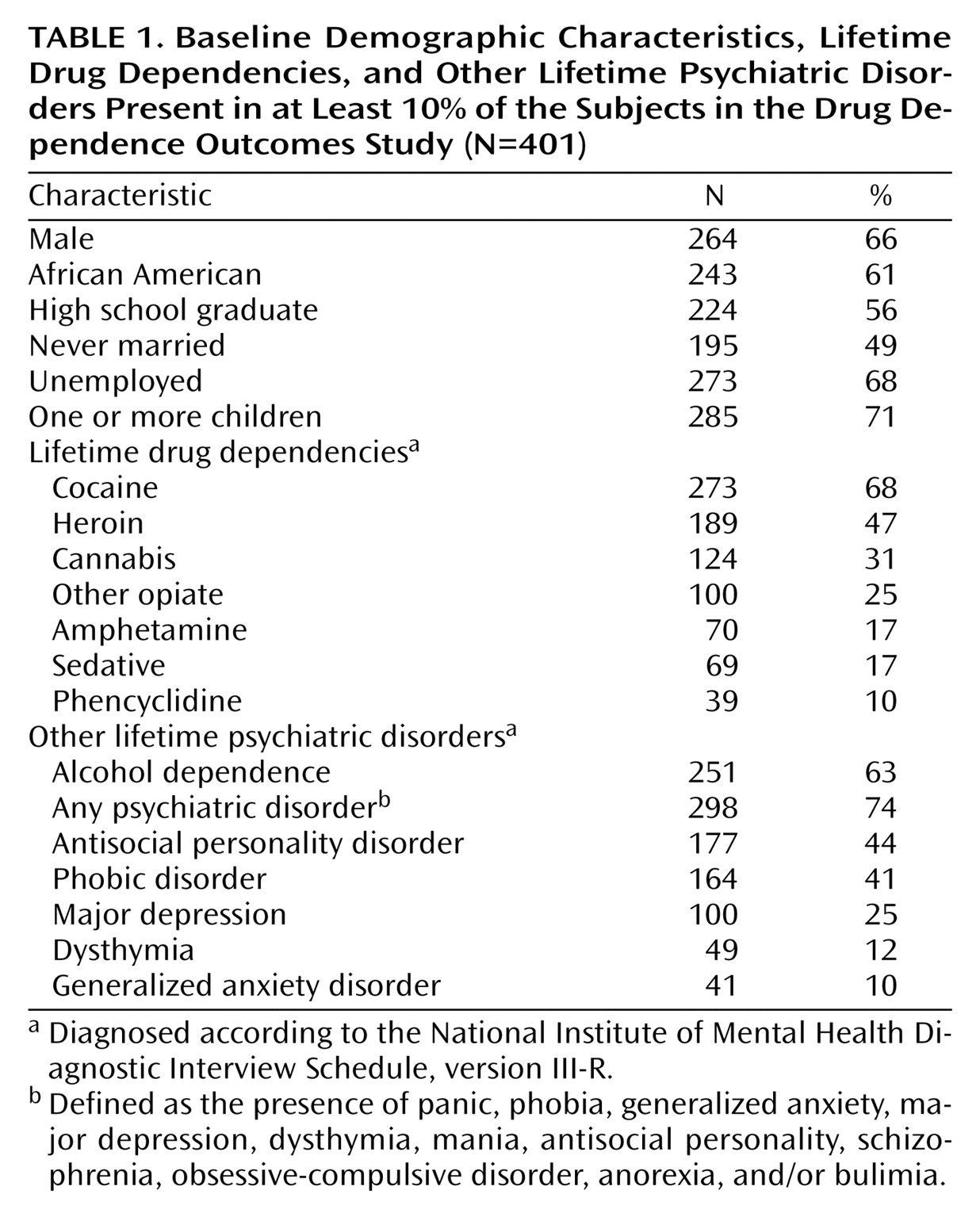
All subjects were dependent on at least one illicit substance according to sample selection criteria; however, the particular substance dependence patterns varied. The most common substance dependence was cocaine, followed by heroin, cannabis, other opiates, amphetamines, sedatives, and phencyclidine. Other illicit substances (hallucinogens and inhalants) were prevalent in less than 10% of the sample and were not considered further.
Alcohol dependence was the most common co-occurring psychiatric disorder with a prevalence of 63%. Also quite common were antisocial personality disorder, phobic disorder, major depression, dysthymia, and generalized anxiety disorder (
Table 1). Mania, schizophrenia, obsessive-compulsive disorder, anorexia, and bulimia were all prevalent in less than 10% and so were not included in predictive models. Any psychiatric disorder (defined as the presence of any comorbid condition other than alcohol dependence) was found in 74%; thus, as found by many authors, comorbidity was the rule rather than the exception.
Impact of Psychiatric Disorders on Outcomes
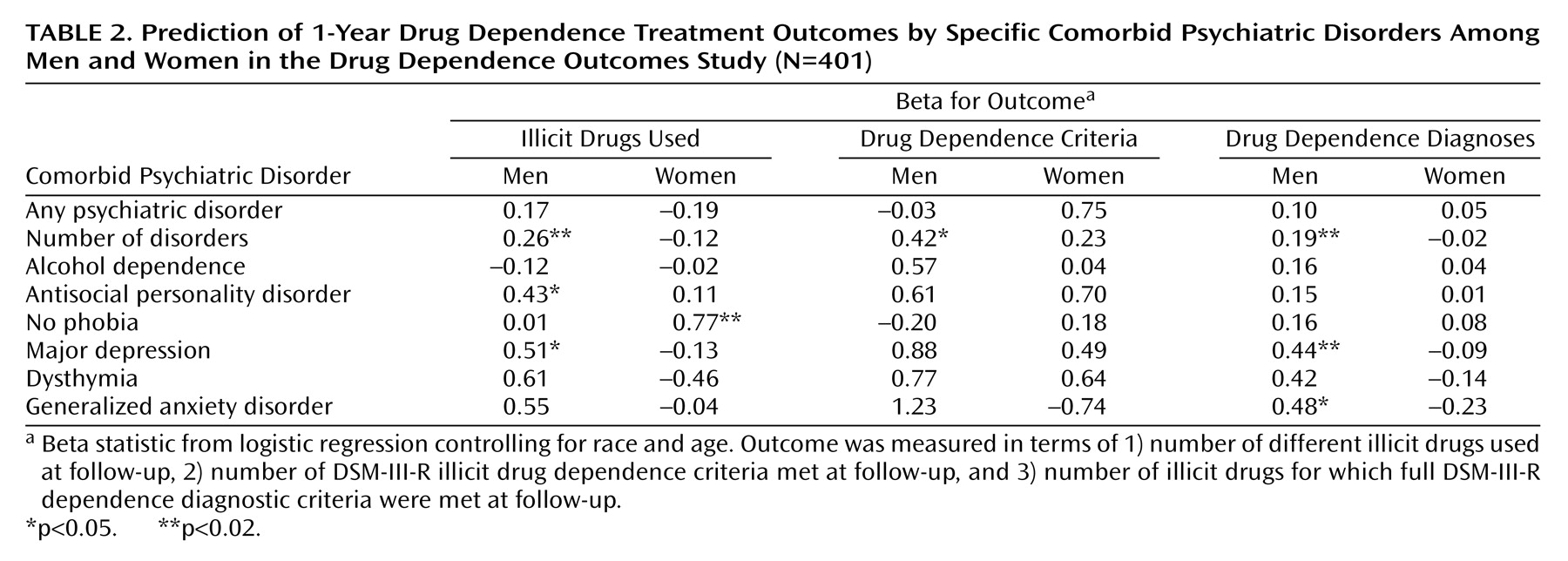
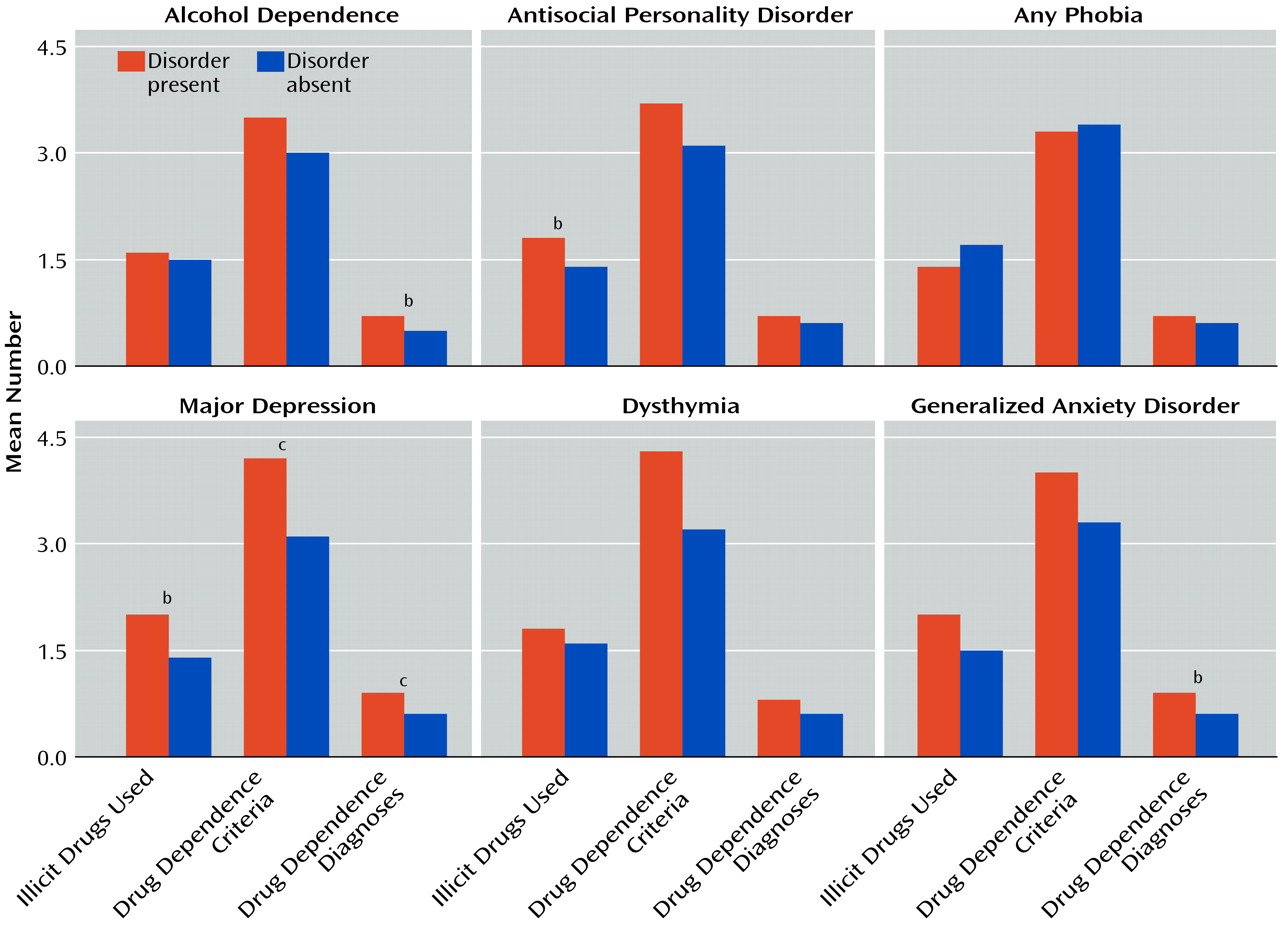
Figure 1 illustrates the impact of specific psychiatric disorders on 1-year drug treatment outcomes in patients with other lifetime psychiatric disorders in addition to lifetime drug dependence.
For subjects with alcohol dependence, the mean number of illicit drugs used, mean number of dependence criteria met for any substance, and mean number of substances for which full dependence diagnostic criteria were met at follow-up were 1.6, 3.5, and 0.7, respectively, compared with for subjects without alcohol dependence, the mean number of illicit drugs used, mean number of dependence criteria met for any substance, and mean number of substances for which full dependence diagnostic criteria were met at follow-up were 1.5, 3.0, and 0.5, respectively. The difference in number of dependence diagnoses was possibly significant at p=0.02.
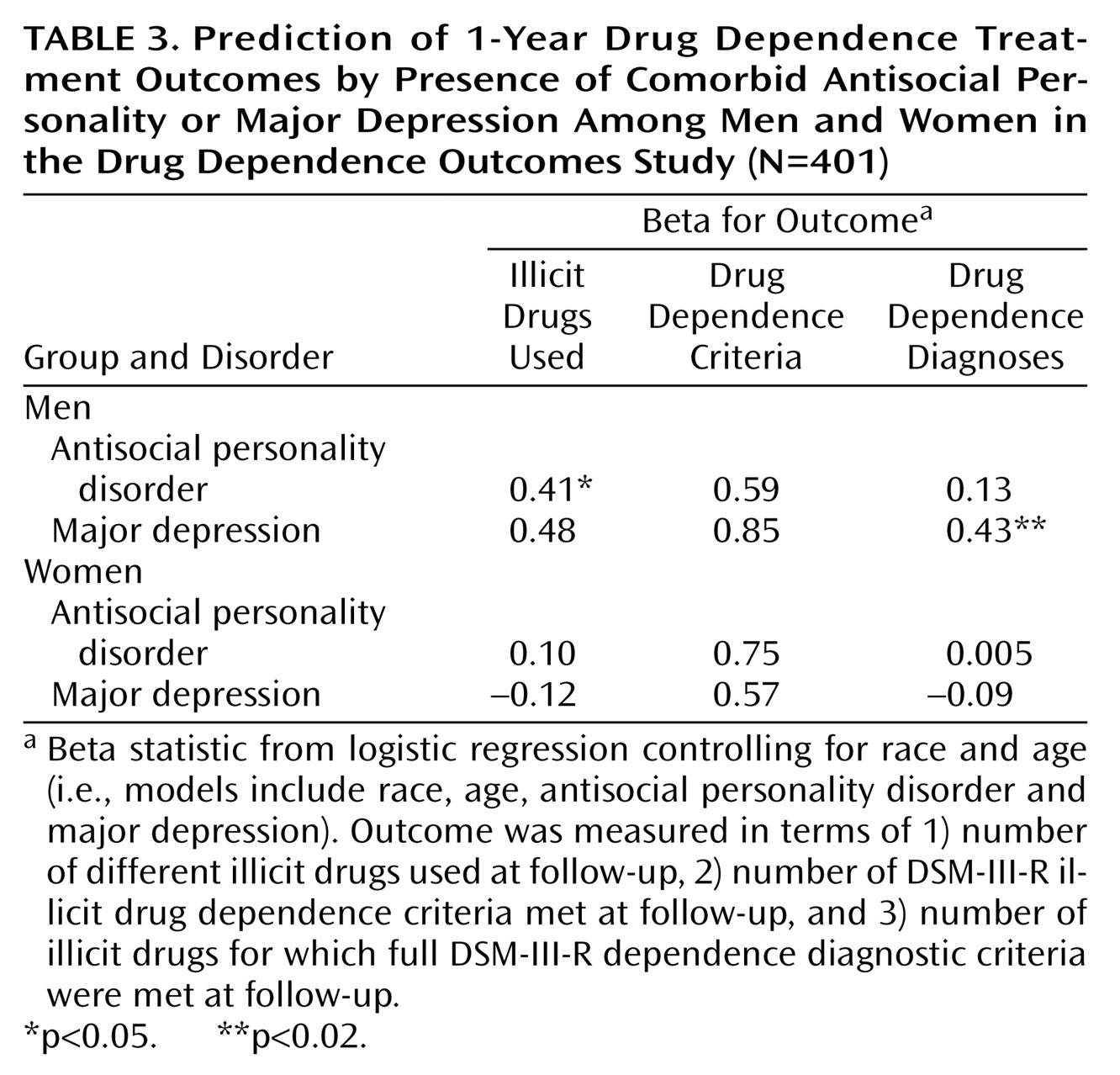
Antisocial personality disorder also influenced substance abuse outcomes in that the presence of antisocial personality disorder seemed to increase the chances of a worse outcome at 1-year follow-up. For subjects with antisocial personality disorder, the mean number of illicit drugs used, mean number of dependence criteria met for any substance, and mean number of substances for which full dependence diagnostic criteria were met at follow-up were 1.8, 3.7, and 0.7, respectively, compared with 1.4, 3.1, and 0.6, respectively, for subjects without antisocial personality disorder. The difference in number of illicit drugs used was possibly statistically significant (p=0.03). The differences in number of dependence criteria and diagnoses were not significant.
Phobias had a possible impact on substance abuse treatment outcomes in that subjects with phobias used fewer illicit substances at follow-up than subjects without phobias, but the difference was not statistically significant. For subjects with phobic disorders, the mean number of illicit drugs used, mean number of dependence criteria met for any substance, and mean number of substances for which full dependence criteria were met at 1-year follow-up were 1.4, 3.3, and 0.7, respectively, compared with 1.7, 3.4, and 0.6, respectively, for subjects without phobic disorders.
Major depression had the most consistent impact on substance outcomes at 1-year follow-up. For subjects with major depression, the mean number of illicit drugs used, mean number of dependence criteria met for any substance, and mean number of substances for which full dependence diagnostic criteria were met at 1-year follow-up were 2.0, 4.2, and 0.9, respectively, compared with 1.4, 3.1, and 0.6, respectively, for subjects without major depression. The differences were statistically significant or possibly significant for all three outcomes: illicit drugs used (p=0.02), dependence criteria endorsed (p=0.01), and dependence diagnoses met (p=0.006).
Dysthymia had a minimal association with outcomes at 1-year follow-up. For subjects with dysthymia, the mean number of illicit drugs used, mean number of dependence criteria met for any substance, and mean number of substances for which full dependence diagnostic criteria were met at 1-year follow-up were 1.8, 4.3, and 0.8, respectively, compared with 1.6, 3.2, and 0.6, respectively, for subjects without dysthymia. None of the differences were statistically significant.
Similarly, generalized anxiety disorder had an association with a worse substance abuse treatment outcome at 1-year follow-up. For subjects with generalized anxiety disorder, the mean number of illicit drugs used, mean number of dependence criteria met for any substance, and mean number of substances for which full dependence diagnostic criteria were met at 1-year follow-up were 2.0, 4.0, and 0.9, respectively, compared with 1.5, 3.3, and 0.6, respectively, for subjects without generalized anxiety disorder. The difference in the number of dependence diagnoses was possibly statistically significant (p=0.04).