High rates of cigarette smoking (
2,
3,
15,
16,
17 ), alcohol and illicit drug abuse (
11 ), and poor diet and lack of exercise (
18 ) in this population may contribute to increased rates of cardiopulmonary (
3,
11,
12,
19,
20 ), metabolic (
2,
3,
11,
12,
16,
21 ), and gastrointestinal (
12,
22 ) diseases. Poor hygiene, use of injection drugs (
23 ), and engagement in high-risk sexual behavior (
24,
25 ) among individuals with schizophrenia are associated with higher risk of gastrointestinal, blood-borne, and sexually transmitted infectious diseases, including hepatitis (
2,
3,
26,
27 ) and HIV (
2,
3,
12,
27 ).
Compared with the general U.S. population, individuals with schizophrenia more often face homelessness (
28,
29,
30 ), substandard living conditions (
31 ), and lack of access to medical care and are less likely to receive general medical check-ups (
32 ). Psychotropic medications that help alleviate symptoms of schizophrenia and improve overall disease prognosis may have significant side effects, including extrapyramidal symptoms and tardive dyskinesia, weight gain, obesity, hyperglycemia and diabetes (
33,
34 ), and cardiovascular disease (
34 ). The association of schizophrenia with some general medical conditions, such as metabolic syndrome (
35 ) and type II diabetes (
36,
37 ), after analyses control for other factors, may indicate shared etiopathogenic pathways.
Virtually all existing studies of comorbid disorders in schizophrenia test hypotheses and focus on a single condition. To our knowledge no systematic analysis of disorders comorbid with schizophrenia has been conducted in the U.S. hospitalized population. In addition, most previous studies have relied on relatively small and nonrepresentative samples. To overcome such limitations and seek new information about poorly examined comorbid conditions, we used National Hospital Discharge Survey (NHDS) data to conduct a systematic analysis of the occurrence of more than one ICD-9 code in the discharge records of hospitalizations for schizophrenia and hospitalizations for other reasons. Demographic characteristics of hospitalized patients with schizophrenia and the proportion of total discharges of patients with schizophrenia over time were also explored.
Results
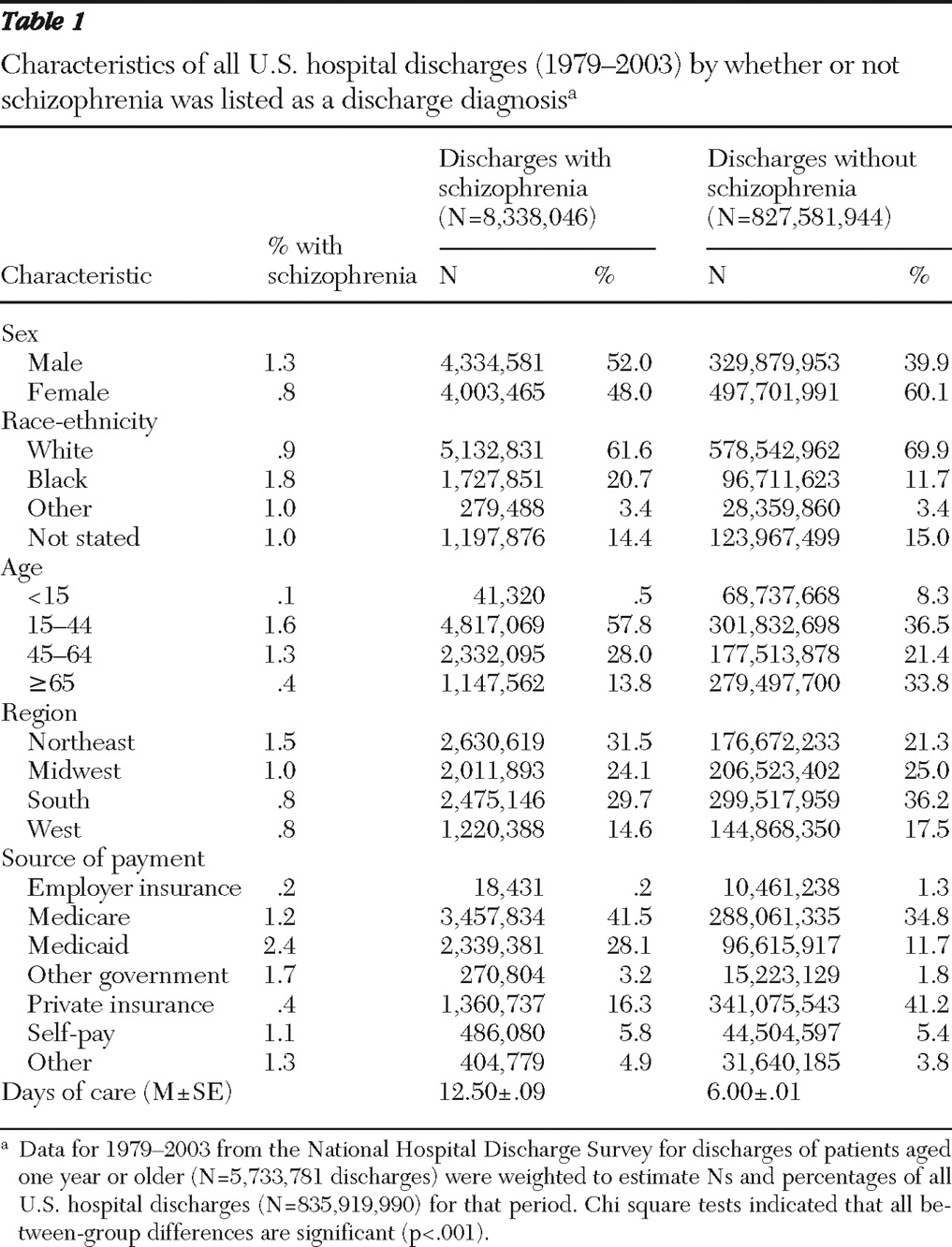
Table 1 presents demographic information from the records of patients with and without a diagnosis of schizophrenia weighted to reflect all U.S. hospital discharges. The overall proportion of discharges with schizophrenia as a diagnosis (not necessarily the primary diagnosis) was 1.0%, and the proportion varied significantly (p<.001) by demographic group. The proportion with schizophrenia was higher among males (1.3%) than females (.8%) and among blacks (1.8%) than whites (.9%) or the "other" racial-ethnic group (1.0%). The proportion was highest among the group aged 15 to 44 (1.6%), followed by the group aged 45 to 64 (1.3%). It was also highest among discharges in the Northeast region (1.5%). The proportion of discharges with schizophrenia was highest among those with Medicaid as source of payment (2.4%), followed by other government funding (1.7%), other sources of payment (1.3%), and Medicare (1.2%).
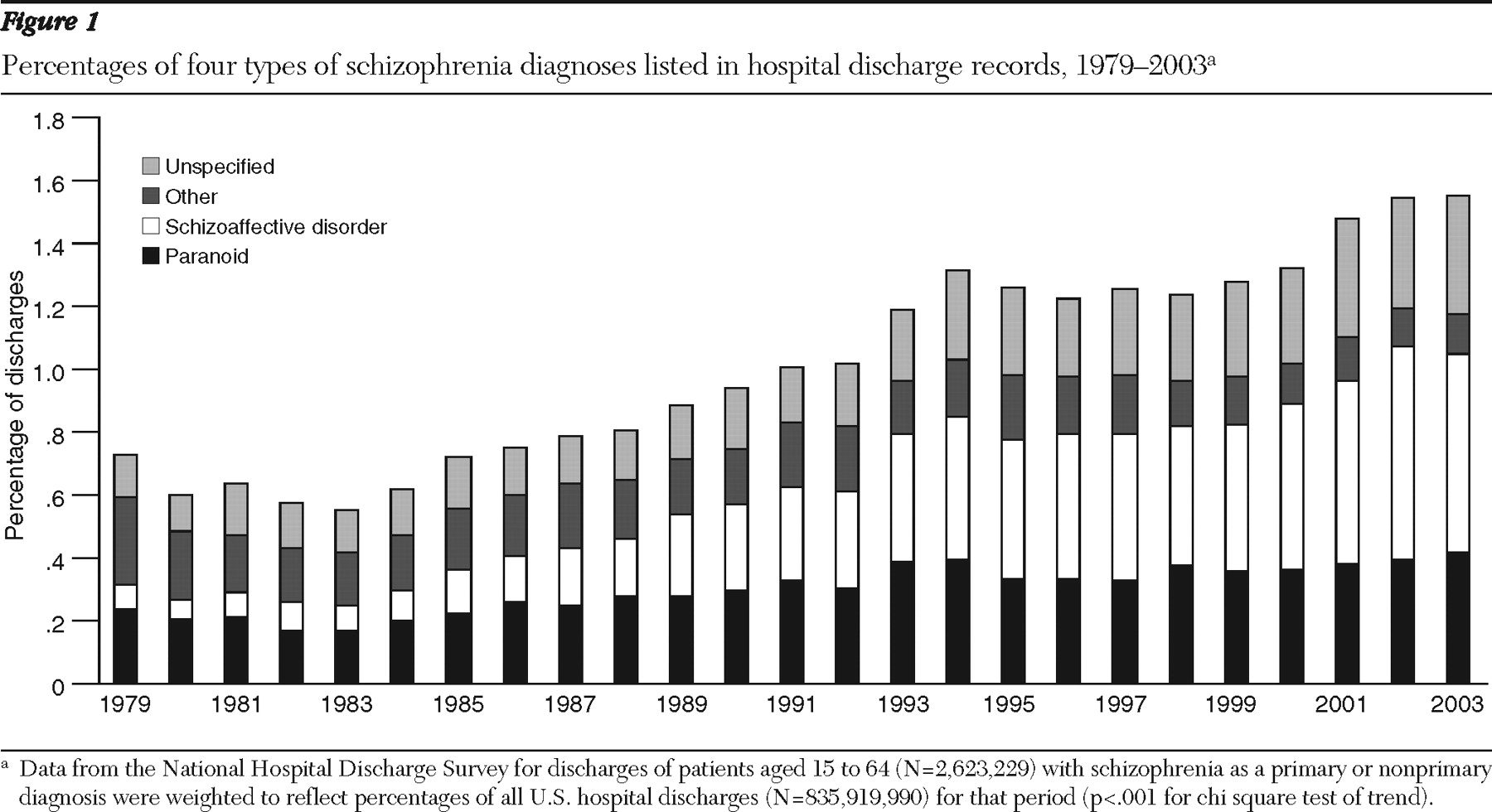
As shown in
Figure 1, the proportion of discharges with any diagnosis of schizophrenia (primary or nonprimary) increased significantly over time (p<.001). The trend in discharges with paranoid schizophrenia, schizoaffective disorder, and schizophrenia not otherwise specified was significant among both males and females (p<.001) (data not shown). Among males the trend was mostly attributable to increases in schizoaffective disorder and paranoid schizophrenia, whereas among females it was primarily attributable to an increase in schizoaffective disorder. In the early 1980s schizoaffective disorder was the least prevalent type among males and females. Starting in the late 1980s it became the most prevalent type among males. This trend was evident among females starting in early 1990s.
The mean±SE length of hospital stay for discharges with any diagnosis of schizophrenia over the study period was 12.50±.09 days, compared with 6.00±.01 days for discharges without schizophrenia. The mean length of hospital stay for all discharges with schizophrenia decreased significantly (p<.001) from 15.81±.51 days in 1979 to 9.92±.37 in 2003. There was also a significant but less substantial decline in the length of stay among discharges without schizophrenia, from 7.19±.02 days in 1979 to 4.82±.02 days in 2003 (p<.001).
The median number of comorbid conditions for discharges with and without any diagnosis of schizophrenia was two among all hospitalizations (aged 15 to 64) and three for discharges restricted to those with two or more
ICD-9 codes. Among 55,292 discharge records that listed a diagnosis of schizophrenia, most (75%, N=41,587) listed it as the primary diagnosis (that is, in the first position), including 26,279 records with at least one comorbid condition.
Table 2 presents data on the number of conditions and proportional morbidity for the 20 most prevalent (>2%) comorbid conditions for the two discharge groups. Psychiatric and behavior-related diagnoses accounted for 45% of comorbid diagnostic categories among schizophrenia discharges, compared with 15% among other discharges.
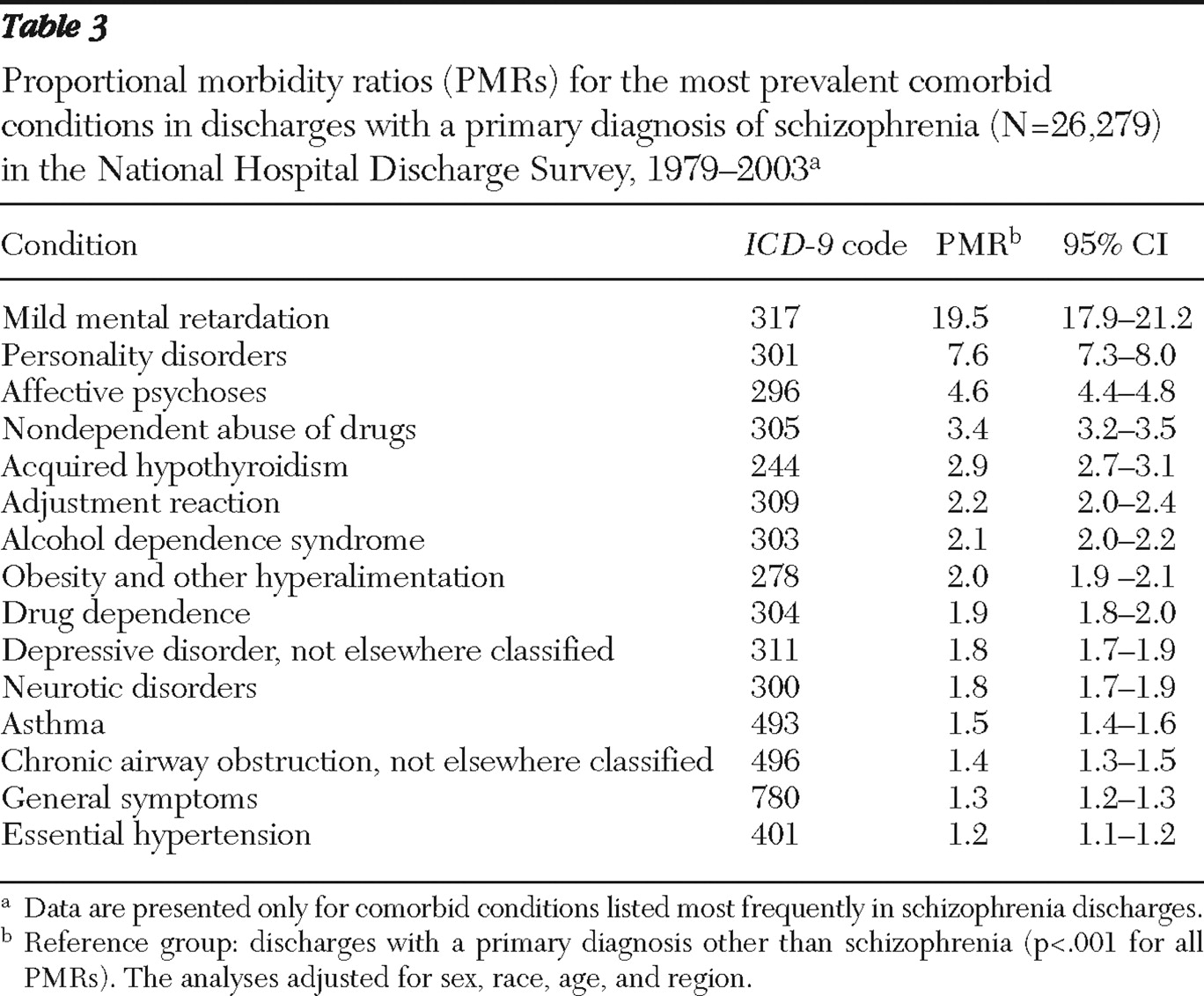
As shown in
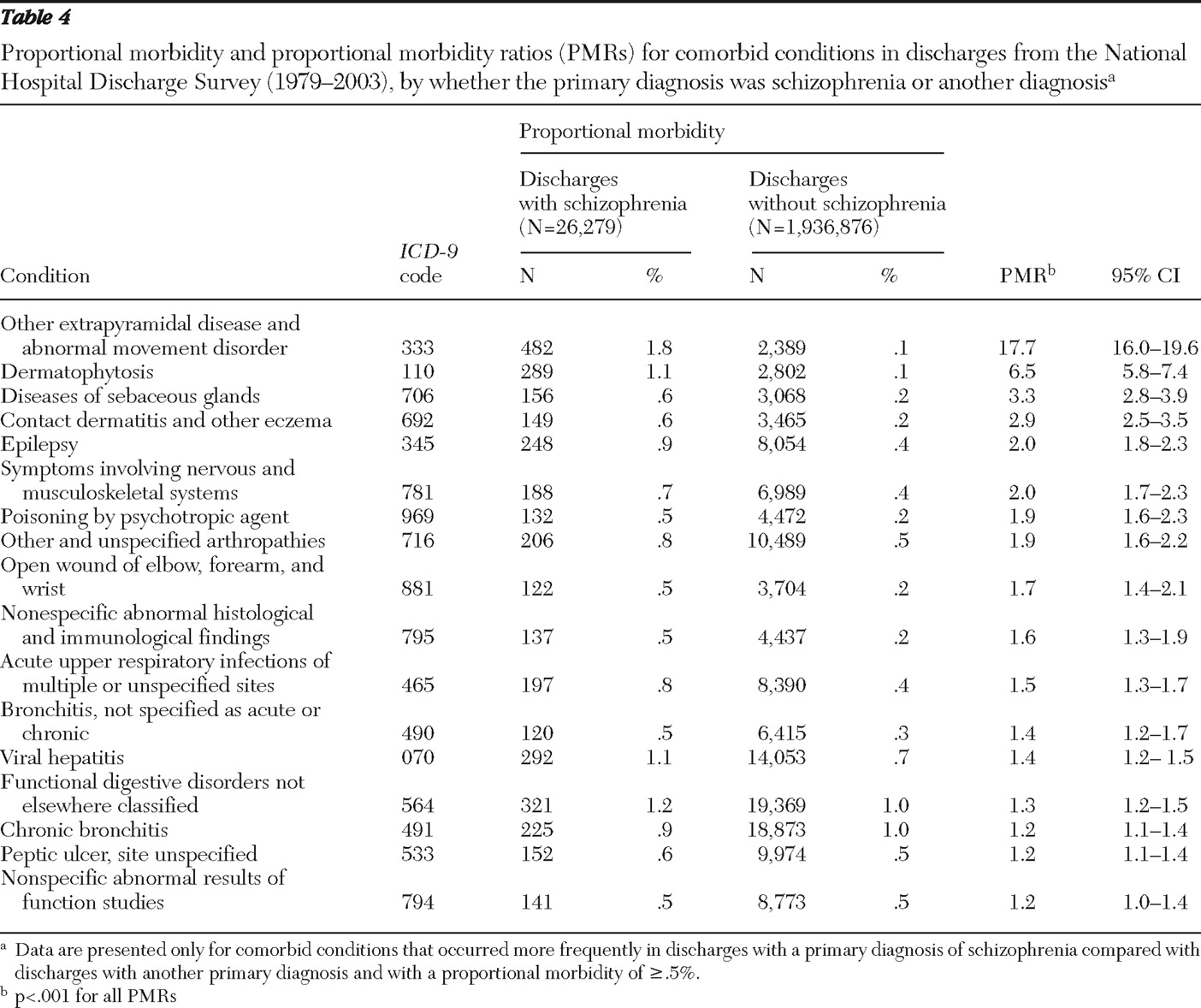
Table 3, the proportion of discharges with comorbid mental disorders was much higher among discharges with a primary diagnosis of schizophrenia, including mild mental retardation (PMR=19.5), personality disorders (PMR=7.6), affective psychoses (PMR=4.6), nondependent abuse of drugs (PMR=3.4), adjustment reaction (PMR=2.2), alcohol dependence (PMR=2.1), drug dependence (PMR=1.9), depressive disorder not elsewhere classified (PMR=1.8), and neurotic disorders (PMR=1.8). In addition, discharge records with schizophrenia as the primary diagnosis were significantly more likely (p<.05) to list the following nonpsychiatric comorbid conditions with a proportional morbidity of more than 2%: acquired hypothyroidism (PMR=2.9), obesity and other hyperalimentation (PMR=2.0), asthma (PMR=1.5), chronic airway obstruction not elsewhere classified (PMR=1.4), essential hypertension (PMR=1.2), and diabetes type II (PMR=1.2). Proportional morbidity of diabetes type II was 6.7% for discharges with schizophrenia and 7.3% for those without schizophrenia (PMR=1.2, 95% confidence interval [CI]=1.2–1.3, p<.001) (data not shown). Discharge records with a primary diagnosis of schizophrenia were also significantly more likely (p<.005) to list other less prevalent (.5%–2%) comorbid nonpsychiatric conditions (
Table 4 ). Other extrapyramidal symptoms and abnormal movement disorder was present among 1.8% of discharges with schizophrenia, and poisoning by a psychotropic agent was present among .5%, compared with .1% and .2%, respectively, among discharges without schizophrenia.
Discussion
Consistent with previous findings, the proportion of hospital discharges that included any diagnosis of schizophrenia was higher among males than among females (
39,
40 ), among blacks than among other racial-ethnic groups (
41,
42 ), and in discharges in the Northeast—the area with higher urbanicity—compared with other U.S. regions (
39,
43,
44 ). The increase in the proportion of discharges with schizophrenia over the study period could be partly explained by changes in diagnostic criteria. The concept of schizophrenia was very narrow in
DSM-III (1980) (
45,
46,
47 ) and even narrower in
DSM-III-R (1987) (
45,
47,
48 ), and thus the proportion of discharges with schizophrenia declined over that period. As criteria progressively broadened in
DSM-IV (1994) and
DSM-IV-TR (2000), the proportion increased. However,
DSM-IV criteria were introduced cautiously to avoid an increase in the epidemiological base rate of schizophrenia so that prevalence estimates would not change substantially (
47 ). In fact, high diagnostic agreement was found between
DSM-III-R and
DSM-IV (
49 ).
Changes in criteria from
DSM-III through
DSM-IV-TR also likely contributed to the increase in the proportion of discharges with schizoaffective disorder (
46 ). In addition, there has been considerable controversy about the stability and usefulness of the diagnosis of schizoaffective disorder since it was introduced in 1933 (
50,
51,
52 ). In our study we used a very broad case definition that included schizophrenia disorders listed in the
ICD-9 classification instead of using the
DSM-IV-TR definition of schizophrenia. We did this in order to overcome uncertainties in regard to the diagnosis of schizoaffective disorder and to capture fluctuations in the population of cases that were artifacts of changes in
DSM definitions of schizophrenia and schizoaffective disorder.
The high prevalence rates of comorbid psychiatric conditions, such as mild mental retardation (PMR=19.5) and personality disorders (PMR=7.6), among discharges with a primary diagnosis of schizophrenia is in accordance with the multiaxial assessment system. As noted in
DSM-IV-TR, the multiaxial system is used for psychiatric assessments to facilitate comprehensive and systematic evaluation with attention to various mental disorders and general medical conditions. Use of the multiaxial system could at least partly explain the much higher prevalence of psychiatric conditions among discharges with a primary diagnosis of schizophrenia. Consistent with previous findings (
53,
54,
55,
56,
57,
58,
59,
60 ), this study found a higher proportion of alcohol dependence (PMR=2.1), drug dependence (PMR=1.9), nondependent abuse of drugs (PMR=3.4), and psychiatric comorbid conditions including depressive symptoms (PMR=4.6 and 1.8) among discharges with schizophrenia.
Of the nonpsychiatric comorbid conditions, acquired hypothyroidism was nearly three times more prevalent among discharges with a primary diagnosis of schizophrenia. This finding is in line with those of previous studies (
2,
6,
61 ) and case reports (
62,
63 ), but reasons for this association remain unclear.
The observed increase in metabolic disorders among discharges with schizophrenia is also consistent with previous reports (
2,
3,
11,
12,
16,
21,
37,
64 ). Obesity and other hyperalimentation were observed more frequently among discharges with schizophrenia. From 1979 through 1983 the likelihood of comorbid obesity was not significantly different between discharges with and without a primary diagnosis of schizophrenia, but in 1984–1988 the PMR rose to 1.5 (CI=1.3–1.9) and in subsequent years the average PMR was 2.0 (CI=1.9–2.1). A less substantial increase was found for diabetes mellitus type II (PMR=1.2) among discharges with schizophrenia. This increase was driven only by the difference in 1998–2003. The temporal increase in obesity and diabetes type II among discharges with schizophrenia might reflect increased use of some second-generation antipsychotic medications (
65 ).
Certain second-generation psychotropic agents can increase levels of triglycerides and low-density lipoprotein cholesterol and decrease high-density lipoprotein cholesterol (
14,
65,
66 ). However, we did not find an increase in these conditions among discharges with schizophrenia, probably for at least two reasons. First, the
ICD-9 codes lack specificity to capture dyslipidemia. Second, screening for and treatment of dyslipidemia are reported to be lower among psychiatric patients than among patients without psychiatric disorders (
14,
67 ).
Chronic obstructive pulmonary diseases were prevalent in a larger proportion of discharges with schizophrenia, specifically asthma (PMR=1.5), chronic airway obstruction not elsewhere classified (PMR=1.4), and chronic bronchitis (PMR=1.2). The prevalence of tobacco use disorder (
ICD-9 305.1) was 1.6 times higher (CI=1.5–1.7) among discharges with schizophrenia. These results are consistent with other findings of a high prevalence of smoking among persons with schizophrenia (
7,
56,
64 ). When tobacco use disorder was added to the multivariable models, the PMR for chronic obstructive pulmonary diseases did not change substantially, which is consistent with recent findings (
68 ).
It is of interest that epilepsy was twice as prevalent among discharges with schizophrenia. This association has no clear pathogenic mechanism and has been reported in only a few previous studies (
6,
64,
69 ).
Among discharges with a primary diagnosis of schizophrenia, we also found PMRs of 6.5 for dermatophytosis, 3.3 for diseases of sebaceous glands, and 2.9 for contact dermatitis and other eczema. Although the associations between these conditions and schizophrenia are largely unexplored, some supportive findings exist in the literature (
2,
70,
71 ). Also consistent with previous findings (
6,
26,
27 ), the prevalence of viral hepatitis was higher (PMR=1.4) among discharges with schizophrenia.
Higher rates of general medical conditions among persons with schizophrenia may be attributable to unhealthy behaviors, low socioeconomic status, and side effects of psychotropic medications. Poor socioeconomic status in itself can reduce access to medical care and increase exposure to unhealthy behaviors and lifestyles. In addition, schizophrenia may share etiopathogenic pathways with some other medical conditions.
This study may have underestimated PMRs for a few reasons. Records selected for comorbidity analyses had schizophrenia as a primary diagnosis, and the patients were presumably attended by psychiatrists. Mental health was most likely the major focus of diagnostic and treatment procedures for these hospitalizations. Therefore, the likelihood that these individuals were routinely screened for a variety of non-life-threatening medical conditions is probably lower than for those who were admitted with a primary diagnosis of a general medical condition. Consistent with this assumption is our finding of a higher prevalence of a few poorly specified conditions and disorders among discharges with schizophrenia. In addition, patients with schizophrenia are much less likely to be aware of their general medical problems and to communicate with health care providers about them (
58 ), which makes it more likely that these problems were not evaluated during primarily psychiatric hospitalizations.
Our study has several strengths. We have described comorbidity among hospital discharge records in a large nationally representative database. This unique and robust data source has been relatively neglected in previous psychiatric research. We systematically determined the most prevalent comorbid conditions for hospitalizations with a primary diagnosis of schizophrenia and for those with any other primary diagnosis and examined temporal trends in the diagnostic coding of schizophrenia types and length of hospitalization over a 25-year period. The multiyear data set was used to standardize variables across years and decrease year-to-year variability. The analysis of proportional morbidity was adjusted for sex, race, age, and geographic region and selectively adjusted for tobacco use disorder.
However, the study has some limitations. First, the observations in these data are hospitalizations, and it is possible that an individual was represented more than once. This is an important confound warranting investigation. If individuals with schizophrenia are more likely to be hospitalized than those without schizophrenia, then the proportional morbidity of schizophrenia among hospital discharges could be overestimated. Also, if individuals with schizophrenia and a comorbid condition have a higher rate of rehospitalization than those with other primary diagnoses and the same comorbid condition, the PMRs for this condition would be biased away from the null. However, because the probability of the same person's being represented in the unweighted data set more than once is low, any such bias would be unlikely to materially change our results or conclusions.
In addition, changes in diagnostic criteria during the study years—particularly the increasing emphasis on listing "comorbid conditions" as part of the diagnosis rather than considering the additional symptoms to be an expression of the primary disorder—could contribute to observations of increasing comorbidity. However, the increase in comorbidity in later study years somewhat compensates for the underestimation of comorbidity in earlier study years, resulting in a realistic median number of comorbid conditions for the overall study population.
Also, our data are cross-sectional. No directionality can be assumed in associations between conditions, and associations do not suggest cause-and-effect relationships. Finally, a database of hospital discharges may disproportionately capture some schizophrenia subpopulations that may have higher rates of hospitalization—for example, individuals with more severe illnesses, those who receive less outpatient care, and those who lack insurance. Thus we cannot extrapolate our findings to the population of nonhospitalized patients with schizophrenia who receive outpatient care in the community, which is presumably much larger but which comprises patients with less severe symptoms.