Controlled clinical trials have demonstrated that specific pharmacological and behavioral treatments can reduce the symptoms and impairment associated with attention deficit hyperactivity disorder (ADHD)
(1–
5). Treatment with stimulants results in a rapid improvement in the conduct, attentiveness, and academic performance of children and adolescents with ADHD
(1). Approximately 70% of the patients with ADHD respond to treatment with stimulant medications in the short term
(2) and over periods of up to 18 months
(3,
4). Behavioral approaches involving teachers
(5,
6), parents
(5), and contingency management programs
(7) are also established treatments for children with ADHD. For some patients, medications in combination with behavioral psychosocial interventions may be more effective than either treatment alone. In the National Institute of Mental Health (NIMH) Multimodal Treatment Study of ADHD, for example, patients who received the combined treatment significantly improved in more areas than those who received either medication management or behavioral treatment alone
(8).
The proportion of children with ADHD who receive any treatment for their symptoms probably varies from community to community
(9,
10). In the NIMH Methods for the Epidemiology of Child and Adolescent Mental Disorders Study
(11), only 12.5% of the children (9 to 17 years) with ADHD had been given stimulants during the previous year (1992). In the Great Smoky Mountain Study
(12), most children ages 9, 11, or 13 who met full ADHD criteria (62%) reported stimulant use in the preceding 3 months (1993). Within a well-diagnosed multisite clinical trial sample (3), 68% of the children received some medication treatment for ADHD over 14 months.
Several lines of evidence suggest that there has been a recent national increase in the treatment of ADHD. Bulk production of methylphenidate
(13), pharmacy-based audits
(14), and physician-based surveys
(15,
16) have revealed increasing consumption of stimulants. A survey of Baltimore County public schoolchildren
(17) and statewide analyses of Medicaid data further suggest that treatment of ADHD has increased
(18,
19). However, few previous studies have examined the overall pattern of ADHD treatments, including psychological treatments, from a population perspective
(20).
In the current study, we examined recent national trends in the treatment of ADHD. The analysis extended to pharmacological and psychological treatments, all types of health care professionals, and outpatient settings. We present national estimates of trends in the treatment of ADHD and identify segments of the population that have been most affected by these trends. Given recent changes in the health care system
(21) and apparent increasing use of medication treatments for ADHD, we also examined whether there have been accompanying changes in the use of psychotherapy to treat childhood ADHD.
Method
Data were drawn from the household section of the 1987 National Medical Expenditure Survey and the 1997 Medical Expenditure Panel Survey. Both surveys were organized by the Agency for Healthcare Research and Quality, the health services research arm of the U.S. Department of Health and Human Services. The surveys provided estimates for the use, expenditures, and financing of health services based upon national probability samples of the U.S. civilian, noninstitutionalized population.
The 1987 National Medical Expenditure Survey used a sampling design in which 15,590 households were selected from within 165 geographic regions across the United States. A sample of 34,459 individuals was included in the study, representing a response rate of 80.1%. The 1997 Medical Expenditure Panel Survey household component was drawn from a nationally representative subsample of the 1995 National Health Interview Survey that used a sampling design similar to that of the 1987 National Medical Expenditure Survey. There were 32,636 participants interviewed from 14,147 households, representing a 74.1% response rate. For both surveys, a designated informant was queried about all related persons who lived in the household.
The Agency for Healthcare Research and Quality devised weights to adjust for the complex survey design and yield unbiased estimates. Sampling weights also adjusted for survey nonresponse and poststratification to population totals based on U.S. census data. More complete discussions of the design, sampling, and adjustment methods are presented elsewhere
(22–
24). Percentages were corrected to provide approximately unbiased national estimates. Significance tests were carried out by using the SUDAAN software package to account for the complex survey design
(25).
Structure of the Surveys
Households selected for the National Medical Expenditure Survey household survey were interviewed four times to obtain health care use information for the 1987 calendar year. The Medical Expenditure Panel Survey included a series of three in-person interviews for 1997. In both surveys, respondents were asked to record medical events as they occurred in a calendar/diary that was reviewed in person during each interview. Written informed consent was obtained from selected survey participants to contact medical providers mentioned during the interviews to verify service use, charges, and sources and amounts of payments.
Income
Respondents were grouped on the basis of total family income in relation to the Bureau of Census poverty line as poor (<100%), near poor (100%–<125%), low income (125%–<200%), middle income (200%–<400%), or high income (≥400%) (23, 24).
Treatment of ADHD
Respondents were asked the primary reason for every outpatient visit and every purchase of medication. Entries were coded according to the revised ICD-9 for the National Health Interview Survey. Interviewers each underwent 80 hours of training, and coders all had degrees in nursing or medical records administration. A total of 5% of the records were rechecked for errors; error rates in these rechecks were less than 2.5%. A staff psychiatric nurse established mental disorder diagnoses in cases of diagnostic ambiguity or uncertainty. Respondents who reported one or more visits for the primary purpose of treating patients with ICD-9 code 314 (hyperkinetic syndrome of childhood) or purchased or otherwise obtained a psychotropic medication for patients with this condition were defined as having received treatment for ADHD.
Providers
The Medical Expenditure Panel Survey and National Medical Expenditure Survey booklets include detailed questions on the health care professionals associated with each health care visit. We considered physicians of all specialties, social workers, psychologists, and a residual group of other providers that included nurses, nurse practitioners, physician’s assistants, chiropractors, and other health care providers. Respondents who made one or more visits during the survey year to a provider group for the primary purpose of treating ADHD were defined as having received treatment from that provider group.
Psychotherapy
The National Medical Expenditure Survey and the Medical Expenditure Panel Survey asked respondents about the type of care provided during each outpatient visit using a flash card containing various response categories. Visits that included psychotherapy or mental health counseling for the primary purpose of treating ADHD were considered “psychotherapy” visits. All other ambulatory visits for the primary purpose of treating ADHD were considered nonpsychotherapy visits. The Medical Expenditure Panel Survey included a section on special education and related services.
Medications
The National Medical Expenditure Survey and the Medical Expenditure Panel Survey ask for the conditions associated with each prescribed medicine bought or otherwise obtained. We focused on prescribed medications associated with the treatment of ADHD. Psychotropic medications were classified as stimulants, antidepressants, clonidine, and other psychotropic medications, including antipsychotics, mood stabilizers, anxiolytics, and hypnotics
(26).
Analysis Plan
We began by examining secular changes in the background sociodemographic, health status, and health service use characteristics of children ages 3 to 18 years. We then determined trends in ADHD treatment rates per 100 children within these strata. The chi-square test was used to examine the strength of associations between rates of treatment of ADHD within sociodemographic strata and across survey years.
To adjust for secular changes in patient characteristics, we combined the 1987 and 1997 surveys and used multiple linear regression to evaluate associations between survey years and number of treatment visits, psychotherapy visits, and stimulant prescriptions, controlling for demographic variables that differed at p<0.10 between those receiving ADHD treatment in 1987 and 1997.
Results
Background Characteristics
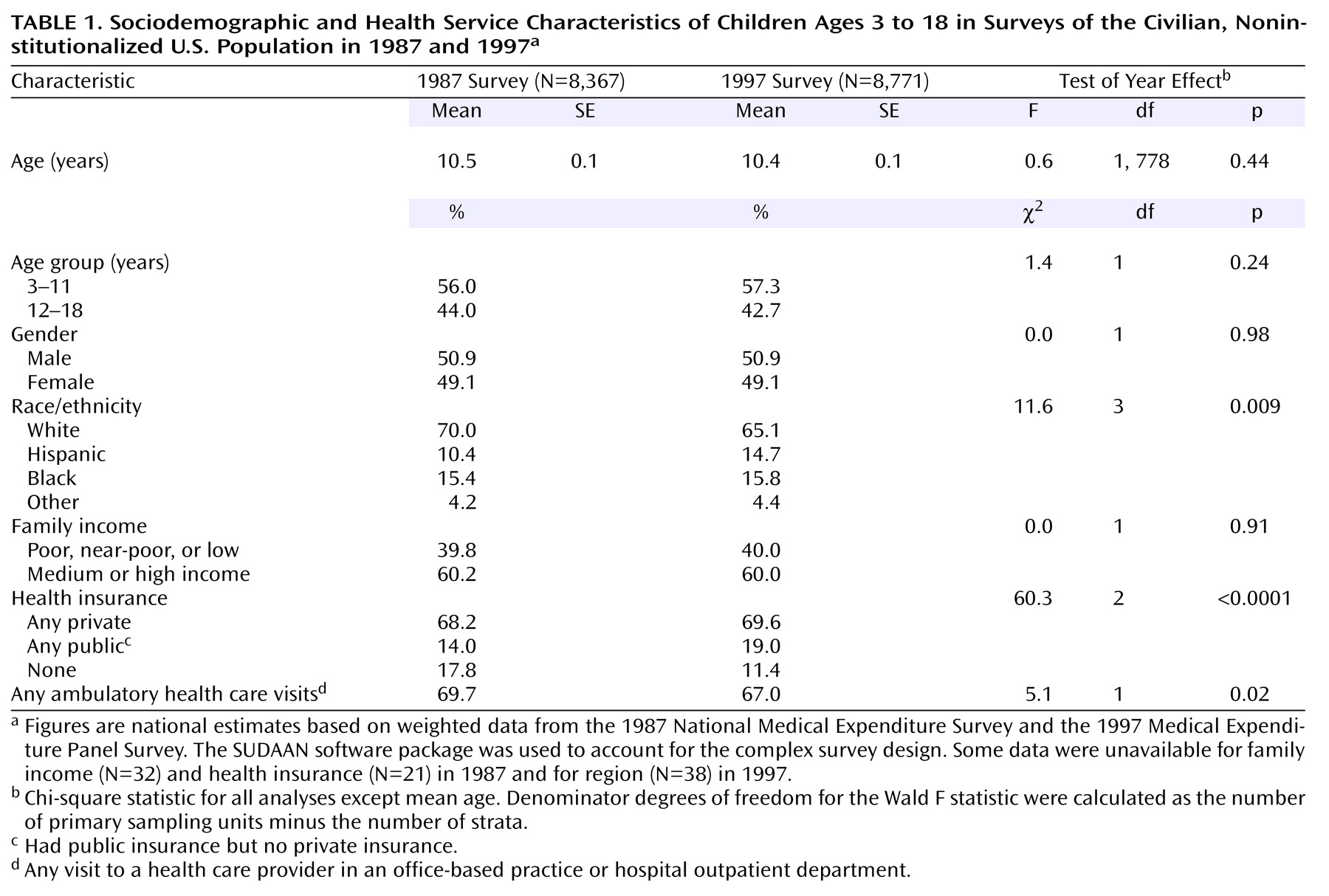
The 1987 survey included 8,367 children ages 3 to 18 years, and the 1997 survey included 8,771 such children. The age, gender, and income distribution of the weighted samples were not significantly different. However, there were increases in the proportion of children of Hispanic ancestry and those with public health insurance (
Table 1).
Rates of Treatment
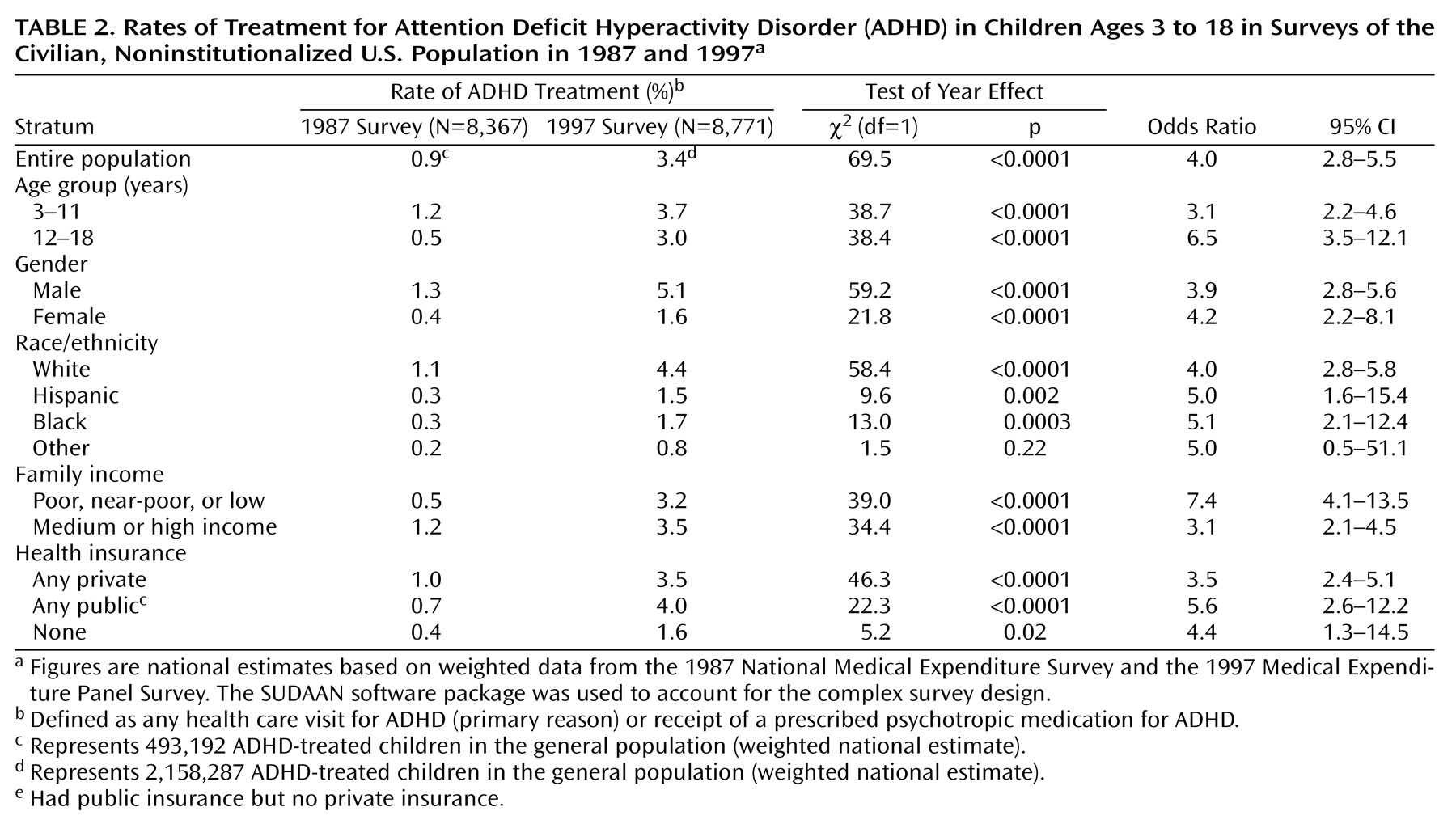
Between 1987 and 1997, there was a significant increase in the overall rate of outpatient treatment of childhood ADHD. The rate of outpatient treatment for ADHD increased from 0.9 per 100 children in 1987 to 3.4 per 100 children in 1997 (odds ratio=4.0, 95% confidence interval [CI]=2.8–5.5). This corresponds to an estimated increase from approximately 493,000 treated children in 1987 to 2,158,000 treated children in 1997. This increase occurred despite a decrease in the proportion of children in the United States who received any ambulatory medical treatment.
Sociodemographic-Specific Rates of Treatment
A significant increase in the rate of treatment of childhood ADHD occurred within all sociodemographic groups we examined, except in a residual “other” race/ethnic category. Older children (12–18 years) experienced a larger proportionate increase in the rate of ADHD treatment than younger children (3–11 years). In both survey years, boys were roughly three times as likely to receive treatment for ADHD as girls, and white children were more than twice as likely as black or Hispanic children to receive treatment (
Table 2).
Family Income and Insurance
In 1987, children from medium- or high-income families were more than twice as likely to receive treatment for ADHD than were children from lower-income families. By 1997, however, the rates of ADHD treatment differed little by family income. The proportionate increase in children treated from lower-income families was more than twice the increase seen in children from medium- or high-income families (
Table 2).
Children with public insurance experienced a larger increase in rates of treatment than those with either private insurance or no health insurance. However, the rate of treatment among uninsured children remained less than one-half of the rate among those with either public or private insurance.
Patterns of Treatment
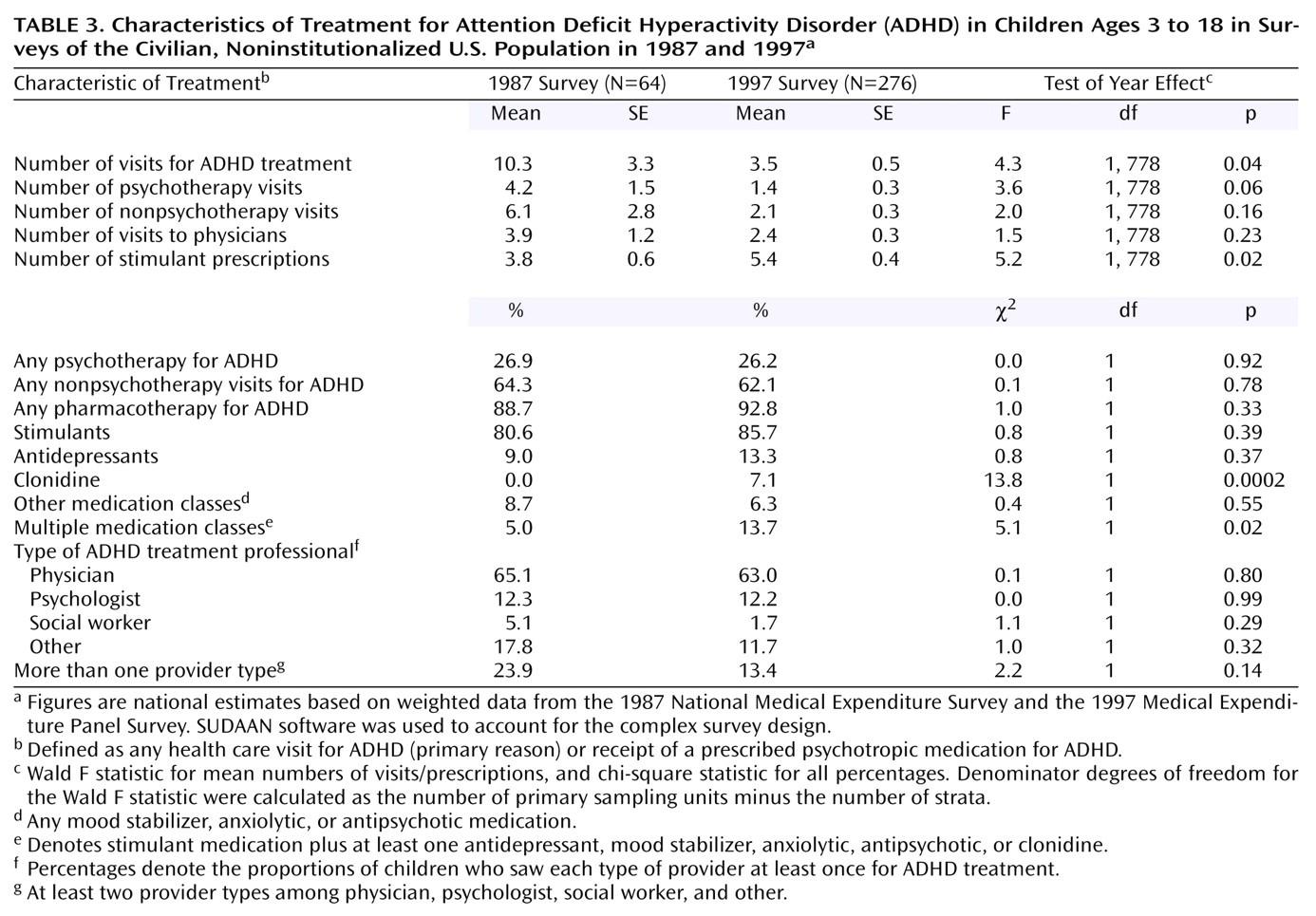
There was a significant decrease in the mean number of ADHD treatment visits used by each treated child (
Table 3). This decline remained significant after control for secular changes in age and family income (beta=–6.5, 95% CI=–0.4 to –12.6). In both surveys, only a minority of treated children received one or more psychotherapy visits for ADHD. Children who received psychotherapy made fewer such visits in 1997 than in 1987 (
Table 3). After control for the potentially confounding effects of age and family income, children who received psychotherapy for ADHD had an estimated 3.0 fewer psychotherapy visits (95% CI=–0.1 to –5.9) in 1997 than in 1987.
Most children who received treatment for ADHD used one or more classes of psychotropic medication for their symptoms. Stimulants were by far the most commonly prescribed psychotropic medications. Although there was no significant change in the proportion of treated children who received stimulants, there was an increase in the mean number of stimulant prescriptions they received. However, this increase fell below the level of statistical significance after control for the effects of patient age and income (beta=–1.3, 95% CI=–3.6 to 1.0). Clonidine, which was not used by any of the treated children in the 1987 survey, was used as part of the pharmacological treatment regimen by 7.1% of the treated children in 1997 (
Table 3). Use of stimulants and at least one other class of psychotropic medication significantly increased.
In both survey years, physicians were involved in the treatment of most children with ADHD (
Table 3). Compared with physicians, psychologists or other health care professionals were involved in the treatment of far fewer children with ADHD.
The 1997 Medical Expenditure Panel Survey included a separate evaluation for special education and related services received by children 5 to 17 years of age. Within this age group, 29.2% of children treated for ADHD received special education or related services. Comparable information was not available from the National Medical Expenditure Survey.
Discussion
During the decade under study, there was a marked expansion in access to treatment for ADHD. In 1997, an estimated 3.4% of children ages 3 to 18 years received treatment for ADHD. This is in the range of community prevalence estimates for ADHD (3% to 5%) among school-age children
(27–
29). Increases in treatment rates were seen in nearly every demographic group studied, with some of the largest increases occurring among groups that have historically received low rates of treatment. Although in 1987, children from poor families were far less likely to receive treatment for ADHD than their more affluent counterparts, this disparity had narrowed considerably by 1997. Similarly, publicly insured children experienced an impressive increase in their rate of ADHD treatment. However, despite significant increases in treatment rates among racial/ethnic minorities, their treatment rates continued to lag well behind those of white children. These findings suggest that cultural factors, rather than economic factors, may explain the low rates of ADHD treatment in racial and ethnic minority groups.
Several factors may have contributed to the observed increase in treatment of ADHD. In 1991, the U.S. Department of Education specifically recognized that students with ADHD could be considered disabled and therefore eligible for special education services
(30). This broadening in the implementation of the Individual Disability Education Act may have helped to increase recognition of ADHD within schools. Together with the growth of school-based health clinics
(31), the reform of special education eligibility may have increased the flow of children into treatment. In one economically disadvantaged community, more than three-fourths of the children receiving mental health services received care exclusively in the education health sector
(32).
Although ADHD assessment instruments have been used by researchers for several decades
(33), brief parent- and teacher-administered scales became widely available during the period under study
(34). Growth in the popularity of easily administered instruments for assessing behavior problems may have promoted recognition and treatment of ADHD.
A growing public awareness of ADHD may have also played a role in the increase in ADHD treatment. In the 1980s, two large national advocacy organizations, Children and Adults with Attention Deficit/Hyperactivity Disorder (CHADD) and the Attention Deficit Disorder Association (ADDA), began holding annual meetings. These groups, which are composed of patients, families, and teachers, provide consumer information and promote awareness of ADHD and its treatment. More recently, the federal government and professional organizations have helped focus attention on the care of ADHD through the development of a consensus statement
(35) and treatment guidelines
(36).
Growth of managed behavioral health care may help to explain the recent decline in visits per treatment episode. Private plans increasingly limit outpatient mental health care visits
(37), and some form of utilization management has become nearly universal
(38). In addition to managed care, changing patient characteristics may have contributed to the declining number of visits per treated child. It is possible that the decline in visits per treated child is a clinical consequence of a decline in the illness severity of children seeking treatment for ADHD
(12).
During the study period, the α-2 agonist clonidine emerged as part of the treatment regimen for a significant proportion of children with ADHD. A meta-analysis of research on clonidine for ADHD symptoms suggests that it may be an effective second-tier treatment
(39). However, concerns have surfaced regarding its many side effects and potential for toxicity in overdose
(40,
41).
The surveys examined have several limitations. The National Medical Expenditure Survey and Medical Expenditure Panel Survey collect data from household informants who may not be fully aware of all of the services used by household members. Stigma, inaccurate recall, and problems distinguishing ADHD from other child mental health problems pose threats to the reporting and classification of the survey data. Without an independent measure of symptoms, it is also not possible to assess the validity of the reported diagnostic codes or to examine secular trends in illness severity. Changes in the coding of the financing of treatment visits prevent us from defining “managed care.”
The treatment of childhood ADHD in the United States expanded during the decade under study. Large numbers of older children, children from lower-income families, children without health insurance, and, to a lesser extent, children from racial and ethnic minority groups were brought into treatment. Children treated for ADHD tended to receive fewer visits but more complex medication regimens. These changes occurred during a period of increasing availability in special education services, growth in the popularity of rapid screening and assessment tools, development of grassroots advocacy groups, and extensive revision in the organization and financing of child mental health services. An important challenge ahead is to link these patterns of service use to key patient outcomes.