTSD indicator to improve the sensitivity of this measure. Analyses revealed that only age, Latino ethnicity, previous use of mental health services, maximum level of PTSD symptoms at follow-up, and perception of a problem were related to postinjury mental health service use (
Table 2).
The study sample included some asymptomatic participants who would have no reason to seek mental health services, which potentially biased our results. We therefore conducted the same set of analyses on the subsample of 114 persons who were symptomatic during the study period, defined as those who reported symptoms averaging 2.5 (a score between moderate and severe) at any of the assessments. Among symptomatic participants, only age and maximum level of PTSD symptoms emerged as significant predictors of use of mental health services.
In the reverse stepwise multivariate logistic regression predicting service use in the year postinjury, we built a model in which age, previous use of mental health services, maximum level of PTSD symptoms at follow-up, and perception of a problem were included as predictors and found that all of these except for previous use of services predicted service use in the year postinjury (
Table 2). The resulting model correctly classified 86 percent of participants, with good fit according to the Hosmer and Lemeshow test (χ
2= 11.50, df=8, p=.18).
We then replicated this model in the symptomatic subsample and found that age and maximum level of PTSD symptoms at follow-up remained significant, whereas perception of a problem did not. The resulting model correctly classified 81 percent of participants, also with good fit (χ2=8.13, df=8, p=.42). Thus we found few predictors of mental health service use beyond the fact that older and more distressed persons are more likely to seek care. However, our sample was small, particularly in the subsample analysis, which limited our power to detect real effects.
Perceived lack of care and barriers to care
Thirteen participants (14 percent) perceived a lack of services in the 12 months after the attack. Those who reported a lack of care identified specific barriers to receipt of care, which are listed in
Table 3. The most frequently endorsed item was a belief that they could deal with the problem themselves.
Discussion
This prospective study of use of mental health services after injury through community violence provided some important new information. With the exception of the survey item that assessed reasons for treatment seeking, which was administered only at the 12-month assessment, the measures used in this study are likely to be relatively free of the recall biases that plague retrospective or cross-sectional studies.
Our results indicate low rates of service use relative to need, with 34 percent of the sample having possible PTSD at follow-up but only 15 percent reporting any mental health service use during the year postinjury. Although this rate seems low, it is consistent with rates of service use for the general population of persons in need. Indeed, a general population study showed that only about 28 percent of persons with a mental disorder saw any health care professional during an average of 2.8 years of follow-up (
24).
As might be expected, objectively determined need and subjectively reported need were not entirely consistent with one another, so we included both in our models. The fact that perceived need predicted service use even when PTSD symptoms were controlled indicates the importance of this factor, which is consistent with studies among persons with serious mental illness (
25). Although perceived need did not remain significant in the symptomatic subsample, this could have been due partly to the correlation between objective and perceived need and to the fact that the number of participants in the subsample analysis was small.
When other factors were controlled, having more severe symptoms and being older increased the odds of service use, which is consistent with the results of other studies (
10,
15). Perceived barriers cited by participants who reported a lack of care included a belief that they could deal with their problems themselves, a lack of knowledge about where to go for help, inconvenience, a belief that they couldn't be helped, and worry about the cost. Thus barriers included issues related both to a lack of knowledge about PTSD and its treatment and structural barriers to care.
Our prediction that participants who had used mental health services before the injury would be more likely to use services after the injury was not supported, although inspection of the parameter estimates showed that this factor might have been predictive if we had had a larger sample.
A strength of this study was its focus on victims of community violence, which disproportionately affects young males (
26,
27,
28) and ethnic minorities (
29), distinguishing it from other forms of interpersonal violence. However, the study's focus on men from ethnic minorities is also a limitation, because we were unable to examine gender or ethnic minority status as predictors of service use. In addition, the sample was restricted geographically to one urban area, and the injuries were in the mild range, although all required hospitalization. Our ability to screen only about half of potentially eligible trauma survivors may also have limited the generalizability of our results. Nonetheless, this study complements the literature on female assault survivors and informs us about another population that is clearly in need of services. Further exploration of roles of ethnicity and gender in help seeking are clearly needed.
Conclusions
Despite high rates of need for services related to PTSD after violent injury, the rate of use of mental health services was low in this sample. These results may help to inform outreach and early intervention efforts. The fact that 25 percent of the sample had possible PTSD yet did not perceive that they had an emotional problem suggests the importance of psychoeducational intervention. Helping people understand the emotional consequences of violent injuries may pave the way for help seeking. However, educational interventions may not be sufficient to promote help seeking, given that only 34 percent of the study participants who perceived a problem sought care in the year after the attack. Thus further studies are needed to better understand the reasons for not seeking care.
Acknowledgments
This work was supported by grant MH-56122 from the National Institute of Mental Health and by a grant from the William T. Grant Foundation. The authors thank David Foy, Ph.D., Suzanne Perry, and Howard Belzberg, M.D., for their help with the conceptualization and implementation of this study and Stacey Kaltman, Ph.D., Lori Frank, Ph.D., Bonnie Green, Ph.D., Jeanne Miranda, Ph.D., and Mary Ann Dutton, Ph.D., for helpful comments.