Light therapy is an effective antidepressant for the winter depressive symptoms in patients with seasonal affective disorder
(1–3). Although clinical experience suggests that mood improvement following light treatment is smaller than the spontaneous improvement during summer, this difference has never been formally documented.
METHOD
We recruited patients with seasonal affective disorder by newspaper and radio advertising in the metropolitan Washington, D.C., area. Patients met the criteria of Rosenthal et al. for seasonal affective disorder
(1) and DSM-IV criteria for a past major depressive episode. The criteria of Rosenthal et al. require at least one past major depressive episode and at least 2 consecutive years in which depression developed in fall or winter and remitted in spring or summer. To start light treatment, a subject had to have a typical depressive score of at least 14 or a minimum typical score of 12 with a total depressive score of at least 20 on the Hamilton Depression Rating Scale, Seasonal Affective Disorder Version
(4). We excluded patients if they had comorbid axis I psychiatric conditions or medical problems or were taking psychotropic medication. Twenty-two patients were eligible, of whom 15 were enrolled in this study (two patients required antidepressants when they did not respond to light, one underwent surgery, and four were unavailable for follow-up). Patients signed informed consent forms. Their mean age was 44.2 years (SD=10.6). Eleven (73.3%) were women and four (26.7%) were men. Nine patients (60%) had unipolar depression, and six (40%) had bipolar disorder.
We rated mood by administering the Hamilton Depression Rating Scale, Seasonal Affective Disorder Version
(4), once during winter when the patients were depressed, once during winter after 2 weeks of light therapy, and once during the following summer. Response to light was defined as at least a 50% decrease in baseline score and a total posttreatment score of 7 or lower on the Seasonal Affective Disorder Version of the Hamilton depression scale
(5). Eight of 15 patients responded to 2 weeks of light treatment, and 13 of 15 patients responded in summer (difference not significant by McNemar test for significance of changes, with Yates’s correction for continuity: χ
2=2.29, df=1, 0.10<p<0.20).
Light treatment consisted of a standard regimen of 10,000-lux cool-white fluorescent light therapy for 45 minutes twice daily. After 2 weeks of the standard regimen, the treatment was individually customized and gradually tapered in spring.
We initially analyzed the patients’ scores on the depression scale by using the Friedman’s two-way analysis of variance with conditions (depressed, light-treated, and summer) as factors. We then compared typical, atypical, and total depression scores across light-treated and summer conditions by using the Wilcoxon signed ranks test. The criterion alpha (two-tailed) was set at 0.015, with a Bonferroni correction for multiple comparisons.
RESULTS
The Friedman analysis for total scores on the depression scale showed a significant effect for condition (Friedman test statistic=26.3, df=2, p<0.001). Similarly, we found a main effect for condition when we applied the analysis to typical (Friedman test statistic=24.4, df=2, p<0.001) and to atypical (Friedman test statistic=26.23, df=2, p<0.001) scores.
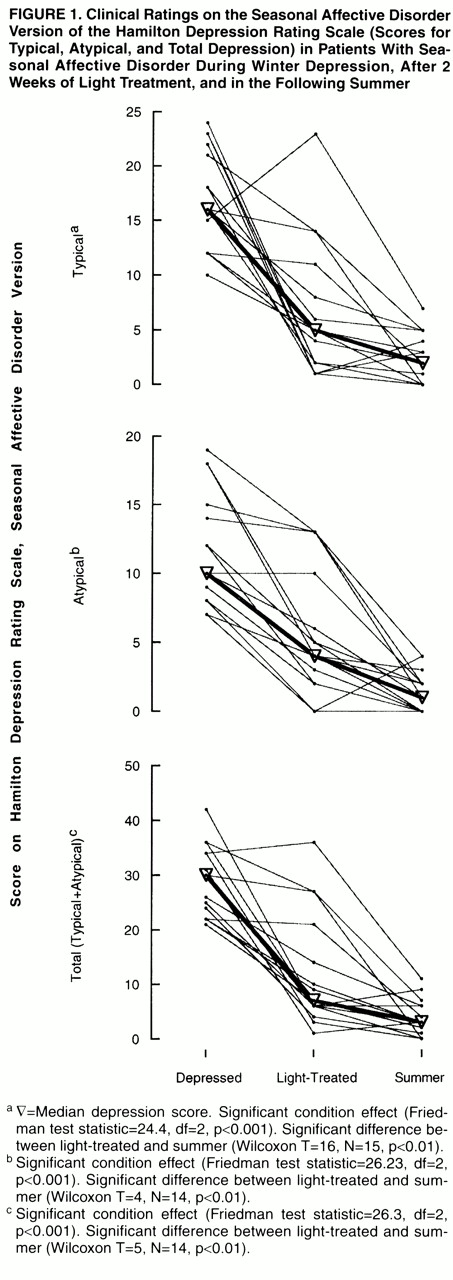
Further Wilcoxon signed ranks test comparisons of light-treated and summer conditions showed that depressive scores were significantly lower in the summer than after light therapy (
figure 1). The median total depression score (30 in depressed state) fell from 7 in the light-treated condition to 3 in the summer (T=5, N=14, p<0.01) The median typical depression score (16 in depressed state) fell from 5 in light-treated condition to 2 in the summer (T=16, N=15, p<0.01). The median atypical depression score (10 in depressed state) decreased from 4 in light-treated condition to 1 in the summer (T=4, N=14, p<0.01).
DISCUSSION
To our knowledge, this is the first report suggesting that mood improvement with conventional light treatment in depressed patients with seasonal affective disorder is not as complete as the spontaneous remission occurring in summertime. In order to verify the seasonal pattern of seasonal affective disorder in participants in a light-treatment study, Magnusson and Kristbjarnarson
(6) rated nine patients with seasonal affective disorder in the summer following light treatment but found no statistically significant difference in the depressive scores between postlight and summer conditions, possibly because of insufficient statistical power.
Our finding cannot be explained in terms of the development of summer hypomania in bipolar patients. First, hypomanic symptoms would tend to increase rather than decrease the typical depressive symptoms. Second, we examined post hoc, separately in unipolar and bipolar patients, the changes in mood between the light-treated and summer conditions; the results in the two subgroups were very similar. The small sizes of these subgroups do not, however, allow for a proper statistical analysis. Such an analysis might be accomplished by future studies on larger groups.
We recognize that there is an ordering effect that may have confounded our result, given that all subjects received light therapy before the arrival of summer. It is, therefore, possible that our finding is due to an overall trend toward improvement with time. It is also possible that a longer trial of light therapy may have yielded effects comparable to those of summer as it has been suggested that further gains are seen beyond 2 weeks’ treatment
(7). Nevertheless, the amount of light treatment given in this study is equivalent to, or greater than, that given in most clinical trials
(5, 8). Moreover, in our study, the rate of response in summer according to the Terman et al. criteria
(5) was 86%, which is superior to the 67% response rate after 4 weeks of light therapy reported by Bauer et al.
(7).
A number of factors—for example, the summer-winter differences in photoperiod, light intensity, and amount of ultraviolet radiation reaching the eye and skin—might have contributed to the superior antidepressant effects of summer as compared with light therapy. Consistent with this last suggestion is a recent report on the possible influence of light exposure to skin on circadian rhythms
(9). Besides light, other physical factors, such as temperature, as well as chemical, biological, and socioeconomic variables, differ between winter and summer and may have an effect on mood and behavior. The influence of these factors on patients with seasonal affective disorder may well be worth studying in their own right.