Treatment
Patients first received a psychological evaluation using a Therapeutic Model of Assessment ([TMA];
Finn and Tonsanger, 1997;
Hilsenroth, 2007). The TMA uses a multi-method assessment (i.e., interview, self-report, performance tasks and free response measures). Moreover, the TMA focuses sharply on the development and maintenance of empathic connections with patients, factors contributing to maintenance-of-life problems (often relational), collaboration in defining individualized treatment goals and tasks, and the sharing and exploration of assessment results with patients. The TMA used in this study consisted of four components, including three meetings between the patient and clinician that totaled approximately four-and-one-half hours, and an additional patient appointment to complete a battery of self-report measures. The three meetings included (1) a semi-structured diagnostic interview (
Westen & Muderrisoglu, 2003,
2006), (2) a follow-up interview, and (3) a collaborative feedback session. The collaborative feedback session emphasized prominent inter- and intra-personal themes derived from the test results, the patient-therapist interaction, and factors contributing to the maintenance-of-life problems. This session also provided an opportunity to explore these new understandings and apply them to the patient’s current problems in living. The patient and clinician also reviewed a socialization interview (SI) (developed by
Luborsky, 1984) on what to expect in psychodynamic psychotherapy. The SI delineates the patient’s and clinician’s roles during treatment and highlights the relational focus of the therapeutic process. An aim is for the patient to become more cognizant of dynamics that were not known before the start of psychotherapy. Finally, the clinician and patient work together to develop treatment goals and to negotiate an explicit treatment frame (i.e., scheduling session times, frequency of treatment session[s], missed sessions and payment plan). For this study, the clinician who carried out the psychological assessment was also the clinician who conducted the formal psychotherapy sessions.
Individual psychotherapy consisted of once- or twice-weekly sessions of psychodynamic treatment that were organized, aided, and informed (but not prescribed) by the technical guidelines delineated in the treatment manuals detailed above. Key features of the psychodynamic treatment model utilized in these sessions included (
Blagys & Hilsenroth, 2000):
1)
focus on affect and the expression of emotion,
2)
exploration of attempts to avoid topics or engage in activities that could hinder the progress of therapy,
3)
identification of patterns in actions, thoughts, feelings, experiences, and relationships,
4)
emphasis on past experiences,
5)
focus on interpersonal experiences,
6)
emphasis on the therapeutic relationship, and
7)
exploration of wishes, dreams, or fantasies.
In addition to these areas of treatment focus, relational patterns, case presentations, and symptoms were conceptualized in the context of cyclical patterns (
Book, 1998;
Luborsky, 1984;
McCullough et al., 2003;
Wachtel, 1993). Also, the
Safran and Muran (2000) model of intervention was used in responding to treatment ruptures and repair as they occurred in the therapeutic relationship. Treatment was open-ended in length, rather than of a fixed duration. Setting a termination date became a frequent area of intervention, since issues related to the termination were often linked to key interpersonal, affective, and thought patterns prominent in that patient’s treatment.
Treatment goals are first explored during the assessment feedback session, and a formal treatment plan is reviewed with each patient early in the course of psychotherapy. This treatment plan is subsequently reviewed at regular intervals for changes, additions, or deletions. Prior to these review points, we reassessed patient functioning on a standard battery of outcome measures as well as process ratings completed by patients and therapists immediately after selected sessions. Patients were informed—both verbally and in writing—that that their therapists would not have access to their responses on any psychotherapy process measure (i.e., alliance, session process, etc.). Also, all treatment sessions (not just the sessions during in which reassessment ratings were completed) were videotaped. Patient process ratings as well as the independent technique ratings for this study were collected at the same point in time, early in therapy (post-TMA assessment), predominantly at the third or fourth sessions. Mean number of sessions attended by these 88 patients was 25 sessions during (an average of) eight months. However, the median number of sessions and length of treatment were somewhat shorter, 21 sessions and six months.
Procedure
All participants were representative of individuals seeking outpatient treatment at a university-based community clinic. Individuals were asked to participate in a research study about patients’ interactions with their therapists. Cases were assigned to treatment practicums and clinicians in an ecologically valid manner based on real world issues including aspects of clinician availability, case load, etc. Moreover, patients were accepted into treatment regardless of disorder or comorbidity. All patients provided informed consent, and they received no monetary compensation for their participation in the study.
All sessions of treatments were videotaped, not just the sessions during which the process measures were completed. Videotapes of an early session (third/fourth) of each patient’s treatment were coded by external raters using the Comparative Psychotherapy Process Scale (CPPS). The Vanderbilt Psychotherapy Process Scale-Short Form (VPPS-S) and The Combined Alliance Short Form-Patient Version (CASF-P) were administered directly after these sessions, and the CPPS was rated by independent coders at a later date, by viewing a videotape from the therapy session.
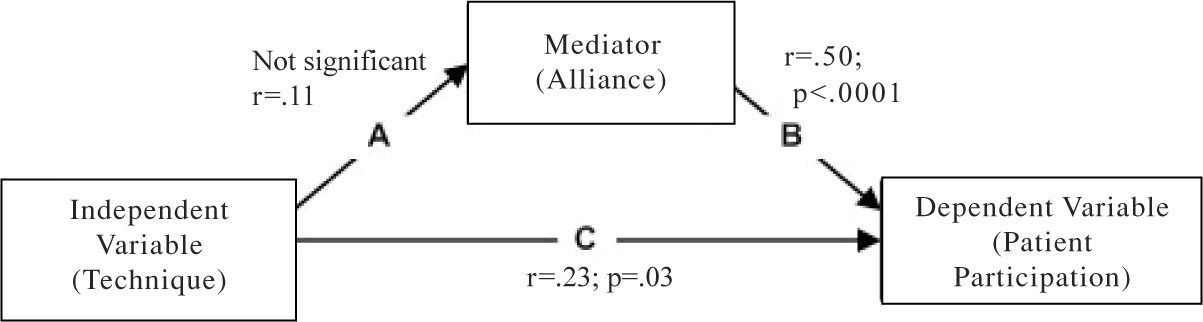
In order to highlight the contribution and relationship among alliance, technique, and participation, we employed a mediational analysis.
Baron and Kenny (1986) explained that the mediator is the catalyst that enables the independent/predictive variable to influence the dependent variable. To establish mediation the following conditions need to be met:
Path A: The independent variable (technique) must be significantly correlated with the mediator variable (alliance);
Path B: The mediating variable (alliance) must account for variance in the dependent variable (patient participation);
Path C: When paths are controlled, previously significant correlations between the independent (technique) and dependent variables (patient participation) become insignificant.
Thus, the following three steps were performed to rule out possible mediation.
Step 1: The correlations between the predictive variable (technique) and mediator (alliance) were examined.
Step 2: Once it is established that the predictive variable (technique) is significantly correlated with the mediating variable (alliance), the relationship of these variables with the dependent variable (patient participation) will be examined.
Step 3: The last stage for mediation is to examine the relationship between the predictor (technique) and dependent variables (patient participation). The relationship must not be significant after the mediator (alliance) is controlled.
Measures
The constructs that were assessed included treatment interventions, which were coded using the Comparative Psychotherapy Process Scale (CPPS;
Hilsenroth, Blagys, Ackerman, Bonge & Blais, 2005), and patient participation in the therapeutic process, which was assessed by utilizing the Patient Participation subscale of the Vanderbilt Psychotherapy Process Scale-Short Form (VPPS-S;
Smith, Hilsenroth, Baity & Knowles, 2003). The Combined Alliance Short Form-Patient Version (CASF-P;
Hatcher & Barends, 1996) was used to assess the therapeutic alliance. Therefore, the data for this study were the patient responses on the VPPS-S, independent ratings of therapeutic techniques using the CPPS from videotaped sessions early in treatment, and patient responses to the CASF-P—all of which were taken from the same early treatment session.
Comparative Psychotherapy Process Scale-External Rater Form (CPPSER;
Hilsenroth, Blagys, Ackerman, Bonge, & Blais, 2005). The CPPS is a brief descriptive measure designed to assess therapist activity and technique used during the therapeutic hour. The CPPS-ER is based on the findings of two empirical reviews of the comparative psychotherapy process literature (
Blagys & Hilsenroth, 2000; 2002). Based on these reviews, a list of interventions were developed that represent characteristic features of psychodynamic-interpersonal therapy ([PI]; defined broadly to include psychodynamic, psychodynamic-interpersonal, and interpersonal therapies) and cognitive-behavioral ([CB]; defined broadly to include items that are significantly more characteristic of cognitive-behaviorally oriented therapy [
Blagys & Hilsenroth, 2002], cognitive, and behavioral therapies). The PI subscale measures the seven domains of therapist activity previously described as key features of the psychodynamic treatment model (
Blagys & Hilsenroth, 2000). The CB subscale consists of items which include:
1)
emphasizing cognitive or logical/illogical thought patterns and belief systems;
2)
teaching skills to patients;
3)
assigning homework to patients;
4)
providing information regarding treatment, disorder, or symptoms;
5)
directing session activity; and
6)
emphasizing future functioning.
The CPPS measure consists of 20 randomly ordered techniques rated on a 7-point Likert scale ranging from 0—not at all characteristic, 2—somewhat characteristic, 4 — characteristic, to 6—extremely characteristic. The CPPS may be completed by a patient (P), therapist (T), or an external rater (ER). Ten statements are characteristic of PI interventions, and ten statements are characteristic of CB interventions. These interventions can then be organized into two scales: one measuring PI features (CPPS-PI, 10 items), and one measuring CB features (CPPS-CB, 10 items).
The reliability and clinical validity of the CPPS has been well established (see
Hilsenroth, 2007 for a review). We have recently reported (
Hilsenroth et al., 2005; Slavin-Mulford, Hilsenroth, Weinberger, & Gold, 2011; Stein, Pesale, Slavin, & Hilsenroth, 2010) on the excellent inter-rater reliability and internal consistency of the CPPS, as well as the results of validity analyses conducted across several different contexts and samples. The CPPS data we utilized in the current study are derived from these reports, follow procedures detailed there, and were provided by trained external raters who have demonstrated the ability to rate these individual techniques in the good (ICC [intra-class correlation coefficient] = .60–.74;
Fleiss, 1981) to excellent range (ICC ≥ .75;
Fleiss, 1981). Several sets of external raters demonstrated good to excellent reliability on the CPPS for the sessions used in the current study (
Stein et al., 2010). All Spearman-Brown corrected mean ICCs for the individual CPPS-PI and CPPS-CB techniques were in the good-to-excellent range (and thus were examined individually), as were the ICCs for the CPPS-PI and CPPS-CB scale scores. Corrected average ICCs were reported for both CPPS technique items and subscales; two external raters evaluated all of the sessions, allowing us to use their more reliable average ratings across their pairs. In the current study, the mean CPPS-PI scale score for the rated sessions was 3.30 (SD = 0.72), and the mean CPPS-CB scale score was 1.28 (SD = 0.57), representing a significant level of therapist technique that was consistent with a psychodynamic treatment model (degrees of freedom [df] = 87,
t = −20.46,
p < .0001,
d = 3.1), in the same session that patient alliance was rated. Coefficient alphas for the CPPS-PI and CPPS-CB scales from the 88 sessions rated in this study were .80 and .75, respectively.
Videotapes of an early treatment session (third/fourth) for each patient were arranged in random order, and entire sessions were watched/rated by two raters independently. Raters were graduate students in clinical psychology. Immediately after viewing a videotaped session, judges independently completed the CPPS; each subscale (PI and CB) was coded in random order. Regular reliability meetings were held during the coding process to prevent rater drift (for a more detailed description of this rater training process, see
Stein et al., 2010).
The Vanderbilt Psychotherapy Process Scale-Short Form: Patient Participation Subscale ([VPPS-S-Patient];
Smith, Hilsenroth, Baity & Knowles, 2003). The VPPS-S-Patient is a Likert-scale (1 = very poor, 2 = poor, 3 = fair, 4 = good, 5 = excellent), in which patients assess their behavior, demeanor, and feelings during session. There are eight items on the Patient Participation subscale. In the section of the VPPS titled “characterize your behavior during this hour,” these subscale items include: “I actively participated in the interaction;” “I took the initiative in bringing up the subjects that were talked about;” “I was motivated for the session;” “I was logical and organized in expressing thoughts and feelings;” and “I talked about my feelings.” Items on the patient participation subscale in the section titled “describe your demeanor and feelings during this hour” include rating the level of “inhibition (reverse scored);” “spontaneity;” and “passivity (reverse scored).”
The VPPS-S has been instrumental in better understanding patient participation during sessions. There have been many studies that have built upon this instrument, such as the studies conducted by Windholz and Silberschatz (1988) as well as
Smith, Hilsenroth, Baity and Knowles (2003). Suh, O’Malley, Strupp and Johnson (1989) discussed the evolution of the Vanderbilt Psychotherapy Process Scale (VPPS). These researchers explained that the VPPS is a clinical rating system that examines positive and negative dimensions of patient and therapist “behavior and attitude” and how these dimensions impacts overall therapeutic outcome (
Suh et al., 1989). The subscales investigate both patient and therapist characteristics (i.e., patient participation and therapist emotional involvement) during session. The subscales of the VPPS demonstrate both high internal consistency and inter-rater reliability. The VPPS is unique in that it is effective irrespective of the theoretical orientation to which a clinician subscribes (
Suh et al., 1989).
Smith and colleagues (2003) reported a coefficient alpha of .76 for the patient participation subscale using a subset of the current participants, as well as the factor structure, psychometric characteristics and convergent validity data. For the current sample, the mean VPPS Patient Participation scale was 4.00 (SD = 0.46; range = 2.75 to 4.88) from the early treatment sessions (i.e., third or fourth) used in this study.
The Combined Alliance Short Form-Patient Version (CASF-P;
Hatcher & Barends, 1996). The CASF-P is a patient-rated alliance measure created from a factor analysis of the responses from 231 outpatients at a university-based community clinic and was based on three widely used measures of alliance: (a) the Penn Helping Alliance Questionnaire (HAQ;
Alexander & Luborsky, 1986), (b) the Working Alliance Inventory (WAI;
Horvath & Greenberg, 1986), and (c) the California Psychotherapy Alliance Scales (CALPAS;
Gaston, 1991). The CASF-P consists of 20 items rated on a 7-point scale consisting of 1—never, 2—rarely, 3—occasionally, 4—sometimes, 5—often, 6—very often, and 7—always. The psychometric properties, reliability and validity of this measure are outlined by
Hatcher and Barends (1996). Hatcher and colleagues (
Hatcher & Barends, 1996;
Hatcher, Barends, Hansell, & Gutfreund, 1995) reported initial evidence on both the construct and incremental validity of this scale with regard to outcome. An examination of the internal consistency of this measure has demonstrated a coefficient alpha of .91 for the Total Scale using a subset of the current participants (
Ackerman, Hilsenroth, Baity & Blagys, 2000). Both
Ackerman et al. (2000) and
Clemence et al. (2005) reported convergent validity data with related measures of psychotherapy process, as well as criterion validity with regard to the prediction of treatment outcome using a sample of clients at the same university-based clinic as the patients in the current study.
The CASF-P consists of four subscales: Confident Collaboration (e.g., “What I am doing in therapy gives me new ways of looking at my problems”); Goals and Tasks (e.g., “My therapist and I are working on mutually agreed upon goals”); Bond (e.g., “My therapist and I trust each other”), and Idealized Relationship (e.g., “How much do you disagree with your therapist about what issues are most important to work on during these sessions? [this particular item is reverse scored]).”