Jerusalem has been subjected to numerous terrorist attacks over the last 60 years, even before modern Israel reached independence (1948). From 1967 through September 2003, there were 486 attacks, with 510 persons killed and 2,636 injured
(1,
2) . During the present armed
intifada (Arabic for insurrection), terrorism has escalated steeply, often including the suicide/homicide bomber modality targeting civilians
(3) . To illustrate, while five large-scale terrorist attacks occurred in Jerusalem between 1995–1997, and four civilians were killed in isolated attacks in 1998, since the beginning of the intifada in late September 2000 through December 2002 the number of attacks rose to 21. These later attacks caused 146 deaths, both of adults and children, untold number of wounded persons, and considerable property damage
(2) . Including the surrounding areas of Jerusalem, the number of terrorist episodes during this period reached 68, with 182 dead and 1,160 wounded.
Terrorist attacks leave in their wake personal and community sequelae of different duration and intensity
(4 –
17) . The psychological and psychopathological effects of terrorism on urban populations (e.g., Northern Ireland [
8,
9 ] and Algeria
[10] ) have been raised anew in the literature following the 2001 events in the United States. The effects may be examined with regard to their psychiatric impact
(14), the population-level behavior
(17), and the human suffering that falls outside the psychopathological domain
(11) . In the United States, the reactions are a matter of ongoing research, with results
(12 –
16,
18) suggesting that the psychiatric impact of the September 11 events may be similar to findings made in other disasters
(19) in that exposure is a risk factor for anxiety, depression, and posttraumatic stress disorder (PTSD).
Prior to the current intifada, several studies were conducted in Israel on the effects of the Iraqi missile attacks during the 1991 Gulf War. The results indicated early elevated cardiovascular mortality
(20) as well as worsened self-appraisal of physical health status, increased smoking, diminished physical activity, changed diet habits, and increased psychological distress
(21) . One study explored reactions among the elderly and found an increased vulnerability among Holocaust survivors
(22) . Nakar et al.
(23) studied general practitioner burden in a highly exposed area and found a decreased total rate of visits. In addition, a laboratory study exploring the Gulf War impact on anxiety and cortisol and growth hormone levels showed that biological measures were within normal limits, presumably as a result of adaptation
(24) .
How does terrorism affect psychiatric services utilization by the general population? American reports suggest that psychiatric services were used sparingly after September 11
(15,
25 –32) but that there were increases in prescriptions of anxiolytic drugs by non-psychiatrists
(27) as well as by existing users
(28) . A similar pattern of changes in service utilization had been noted in Northern Ireland, where terrorism has been long-lasting
(8) . Despite reporting relatively elevated rates of traumatic stress-related symptoms, a low proportion (5.3%) of Israelis sought professional help according to a national telephone survey conducted during the current intifada
(6) .
Thus, the New York, Northern Ireland, and Israel studies suggest that under the stress of terrorism there are changes in some, but not all, health behaviors. In the study reported here we examined a comprehensive mosaic of routinely collected mental health and general health service indicators to ascertain intifada-related health utilization demands of specialized and nonspecialized services among Jerusalem residents.
Discussion
Our inquiry focused on a single behavioral dimension, health service use, among the general population in response to terrorism. Analogously, Stecklov and Goldstein
(17) focused on driving behavior during part of the period we covered. Neither that study nor ours targeted people that survived the attacks or were bereaved by the loss of a significant other.
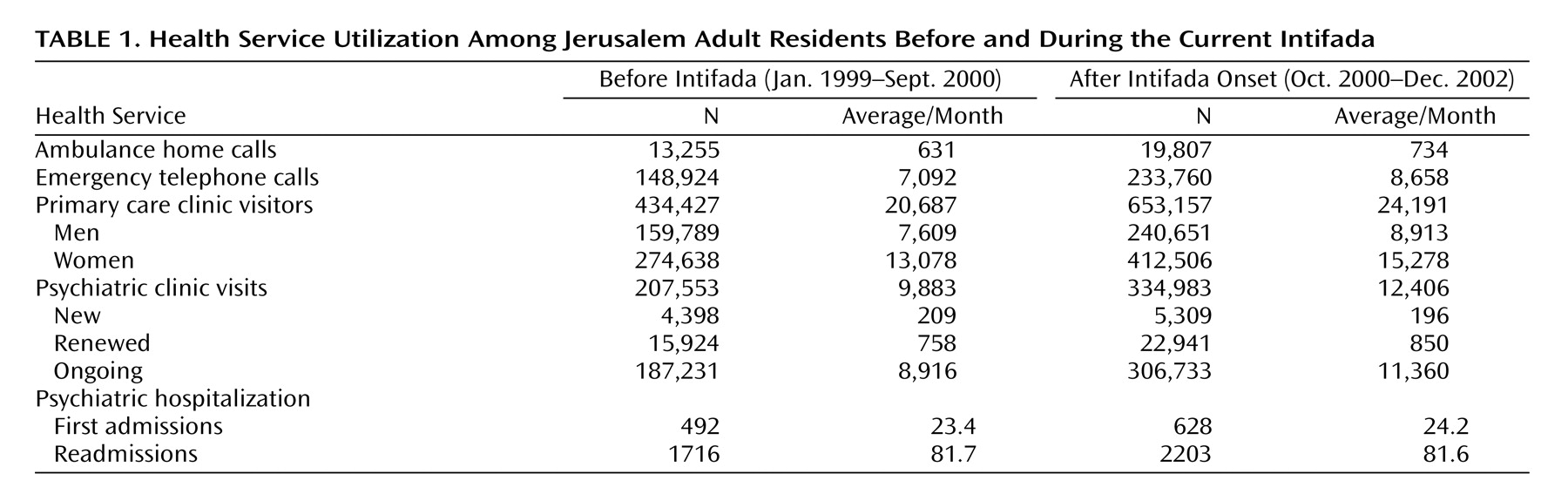
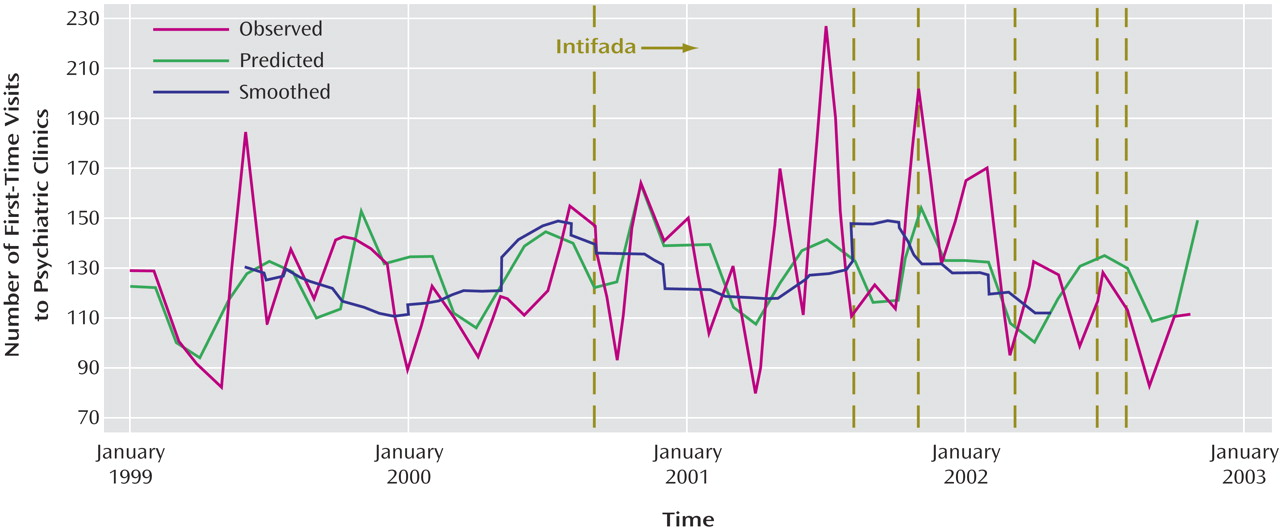
Our results show that, with few exceptions, the Jerusalem residents did not seek increased help from psychiatric services during the study period. Thus there was no increased influx of adult patients to governmental psychiatric clinics, except for elderly patients, a subgroup that may be vulnerable to terrorism-related stress due to earlier life exposure to the Holocaust and past wars
(22) . Last, the changes in the relative proportion of diagnoses over time among new patients failed to remain significant following statistical correction. These almost general negative findings are reinforced by the reduction in the long-term first psychiatric hospitalizations, or, stating it more conservatively, by the nonreversal of a negligible descending trend that characterizes first inpatient admissions in the country
(35) . The readmission of patients who had been previously hospitalized showed mixed results, a short-term increase (a possible effect of stress on this vulnerable group
[36] ) but no long-term changes, perhaps an effect of adaptation. Consistent with studies in the United States
(37) and in Israel
(6), emergency personal crisis telephone hotline service use increased. This is not surprising, since this service is easily accessible from home, it operates around the clock, it is free, and it is anonymous. It is important to note in order to better judge the results that Jerusalem did not lose more residents during the period studied compared with previous years (www.jils.org.il/shnaton), although life in the city was more dangerous.
This report has some limitations. Information was collected and recorded by agencies outside our immediate supervision, except those from the government
(35) . Also, data from the university clinic specializing in stress reactions following all types of traumatic events were not collected nor were data from private practice psychologists funded by the National Insurance Institute. Those settings, which charge a fee for their services, mostly or solely provide care for survivors of the attacks and their families as well as for bereaved families that may be referred by the National Insurance Institute rehabilitation officers upon need. Recall here that our focus was the general Jerusalem population and not persons directly involved in the attacks.
The two health insurers that provided data on visits to primary care physicians cover slightly over 40% of the Jewish city residents. We are confident, however, that the populations covered are not biased, since the insured belong to a heterogeneous population in terms of socioeconomic status, degree of religious observance, and residence, and their doctors’ clinics are spread across the city, including the neighborhoods in which the attacks occurred. Obviously, our study is neither covering later periods of the current intifada nor the time when terrorism will cease and peace and reason will prevail. Thus, we cannot claim that the mental health help-seeking pattern will remain as we found it here.
This study has several strengths. Methodologically, it relies on a composite mosaic built by using multiple sources of information that kept their system of data collection unchanged over the years under examination. Note here that, in contrast with the community surveys conducted in New York City
(32) and Israel
(6), purported to provide unbiased population rates, our data sources were not affected by the relatively low response rates obtained in those studies nor by respondent recall. With regard to the analysis, we utilized time-series analyses, controlling for long-term effects and seasonal fluctuations. Boscarino et al.
(25), who did not use time-series analysis, found a small, yet significant increase in 1-month services utilization in Manhattan after September 11, 2001, but their finding may be questioned by lower services utilization in the month of August, when many New Yorkers (including service providers) are on vacation. Rosenheck and Fontana
(31) studied six 6-month periods of services utilization and applied analysis of variance to assess the impact of the September 11 attacks in New York on Veteran Affairs mental health services utilization. Their study likely contains too few data points to distinguish between short-term and long-term effects and to ensure that identified effects (or the lack thereof) are not the result of a general trend. The importance of adjusting for a general linear trend, which reflects inherent dynamics of service utilization, is obvious since changes due to the greater use of the services by an increasingly health-educated population may be mistakenly attributed to the stress of terrorism.
The field of public mental health faces a certain paradox. Community-based surveys on terrorism highlight adverse psychopathological effects
(4,
6,
12 –16) . Yet, our data and previous service-based inquiries
(15,
23 –
27,
29) reveal a much less worrisome picture. Of late, Druss and Marcus reached a similar conclusion
(28) . We acknowledge that treatment gaps measured by true prevalence studies and services utilization rates are no novelty
(38), but under the shadow of terrorism, the treatment gap with regard to psychiatric services looms very large. Indeed, a relatively small gap would have been expected, given that the social stigma of terrorism-induced mental disorder is conceivably less than that surrounding most other disorders, and that terrorism-induced psychopathology is likely to have a relatively sudden
(19) and thus noticeable onset to the person and others compared with the insidious beginning of most mental disorders. In addition, one would expect that the public mental health information continuously available through the media during the current intifada, and the encouragement to seek consultation if needed, may have led to a lowering of the threshold for utilization of specialized services.
For the apparent paradox we offer two preliminary explanations. First, most trauma-exposed persons may consider their suffering as a normal psychological reaction and do not believe that psychiatric services are the adequate address to obtain the necessary relief. As noted, “In the aftermath of terrorist attacks, many Americans may have regarded their distress as a ‘normal’ reaction…than as a disorder needing [psychiatric] care”
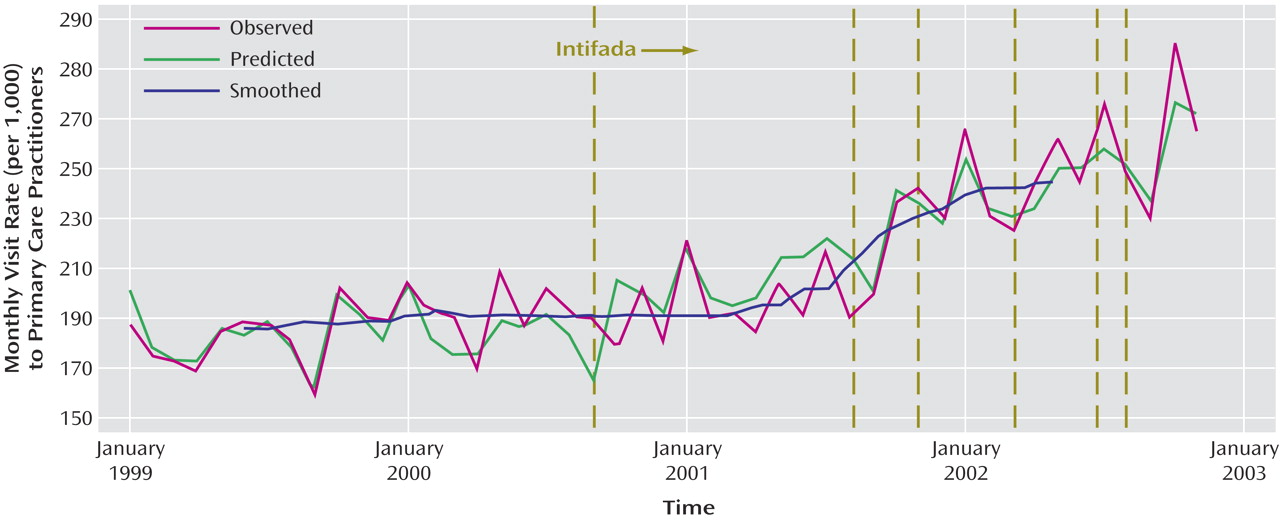
(28) . As in regular times, people that may react with varied symptoms of terrorism-induced stress seem to turn to their general practitioner for help or to other sources
(28) . To better ascertain this we would have required the general practitioner diagnoses, assuming that they were reliable, but this is not yet feasible.
Second, some epidemiological studies may overstate the extent of trauma-related psychopathology
(4,
6,
12 –16) ; up to 14.3% of those living in proximity to the World Trade Center in Manhattan surveyed in October 2001 met criteria for PTSD or depression
(32) . In contrast to these results, Northern Ireland psychiatrists stated: “because someone experiences or witnesses an act of violence does not mean that…[he or she] will inevitably develop psychiatric morbidity”
(10) .
The time may be approaching to re-evaluate psychiatric predictions of the effects of terrorism and to make better empirical attempts to explain this paradox. In particular, research is needed on determinants of help-seeking both among trauma survivors and the general population indirectly affected. The pathway from the perception of distress to the utilization of psychiatric services involves attribution of lack of normalcy to the distress and, obviously, available effective care. These perceptions need to be studied in detail. Meanwhile, access to mental health care should be facilitated by buttressing the mental health component in primary health care in emergencies, as recommended by the World Health Organization
(38,
39) and clearly showed in this inquiry. This strategy is most effective when the specialized mental health agents are community-based and collaborate with the general practitioners and nurses in dealing with the diverse trauma-related reactions, provided they avoid “medicalizing [complaints] without justification”
(40) .