Advance directives (“living wills”) have been widely advocated as a means of extending the autonomy of patients. These documents, written while someone is competent, specify how they wish to be treated if they become incompetent. Although their impact has been small, advance directives are particularly relevant in the care of individuals with mental illness, which is frequently characterized by alternating periods of competence and incompetence
(1). Psychiatrists have important contributions to make to the process of decision making about life-sustaining treatments, particularly in assessing the influence of mental illness on decision making and decision-making capacity
(2). Although research exists on the effect of depression and its treatment on preferences for life-sustaining medical treatments
(3), little is known about the influence of cognitive impairment.
Previous work on the relationship between cognitive impairment and treatment choices has been inconclusive and hampered by small numbers. Two studies have found no correlation. One of these involved 52 nursing home residents and found no relationship between treatment preferences (for cardiopulmonary resuscitation [CPR] and tube feeding) and Mini-Mental State scores or number of years of education
(4). The other study used a 10-point mental status test to rate cognitive functioning
(5). In contrast, in a study of 21 outpatients
(6), higher Mini-Mental State scores were correlated with CPR refusal.
We report on a study of 100 elderly individuals who were asked about their preferences regarding life-sustaining medical treatment and who were also given a cognitive assessment. Our aim was to determine how treatment preferences are affected by cognitive impairment. In addition, we aimed to investigate the effects of premorbid intelligence and decision-making capacity to complete advance directives on preferences for life-sustaining treatments.
Method
One hundred individuals aged 60 or older were recruited to take part in the study, based in Oxford, United Kingdom. Fifty were patients with a DSM-IV diagnosis of dementia at the time of referral from primary care to two community psychogeriatric teams (covering both urban and rural areas). Patients with a clinical diagnosis of mood disorder or psychotic illness were excluded. In addition, 50 community-dwelling elderly volunteers were recruited from retirees’ lunch clubs. This enabled us to determine the treatment preferences of a range of subjects, from those who were not cognitively impaired to those who had moderate degrees of dementia.
Informed written consent for this study was obtained from all subjects or, when relevant, their caregivers. Nineteen patients with dementia refused to participate. There were no significant differences in Mini-Mental State
(7) or National Adult Reading Test
(8) scores between these 19 patients and the 50 patients who did participate. The Oxfordshire Psychiatric Research Ethics Committee approved the project.
Three clinical vignettes were specifically designed to describe realistic situations in the care of the elderly where advance directives would make a difference to medical practice. We avoided using standard instruction directives that apply when patients are permanently comatose or will soon die irrespective of medical intervention because such directives have been criticized in the elderly, where the possibility of life-sustaining treatments, such as tube feeding or antibiotics, often arises before terminal illness
(9). In contrast, disease-specific advance directives make treatment options easier to understand
(10). Each vignette was written simply and presents a hypothetical medical problem with symptoms, together with treatment alternatives leading to an intervention or nonintervention (
Appendix 1).
All interviews were conducted by one of us (S.F.) in a quiet area in a lunch club for the community-dwelling elderly or at home or in the hospital for patients with dementia. The Mini-Mental State
(7) and the National Adult Reading Test
(8), a valid and reliable index of premorbid IQ in the elderly, were administered. Each vignette was read to each subject, followed by a semistructured interview that determined treatment preferences. No previous explanation of the vignettes was given. Decision-making capacity to complete advance directives was determined by using an instrument recently shown to validly assess this specific competence
(11). This instrument used the semistructured interview that followed the presentation of the vignettes to address the legal standards of competence: communicating stable choices, comprehending information presented, appreciating consequences of decisions, and reasoning ability.
Each subject was asked his or her intervention preferences for the three vignettes. A preference for an intervention (such as antibiotic treatment or tube feeding) in a particular vignette was given a score of 1, and a preference for not having that intervention was scored 0. The mean intervention score per vignette was then computed for each individual. Those whose mean score was 0.5 or higher formed part of the intervention group, and those who scored less than 0.5 were the nonintervention group. Independent t tests were used to compare intervention and nonintervention groups as well as differences in mean intervention scores of the subjects who were or were not capable of making decisions (“competent” and “incompetent” groups).
Results
The mean age of the 100 subjects interviewed was 77.3 years (SD=7.2, range=60–99). Forty-three were men. All but one of the subjects was Caucasian. The patients with dementia (mean age=79.8, SD=6.6) were significantly older than the elderly volunteers (mean age=74.9, SD=6.2) (t=–3.82, df=98, p<0.001). The mean Mini-Mental State score of the 100 subjects was 21.4 (SD=7.6), and their mean estimated premorbid IQ (according to the National Adult Reading Test) was 98.9 (SD=15.9). Fifteen subjects were so incompetent that they were not able to give any intervention preferences. Of the remaining 85 subjects, 83 completed vignette 1, 79 completed vignette 2, and 77 completed vignette 3.
In vignette 1, 48 [57.8%] of the subjects opted for medical interventions (tube feeding); in vignette 2, 61 [77.2%] chose interventions (investigative tests with or without surgery); and in vignette 3, 54 [70.1%] chose interventions (antibiotics with or without hospitalization).
No significant difference in intervention preferences was found between the elderly volunteers (mean intervention score=0.65, SD=0.29) and the patients with dementia (mean intervention score=0.75, SD=0.36) (t=1.37, df=83, p=0.12) or in the intervention preferences for individual vignettes (28 [54.9%] of the elderly volunteers chose interventions in vignette 1, 40 [78.4%] in vignette 2, and 33 [64.7%] in vignette 3, compared with 20 [62.5%], 21 [75.0%], and 21 [80.8%] of the patients with dementia, respectively).
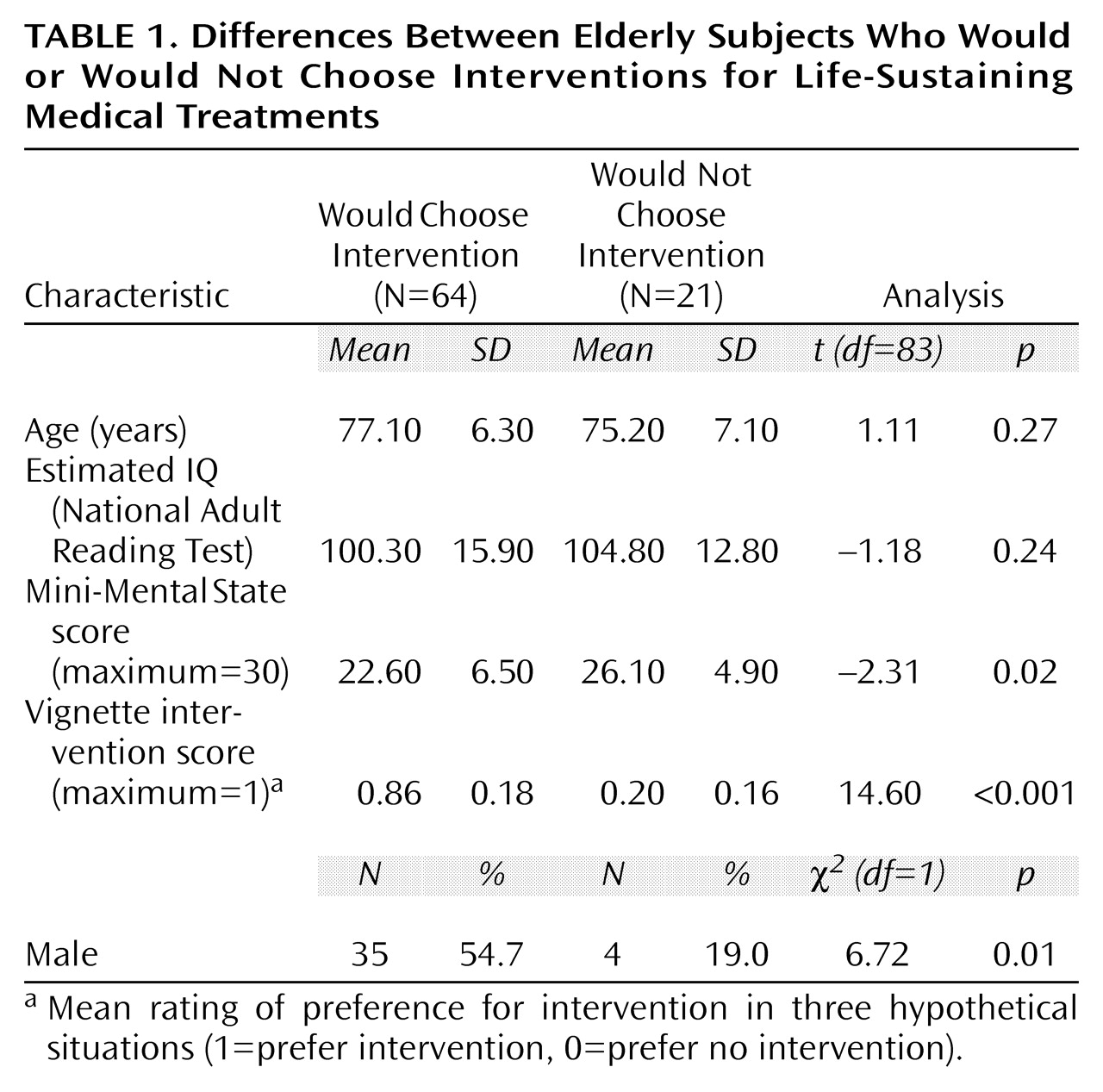
Table 1 compares intervention and nonintervention groups. We found no difference in estimated IQ (National Adult Reading Test) between these groups, but there was a significant difference in Mini-Mental State scores: the elderly subjects who opted for medical interventions had lower Mini-Mental State scores. We compared competent and incompetent groups in terms of intervention preferences (data not shown). There was a significant difference (t=2.04, df=83, p<0.05) between the mean intervention scores of the competent and incompetent groups: elderly subjects who were capable of making decisions were more likely to choose nonintervention in end-of-life treatment decisions.
Discussion
This study of 100 elderly individuals has explored whether cognitive impairment and premorbid intelligence in elderly individuals affect treatment preferences for life-sustaining medical therapy. We found that subjects who opted for life-sustaining medical therapy had lower Mini-Mental State scores. There was no difference in estimated IQ (National Adult Reading Test) between subjects who did or did not opt for intervention. Our present investigation is preliminary, and more detailed cognitive tests are necessary to establish the nature of the changes that correlate with differences in treatment preferences.
Our results also suggest that elderly subjects who lack the capacity to complete advance directives are more likely to choose interventions when faced with end-of-life treatment decisions. This result is supportive of the finding in a study of 29 nursing home residents that nonsignificantly more incompetent than competent residents requested life-sustaining treatments
(12). This contrasts with the preferences of relatives and staff caring for incompetent individuals, who chose interventions in less than half of the cases
(13).
The rates of intervention preferences that we found are similar to those reported in other studies of the elderly. In a survey of 218 community elderly, half of the respondents said that, if they developed Alzheimer’s disease, they would opt for tube feeding and a ventilator, and nearly three-quarters said they would choose antibiotics for a serious infection
(14). This contrasts with studies of the general adult population, 10% of whom said they would request tube feeding and a ventilator if they developed dementia
(15).
Why do people with cognitive impairment tend toward intervention? We suggest three possible reasons. First, cognitive impairment may limit their ability to understand the consequences of their decisions, therefore leading to overly aggressive treatment choices. It may also lead to impulsive decisions and/or overestimating benefits if judgment is impaired. Second, an awareness of one’s own cognitive impairment may lead to recognition of one’s own vulnerability and a consequent wish to accede to medical wisdom. This may be equated with intervention in most people’s minds. This parallels the finding that a sense of vulnerability to deteriorating social supports and disability in terminal illness causes people to prefer more aggressive care
(16). Third, people who already have cognitive impairment may put a higher value on their life than the value that people without cognitive impairment put on their future hypothetical life with dementia
(17).