During the past decade or so, the case has been building that eating fish, or a diet rich in omega-three fatty acids, can help ward off Alzheimer's disease.
Now the argument is being bolstered by results from a new study. Seniors with a higher level of a particular omega-three fatty acid in their blood—docosahexaenoic acid (DHA)—were found to be less susceptible to Alzheimer's and other forms of dementia than were seniors with lower levels of DHA in their blood.
The study was headed by Ernst Schaefer, M.D., director of the Lipid Metabolism Laboratory of the Jean Mayer USDA Human Nutrition Research Center on Aging at Tufts University. Results were published in the November 2006, Archives of Neurology.
Schaefer and his team wrote, “To our knowledge, our study is the first prospective analysis to assess the predictive value of plasma....DHA content in the occurrence of dementia and [Alzheimer's] disease.”
The researchers measured the level of the omega-three fatty acids in the blood of 899 seniors, who were on average 76 years old and free of Alzheimer's or other types of dementia. They were followed for a mean of nine years to see whether they developed dementia. Ninety-nine new cases of dementia, 71 of which were Alzheimer's, were diagnosed in the followup period. The researchers then investigated whether there was any connection between the amount of omega-three fatty acids in the blood of the subjects at the start of the study and their later risk of developing dementia, taking possibly confounding factors such as age, gender, education, and the apolipoprotein E e4 variant into consideration.
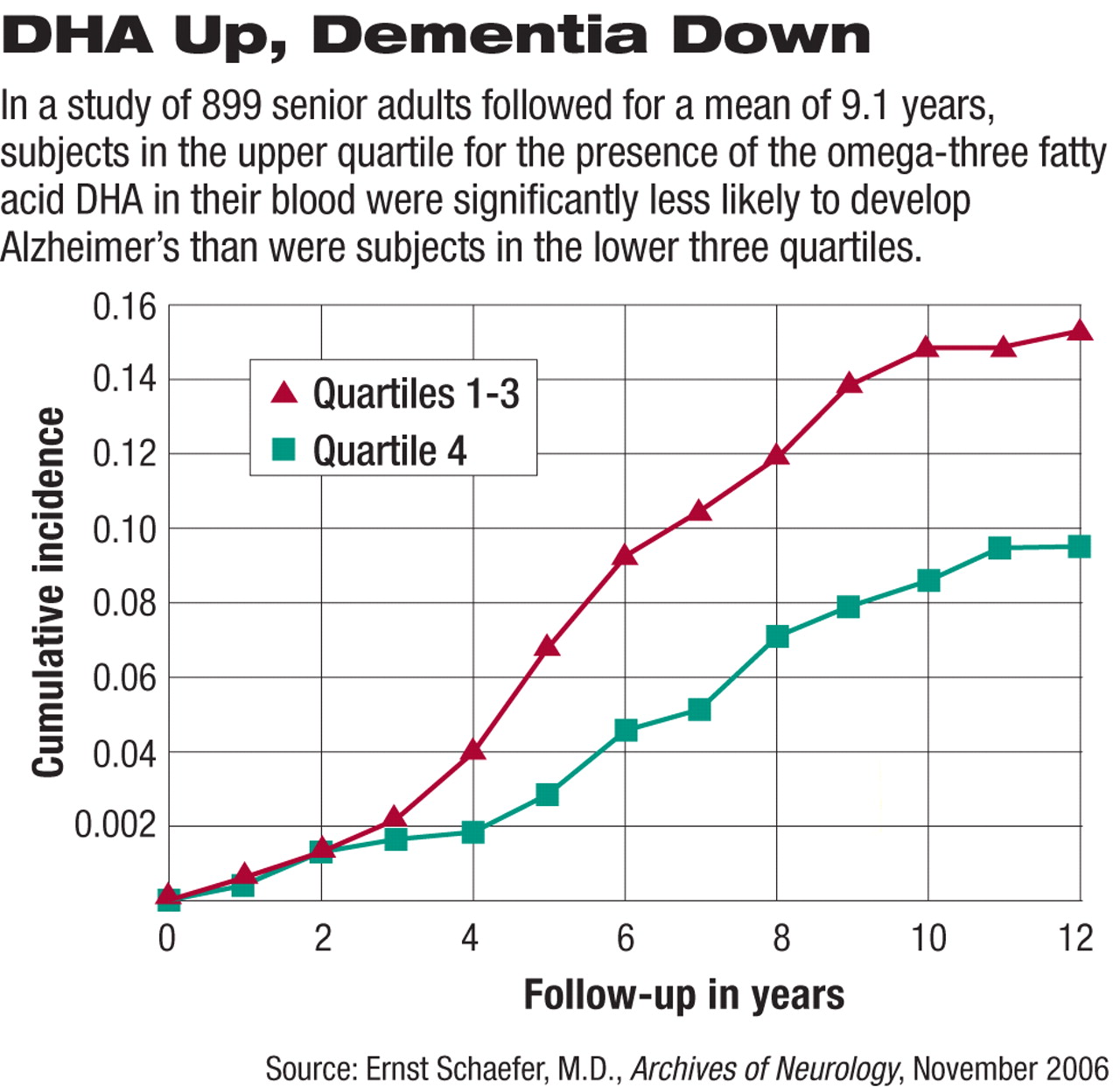
Schaefer and his group found a link between only one omega-three fatty acid—DHA—and the risk of developing dementia. The subjects whose blood levels of DHA were in the top quartile at the start of the study experienced a significant 47 percent lower risk of developing dementia by the end of the study than did those subjects whose blood levels of DHA were in the lower three quartiles at baseline. Moreover, dietary information from 488 of the subjects revealed that those persons whose DHA levels constituted the top quartile ate, on average, three servings of fish a week.
Although DHA must be obtained through the diet, its content is fairly consistent across all types of fish, Martha Clare Morris, Sc.D., pointed out in an accompanying editorial. Morris is an associate professor at Rush University's Institute for Healthy Aging and an authority on the subject. This is not the case for the omega-three fatty acid eicosapentaenoic acid (EPA), she added, which has been fairly well established to prevent cardiac death and which is found mostly in cold-water fatty fish.
Further, a person might be able to eat fewer than three servings of fish a week and still receive protection from Alzheimer's, she said, because in previous epidemiological studies, the protective effect was observed in persons who ate fish once a week versus those who rarely or never ate fish.
Morris emphasized, however, that some crucial questions about fish and DHA's ability to protect people from Alzheimer's still need to be answered. For instance, would taking DHA supplements work as well as eating fish? And does the Alzheimer's protection offered by fish outweigh any deleterious effects that mercury in fish might pose? The only way to answer this question, she said, is to “examine, directly in humans, mercury intake from fish and its effects on various health outcomes relative to the beneficial effects of the omega-three fatty acids consumed.”
The study was funded by the National Institutes of Health, the U.S. Department of Agriculture Research Service at the University of Connecticut, Martek Biosciences Corporation, and Pfizer.

