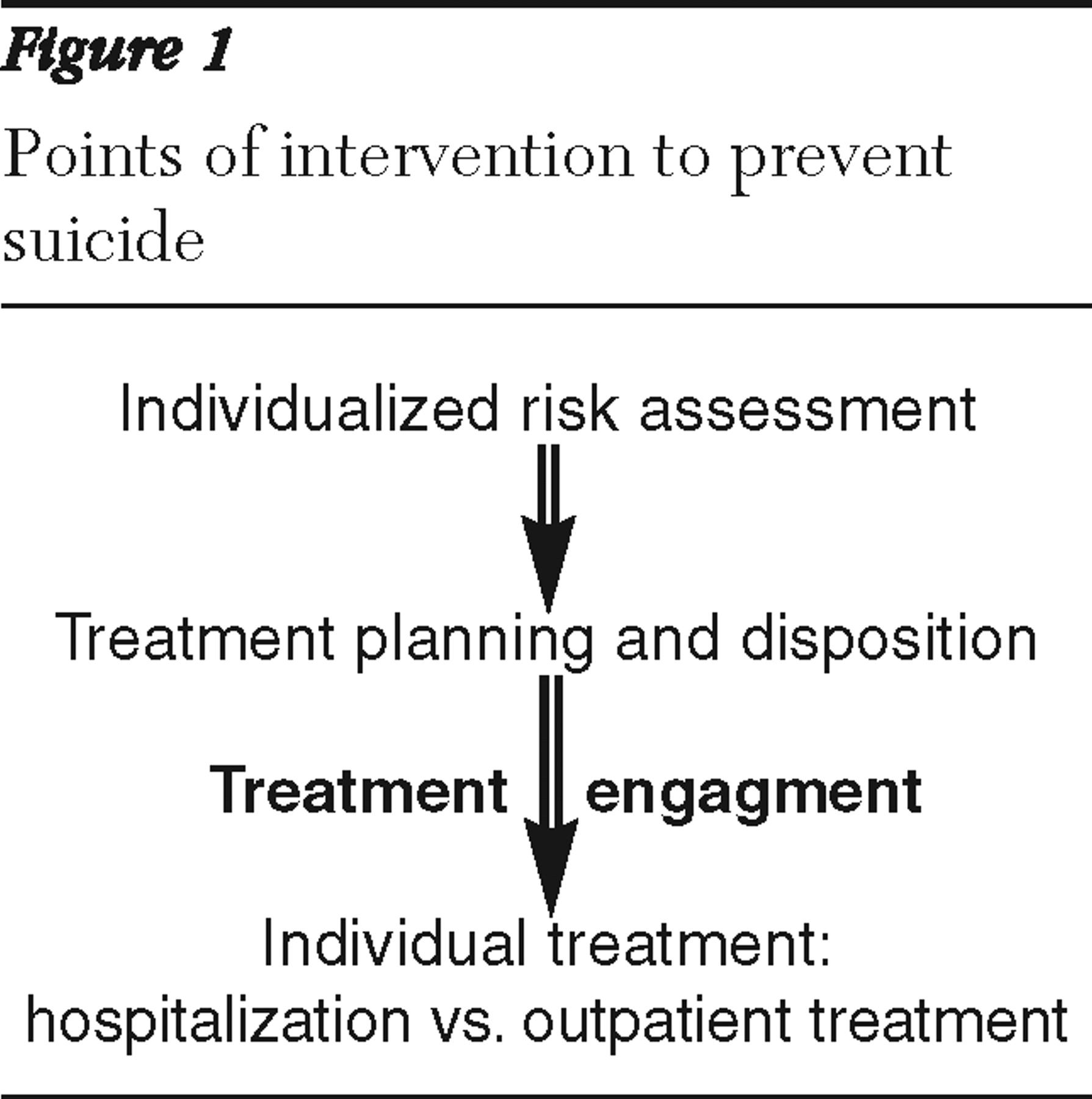
What is treatment engagement?
No universal definition of treatment engagement is used consistently across studies. However, we propose that the term refers to being committed to the therapeutic process and being an active participant in a collaborative relationship with a therapist to work to improve one's condition.
Studies examining engagement in psychiatric treatment typically operationalize engagement in one of two ways: first, whether or not the patient attended his or her first scheduled outpatient appointment, and second, the total number of sessions attended by the patient (
2,
3,
4,
5,
6,
7 ).
Thirteen studies focusing on brief interventions targeting suicide attempters were identified in this review. Seven of the studies focused on interventions specifically designed to enhance treatment engagement of suicidal adults and adolescents, and the other six focused on reducing risk of repeat suicidal behavior, with implications for engaging suicide attempters in treatment.
Interventions designed to improve continuity of care
In an effort to enhance treatment attendance, three studies have explored interventions aimed at improving treatment engagement of suicidal adults (
2,
3,
4 ). Cedereke and colleagues (
4 ) examined whether follow-up telephone contact with patients after their discharge from the emergency department had an effect on rates of treatment adherence. The intervention consisted of follow-up telephone calls four months and eight months after discharge from the emergency department. During the calls, semistructured interviews were conducted to assess the individual's suicidal behavior, psychosocial functioning, physical health, and level of satisfaction with treatment received. Patients who were in treatment were encouraged to continue attending treatment, and patients who had not attended or had dropped out of treatment were encouraged to attend treatment. When necessary, interviewers provided advice and assisted patients in seeking treatment. The goal of the phone contact was to increase and maintain treatment engagement throughout the follow-up period, thus reducing suicidal behavior. The intervention was not found to be effective, suggesting, perhaps, that contact needs to be initiated immediately on presentation to the emergency department or that the level of contact was not sufficient.
Van Heeringen and colleagues (
2 ) tested the effectiveness of sending a visiting nurse to former patients' homes as a means of improving treatment adherence within a one-year period. After discharge from the emergency department, patients who were nonadherent with treatment received home visits from a community nurse, who assessed reasons for nonadherence and specific treatment needs. A significant improvement in adherence was found among the nonadherent patients in the intervention group once they received home visits. It is unclear which components of the home visit were effective because the study did not use standardized procedures for the visits, and data regarding the process of the visits were not gathered. Although the specific factors of the intervention that led to improvement in treatment adherence could not be identified, it seems likely that problem solving with regard to obstacles to treatment adherence may have been helpful in increasing treatment attendance. In addition, because of its burdensome nature—in terms of the economic and time commitments required—this intervention may not be practical and could not easily be incorporated into standard treatment procedures.
Spooren and colleagues (
3 ) attempted to improve treatment engagement by providing a comprehensive referral, with a fixed appointment and a flexible treatment approach. Treatment could include family involvement, meeting with the outpatient treatment provider, incorporating the patient's perspective, and motivating the patient to attend treatment. Results showed that adherence rates were significantly higher in the intervention group than in the control group. However, the results held only for the two hospitals in which most of the aftercare referrals were made within the institution. Thus the results suggest that initial reaching out to patients must be followed with relatively easy access to outpatient treatment.
Four studies focused on treatment engagement of suicidal adolescents (
5,
6,
7,
8 ). Zimmerman and colleagues (
7 ) examined the effectiveness of a contact intervention that consisted of a two-hour multifamily orientation group before intake at an outpatient clinic. The group provided an overview of the clinic and evaluation processes, psychoeducation regarding suicidality, and alternate adaptive behaviors. The goal of the intervention was to improve treatment adherence by reducing the period between initial telephone contact with the clinic and the first clinic appointment. Adherence was measured both by attendance at the initial clinic appointment and by continuation in treatment beyond two appointments. Those in the orientation group had a significantly better attendance rate than others who had received usual treatment at the first clinic appointment, but the intervention did not have an impact on treatment adherence beyond the first appointment.
Rotherham-Borus and colleagues (
9 ) tested the effectiveness of a contact intervention designed to address structural factors believed to impede treatment adherence, such as negative attitudes, expectations, and behaviors of both emergency department staff and adolescent suicide attempters. The intervention comprised three components: staff training workshops, a video that was shown to attempters and their families and aimed at improving the understanding of adolescent suicide and outpatient treatment, and a brief family session held in the emergency department. After emergency department treatment, all attempters were referred to a specialized outpatient clinic, where they received a six-week treatment program designed for the study. Three levels of treatment adherence were assessed: adherence to one session, completion of the six-week program, and the total number of sessions attended. Adolescents in the specialized emergency department program were significantly more likely than those receiving treatment as usual to attend any treatment postdischarge from the emergency department. However, the program led to only a marginally significant increase in the total number of sessions attended and the likelihood of completing the six-week treatment program.
Donaldson and colleagues (
5 ) examined the effectiveness of an intervention involving a verbal contract to attend treatment, which was followed up with phone contact. The intervention focused on psychoeducation regarding outpatient treatment (including a review of expectations for treatment and resistance to treatment) and a verbal contract to attend at least four psychoeducation sessions. Over a period of eight weeks postdischarge, patients received three structured telephone contacts that used a problem-solving approach targeting suicidal ideation and adherence to treatment. Results indicated that although there was a trend toward differences between the two groups in rates of adherence, the differences were not significant.
In an attempt to address patients' low engagement with aftercare treatment after first-time episodes of nonfatal deliberate self-harm, Spirito and colleagues (
8 ) offered the patients rapid, easy access to on-call trainee psychiatrists in the event of further difficulties. Patients were also encouraged to seek help at an early stage should such problems arise. The follow-up data obtained after one year showed a significant reduction of actual or seriously threatened deliberate self-harm in the experimental group, who also utilized fewer general medical and psychiatric services compared with a control group.
These studies reinforce the importance of follow-up contact and suggest that the level of contact has to be substantial to be effective. They also highlight the value of immediate contact postdischarge from the index hospitalization as well as the need for a comprehensive, multifaceted intervention. In addition, the findings demonstrate how little is actually known about what factors improve treatment engagement.
Brief interventions to reduce suicidal behavior
Although very brief interventions designed to reduce suicidal behavior are appealing because of their simplicity and cost-effectiveness, their efficacy has been limited. To date, none of these tested interventions have been administered in an emergency setting. All have occurred postdischarge. Carter and colleagues (
10 ), Motto and Bostrom (
11 ), and Morgan and colleagues (
12 ) examined the effectiveness of written communication (a postcard, a shot letter, and a card with the phone number of a 24-hour hotline, respectively) on reducing future suicidality. Vaiva and colleagues (
13 ) and Fleischmann and colleagues (
14 ) tested the effectiveness of phone contact on reducing risk of suicide. Greenfield and colleagues (
15 ) examined the effect of rapid follow-up on reducing rehospitalization rates and levels of suicidality of suicidal adolescents.
Morgan and colleagues (
12 ) assessed patients who presented to the emergency department for a first episode of nonfatal deliberate self-harm, defined as suicidal and nonsuicidal self-injurious behavior. In an effort to decrease the rate of repetition of deliberate self-harm, the investigators randomly assigned patients to receive either standard emergency department care or an intervention consisting of a green index card that provided a number for rapid, easy access to on-call psychiatry trainees and encouragement to seek help should they begin to experience difficulties again in the future. Patients in the intervention group received the green card in the emergency department before discharge and were then mailed an additional copy of the card to their homes three weeks later. General practitioners were also sent copies of the green card and were encouraged to remind their patients about it as needed. Intervention and control group patients were compared on number of inpatient days, day-treatment days, community nurse visits, and kept outpatient appointments over a one-year period. Results indicated that although patients in the intervention group harmed themselves less frequently than those in the control group, the reduction was not statistically significant.
Motto and Bostrom (
11 ) explored a long-term contact intervention that consisted of written communication with suicidal patients. The investigators hypothesized that reducing demands placed on patients (by approaching them rather than expecting them to seek out services) and reducing their sense of isolation would decrease future suicidality. One month postdischarge from the emergency department, patients were contacted to determine whether they had accepted and adhered to their postdischarge treatment plan for that 30-day period. The contacts were primarily intended to show concern for patients and their well-being. Those who were in treatment were designated as the treatment group. Those who were not in treatment were then randomly assigned to either the intervention group, in which they received periodic contact in the form of a letter (24 letters over five years), or the control group, which received no further contact. Results indicate that although the intervention was initially successful at reducing suicidality, as the frequency of the contact was reduced its protective influence ceased.
Greenfield and colleagues (
15 ) examined suicidal adolescents presenting to the emergency department of a pediatric hospital. Patients were assigned to either rapid-response outpatient follow-up (the experimental group) or to a control group that involved a ten-day wait for outpatient follow-up postdischarge from the emergency department. At the six-month follow-up assessment, no between-group differences were observed in changes in levels of suicidality or in overall functioning over the follow-up period. Overall, suicidal adolescents who received rapid-response outpatient follow-up had a lower hospitalization rate than those who did not. The two groups achieved similar increases in levels of functioning and decreased levels of suicidality, suggesting that suicidal adolescents can be treated within a rapid-response outpatient model and thus avoid hospitalization.
Carter and colleagues (
10,
16 ) sent one postcard a month for the first four months postdischarge from the emergency department for self-poisoning and then one postcard every two months for the next eight months (for a total of eight postcards over one year). The postcard consisted of two sentences, the first expressing hope that the patient was doing well and the second indicating that if the patient wished to make contact, it would be welcomed. The intervention reduced repetitions of deliberate self-harm, although it did not significantly reduce the proportion of individual repeaters.
Vaiva and colleagues (
13 ) tested the effectiveness of phone contact on reducing repeat attempts. The intervention consisted of one phone call at either one month or three months postdischarge from the emergency department. The goal of the telephone call was to review the reasons that outpatient treatment had been advised and to provide support, advice, and, if necessary, crisis intervention. Individuals contacted one month after their discharge from the emergency department experienced a significantly lower rate of repeat attempts than a control group that received no contact. Those contacted at three months postdischarge from the emergency department did not differ on rate of repeat attempts from those who did not receive contact.
Fleischmann and colleagues (
14 ) conducted a one-hour informational session in the emergency department before the patient was discharged. The session covered correlates of suicidal behavior and alternative coping measures. Nine follow-up phone calls or visits were conducted over the 18 months postdischarge. Compared with treatment as usual, the intervention was found to significantly reduce the rate of completed suicides over the course of the 18-month follow-up period. However, the study did not report on the effectiveness of the intervention at reducing the number of repeat suicide attempts that did not result in death.
Although some positive findings are reported in these studies, none of these interventions was effective in reducing the number of repeat attempters over the long term. Although such interventions are attractive because of their cost-effectiveness and transportability, their limited efficacy is not surprising given the extent and severity of suicide attempters' problems. Treatment engagement was not tested in these studies. It is possible that these interventions might not be effective in reducing suicidal behavior in the long term but may be helpful in encouraging patients to seek and remain in treatment. They should be explored further for their effectiveness as contact interventions focused on improving treatment engagement.