Dissociative Flashbacks After Right Frontal Injury in a Vietnam Veteran With Combat-Related Posttraumatic Stress Disorder
Abstract
CASE REPORT
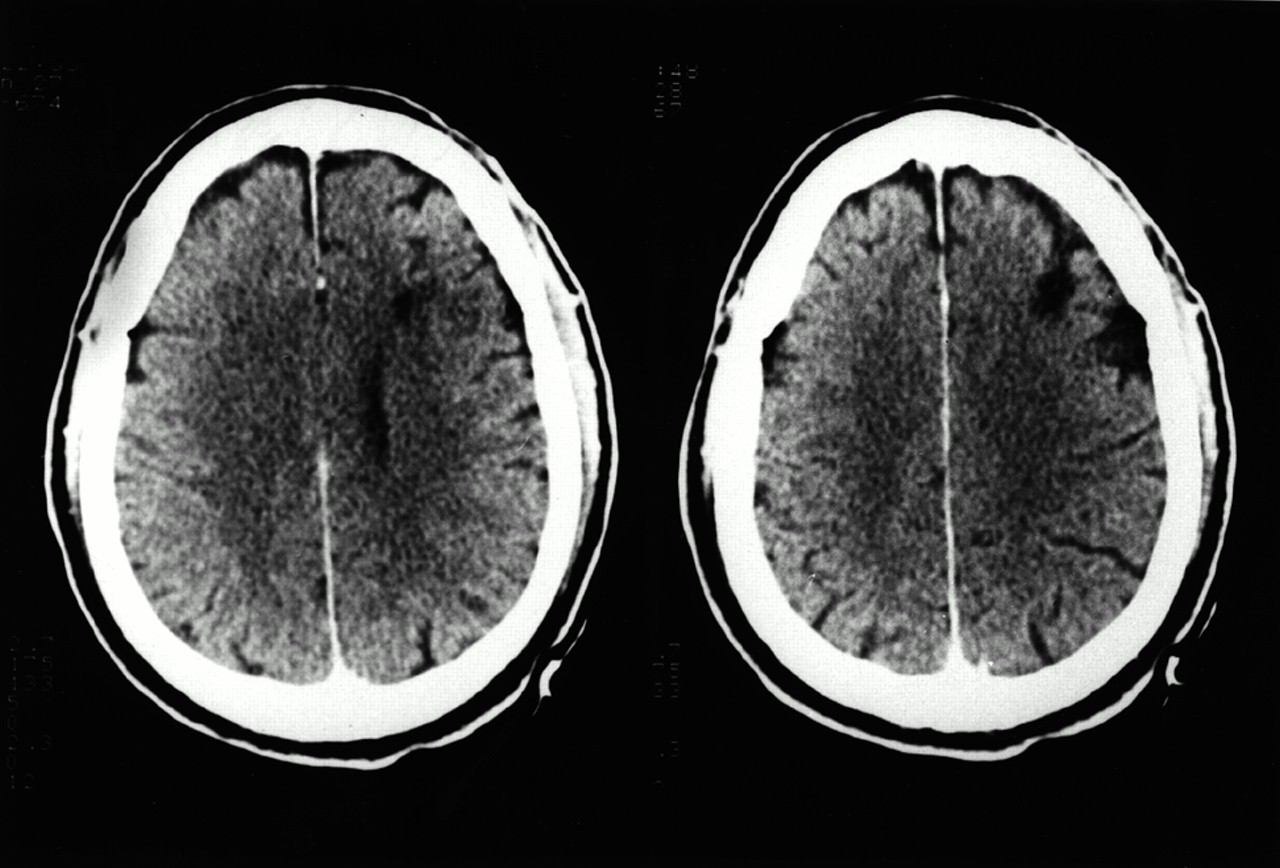
C.G., a 49-year-old Vietnam War veteran (a professional soldier from the United Kingdom who served with the allied forces), was admitted to the emergency room with excruciating right orbital headache, chest discomfort, and recurrent episodes of “confusion related to war experiences.” Nine months before admission, he had been hit by a car while walking and sustained a closed head trauma with a right frontal scalp laceration. Clinical records from another hospital revealed that C.G. had had a transient loss of consciousness and a posttraumatic amnesia of about 30 hours. His past medical history was also remarkable for a myocardial infarction 7 years before the TBI, angina, peripheral vascular disease, and a transient ischemic attack causing a left hemiparesis (a CT scan was negative). In addition, C.G. described a number of life-threatening experiences during his years in Vietnam, but the most stressful incident was the death of his Vietnamese partner and their young daughter, who were killed, together with other people, during an attack by the enemy on a refugee village. In this incident, C.G. was captured and subjected to torture and interrogations under the effects of a mind-altering drug (scopolamine) over a 1-week period.After the traumatic incident, C.G. met only the DSM-IV18 criterion “A” for PTSD (exposure to a severe traumatic event), and although he has intermittently had overt symptoms of PTSD (reexperiencing the trauma on exposure to external cues related to the war experience, dreams reminiscent of the trauma, outbursts of anger), he did not show the other behavioral symptoms (avoidance, numbing, exaggerated startle response) necessary to fulfill the diagnostic DSM-IV criteria for PTSD. In particular, he never experienced dissociative flashback phenomena before the TBI. Despite the disastrous outcome of the village attack, C.G. said: “There were no things to try to remove because I didn't remember it before the accident [TBI].”His medical and psychiatric problems led to his early retirement to a rural area in Málaga, Spain. There he met his current wife, and both now devoted much time to the breeding of horses. He also served his community as a volunteer in an organization serving the mentally handicapped. His wife indicated that he had abused alcohol to control anxiety symptoms and maladaptive personality changes (suspiciousness, restricted range of emotional expression, need for admiration), but he never sought psychiatric treatment before suffering the TBI.During the current hospitalization, C.G presented several flashback episodes that were witnessed by the attending nurse and neurology staff. The content of the dissociative flashbacks was extremely realistic and clearly reproduced the index incident that C.G. had lived while he was in Vietnam. He apparently experienced frightening visual and auditory hallucinations, describing the attack on the refugee village in great detail. During the dissociative episodes, he acted as if he were back in Vietnam, and on one occasion he even wrote: “I can't go into great detail for ‘security reasons.’ I saw men burnt alive in a vehicle and a whole village (mainly children and old people) killed with gas. I was caught and tortured…but escaped…. The bastards!!!”Also, he automatically drew several badly decipherable symbols and wrote words with high negative emotional salience (e.g., “napalm gas”), as shown in Figure 1. The flashbacks lasted several minutes, occurred two or three times a day, and were accompanied by hypervigilance, agitation, confusion, and somatic symptoms of anxiety. Between episodes, C.G. could not recall the details of the dissociation phenomena, but his thoughts were well organized and there was no evidence of illogical thinking or loosening of associations. Neurological examination was always normal. His score on the Mini-Mental State Examination19 was within normal limits (28/30). The Impact of Event Scale (IES)20 was used to measure intrusive thoughts and avoidance behavior associated with either the TBI or the war incident (the refugee village attack). He obtained high scores on the IES; for the TBI incident his total IES score was 44 (intrusion subset score=29; avoidance subset score=15), whereas for the war incident his total IES score was 51 (intrusion subset score=33; avoidance subset score=18).Although he had posttraumatic amnesia, not recalling anything about the circumstances of the accident, it is possible that he learned details of the traumatic event through information verbally mediated by witnesses and family members.21 He had intrusive thoughts and images of the street where he was run over by the car, he avoided talking about the accident, and he commented that his facial scars were continuous reminders of the injury. On the Hamilton Rating Scale for Depression,22 his score was 13 points. He was also administered the Structured Clinical Interview for DSM-III-R Personality Disorders (SCID-II23) and was found to meet criteria for paranoid, schizoid, and narcissistic personality disorders. While an inpatient, C.G. was treated with carbamazepine (800 mg/day) and the dissociative flashbacks remitted after a few days.Serial EEGs carried out between dissociative episodes were always normal. A CT scan of the brain (Figure 2) showed a low-density lesion in the right dorsolateral frontal lobe (Brodmann area 6). Regional cerebral blood flow (rCBF) was studied in C.G., when he was free of medication and between dissociative episodes, with [99mTc]HMPAO and SPECT, using an Elscint Apex 609 RG gamma camera. Focal blood flows were analyzed semiquantitatively in regions of interest (ROIs; circular, 4×4 pixels), which were placed in cortical and subcortical regions of seven successive transaxial slices.24 The total number of ROIs was combined to create eight cortical areas: inferior frontal cortex, superior frontal cortex, anterior temporal cortex, mesial temporal cortex, posterior temporal cortex, anterior cingulate, parietal cortex, and occipital cortex. Additional ROIs were placed in the cerebellum, thalamus, and basal ganglia (caudate nucleus). An rCBF was calculated for each ROI as the average activity in the region divided by the activity in the cerebellum (region [right−left] average/cerebellum).25 According to our own previous data from normal subjects (mean ratio: 1.00±0.03), ratios below 0.93 were considered abnormal.24The most marked rCBF decreases were seen in the anterior temporal cortex (0.78) and superior frontal cortex (0.78). Less robust decrements (but always 2 SD below the mean of normal control subjects) were seen in the inferior frontal cortex (0.91), parietal cortex (0.91), and posterior temporal cortex (0.92). Decrements were always more prominent in the right than the left hemisphere. On the other hand, rCBF increases were seen in anterior cingulate (1.13), caudate nucleus (1.14), and thalamus (1.10). No relevant changes were seen in the mesial temporal (amygdala) and occipital cortices.
DISCUSSION
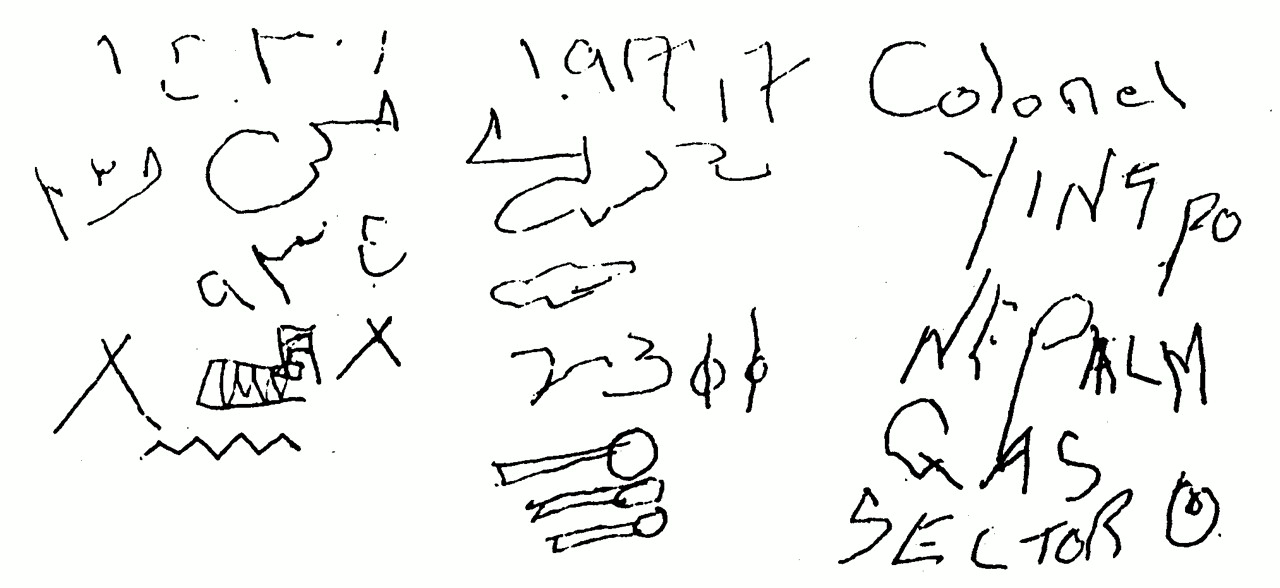
References
Information & Authors
Information
Published In
History
Authors
Metrics & Citations
Metrics
Citations
Export Citations
If you have the appropriate software installed, you can download article citation data to the citation manager of your choice. Simply select your manager software from the list below and click Download.
For more information or tips please see 'Downloading to a citation manager' in the Help menu.
There are no citations for this item
View Options
View options
PDF/ePub
View PDF/ePubGet Access
Login options
Already a subscriber? Access your subscription through your login credentials or your institution for full access to this article.
Personal login Institutional Login Open Athens loginNot a subscriber?
PsychiatryOnline subscription options offer access to the DSM-5-TR® library, books, journals, CME, and patient resources. This all-in-one virtual library provides psychiatrists and mental health professionals with key resources for diagnosis, treatment, research, and professional development.
Need more help? PsychiatryOnline Customer Service may be reached by emailing [email protected] or by calling 800-368-5777 (in the U.S.) or 703-907-7322 (outside the U.S.).

