From falling leaves to shedding fur, nature provides many external signs that the seasons are changing. Seasonality affects humans as well—just ask anyone with arthritis or allergies. Yet, how seasons impact the underlying molecular details of human physiology is not well understood.
This is an important area to consider in terms of mental health, as more and more research studies are finding evidence that, like many other diseases, psychiatric disorders have seasonal patterns of activity.
A new genetic study appearing in Nature Communications indicates that such seasonal differences have a strong biological component. Researchers examined over 22,000 genes from a diverse set of individuals—from both Northern and Southern hemispheres—and found that nearly a quarter of them (5,136) showed some seasonal variation.
The genes showed a roughly equal split in their activity, with around 2,300 genes being more active in the summer and 2,800 more active in the winter. Most of these genes contributed to processes that seemed quite logical; for example, the composition of blood and fat cells changed during the winter, in line with the concept of preparing to keep the body warm. Genes related to the immune system were also seasonally dynamic, including many genes that affect vaccination response.
“In some ways, it’s obvious,” noted study author John Todd, Ph.D., director of the JDRF/Wellcome Trust Diabetes and Inflammation Laboratory at the Cambridge Institute for Medical Research. “It helps explain why so many diseases, from heart disease to mental illness, are much worse in the winter months.”
The surprising aspect, Todd noted, was the breadth of seasonal change that this study uncovered. He believes the findings may have implications for how we administer vaccines, treat certain diseases, or even carry out research studies.
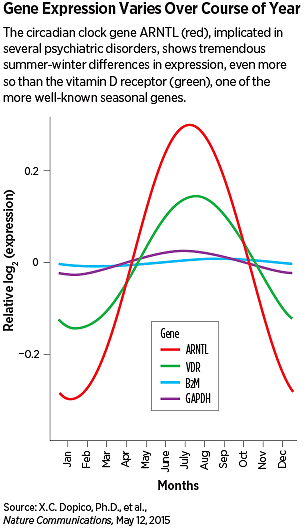
One notable gene of interest to psychiatry was the circadian clock gene ARNTL, which showed a 50 percent increase in activity between February (low) and August (high). (Interestingly, while circadian clock genes might be prime candidates for seasonal change, only about half of the clock genes tested changed in activity during the year.)
ARNTL has been connected with depressive symptoms, especially those in seasonal affective disorder, but has also emerged as a potential player in other mental disorders including bipolar disorder, schizophrenia, and autism.
How the circadian clock may affect a symptom like psychosis is still being teased out, though Todd and his colleagues did find that several anti-inflammatory genes, such as the receptors that bind the stress hormone cortisol, had expression profiles that mirrored ARNTL. Numerous research studies have hinted at a connection between schizophrenia and the immune system, including a recent analysis carried out by the Psychiatric Genomic Consortium that identified over 80 new schizophrenia risk genes (
Psychiatric News, August 5, 2014).
The current study used data from over 16,000 volunteers from the United States, United Kingdom, Iceland, Germany, Australia, and The Gambia. The work was supported by the National Institute for Health Research. ■
“Widespread Seasonal Gene Expression Reveals Annual Differences in Human Immunity and Physiology” can be accessed
here.