Despite the need for expanding child psychiatric services, telepsychiatry has been used primarily in adult psychiatric practice. Efforts to use this medium in child psychiatry are limited. There are fewer than 8,000 child psychiatrists in the United States and a limited number in child psychiatry fellowship training; the Surgeon General estimates that less than 20% of the 13.7 million children and adolescents in need of treatment for mental illness receive care (
1). Similar to adult rates, 20% of children and adolescents in the United States are estimated to have emotional and behavioral disorders. Suicide was the third leading cause of death among children aged 10–24 in 2004 (
2), and there is evidence of even higher suicide rates among children in rural areas (
3,
4). Calloway et al. (
5) noted several articles reporting that rural youth receive fewer mental health services than urban youth. Almost three-fourths of smaller rural counties with populations of 2,500–20,000 lack a psychiatrist and 95% lack a child psychiatrist. Consequently, children in these regions with serious mental health problems are among the most disadvantaged in receiving care (
6).
The use of videoconferencing technology gives specialists a means of providing care at a distance. Its application would improve the quality of treatment, reduce its cost, and clearly create accessibility for patients (
7). Telemedicine applied to psychiatry is defined as the use of electronic communication and information technologies in order to provide or support its application of clinical psychiatric care at a distance (
2). Videoconferencing technologies enables a real-time patient and a mental health professional to simultaneously connect with one or more primary sites and one or more secondary sites for a diagnostic, therapeutic, or educational direction (
9).
A review of the literature revealed 33 articles relevant to child telepsychiatry. Eight published case studies (
5–
12) demonstrated that telepsychiatry can benefit children, adolescents, and their families. In three studies comparison groups were used to measure the reliability of interactions in face-to-face versus telepsychiatry consultations. Myers et al. (
13) found that there were no significant differences between a direct care and a telepsychiatry treatment group. There were no significant differences in the two randomized controlled trials comparing face-to-face with telepsychiatry diagnosis and treatment outcomes (
14,
15).
There have been several published child telepsychiatry program descriptions. However, none of these provide enough specific data and detail about the telepsychiatry clinics in order to replicate them for clinical or research purposes. Programs have been used in hospitals, schools (
9,
11,
15,
17), forensic settings (
21), and youth correctional facilities (
25). Eighteen articles evaluated satisfaction with clinical care, services, education, and technology offered through telepsychiatry (
7,
14,
15,
18,
20,
21,
25–
36).
Child telepsychiatry systems have been implemented for a variety of educational purposes. Reports of successful uses in continuing professional education and in-service training were established (
17,
20,
21,
31,
37). Interactive sessions were also implemented, focusing on current clinical cases for which supervision or consultation was also provided through videoconferencing (on an ongoing or as-needed basis) (
16,
27,
30,
35,
38). Four comprehensive articles pertained to child and adolescent psychiatry (
30,
39–
41). Three of these authors made recommendations for future research and programmatic design. Alessi (
39) concluded that more standardized empirical research studies and empirically validated measures are needed. Boydell et al. (
40) created a framework to guide the development of telepsychiatry programs.
A TELEPSYCHIATRY MODEL
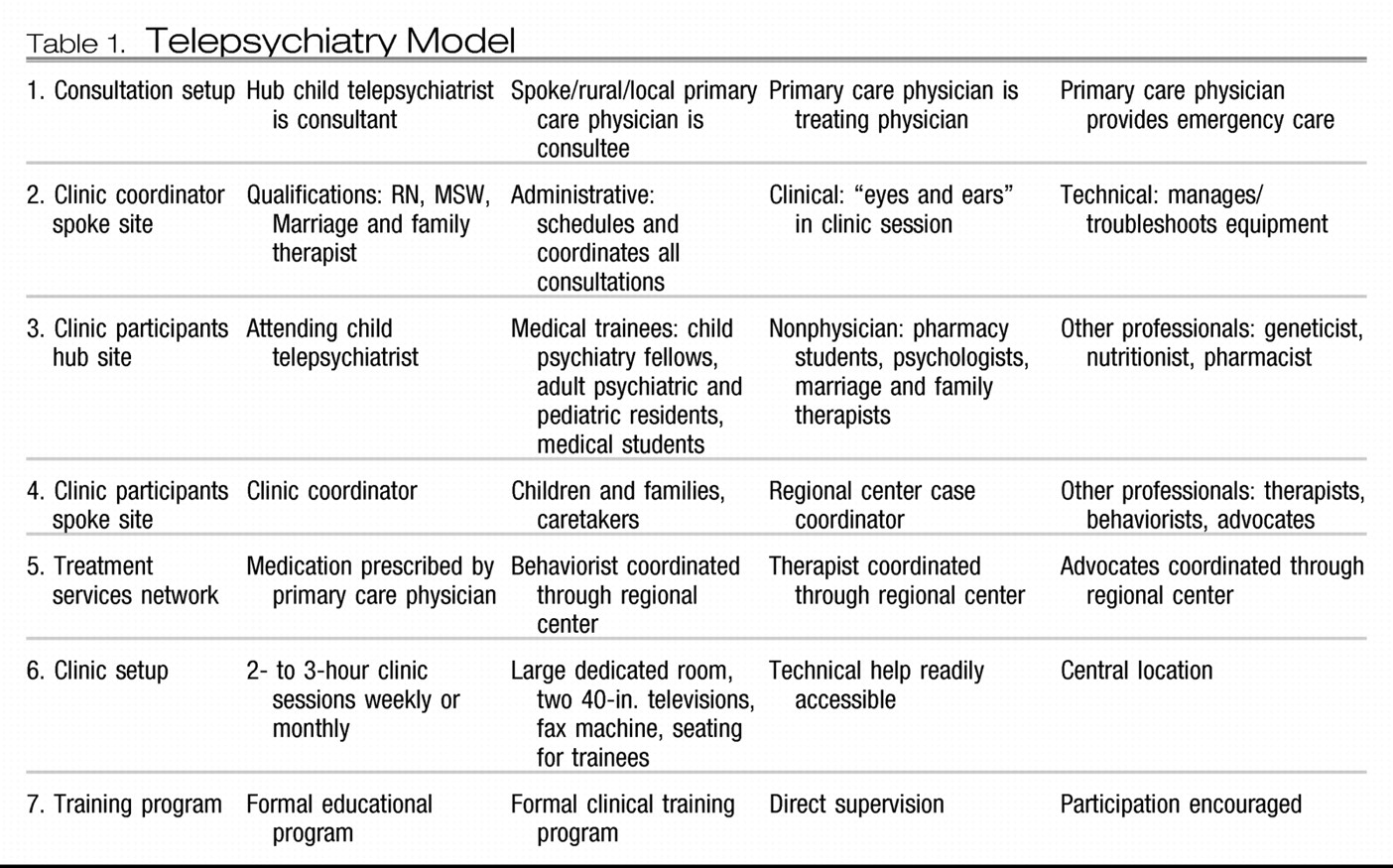
Many telepsychiatry clinics fail or fall short of success. We highlight seven components that are critical for sustainability (
Table 1).
1.
Telepsychiatrists as collaborative consultants to primary care rural doctors. “Hub site” telepsychiatrists work as consultants and do not provide direct care. All treatment is local, including emergency treatment. The primary care doctor, or consultee, is not present during the consultation but will implement treatment recommendations for medications and medical or laboratory tests. He or she may phone the telepsychiatrist with any questions or concerns. The telepsychiatrist continues to consult with the patient virtually while actively monitoring progress in follow-up visits.
2.
Consultation input: Multidisciplinary data provided for each consultation. The “spoke site” clinic coordinator gathers critical information from multiple sources for all clinic visits, starting with the evaluation. Without this information including report cards, individual educational plans (IEPs), laboratory tests, psychological testing, therapist reports, teacher progress notes, and symptom rating scales, the hub child psychiatrist will not have necessary data to evaluate progress.
3.
Interactive multiple participant consultation. This consultation often includes four or five people at both the hub and spoke sites, creating a large treatment team that collaborates with the parent. The clinic coordinator manages the spoke clinic and helps with on-site issues such as escalating behavior. In congruence with the finding of Hilty et al. for patients (
42,
43), we have found that by hearing the process of the treatment team creating a plan helps parents feel more in control and more comfortable with the telepsychiatrist's recommendations. The parents gain insight into the thought process behind decisions and become more informed about their child's treatment and problem.
4.
Consultation outpatient: Treatment network. The telepsychiatrist usually recommends medical, psychopharmacological, behavioral, psychological (for child and family), treatment as well as school and developmental interventions for the child. The spoke site must coordinate with providers who can supply specific services and are willing to work with the clinic.
5.
Teleclinic coordinator with both administrative and clinical roles. The spoke site clinical coordinator must have expertise with technology and clinic administration, participate in clinics, and coordinate follow-up care and triage issues that arise. Because of the limits to what the telepsychiatrist can see, the coordinator is the in-session eyes and ears, observing the patient and actively directing the psychiatrist to things he or she cannot observe directly.
6.
Clinic setup. Clinics must occur in structured blocks of at least 2 hours.
7.
Education: training of professionals. Trainees can attend telepsychiatry clinics with less intrusion than families would experience in a face-to-face consultation. Trainees can participate easily and actively learn from direct rather than “after the fact” supervision.
CONCLUSION
Child telepsychiatry needs empirical psychometrically sound research studies, well-developed clinic protocols, and a collaborative consultation treatment model for future growth. Psychiatric consultation using telepsychiatry, as described in our model, is different from the traditional medical model of psychiatric treatment. Teleclinics create a new clinic team involving a coordinator who participates directly in the clinics and an off-site local primary care doctor. These clinics require greater parent involvement and education. They require greater overall structure for success. The rural primary care doctors enjoy the opportunity to broaden their ability to use psychiatric medications and to see their patients improve. The clinics provide an excellent opportunity for psychiatric training. The telepsychiatrists find this multidimensional clinic interesting and stimulating, providing an opportunity to see patients rarely seen in local clinics. Because of the lack of adequate diagnosis before consultation, cases can have added complexity. From our telepsychiatry chart review, we found that more than half of the new patients seen had incorrect diagnoses and medications but the conditions of these patients improved after they were seen in our clinic. We have experienced an extremely high treatment compliance rate and a low no-show rate, compared with face-to-face consultations, which we believe results from the strengths of our model.
RESEARCH
Child telepsychiatry has not kept pace with the general field of child psychiatry for which there has been a large increase in reliable standardized methodologies for assessment and characterization of mental and emotional disorders. Scientific standards including randomized controlled studies that incorporate test-retest and inter-rater reliability must be adopted (
39). In addition, studies need to be longitudinal and have larger subject pools that focus on the impact of telepsychiatry on different diagnoses, treatment, and specific outcomes. This information will show us which disorders can best be treated and what treatment methodologies can be used in telepsychiatry. Also, research can further help us identify the important differences between face-to-face versus telepsychiatric psychiatric consultations.
STANDARDS FOR TELEPSYCHIATRY
The quality of care of telepsychiatry should compare to that for face-to-face consultations with the high standard of conventional child and adolescent psychiatry practice as the optimal reference point in the field (
44). Psychiatry needs to establish its own telepsychiatry protocols. Standards will help address issues of liability and emergency care, which are particularly important in this area. Only with an appropriate and sound clinical child telepsychiatry set up can the optimal care be provided as a base for high-quality research.
CLINICAL CARE
Telepsychiatry can extend the reach of urban child psychiatrists to the rural youth in need by providing evaluations and follow-up consultations. The combination of treating, training, and teaching, which is our clinic mission, will help child telepsychiatry reach its greatest potential.