On the basis of multicenter trials with fixed doses from 1 to 16 mg/day, the proposed standard clinical dose of risperidone is 6 mg/day
(7,
8). However, a standard dose based on the response rates of groups of patients is likely to be higher than necessary for most patients. In a population of patients, the same dose will produce a range of concentrations in blood and in brain. If a certain minimal drug concentration in brain is required to induce an antipsychotic effect, the dose required to obtain maximal response in a group of patients should be considerably higher than the minimal effective dose in most individuals. This becomes clinically important if adverse effects occur at doses only moderately higher than those required for an antipsychotic effect. For risperidone, a dose-related increase in extrapyramidal side effects was indeed observed
(7,
8). Thus, there is need for a rational approach to find the minimal effective dose of risperidone.
In contrast, patients responding to a wide dose range of the prototype atypical antipsychotic clozapine had only low (20%–63%) D
2 receptor occupancy
(11). The mechanism of action of clozapine may thus be distinct from that of classical neuroleptics. The atypical properties of clozapine have been attributed to a high ratio of 5-HT
2A to D
2 receptor antagonism
(12). We have confirmed high 5-HT
2A receptor occupancy in patients treated with low doses of clozapine
(11). This finding supports the candidate role of the 5-HT
2A receptor as a mediator of atypical effects.
In a previously reported PET study
(13), we found that a single 1-mg dose of risperidone induced about 50% D
2 receptor occupancy and a higher 5-HT
2A receptor occupancy. These findings predict that the suggested standard dose, 6 mg/day, should produce about 80% D
2 receptor occupancy in most patients. This view has been supported by other investigators using PET
(14) or single photon emission computed tomography
(15) who have reported high D
2 receptor occupancy in patients treated with risperidone, 2–14 mg/day. A preliminary analysis of the first four patients in the present study confirmed high D
2 receptor occupancy at 6 mg/day
(16).
The aims of the present study were to define relationships among doses and plasma concentrations of risperidone and D2 and 5-HT2A receptor occupancy and to suggest guidelines for the minimal effective dosing of risperidone based on such relationships. To achieve these aims, receptor occupancy was measured in schizophrenic patients treated with two consecutive fixed doses of risperidone, 6 and 3 mg/day, and correlated with clinical efficacy and extrapyramidal side effects in each patient. We were particularly interested in examining whether the suggested threshold for extrapyramidal side effects at 80% D2 receptor occupancy also applies to patients treated with risperidone.
METHOD
The study was performed at the Department of Clinical Neuroscience, Psychiatry Section, Karolinska Hospital, Stockholm, after approval by the local ethics and radiation safety committees and the Medical Products Agency of Sweden. Eight schizophrenic patients with acute psychotic symptoms participated in this open study after giving informed consent. The patients were hospitalized at least until the first two PET measurements and could then continue on a day care basis. After an initial drug-free observation period of 4 days or more, they were treated with risperidone for 6 weeks: 6 mg/day for 4 weeks and then 3 mg/day for 2 weeks. D
2 and 5-HT
2A receptor occupancy was measured with PET after 4 weeks and again after 6 weeks. Psychopathology and extrapyramidal side effects were evaluated once weekly. Psychopathology was assessed according to the Positive and Negative Syndrome Scale for schizophrenia
(17,
18) and the Clinical Global Impression (CGI) scale
(19). Extrapyramidal side effects were assessed according to the Extrapyramidal Symptom Rating Scale
(20), and akathisia was rated according to the Barnes Akathisia Rating Scale
(21). In a categorical analysis of extrapyramidal side effects, patients with no parkinsonism or questionable parkinsonism (Extrapyramidal Symptom Rating Scale global item score) and no akathisia or questionable akathisia (Barnes scale global item score) were placed in the category “extrapyramidal side effects not present.” Two trained raters conducted each interview, and ratings were based on consensus.
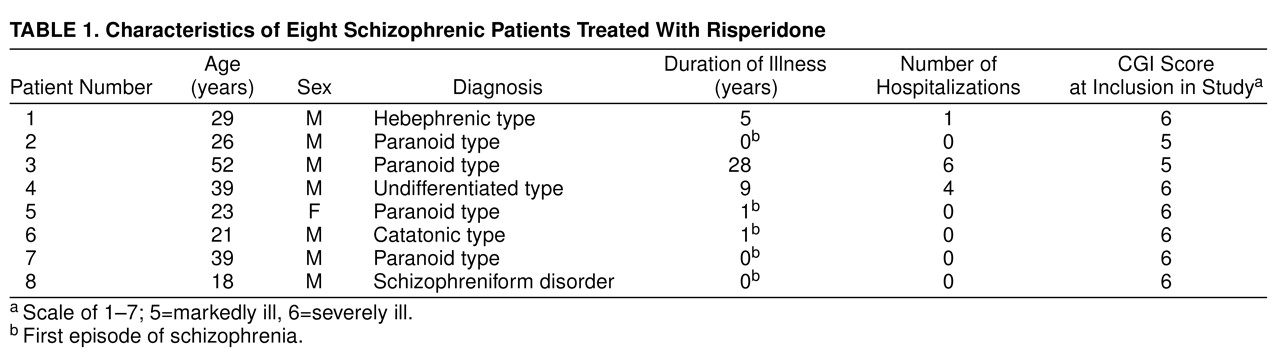
The patients met the DSM-III-R criteria for schizophrenia with acute exacerbation. Five patients were having their first episode of schizophrenia and had never been treated with antipsychotic drugs. Characteristics of the patients are shown in
Table 1.
For inclusion in the study, a minimum score of 4 points (moderately ill) on the CGI was required. Before inclusion, a washout of at least 8 weeks from previous treatment with oral neuroleptics or at least 12 months from depot neuroleptics was required. Patients could not be included if they were severely agitated, actively refused medication, or were unable to give informed consent. They did not have any other mental or physical illness or any substance abuse disorder. Urine samples for screening of opiates, amphetamine, cocaine, and cannabis were collected at inclusion in the study and were found to be negative in all cases.
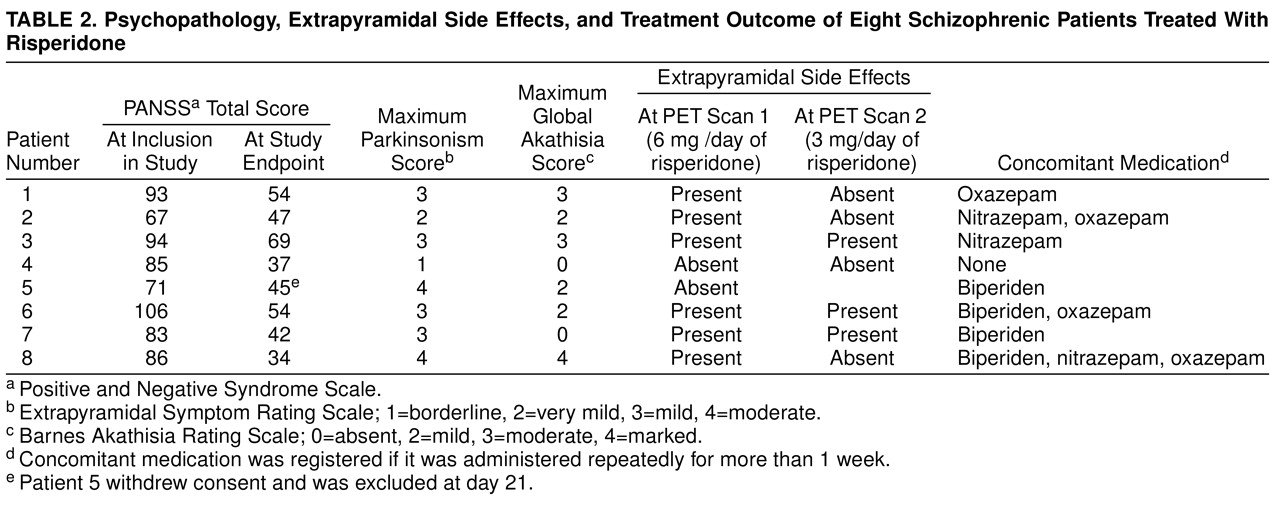
Risperidone was administered as one oral tablet twice daily. On the first treatment day, the dose was 1 mg b.i.d.; on the second day, 2 mg b.i.d.; and thereafter, 3 mg b.i.d. until day 28. From day 29 to day 42, the dose was 1.5 mg b.i.d. Concomitant treatment for anxiety with oxazepam, 10 mg, and for insomnia with nitrazepam, 5 mg, was allowed. In case of extrapyramidal side effects, oral biperiden, 2 mg, could be given. Concomitant medication was given in single doses only as the need was identified on each occasion. Patients who received multiple doses of concomitant medication for more than 1 week are indicated in
Table 2.
Blood samples (10 ml) for the determination of plasma risperidone concentrations were collected before the morning dose at the end of each treatment week. The samples were drawn into heparin-treated glass tubes and centrifuged, and plasma was frozen at –20˚C until analyzed. Plasma concentrations of risperidone and the sum of risperidone and 9-hydroxyrisperidone (the “active moiety”) concentrations were determined by radioimmunoassay
(22). The limit of determination was 0.10 ng/ml for risperidone and 0.20 ng/ml for the active moiety.
PET Measurements
Two consecutive PET examinations were performed within 2.5 hours on day 28 and repeated on day 42. The first examination started 3.5–4 hours after the morning dose of risperidone. D
2 and 5-HT
2A receptor binding was examined with the use of [
11C]raclopride and [
11C]
N-methylspiperone, respectively, as previously described in detail
(13). [
11C]raclopride and [
11C]
N-methylspiperone were prepared according to the methods of Halldin et al.
(23) and Nyberg et al.
(24), respectively. The specific radioactivity at the time of injection was higher than 500 Ci/mmol (18.5 GBq/µmol) for both radioligands. The PET system Scanditronix PC2048-15B (Uppsala, Sweden), which measures radioactivity in 15 sections
(25), was used for patients 1–4, and the new PET system Siemens ECAT EXACT HR 47 (Knoxville, Tenn.), which measures radioactivity in 47 sections
(26), was used for patients 5–8. Radioactivity in the brain was measured continuously for 51 minutes after radioligand injection.
A head fixation system with individually molded plastic helmets was used throughout to avoid movement artifacts and to ensure that the same regions of interest could be used for all experiments in each subject. The fixation system was also used in an initial morphological examination with computerized tomography (patients 1–4) or magnetic resonance imaging (patients 5–8).
Regions of interest were drawn on the reconstructed PET images. The total volume of interest of the putamen was about 6 ml; of the cerebellum, 10–20 ml; and of the neocortex, about 100 ml. Data from different sections of the same regions were pooled before calculation of regional radioactivity. To obtain uptake curves, regional radioactivity was calculated for each frame, corrected for decay, and plotted against time.
Calculation of D2 and 5-HT2A Receptor Occupancy
The quantitative approach for calculation of D
2 and 5-HT
2A receptor occupancy has been described previously
(13,
27,
28). In summary, an equilibrium analysis was applied that used the ratio R between the total radioactivity in the region of interest and the total radioactivity in a reference region with negligible density of D
2 and 5-HT
2A receptors. To calculate D
2 receptor occupancy, the putamen was used as the region of interest; for 5-HT
2A receptor occupancy, the frontal neocortex was used as the region of interest. The cerebellum was used as a reference region in both cases.
Receptor occupancy was defined as the percent reduction in ratio R as compared with the average ratio found in control subjects. Since the two PET systems we used were different with respect to resolution and recovery, separate baseline binding ratios were used for each PET system. The use of a control group binding ratio introduces a small error, which has been discussed in detail elsewhere
(9,
27). A consequence of this method is that the numerical value of receptor occupancy may exceed 100%, although this is more than the theoretical maximum.
In patients 1–4, examined in the Scanditronix PET system, D2 receptor occupancy was calculated by using a control ratio of 3.77, which was previously obtained in 34 healthy subjects (ages=18–50 years), and 5-HT2A receptor occupancy was calculated with a control ratio of 0.77, found in 13 healthy subjects (ages=20–40 years).
In patients 5–8, examined in the Siemens PET system, D2 receptor occupancy was calculated by using a control ratio of 3.17, which was previously obtained in seven healthy subjects (ages=19–43 years), and 5-HT2 receptor occupancy was calculated with a control ratio of 0.69, found in nine healthy subjects (ages=19–30 years).
The calculation of 5-HT
2A receptor occupancy is based on the assumption that [
11C]
N-methylspiperone only binds to 5-HT
2A receptors in the human neocortex. However, [
11C]
N-methylspiperone has affinity not only with D
2 and 5-HT
2A receptors but also with 5-HT
2C and α
1-adrenergic receptors. We have recently confirmed that this lack of selectivity may result in an underestimation of 5-HT
2A receptor occupancy
(28).
D
2 receptor occupancy was plotted against the corresponding plasma concentration of the active moiety of risperidone. According to the law of mass action, the relation between receptor binding and the concentration of ligand at equilibrium is described by a hyperbolic function
(27,
29), as expressed by the equation
Occupancy (%)=0max×concentration/Kiapp+concentration (equation 1),
where Omax is the assumed maximal occupancy (i.e., 100%), and Kiapp is the apparent equilibrium inhibition constant. The calculation assumes linear pharmacokinetics and a linear relationship between drug concentrations in brain and plasma. Each pair of measurements was treated as a separate observation, and equation 1 was fitted through an iterative procedure in a least squares sense to the experimental data. In addition, the relationship between administered dose and receptor occupancy was explored according to equation 1. Thus, the constant Kiapp, corresponding to 50% receptor occupancy, was calculated for both plasma concentrations and oral daily doses.
Statistical Analyses
Changes in psychopathology (Positive and Negative Syndrome Scale total scores) and extrapyramidal side effects (Extrapyramidal Symptom Rating Scale parkinsonism global item score and Barnes akathisia scale global item score) from baseline to day 28 were analyzed with repeated measures analysis of variance (two-way ANOVA).
To examine whether there was an effect of risperidone dose with respect to extrapyramidal side effects, the differences between day 28 assessments (at the dose of 6 mg/day) and day 42 assessments (at 3 mg/day) were analyzed with Student’s t test.
Patient 5 completed only the first 3 weeks of the study and then withdrew consent; she was examined with PET on day 21 instead of day 28. For this patient, both the PET data and the clinical ratings from day 21 were carried forward to the analysis of the data of the other seven patients at day 28. Since the dose of risperidone was changed at day 28, data from patient 5 were then excluded from further analyses.
RESULTS
Seven patients completed the study and responded to treatment. At inclusion in the study, two patients were markedly ill and six were severely ill according to the CGI. Six were much improved or very much improved at both 4 and 6 weeks. Two patients were minimally improved, one of whom was the patient who discontinued on day 21.
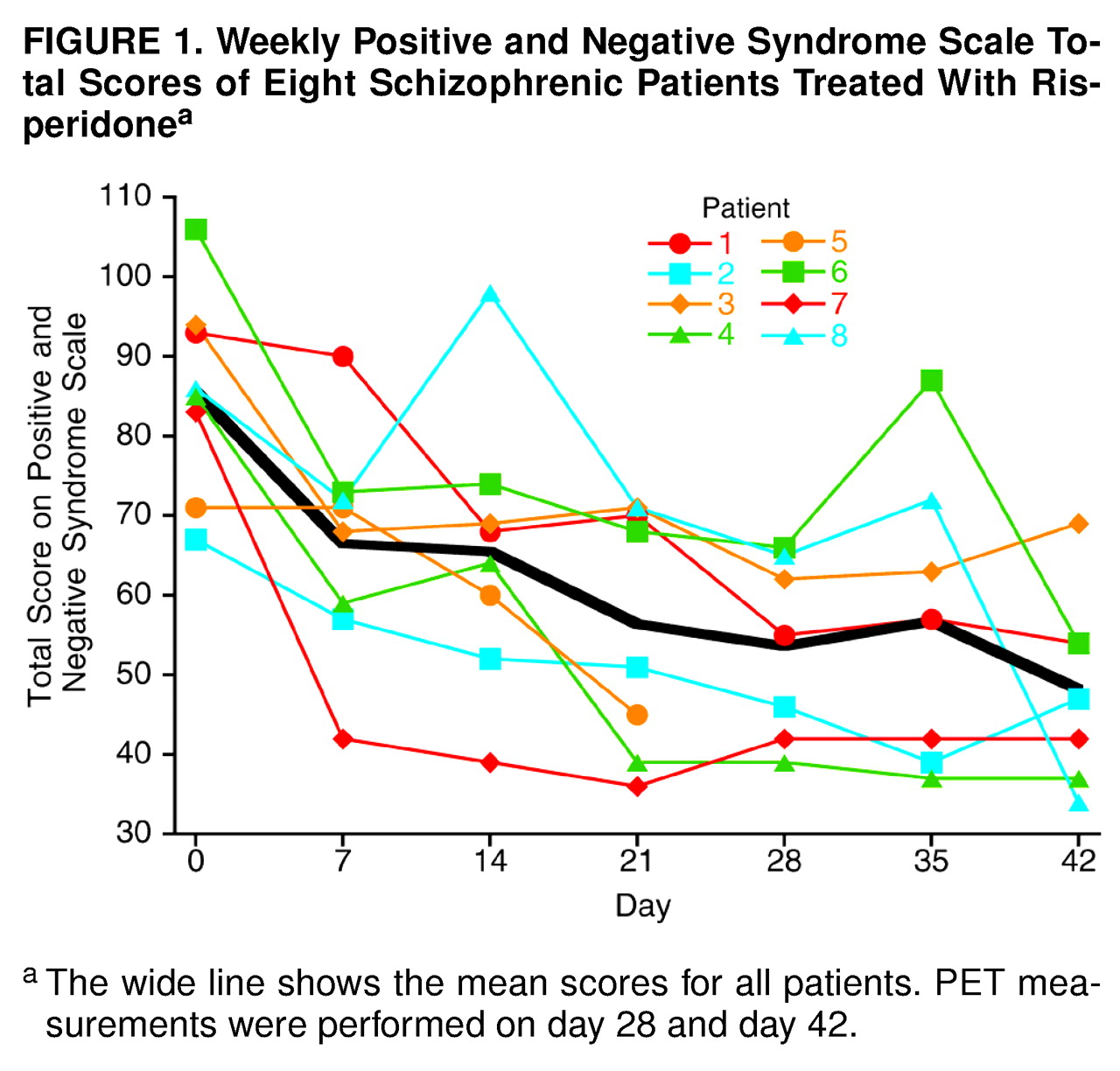
The total Positive and Negative Syndrome Scale scores during the study are shown in
Figure 1. There was a significant decrease in these scores from day 0 to day 28 (repeated measures ANOVA, F=6.57, df=4, 28, p=0.0007), with a mean reduction of 38.6% (range=24.4%–54.1%). At endpoint (day 42) the mean reduction in total Positive and Negative Syndrome Scale scores was 44.8% (range=26.6%–60.5%).
No patient had any score on extrapyramidal side effects at the global ratings of parkinsonism and akathisia at the beginning of the study. After 4 weeks of treatment with risperidone at the dose of 6 mg/day (day 28), six patients had developed extrapyramidal side effects. Six patients had very mild or mild parkinsonism (Extrapyramidal Symptom Rating Scale clinical global impression [item VI]), a significant increase as compared with baseline (F=3.63, df=4, 28, p<0.02). Four patients had mild to marked akathisia (Barnes scale global clinical assessment), and three patients had no akathisia.
The dose of risperidone was reduced to 3 mg/day at day 29 and maintained for another 2 weeks. At endpoint (day 42) only three of seven patients had extrapyramidal side effects (
Table 2). Two patients had very mild parkinsonism, and the others had none. The reduction of parkinsonism scores (Extrapyramidal Symptom Rating Scale item VI) from day 28 to day 42 was statistically significant (p<0.02, Student’s t test). Two patients had mild akathisia, and the others had none.
Patients who required concomitant medication are shown in
Table 2.
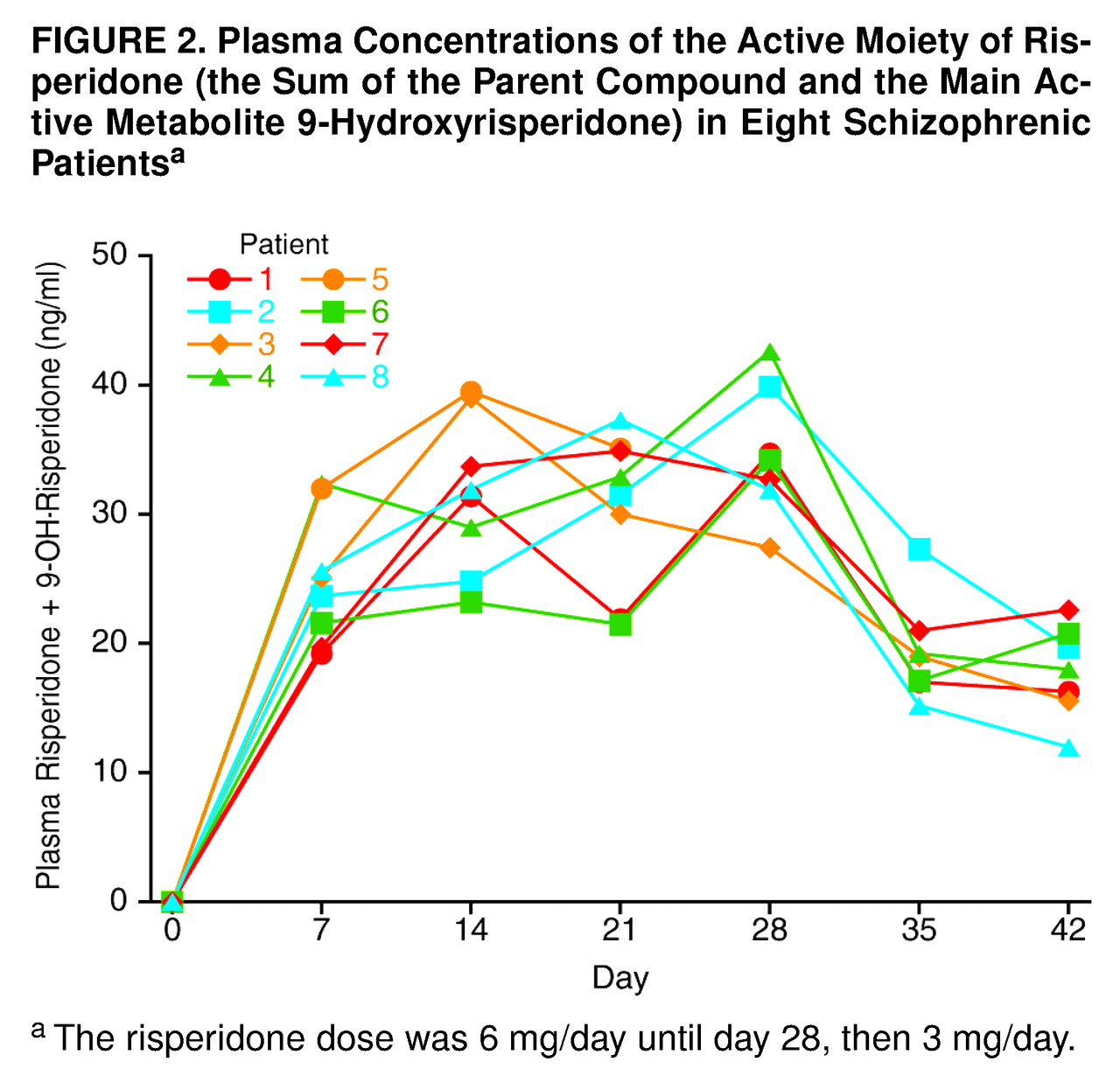
Concentrations of the sum of risperidone and the main active metabolite 9-hydroxyrisperidone were plotted against time, as shown in
Figure 2. After 4 weeks of treatment with risperidone, 6 mg/day (day 28), the mean concentration of the active moiety was 34.8 ng/ml (range=27.4–42.6). At day 42, after 2 weeks of treatment with risperidone, 3 mg/day, the mean concentration of the active moiety was 17.9 ng/ml (range=12.0–22.6).
PET examinations were performed as scheduled on day 28 and day 42 in seven patients. As mentioned, patient 5 withdrew consent at day 21 and was examined with PET at that time. In patient 4, 5-HT2A receptor occupancy on day 28 could not be analyzed because of a technical error.
After risperidone, 6 mg/day, there was a high D2 receptor occupancy (mean=82%, range=79%–85%) and a very high 5-HT2A receptor occupancy (mean=95%, range=86%–109%). After reduction of the risperidone dose to 3 mg/day, the mean D2 receptor occupancy was 72% (range=53%–78%), and the mean 5-HT2 receptor occupancy was 83% (range=65%–112%).
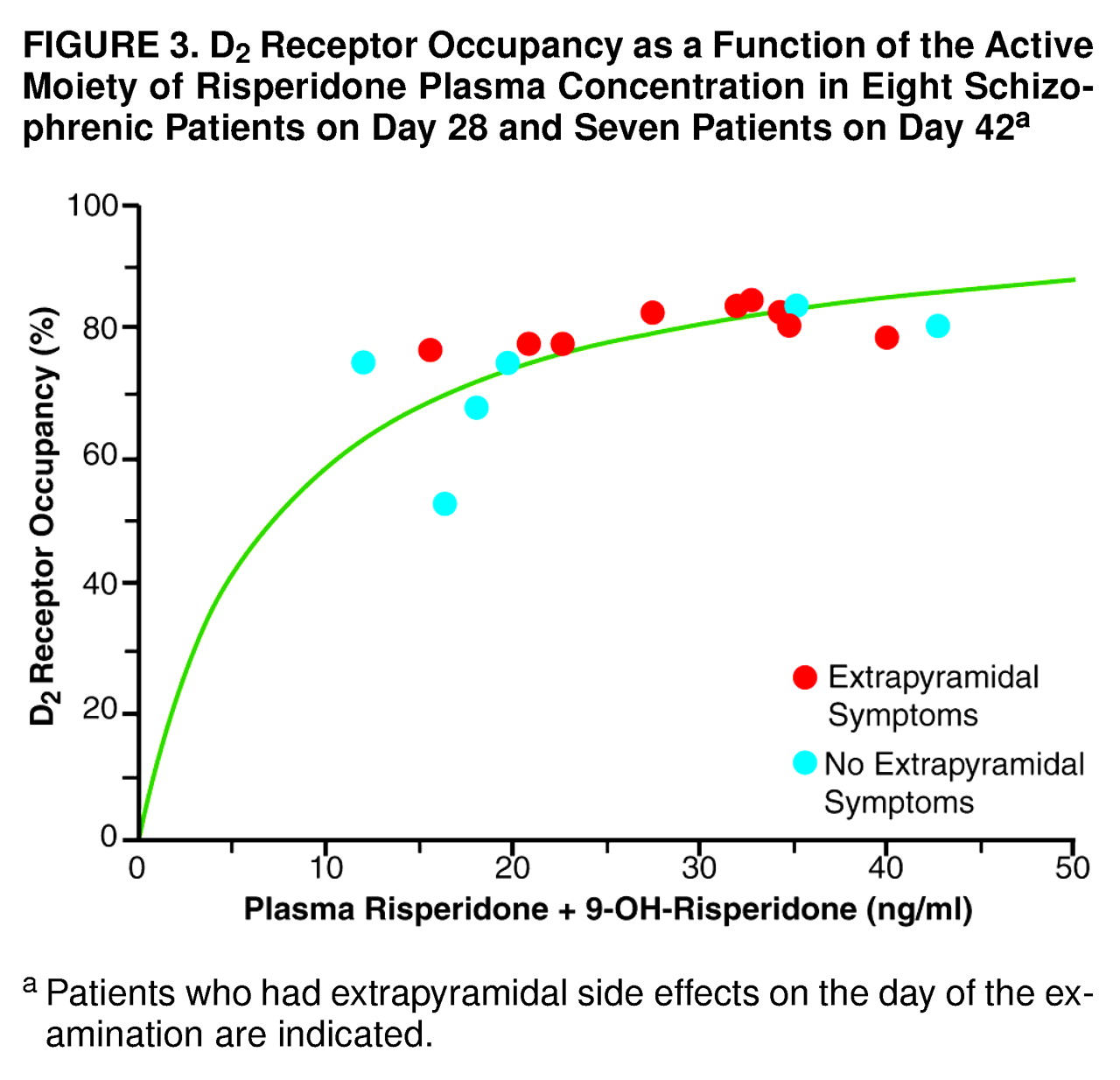
D
2 receptor occupancy was plotted against the corresponding plasma concentration of the active moiety of risperidone (
Figure 3). The curvilinear function of equation 1 could be fitted to the experimental data with the correlation r=0.59. The calculated inhibition constant K
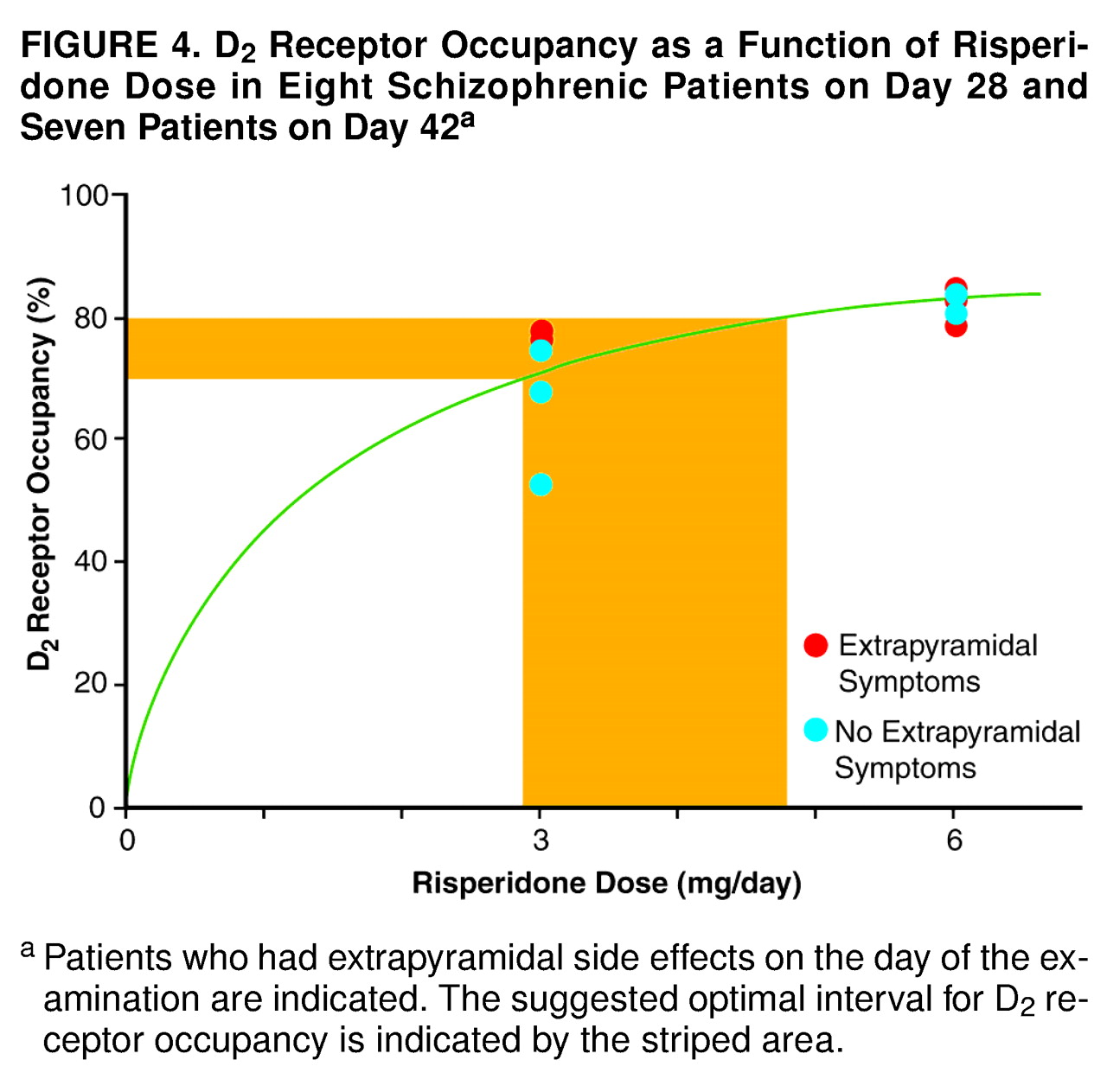
iapp was 6.87 ng/ml. The correlation between D
2 receptor occupancy and oral daily dose was 0.66, with a K
iapp of 1.2 mg/day (
Figure 4).
DISCUSSION
Eight acutely psychotic patients who either were drug naïve or had undergone good washout of previous medication were treated with risperidone at the suggested standard dose, 6 mg/day. D
2 receptor occupancy was consistently high (79%–85%) and in the high range of that previously found in patients responding to classical neuroleptics
(9). The concomitant 5-HT
2A receptor occupancy was even higher (mean=95%). We have previously reported a high test-retest reliability of [
11C]raclopride binding measurements in unmedicated subjects as well as patients treated with antipsychotics
(30,
31). In this study we found a good correlation of D
2 receptor occupancy with both dose and plasma concentrations of the active moiety of risperidone (
Figure 3 and
Figure 4). Thus, the D
2 receptor occupancy found here should be representative of that of patients treated with risperidone and relevant to the dose-response analysis of the large, double-blind, clinical phase III trials of risperidone
(7,
8). In contrast, the clinical response to antipsychotic drug treatment is generally quite heterogeneous, and the susceptibility to adverse reactions varies among patients. Therefore, the clinical drug effects of the present study should be interpreted conservatively and bearing in mind that the study was open and comprised only eight patients. The patient group was heterogeneous with respect to duration of illness. Five patients were experiencing their first episode of schizophrenia, while the others had been ill for several years and had previously received antipsychotic drugs. However, all patients had a similar severity of illness, and all were completely unmedicated at inclusion in the study. This may have contributed to the fact that the overall response to treatment appeared to be more robust than that reported in the phase III trials of risperidone
(7,
8). Those trials mainly included chronic patients with a recent history of medication.
According to the open clinical evaluation, there was a marked reduction of psychotic symptoms in all patients. In six of the eight patients, extrapyramidal side effects were recorded at the time of the first PET examination. This finding is consistent with a suggested threshold for extrapyramidal side effects at D
2 receptor occupancy above 80%
(9). After dose reduction to 3 mg/day, there was a statistically significant decrease in extrapyramidal side effects, while D
2 receptor occupancy was at 53%–78%. This further supports the view that the risk of extrapyramidal side effects is related to high D
2 receptor occupancy.
A limitation of the present study design is that the effects of the two doses cannot be evaluated independently. In particular, the dosing sequence and duration might confound results concerning both efficacy and extrapyramidal side effects. Thus, the pharmacodynamic effects observed during the 2 weeks of treatment with 3 mg/day might have been influenced by the previous higher dose.
A standard dose of 6 mg/day has been suggested for risperidone on the basis of the results of phase III trials
(7,
8). A limitation of those studies is that they were conducted mainly with hospitalized chronic patients in whom carryover effects from previous drug treatment cannot be ruled out. Moreover, the aims of those studies were to identify a dose at which most patients could be expected to respond. Considering the variability of risperidone pharmacokinetics
(32), and assuming that a certain minimal brain concentration is required for antipsychotic effect, a standard dose so defined should be considerably higher than the minimal effective dose for most patients. This is clinically important, since the risk of extrapyramidal side effects was reported to be dose-related. Although risperidone, 6 mg/day, compared favorably with haloperidol, 10–20 mg/day, with regard to extrapyramidal side effects, even lower doses of risperidone produced extrapyramidal side effects in some patients. Thus, it should be clinically advantageous to identify a minimal dose with the best likelihood of therapeutic response and the least risk of extrapyramidal side effects.
In the present study, there was about 80% D
2 receptor occupancy after risperidone, 6 mg/day, with little intersubject variation. Previous PET studies have suggested that antipsychotic effects should be expected at D
2 receptor occupancy above 70%
(9,
10). Our observations suggest that risperidone, 6 mg/day, is likely to induce an unnecessarily high D
2 receptor occupancy in most patients, with a consequent risk of extrapyramidal side effects.
On the basis of the present findings, it can be estimated that 70%–80% receptor occupancy should be expected in most patients at doses of 3–5 mg/day (
Figure 4). We therefore suggest that 4 mg/day of risperidone should be a suitable initial dose to achieve sufficiently high D
2 receptor occupancy for antipsychotic effect with a minimal risk of extrapyramidal side effects in most patients. The corresponding interval of plasma concentrations of the active moiety of risperidone is 16–27 ng/ml (
Figure 3).
It has been suggested that 5-HT
2A receptor antagonism may reduce the risk of neuroleptic-induced extrapyramidal side effects
(1–
3). The relevance of this hypothesis ultimately depends on the clinical efficacy and side effect profile of drugs for which 5-HT
2A receptor antagonism is confirmed in vivo
(33). In this study, all patients had very high 5-HT
2A receptor occupancy at both doses of risperidone. However, there were more extrapyramidal side effects when D
2 receptor occupancy was high. The present results do not support the view that 5-HT
2A receptor blockade provides complete protection against extrapyramidal side effects. The severity of extrapyramidal side effects was mild; this may partly be explained by the effects of concomitant medication (
Table 2). However, this does not rule out the possibility that the high 5-HT
2A receptor occupancy may have mitigated the severity of extrapyramidal side effects.
The atypical properties of clozapine have been attributed to low D
2 and high 5-HT
2A receptor affinity
(1). We have previously reported low (20%–67%) D
2 receptor occupancy and very high 5-HT
2A receptor occupancy in patients treated with clozapine
(11). It has been suggested that risperidone has better efficacy than conventional antipsychotics against the negative symptoms and cognitive deficits of schizophrenia
(7,
8,
34); these effects have been attributed to high 5-HT
2A receptor occupancy. We have shown that 5-HT
2A receptor occupancy was already high after a 1-mg single dose of risperidone in healthy subjects
(13). In the present study 5-HT
2A receptor occupancy was very high at both 6 and 3 mg/day of risperidone. Thus, risperidone in the dose range of 1–4 mg/day should produce D
2 and 5-HT
2A receptor occupancies similar to those found in patients treated with clozapine. It is interesting that phase III trial results suggest that even the lowest doses of 1 or 2 mg/day were effective in some patients
(7,
8). Thus, a careful reevaluation of the efficacy of risperidone in the low dose range should provide grounds for a critical evaluation of the benefit of 5-HT
2A receptor antagonism in the treatment of schizophrenia.