Sutter Health, a Northern California hospital system, is gradually rolling out a telepsychiatry program at all 24 of its locations to better meet patients’ needs and solve their psychiatrist shortage problem, especially at their most rural hospitals.
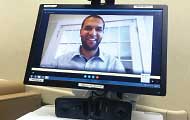
Now, with the service in operation at 13 of their hospitals, telepsychiatrists access patients via a workstation that can be wheeled into the patient’s room. The board-certified psychiatrists are based all over the country and spend about 45 minutes with each patient from their home office.
“A number of our hospitals are in rural areas and had no psychiatry services or had very limited pockets when a psychiatrist was available,” explained Tim Jones, N.P., Sutter Health’s telepsychiatry program manager. “But psychiatric care emergencies occur 24-7, and we wanted to make sure we had robust acute care in our emergency rooms and on our medical floors that meets patients’ needs.”
While in many emergency rooms across the country, wait times for patients who need to see a psychiatrist range from several hours to several days, Sutter Health patients who need a psychiatric consult in the emergency department or on their medical floors can often be seen within an hour of a provider’s request to a central call center.
The participating psychiatrists are all licensed to work in California and hired by Virtual Medical Staff, an Atlanta-based company that has been providing telepsychiatry services to hospitals for the past seven years. The psychiatrists go through a credentialing process and get privileges at each hospital in which they practice. They are given real-time access to the patients’ electronic health records so they can order labs, tests, or medications and enter treatment notes.
Virtual Medical Staff’s telepsychiatrists are issued enhanced audiovisual equipment, and the live feed between the patient and the physician is protected with (128-bit) encryption technology and is HIPAA compliant, explained Jack Williams, president of Virtual Medical Staff.
The company provides telepsychiatry services for about 350 hospitals nationwide. For about half of them, it provides 24-7 coverage, like at Sutter Health, and for half its patients, it supplements an in-house psychiatry service by covering the night shifts, 7 p.m. to 7 a.m.
For clinicians, the telepsychiatry setup gives them work flexibility and the ability to reach a broader population than would otherwise be possible if they had to drive to various locations throughout the state, Williams said. “They really like the technology because it allows them to see more patients faster and without having to physically travel,” he said. “They are able to make a bigger impact than they would if they were just working at one location.”
“This is another way for them to extend their practices,” Jones said. “For patients, it helps clarify their diagnoses: Is this delirium, dementia, or new-onset psychosis? Psychiatrists help us clarify these ‘gray area’ presentations we often find.”
One task the telepsychiatrists can’t do is complete a California 5150, an involuntary hold that requires on-site clinician involvement. “They can recommend it, but by law the applications must be completed by on-site staff,” Jones explained.
More than 1,500 telepsychiatry consults have been completed within Sutter Health since the launch of the program last fall, and the service will be rolled out to all of its hospitals by the end of the first quarter of 2019, Jones said.
At this time Sutter Health is not passing along the cost of the program to its patients “because we believe this is the right thing to do for our patients. They need this level of care and service, and by actively treating their psychiatric symptoms, we can reduce their length of stay and in many instances reduce their need for higher levels of care like psychiatric hospitalization.” ■
APA’s Telepsychiatry Toolkit, developed by the APA Work Group on Telepsychiatry, can be accessed
here.