Autism spectrum disorder (ASD) is characterized by impairments in social communication and interaction and by the presence of restricted interests and repetitive behaviors (
1). The presentation of core and related symptoms, such as intellectual disability (
2), aggressive and self-injurious behaviors, and sleep and eating problems, can vary widely among children with ASD and persist across the lifespan (
3–
7). As a result, children with ASD often receive intensive and costly long-term care, particularly in schools (
8). Generally, school-based services address specific behaviors (for example, aggression, self-injury, attention, and impulse control) that significantly interfere with overall adaptation, learning, and functioning. Services may also include instructional and behavioral support from one-on-one aides (
9). Given the amount of time that children with ASD spend in schools, access to these services is critically important (
10).
The Centers for Disease Control and Prevention has estimated that one in 68 children in the United States has ASD (
11). The growing number of children with ASD has raised concerns about the cost of care, which is generally higher than for children with other psychiatric disorders (
12). Children with ASD receive educational services through the Individuals with Disabilities Education Act (IDEA), which provides services necessary for children to receive a “free and appropriate education” (
8,
13). IDEA prohibits use of federal education funds to pay for medical care, even though this care may be related to academic functioning (
14). IDEA also is underfunded. The U.S. Department of Education’s National Center for Education Statistics reports that in 2014 IDEA funds covered only 16% of the estimated cost of educating children with disabilities (
15). Because IDEA does not cover medical services and because it is so underfunded, many states leverage Medicaid to pay for school-based services for children with special needs, including those with ASD (
16–
18). There is no published estimate, however, of the scale of Medicaid spending on school-based services for children with ASD.
This issue has assumed particular urgency because the number of children receiving Medicaid-reimbursed services is anticipated to increase by millions under the Affordable Care Act (ACA) (
19). The ACA contains important provisions that may expand access to services for individuals with ASD. Under the ACA, most health insurance plans are no longer allowed to deny, limit, exclude, or charge more for coverage to anyone on the basis of a preexisting condition, including ASD; most private insurance plans must cover preventive services for children (including screening); individuals with ASD have expanded access to Medicaid and other affordable insurance options; and new health plans must cover “essential health benefits,” including hospitalization, preventive services, and prescription drugs, to help ensure that individuals have the coverage needed to stay healthy (
20). With the ACA’s implementation, there has been ample discussion about medical homes and community-based services; however, school-based services are not mentioned. Rigorous estimates of the number of children with ASD receiving Medicaid-reimbursed school-based services and the associated expenditures will guide policy makers and behavioral health care professionals as they make decisions about whether Medicaid expansion and the ACA should cover school-based mental health services.
To provide some insight into this issue, we identified use of in-school individual behavioral health services and out-of-school behavioral health services and average annual Medicaid expenditures for service use among children with ASD from 2008 to 2009 in a large, metropolitan county of Pennsylvania. To place these numbers in context, we compared service use and expenditures for children with ASD with those of other Medicaid-enrolled children with psychiatric disorders.
Methods
Data Source and Study Sample
Philadelphia County Medicaid claims were used to identify a subset of children between the ages of five and 17 who received behavioral health services through Medicaid during October 2008 through September 2009 (N=24,271). The University of Pennsylvania’s Institutional Review Board and the Institutional Review Board of the City of Philadelphia Department of Public Health approved the study protocol.
Variables
All variables, including age, sex, race-ethnicity, psychiatric diagnosis, behavioral health service use, and expenditures, were extracted from the Medicaid claims data. Annual mean Medicaid expenditures were calculated by summing the reimbursed dollar amount (2008–2009 dollars) per Medicaid claim by behavioral health service type and dividing the total amount by the number of service users. Children were categorized as having ASD, conduct disorder or oppositional defiant disorder (conduct-ODD), attention-deficit hyperactivity disorder (ADHD), or other psychiatric disorders. Children with two or more Medicaid claims associated with an ICD-9 primary diagnosis of 299.xx were identified as having ASD. Children with two or more Medicaid claims associated with an ICD-9 primary diagnosis of 312 or 313 were identified as having conduct-ODD. Children with two or more ICD-9 primary diagnoses of 314 were identified as having ADHD. Children with other ICD-9 primary diagnoses were categorized as having other psychiatric disorders. Children with comorbid diagnoses were classified according to the hierarchy of ASD, ADHD, conduct-ODD, and other psychiatric disorders. Of the 24,271 children in the sample, 4.4% (N=1,068) had two different psychiatric diagnoses and .02% (N=4) had three different psychiatric diagnoses in the Medicaid claims data.
Behavioral health services were categorized on the basis of the Level of Care codes from Medicaid claims data as in-school individual behavioral health services (one-on-one behavioral support) and out-of-school behavioral health services (outpatient treatment and out-of-school Behavioral Health Rehabilitation Services [BHRS]). In Pennsylvania, BHRS include wraparound services designed to provide therapeutic intervention to children ages three to 21 with serious emotional disturbance or social or behavioral problems (
21). Demographic variables included age (recoded as 5–11, 12–14, and 15–17 years), sex (male and female), and race-ethnicity (African American, white, Hispanic, and other race).
Analysis
First, we examined the distribution of demographic characteristics and behavioral health service use by psychiatric disorder. Chi square tests were used to examine differences in distributions. Second, logistic regression analyses were used to model children’s in-school and out-of-school behavioral health service use (dependent variable) by psychiatric disorder, adjusting for age, sex, and race-ethnicity. We also calculated annual mean Medicaid expenditures for service users by service type and total mean Medicaid expenditures for in-school and out-of-school service use for each psychiatric disorder. Generalized linear models with a gamma distribution and log link function were used to compare differences in expenditures for in-school and out-of-school behavioral health service use and total mean expenditures for in-school and out-of-school service use by psychiatric disorder, adjusting for age, sex, and race-ethnicity.
Results
A total of 170,202 children ages five to 17 were enrolled in Medicaid in Philadelphia during the 2008–2009 school year; 24,271 received Medicaid-reimbursed behavioral health services.
Table 1 presents demographic characteristics by psychiatric disorder. The most common psychiatric diagnosis was ADHD (39.8%); 35.2% had other psychiatric disorders, 21.1% had conduct-ODD, and 3.9% had ASD. Most of the children (63.1%) were male, and the average age was 11.3±3.6. Most of the children with ASD (69.7%) and with ADHD (66.6%) were between the ages of five and 11, whereas children with conduct-ODD and children with other psychiatric disorders had more evenly distributed ages. Psychiatric disorder groups differed by sex and race-ethnicity. Whereas only 15.6% of children with ASD were females, 33.4% children with conduct-ODD, 28.0% of children with ADHD, and 51.5% of children with other psychiatric disorders were females. Less than 50% of children with ASD or ADHD were African Americans, whereas 74.8% of children with conduct-ODD and 59.7% of children with other psychiatric disorders were African Americans. The ADHD group had the highest proportion of children of Hispanic origin (38.7%), followed by other psychiatric disorders (24.7%), conduct-ODD (16.2%), and ASD (13.6%).
Table 2 presents data for in-school and out-of-school behavioral health service use and annual mean Medicaid expenditures by psychiatric disorder. Behavioral health service use differed by psychiatric disorder in the unadjusted models. Among children with ASD, 51.9% used in-school individual behavioral health services, compared with 5.1% of children with conduct-ODD, 8.2% of children with ADHD, and 1.7% of children with other psychiatric disorders (p<.001). Although most children used out-of-school behavioral health services, the percentages of users ranged from 89.7% for children with conduct-ODD to 97.7% of children with ADHD (p<.001).
Table 2 presents adjusted ORs and 95% confidence intervals for behavioral health service use by psychiatric disorder. Compared with children with ASD, children with conduct-ODD were less likely to use in-school services (OR=.06) and also less likely to use out-of-school services (OR=.29) (p<.001 for both). Compared with children with ASD, those with ADHD were less likely to use in-school services (OR=.09) and more likely to use out-of-school services (OR=1.13) (p<.001 for both). Compared with children with ASD, those with other psychiatric disorders were less likely to use in-school services (OR=.02) and to use out-of-school services (OR=.96) (p<.001 for both).
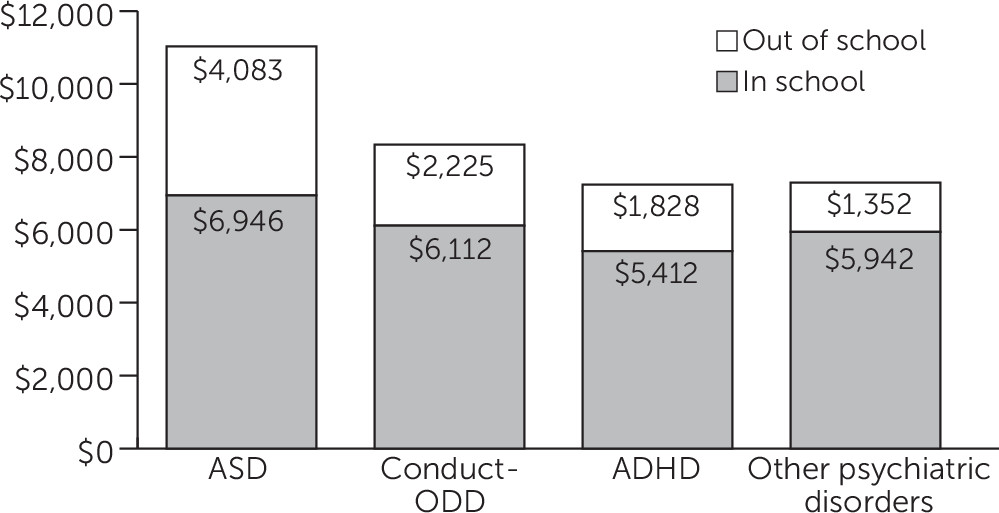
Figure 1 shows annual unadjusted mean Medicaid expenditures for in-school individual behavioral health services and out-of-school behavioral health services, by disorder. Mean±SD expenditures for both in-school and out-of-school services were highest for children with ASD ($6,946±$3,609 and $4,083±$5,375, respectively). Children with ASD had higher mean expenditures for in-school services than did children with conduct-ODD ($6,112±$3,560), ADHD ($5,412±$3,589), and other psychiatric disorders ($5,942±3,949). Children with ASD also had higher mean expenditures for out-of-school services than children with conduct-ODD ($2,225±$4,027), ADHD ($1,828±$3,368), and other psychiatric disorders ($1,352±$2,946).
The generalized linear model analysis with gamma distribution indicated significant differences in adjusted Medicaid expenditures for both types of behavioral health service use by psychiatric disorder (
Table 3). Compared with expenditures for in-school individual behavioral health services for children with ASD, expenditures were lower for children with conduct-ODD (OR=.89, p<.05)) and children with ADHD (OR=.80, p<.001). Compared with expenditures for out-of-school services for children with ASD, expenditures for children with conduct-ODD, children with ADHD, and children with other psychiatric disorders were lower (OR=.50, OR=.47, and OR=.32, respectively, p<.001 for all). Adjusted and unadjusted total expenditures for in-school and out-of-school services also differed significantly by psychiatric disorder (p<.001 for all). Compared with the total mean expenditures for children with ASD, expenditures for children with conduct-ODD, children with ADHD, and children with other psychiatric disorders were lower in the adjusted model (OR=.33, OR=.31, and OR=.20, respectively, p<.001 for all).
Discussion and Conclusions
Our findings suggest the importance of Medicaid-funded behavioral health services for children with ASD. Children with ASD were significantly more likely than children with all other psychiatric disorders to use in-school behavioral health services. Children with ASD were also significantly more likely than children with conduct-ODD and with other psychiatric disorders (except those with ADHD) to use out-of-school behavioral health services. Medicaid-reimbursed expenditures for in-school services for children with ASD were significantly higher than for children with conduct-ODD or ADHD. Medicaid expenditures for out-of-school services for children with ASD were significantly higher than for children with any other psychiatric disorder. Although children with ASD constituted the smallest group of those receiving Medicaid-funded behavioral health services, total expenditures for in-school and out-of school service use were significantly higher than for children with all other psychiatric disorders. The behavioral health system spends more on services for children with ASD than for children with any other disorder, despite the relatively small number of children with ASD.
Some study limitations should be mentioned. First, the analysis was limited to Philadelphia Medicaid claims, which limits the geographic generalizability of the findings and does not take into account the potential role of spending through the education system, through private insurance, or out-of-pocket costs. Philadelphia is an important study site in its own right, in that it serves one-third of Pennsylvania’s Medicaid population, is more urban, and has a higher number of children from racial-ethnic minority groups than other counties. Large, urban school districts, such as Philadelphia, serve a disproportionately large number of children in the United States (
22) and therefore represent important areas for study.
A second limitation is that our analysis was based on one year of cross-sectional data. The results should be interpreted with caution because the content of services and the reimbursement structure may change over time and service use and expenditures change accordingly. Finally, diagnoses were not validated, although recent studies suggest the accuracy of the autism diagnosis in Medicaid claims (
23).
Despite these limitations, the findings have important implications. Medicaid is a particularly important resource for children with ASD in providing school-based behavioral health services. However, it is unclear how behavioral health services will be financed and delivered in schools under the ACA. States that participate in the Medicaid expansion must offer benefits similar to those provided by private insurance companies in that state (
24). These services generally include inpatient and outpatient hospital services, X-ray and lab services, physician services, mental health services, well-child care, and prescription drugs (
24). School-based services are notably absent from this list.
The number of families seeking Medicaid-funded ASD services may decrease as more states enact mandates that require private insurance companies to cover autism services (
23). However, autism insurance mandates notably do not cover ASD-related services in schools (
12). It is imperative that as the number of mandates increases, coverage of school-based services is not lost. Although a large amount of money is spent on in-school individual behavioral health services, a growing body of research suggests that the quality and outcomes of these services are relatively poor. Thus further investigation to identify high-quality, evidence-based interventions for effective and efficient school-based care in the real-world setting is important. The ACA explicitly emphasizes the importance of using evidence-based practices, but there is no discussion in the legislation of how these practices should be chosen, implemented, or measured. On the basis of our findings, protecting Medicaid-reimbursed school-based care for children with ASD is of the utmost importance. Schools should be considered an important site for service delivery for children with ASD and other psychiatric disorders, regardless of the funding mechanism.