Atrial natriuretic peptide is not only synthesized by atrial myocytes
(1) and released into the circulatory system but is also found in the neurons of different brain regions in which specific atrial natriuretic peptide binding sites have been found
(2). Atrial natriuretic peptide is released in patients with panic disorder when panic attacks are experimentally induced
(3). This endocrine response possibly serves as a humoral feedback signal to mute overshooting anxiety. Preclinical data have given further evidence for the anxiolytic activity of atrial natriuretic peptide
(4).
Cholecystokinin tetrapeptide (CCK-4) has enhanced panicogenic activity in patients with panic disorder
(5). As with sodium lactate- and CO
2-induced panic attacks, CCK-4-induced attacks are accompanied by hyperventilation and resemble the pattern of panic symptoms induced by CO
2 administration
(6). Furthermore, CCK-4-induced panic attacks are blocked by antipanic treatment
(7) and can be used to study putative new treatment approaches. Therefore we studied the potential anxiolytic activity of atrial natriuretic peptide in patients with panic disorder during a CCK-4 challenge.
Method
Ten patients (five women and five men, mean age=36.0 years, SD=9.7) with a diagnosis of panic disorder but without a comorbid axis I disorder as assessed with the Structured Clinical Interview for DSM-IV, were studied. The patients had been free of medications for at least 10 days and had undergone thorough medical examinations to rule out other illnesses, drug intake, and lifestyles (with sleep deprivation, changes in the sleep/wake cycle) with effects that could interfere with our study. The protocol was approved by the local ethics committee for human experiments. After complete description of the study to the subjects, written informed consent was obtained.
All subjects were studied from 9:00 a.m. to 1:00 p.m. while lying in a supine position in a soundproof room on a single bed. Each subject received a bolus injection of 25 μg of CCK-4 (Clinalfa, Laufelfingen, Switzerland) dissolved in 10 ml of 0.9% saline solution at 11:00 a.m. In a double-blind, randomized study, 150 μg of atrial natriuretic peptide (Clinalfa, Laufelfingen, Switzerland) or 0.9% saline was administered from 10:40 until 11:10 a.m. (1 ml/min). The infusions were administered on separate days, with at least 2 days between experimental conditions. The Acute Panic Inventory
(8) was administered at 10:40 a.m. (baseline) and 11:05 a.m. by a rater (A.S.) who was blind to the procedure; the maximum intensity of symptoms during the observation period was noted. To further characterize the possible effects of atrial natriuretic peptide, the anxiety subscore (afraid of dying, general fear) and the somatic subscore (palpitations, rapid breathing, nausea) of the Acute Panic Inventory are provided. In order for the rater to make a decision that a panic attack had occurred, an Acute Panic Inventory total score exceeding 20 and an increase of at least 14 points over the preinjection score
(8,
9) were required.
The frequencies of panic attacks during the two treatment conditions were compared by using McNemar’s paired chi-square test. For statistical comparisons of mean Acute Panic Inventory scores and subscores between the saline and atrial natriuretic peptide conditions and between the two time points, a two-factorial multivariate analysis of variance (MANOVA) with a repeated measures design was performed. Treatment and time were the two within-subjects factors, each containing two levels. Hypothesis tests for the main and interaction effects of these factors were based on multivariate criteria, such as Wilks’s lambda and its approximated F value. When significant main or interaction effects were found, univariate F tests were performed in an analysis of variance (ANOVA) to locate the levels of the factor with significant differences in mean Acute Panic Inventory scores and its subscores that fell between the levels of the other factor. The contrasts (group mean differences) were tested for significance with approximated F values. Because of the small group size and a possible order effect, CCK-4-induced changes were normed (divided by the group mean) to their baseline values under each experimental condition. As a nominal level of significance, alpha=0.05 was accepted. To keep the type I error at 0.05 or less, all post hoc tests (tests with contrasts) were performed at a reduced level of significance (with an alpha adjustment according to the Bonferroni procedure).
Results
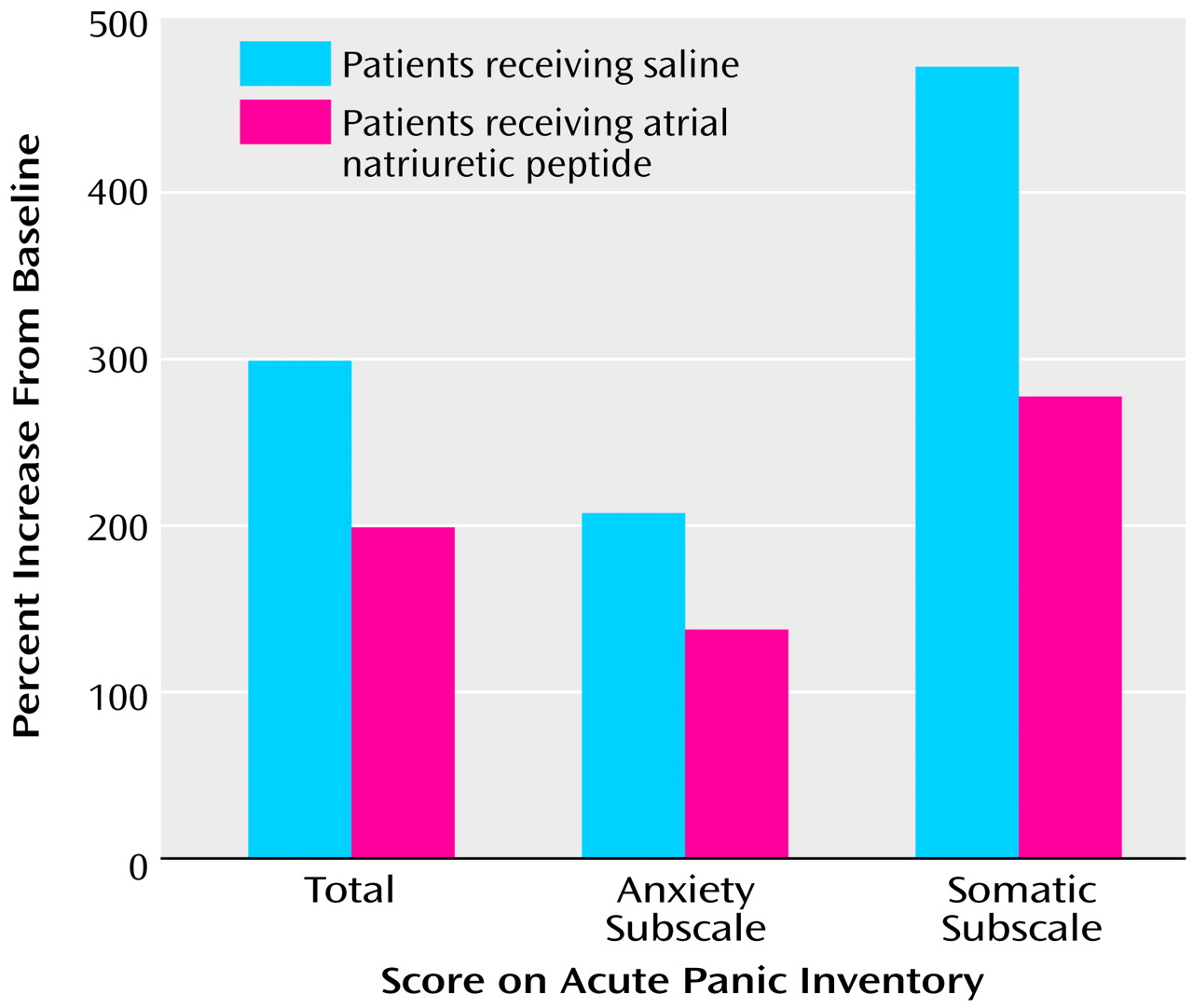
The rate of panic attack was two of 10 in the atrial natriuretic peptide and seven of 10 in the placebo condition. Although coadministration of atrial natriuretic peptide prevented the occurrence of CCK-4-induced panic attacks in five of the seven patients with CCK-4-induced panic attacks, this effect possessed only marginally statistical significance (p=0.06, McNemar’s test). MANOVAs revealed significant main effects of time (F=17.91, df=3, 7, p=0.001) and treatment (F=7.46, df=3, 7, p=0.01) and a significant interaction effect of time and treatment as well (F=8.05, df=3, 7, p=0.01). ANOVAs of Acute Panic Inventory scores yielded significant main effects of time (F=59.48, df=1, 9, p<0.001) and treatment (F=5.93, df=1, 9, p=0.04) and a significant interaction effect of time and treatment as well (F=26.37, df=1, 9, p=0.001). Since the mean Acute Panic Inventory scores before treatment did not differ from the scores after treatment because of norming, we can conclude that CCK-4 increased Acute Panic Inventory scores in both conditions significantly. However, the CCK-4-induced increase in the Acute Panic Inventory scores was significantly reduced by atrial natriuretic peptide (F=21.40, df=1, 9, p=0.001) (
Figure 1).
Analysis of the subscores of the Acute Panic Inventory revealed a significant main effect of time (F=7.60, df=1, 9, p=0.02) and a significant interaction effect of time and treatment (F=14.19, df=1, 9, p=0.004) for the anxiety subscore and significant main effects of time (F=24.08, df=1, 9, p=0.001) and treatment (F=18.43, df=1, 9, p=0.002) and a significant interaction effect of time and treatment for the somatic subscore (F=11.41, df=1, 9, p=0.008) as well. Atrial natriuretic peptide administration reduced the CCK-4-induced increase in anxiety (F=6.55, df=1, 9, p=0.03) and also in somatic symptoms (F=27.03, df=1, 9, p=0.001).
Discussion
The major finding of this exploratory study in patients with panic disorder was that atrial natriuretic peptide had antipanic activity in five of seven patients with CCK-4 induced panic attacks. However, most possibly owing to the small group size, this effect failed to reach statistical significance. In addition, the CCK-4-induced increase in the Acute Panic Inventory scores was significantly reduced by the administration of atrial natriuretic peptide. Subscore analysis of the Acute Panic Inventory scores indicated that atrial natriuretic peptide decreases CCK-4-induced somatic as well as anxiety symptoms, providing further evidence for the anxiolytic activity of atrial natriuretic peptide in patients with panic disorder.
We know of no current evidence that peripheral atrial natriuretic peptide crosses the blood-brain barrier in physiologically significant amounts. A passive, nonsaturable transport of about 1%–2% of an administered dose, however, may be of significance if pharmacological amounts of the peptide are given
(10). Since it is known that peptides exert their effects in the nanomolar range, a low amount of atrial natriuretic peptide administered peripherally may be sufficient to exert effects by means of central receptors. In addition, atrial natriuretic peptide may affect central receptors in brain regions that are not fully protected by the blood-brain barrier. Furthermore, atrial natriuretic peptide may exert effects by means of peripheral receptors: besides a direct depressant action on sympathetic nerve function
(11), a suppression of adrenaline release and a stimulation of sympathoinhibitory afferent vagal activity from the cardiopulmonary baroreceptor system may be involved in the observed anxiolytic activity of peripherally administered atrial natriuretic peptide. However, at the moment, the site of action of atrial natriuretic peptide is unknown and central as well, as peripherally mediated effects may be involved in its anxiolytic activity.
In summary, our findings give clinical evidence for the anxiolytic activity of atrial natriuretic peptide in patients with panic disorder. Limited by our study’s small group size, our results call for further studies on the potential anxiolytic and antipanic activity of atrial natriuretic peptide. Together with preclinical data
(4), our results suggest that trials with nonpeptidergic atrial natriuretic peptide receptor ligands may ultimately lead to new anxiolytic drugs.