Increasing evidence suggests that cerebrovascular disease, and especially ischemic disease involving small vessels, may be a factor in the pathogenesis of late-life major depression. Cerebrovascular risk factors are more common in depressed than in nondepressed older persons
(1). Similarly, magnetic resonance imaging (MRI) studies of patients with major depression commonly show signs of ischemic small-vessel disease in the form of signal hyperintensities in the white matter
(2), especially in the deep white matter
(3–
5). These findings have led to the hypothesis that among older persons suffering from major depression, there is a subgroup of individuals who have “vascular depression”
(6–
8). The clinical characteristics of vascular depression are thought to include: 1) the occurrence of a first episode of major depression late in life, 2) the presence of MRI signal hyperintensities in the subcortical white matter (white matter hyperintensities [WMHs]), 3) a loss of motivation or interest, and 4) the presence of cognitive decrements, especially those associated with frontal lobe dysfunction
(6,
7).
Although cerebrovascular disease may be a susceptibility factor or correlate for major depression in elderly persons, whether there is a relationship between cerebrovascular disease and milder depressive symptoms remains to be determined. Major depression per se is not particularly common in community-dwelling elderly persons, but many older individuals do have substantial depressive symptoms
(8,
9) that do not rise to the level of clinical depression. While the absolute number of depressive symptoms and their level of severity may be low in community-dwelling elderly persons, the presence of depressive symptoms in this group has been linked to the subsequent development of major depression
(10). Cerebrovascular disease and its associated neuropathology, as evidenced by WMHs, become more frequent as people grow older
(11), but it is not clear whether this pathology is related to the presence of depressive symptoms in older persons who are
not suffering from major depression. Recent evidence has suggested that cerebrovascular disease risk factors in nondepressed elderly primary care patients are associated with later development of depressive symptoms
(12).
In examining the relationship between cerebrovascular disease and depressive symptoms, it may be important to differentiate various types of symptoms. Patients with vascular depression show low levels of interest and motivation coupled with a high level of cognitive dysfunction and a low level of depressive ideation
(6). A factor analysis of symptoms of depression in a group of community-dwelling elderly persons found two major symptom clusters: 1) a mood disturbance cluster and 2) a motivational disturbance cluster that encompassed loss of energy or interest and difficulty in concentrating and making decisions
(13). If the depressive symptoms found in
nondepressed elderly individuals are the result of vascular disease, then evidence of cerebrovascular disease, such as WMHs, should be more strongly associated with reports of disturbed motivation and concentration than with symptoms of a mood disturbance.
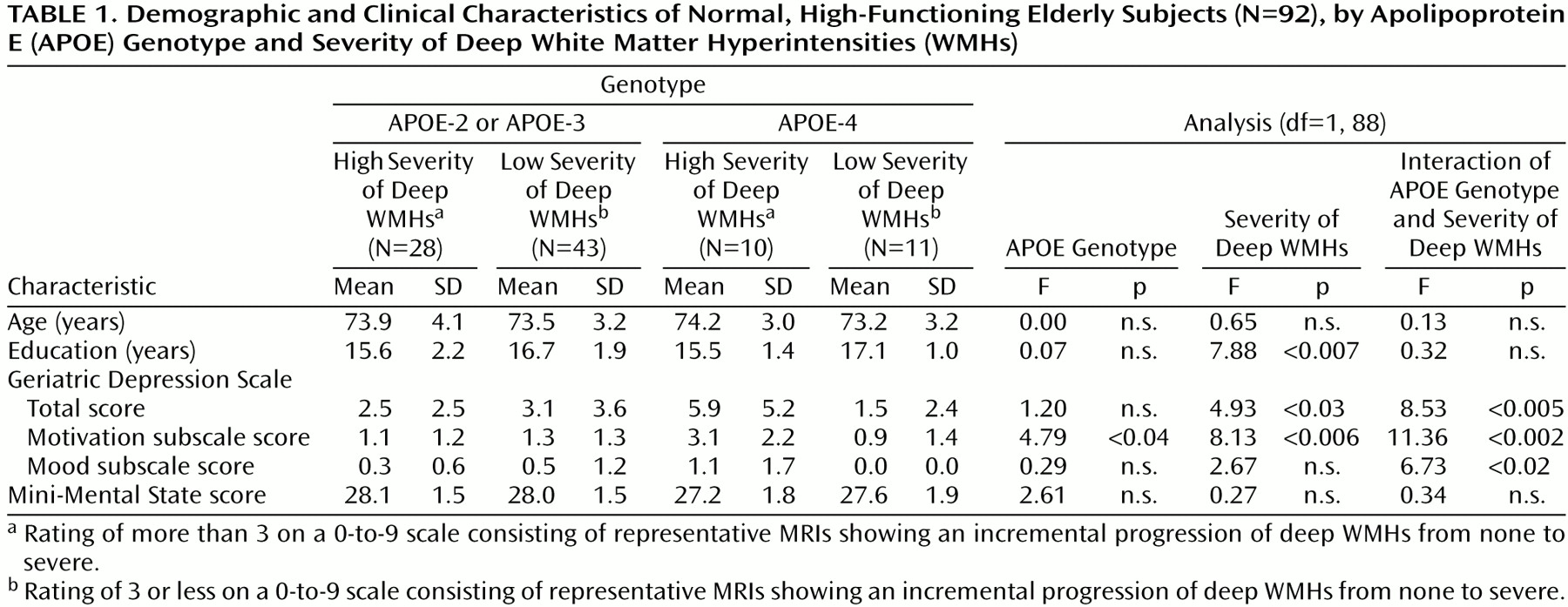
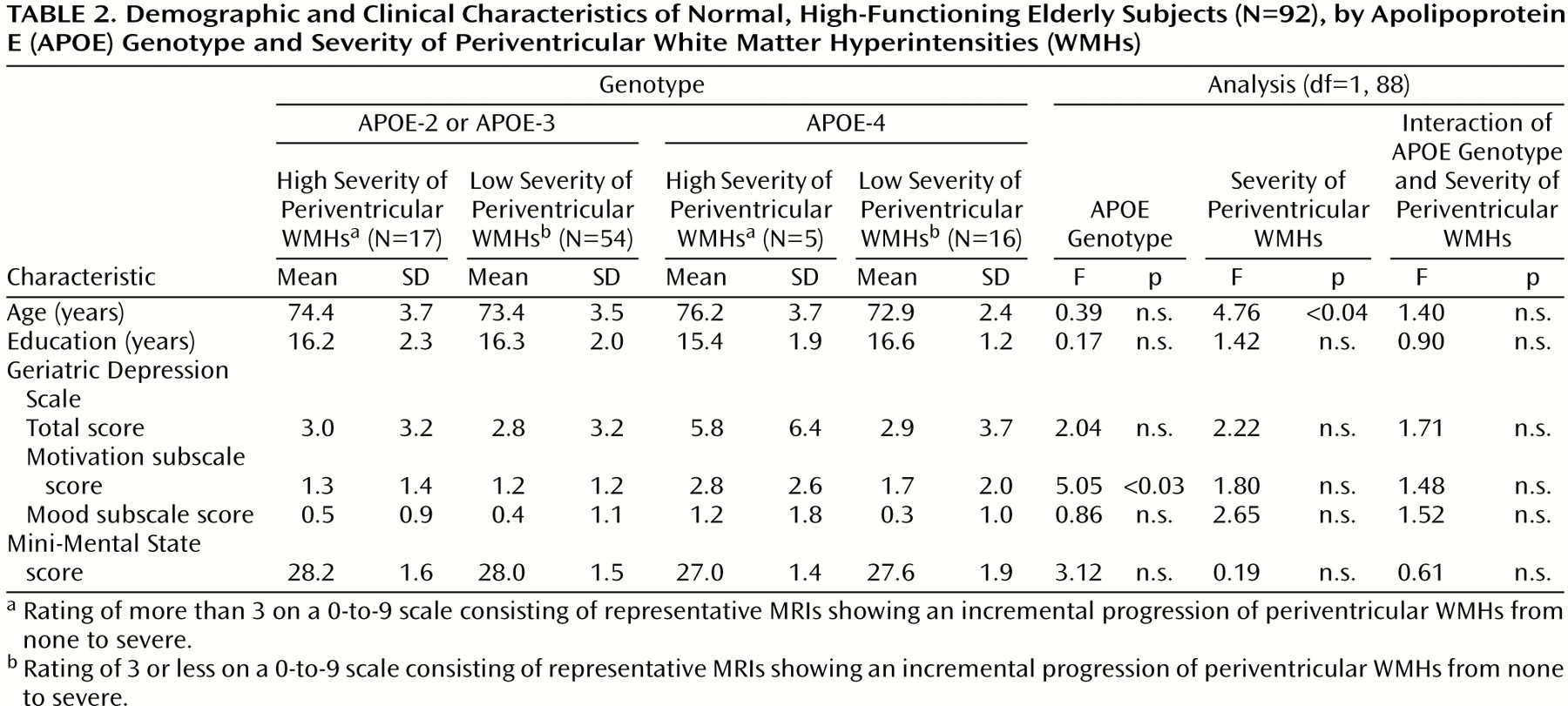
The present study examined whether the presence of WMHs is associated with depressive symptoms in high-functioning community-dwelling elderly persons and whether depressive symptoms in this group are more likely to be related to deep WMHs, as is the case in geriatric major depression
(4,
5), than to periventricular WMHs. The study also examined whether the presence of WMHs was more likely to be related to motivational symptoms than to mood symptoms.
Because ischemic cerebrovascular disease is more common in individuals carrying an apolipoprotein E-4 (APOE-4) allele
(14), we also examined the relationship between depressive symptoms, WMHs, and APOE genotype. APOE-4 carriers with vascular disease are more likely to have WMHs than are noncarriers
(15). APOE genotype and vascular disease have also been shown to have an interactive effect on cognitive performance
(16), with APOE-4 carriers showing more decrements in the presence of vascular disease than do noncarriers. If cerebrovascular disease contributes to the presence of depressive symptoms in elderly persons, then it is possible that APOE genotype interacts with the severity of WMHs and that APOE-4 carriers will show more depressive symptoms than noncarriers.
Method
Subjects
The 92 subjects in this study were recruited from the community and were participants in an ongoing investigation of WMHs in normal aging. This study was approved by the University of Pittsburgh Institutional Review Board. After the entire study was explained to the potential subjects, written informed consent was obtained. Subjects were 66–80 years of age (mean=73.6 years, SD=3.4) and were highly educated (mean=16.3 years of education, SD=2.0). Their mean Mini-Mental State score was 27.9 (SD=1.6). Twelve subjects were African American, and the rest were Caucasian. Exclusion criteria included a history of major head injury, stroke, Alzheimer’s disease, Parkinson’s disease, Huntington’s disease, alcoholism, schizophrenia, or bipolar disorder. We also excluded anyone with a history of depression within the last 5 years. None of the subjects in this study had ever received a diagnosis of major depression. However, three had received antidepressant medication from their primary care physician. One of the three had received fluoxetine as a “precaution” after retirement, the second was taking paroxetine for anxiety, and the third had received an unknown antidepressant for a short time 30 years before the present study.
The subjects were examined by a physician’s assistant from the University of Pittsburgh Alzheimer’s Disease Research Center. Each subject provided a complete history and received a physical examination, including a neurological evaluation, ECG, blood pressure measurement, and laboratory tests to measure serum lipids. APOE genotyping was performed by staff of the Genetics Core (Dr. I. Kamboh) of the Alzheimer’s Disease Research Center.
Assessment of Depressive Symptoms
The subjects completed the Geriatric Depression Scale, a self-rating measure of depressive symptoms designed especially for screening older individuals
(17). It consists of 30 yes/no questions (e.g., “Do you often feel downhearted and blue?”). Besides the questions about mood, the Geriatric Depression Scale includes questions about cognitive decrements that often co-occur with depression in older persons, such as problems in making decisions or in concentrating. The scale has a high test-retest reliability (0.85) and has been widely used as a screening measure for depressive symptoms in community-dwelling elderly persons. The Geriatric Depression Scale differs substantially from the depression scale for which a factor analysis by Forsell et al.
(13) found separate clusters of mood and motivational symptoms. However, similar clusters of mood and motivational symptoms emerged in a factor analysis of Geriatric Depression Scale data from more than 300 community-dwelling elderly subjects
(18). The mood symptom factor, which consisted of nine Geriatric Depression Scale items (items 6, 8, 10, 13, 16, 18, 22, 23, and 25), reflected the presence of a sad mood. The motivational symptom factor consisted of six items (items 2, 20, 21, 26, 29, and 30) and identified a loss of motivation or energy and difficulty in concentrating and making decisions. In the study reported here, we used the two groups of items associated with these factors as separate subscales for mood and motivation symptoms.
MRI Acquisition
MRI scans were acquired with a 1.5-T Signa scanner (GE Medical Systems, Milwaukee). The following axial series oriented parallel to the plane connecting the anterior and posterior commissures were obtained: T1-weighted (TR/TE=500/11; 1 excitation); fast spin-echo T2-weighted (TR/TE=2500/111 effective; 1 excitation); fast spin-echo proton-density-weighted (TR/TE=2200/17 effective; 1 excitation); fast fluid-attenuated inversion recovery (TR/TE=9002/56 effective; TI=2200; 1 excitation). The section thickness was 5 mm with a 1-mm intersection gap. All axial sequences were obtained with a 24-cm field of view and a 192 × 256 pixel matrix.
White Matter Ratings
Two neuroradiologists (M.B.F., R.L.W.) independently evaluated WMHs on the fluid-attenuated inversion recovery images. Separate ratings were made for hyperintensities in the periventricular white matter (those in contact with the ventricles) and hyperintensities in the deep white matter (those not in contact with the ventricles). The ratings were based on a system developed for the Cardiovascular Health Study
(19,
20), which gave only one rating for all WMHs. Our examination of the rating standards used in the Cardiovascular Health Study suggested that most of the variability in the mild to moderately severe ratings reflected differences in the severity of periventricular WMHs. Therefore, we used the original Cardiovascular Health Study rating standards as our measure of periventricular WMHs, and we devised a comparable scale to evaluate hyperintensities in the deep white matter.
Rating of periventricular WMHs
A numerical rating for periventricular WMH burden was assigned by comparing each subject’s imaging data to predefined Cardiovascular Health Study visual standards that represent progressive severity with a 10-point scale (0 through 9). If the two independent raters differed in their rating by one point, the final rating was the mean of the two values. A greater than 1-point difference between raters was considered a disagreement and was adjudicated by consensus. The percentage of interrater disagreement for the ratings of the periventricular WMHs in this study was 8.7%. We also had ratings of periventricular WMHs from T
2-weighted and proton-density-weighted images for 91 of the 92 subjects. Since the original Cardiovascular Health Study rating scheme was designed to examine T
2-weighted and proton-density-weighted images, we compared each subjects’ rating for the fluid-attenuated inversion recovery image with the rating for the T
2-weighted and proton-density-weighted images. We used intraclass correlations to examine interrater reliability on the periventricular WMH ratings for the T
2-weighted and proton-density-weighted images and for the fluid-attenuated inversion recovery images. The two intraclass correlations were almost identical (0.81 versus 0.83). The ratings of the periventricular WMHs in the T
2-weighted and proton-density-weighted images and the fluid-attenuated inversion recovery images were very highly correlated (r=0.91, df=89, p<0.0001). The mean ratings of the fluid-attenuated inversion recovery images was significantly higher than the mean ratings of the T
2-weighted and proton-density-weighted images (mean=2.6, SD=1.5 versus mean=2.2, SD=1.5; t=4.93, df=91, p<0.0001), as would be expected, since the former type of scan is more sensitive to the presence of WMHs than the latter type
(21).
Rating of deep WMHs
Hyperintensities in deep white matter were assessed by using a 10-point scale (0 through 9) modeled after the Cardiovascular Health Study scale. The scale for rating deep WMHs was developed by three neuroradiologists (M.B.F., R.L.W., C.C.M.) and consisted of images representative of an incremental progression of deep WMHs from none (score=0) to severe (score=9). Like the Cardiovascular Health Study scale, the scale for rating deep WMHs provided visual standards corresponding to ratings 1 through 8, indicating increasing severity. Where no WMHs were present, a rating of zero was assigned. Where WMHs more severe than the visual standard for the rating of 8 were present, a rating of 9 was assigned. The intraclass correlation for the ratings of deep WMHs was almost identical to that for the ratings of periventricular WMHs (0.84 versus 0.83).
Statistical Analysis
The total Geriatric Depression Scale score, the mood and motivation subscale scores, and demographic measures were analyzed with univariate two-way analyses of variance (ANOVA) testing the main effects of high versus low ratings of deep and periventricular WMHs and the presence of an APOE-4 allele. Interactions between these main effects were also tested. The p values for all test results are two-tailed.
Discussion
The results of this study suggest that WMHs are related to the presence of depressive symptoms even in nondepressed, high-functioning elderly individuals. While the absolute amount of depressive symptoms seen in this group was low, the presence of depressive symptoms was related mainly to the severity of deep WMHs, not periventricular WMHs, a pattern similar to that found in geriatric major depression
(3–
5). The relationship between deep WMHs and major depression has been considered evidence for the existence of a “vascular” form of depression. Also, as in the characterization of vascular depression
(6), the symptoms most strongly related to deep WMHs in the present study were problems in motivation and concentration. Thus, the location of the hyperintensities related to depressive symptoms and the nature of these symptoms is similar in both nondepressed older normal subjects and persons with actual geriatric major depression.
There was a significant interaction effect of APOE genotype and deep WMH severity on the Geriatric Depression Scale total score and on the motivational subscale score. Subjects with severe deep WMHs who also carried an APOE-4 allele reported considerably more depressive symptoms than did non-APOE-4 carriers. The nature of this interaction is similar to that reported by Slooter et al.
(16), who showed that the deleterious effect of WMHs on cognitive performance is greater if subjects also carry an APOE-4 allele. The existence of an interaction between deep WMH severity and APOE genotype is consistent with a role for cerebrovascular disease in producing depressive symptoms, even in nondepressed, high-functioning normal individuals, just as it does in some individuals with geriatric major depression.
Recent studies by Sato et al.
(24) and by Steffens et al.
(25) examined the relation of MRI variables to the presence of depressive symptoms in a large population-based sample (the Cardiovascular Health Study). Neither found any strong evidence for a link between WMHs and depressive symptoms. There are several possible explanations for why the present study found a relationship between WMH severity and depressive symptoms while the two earlier studies did not. First, there were substantial differences in MRI methods. The Cardiovascular Health Study rated WMHs on T
2 images, whereas we used the newer fluid-attenuated inversion recovery technology, which is more sensitive to the presence of white matter pathology
(21). The present study also differentiated between periventricular WMHs and deep WMHs, while the WMH rating scale used by Sato et al. and by Steffens et al. was heavily weighted toward variability in periventricular WMHs, except at the most severe end of the scale. A second area of difference is the method used to measure depression. The Cardiovascular Health Study used a modified version of the Center for Epidemiologic Studies Depression Scale (CES-D Scale), whereas the present study administered the Geriatric Depression Scale. More important, in the present results the strongest relationship between deep WMHs and depressive symptoms involved a subset of items dealing with difficulties in motivation, concentration, and problem solving, and not items dealing with depressed mood. The studies by Sato et al. and Steffens et al. measured depressive symptoms using the total CES-D Scale score and did not distinguish between mood and motivation symptoms. Finally, in the present study, APOE genotype interacted strongly with deep WMH severity, while the effect of APOE genotype was not examined in the two earlier studies.
Why should cerebrovascular disease be related to motivational symptoms in this group of nondepressed elderly subjects? One possibility is that the subjects’ reports of motivational difficulties are signs of a mild depressive state. Depressed individuals tend to assess their own cognitive performance as poor, even when their actual scores are no worse than those of nondepressed persons
(26). Vascular depression is thought to be particularly characterized by a loss of interest and motivation
(6). In this sense, the relation of WMH severity to our subjects’ complaints of problems in motivation and concentration would fit with the concept of vascular depression. Arguing against the view that motivational and concentration complaints are early symptoms of a subclinical depression is the paucity of actual mood symptoms in our subjects; on the mood subscale of the Geriatric Depression Scale, there was little evidence for feelings of sadness or hopelessness. Another possibility is that the frontostriatal dysfunction associated with deep WMHs produces genuine deficits in motivation, concentration, and decision making
(4). If this were the case, subjects’ complaints of impairments in these areas would not necessarily be signs of a mood disturbance, but rather a realistic self-assessment of actual difficulties. The data in the present study do not allow us to differentiate between these two possibilities.
Although we have interpreted the present results as demonstrating a relation between deep WMHs and depressive symptoms, there is an alternative explanation. Some of the individuals with a large amount of deep WMHs could have incipient dementia. Hyperintensities tend to be more common in persons with Alzheimer’s disease than in normal elderly persons
(5), and depressed mood can be an early manifestation of Alzheimer’s disease
(27). Thus, the relation between deep WMHs and depressive symptoms in this study, and especially the interaction of deep WMH severity with an APOE-4 genotype, could reflect the presence of preclinical Alzheimer’s disease among our subjects. While we cannot exclude this possibility, several pieces of evidence argue against it. First, WMHs in Alzheimer’s disease appear to be located predominantly in the periventricular region rather than in the deep white matter, whereas the hyperintensities related to major depression in previous studies
(4,
5) and to depressive symptoms in the present study were predominantly in the deep white matter. Second, in the present study, subjects with a high rating for deep WMH and those with a low rating did not differ in their Mini-Mental State scores. There was also no direct effect of APOE genotype on Mini-Mental State score, nor did APOE genotype interact with the effect of deep WMHs. However, the Mini-Mental State is relatively insensitive to dementia in highly educated subjects, and so the results on this scale do not rule out the possibility that incipient Alzheimer’s disease contributed to the present results. A 3-year follow-up of these subjects is presently under way and will hopefully resolve whether preclinical Alzheimer’s disease played any role in producing depressive symptoms in this study.
Overall, the present results show that in a high-functioning group of nondepressed older individuals, the burden of deep WMHs is related to the total amount of depressive symptoms and more specifically to problems of motivation and concentration. This pattern of results is similar to that found in patients with geriatric major depression and generally supports the possibility of a vascular origin for at least some of the depressive symptoms that are common in older individuals.